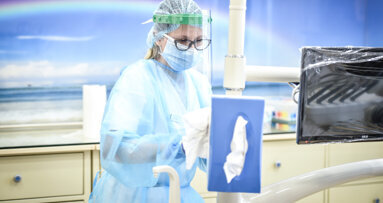
ARLINGTON, Va., U.S.: The importance of sterilization in the dental practice and operating room cannot be underestimated. In a new study, researchers have found that adherence to proven protocols for disinfecting hands, patients’ skin and surfaces could help to halt the spread of dangerous Staphylococcus aureus pathogens from controlled spaces and beyond.
Despite the solid evidence supporting improved practices for hand hygiene, vascular access, and patient skin disinfection, researchers from the University of Iowa Hospitals and Clinics have reported that adherence to preventive measures is abysmal. They suggested that the poor practices may help to explain why up to 7 percent of patients undergoing surgery continue to contract at least one postoperative infection.
With the increased spread of antibiotic-resistant S. aureus pathogens from acute care settings to healthy members of the community, the researchers identified and characterized the epidemiology of particularly pathogenic S. aureus sequence types (STs) in the operating room. “The increase in the spread of S. aureus pathogens beyond the acute care setting is alarming, but we know that there are evidence-based practices that can address this critical patient safety issue,” said the study’s lead author, Dr. Randy W. Loftus from the Department of Anesthesia. “The goal of the study was to increase awareness around the transmission of the different strains, with the aim of improving compliance with proven infection control measures.”
In the study, S. aureus isolates were collected from three academic medical centers. After this, transmission dynamics for hypertransmissible, strong biofilm-forming, antibiotic-resistant and virulent STs were assessed using a systematic phenotypic and genomic approach combined with a new software platform. The transmission story for these key pathogens was then mapped and reported.
The researchers found that S. aureus ST 5 is a more pathogenic strain associated with increased strength of biofilm formation and increased risk of transmission and infection. Two of the ST 5 isolates were linked by whole-cell genome analysis to postoperative infection, something the researchers believe is an alarming finding that likely underestimates the true magnitude of the problem. The combination of ST 5 pathogenicity, an aging patient population, and increasingly complex surgical procedures may help to explain the increase in the community spread of invasive methicillin-resistant S. aureus infections.
Unsurprisingly, the researchers confirmed patient skin surfaces and healthcare provider hands as sources of ST 5 pathogen transmission. They suggested that strict compliance with processes to decolonize patients of bacteria before surgery and to maintain hand hygiene compliance during surgery will likely help control the spread of this important strain characteristic. They noted as well that operating room environmental surfaces were linked with transmission, indicating the importance of continually assessing the effectiveness of environmental cleaning protocols.
The study, titled “High-risk Staphylococcus aureus transmission in the operating room: A call for widespread improvements in perioperative hand hygiene and patient decolonization practices,” was published in the October issue of the American Journal of Infection Control.
Tags:
Dr Michael Bornstein is Clinical Professor in Oral and Maxillofacial Radiology and Associate Dean for Research and Innovation at the University of Hong Kong...
ZAGREB, Croatia: As 3D-printed aligners gain traction, many patients and clinicians continue to apply cleaning routines that were originally developed for ...
IRVINE, Calif., U.S.: BIOLASE, a global leader in dental lasers, has reported the results of a clinical trial conducted at the McGuire Institute. Designed ...
Many are calling it the post-pandemic era—the time in which we will simply have to live with the SARS-CoV-2 virus as part of our daily personal and ...
CHICAGO, US: An expert panel established by the American Dental Association (ADA) Council on Scientific Affairs has published new recommendations for safety...
LANZHOU, China: The journey that Homo sapiens has embarked on is something that has enthralled modern scientists for many centuries. Now, as technology ...
As part of its specialty symposia series, Dental Tribune International will host an online symposium on artificial intelligence (AI) and digital dentistry ...
CHENGDU, China: Tooth root development depends on precise cell communication pathways. Researchers from China have shown how two genes, Gli2 and Gli3, work...
MELBOURNE, Australia: Tooth loss can have a profound impact on social interactions and self-esteem. While poor oral health is known to be associated with ...
NEW YORK, U.S.: The risks associated with poor oral health are many. In the past, scientists have demonstrated that around a third of colorectal cancers are...
Live webinar
Tue. 26 May 2026
12:00 pm EST (New York)
Live webinar
Tue. 26 May 2026
2:00 pm EST (New York)
Live webinar
Wed. 27 May 2026
8:00 am EST (New York)
Live webinar
Thu. 28 May 2026
12:00 pm EST (New York)
Dr. Anthony Viazis DDS, MS. Inventor & Founder of Fastbraces®
Live webinar
Mon. 1 June 2026
1:00 pm EST (New York)
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East
































To post a reply please login or register