CLEVELAND, U.S.: In a recent advancement in cancer research, scientists have used artificial intelligence (AI) to help customize the radiation dosage for individual patient treatments. An earlier study showed that radiation therapy for throat cancer can produce better results than transoral robotic surgery (TORS). This latest development may help physicians in all fields prescribe better treatments and save more lives.
“While highly effective in many clinical settings, radiotherapy can greatly benefit from dose optimization capabilities,” explained lead author Dr. Mohamed Abazeed, a radiation oncologist at Cleveland Clinic’s Taussig Cancer Institute and a researcher at the Lerner Research Institute. “This framework will help physicians develop data-driven, personalized dosage schedules that can maximize the likelihood of treatment success and mitigate radiation side effects for patients.”
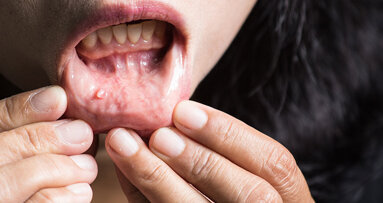
After the recent increase in HPV infections and the doubling of cases of oropharyngeal cancer since the 1990s, treatment methods are becoming increasingly important. As reported by Dental Tribune International, results from the study investigating swallowing outcomes for throat cancer patients who underwent either TORS or radiation therapy challenged commonly held beliefs. This new study could potentially aid in producing even better outcomes.
“The development and validation of this image-based, deep-learning framework is exciting because not only is it the first to use medical images to inform radiation dose prescriptions, but it also has the potential to directly impact patient care,” said Abazeed. “The framework can ultimately be used to deliver radiation therapy tailored to individual patients in everyday clinical practices.”
According to the study, the AI system was constructed by using the information from 944 lung cancer patients treated with high-dose radiation, their CT scans and electronic health records. Pretreatment scans were entered into a deep-learning model, which analyzed the scans to create an image signature that predicted treatment outcomes. Using sophisticated mathematical modeling, this image signature was combined with data from patient health records—which describe clinical risk factors—to generate a personalized radiation dose.
Abazeed predicted that machine learning tools will play a larger role in the health care sector. He said that the image-based information platform not only can provide the ability to individualize multiple cancer therapies but is also is a leap forward in radiation precision medicine.
The study, titled “An image-based deep learning framework for individualising radiotherapy dose: A retrospective analysis of outcome prediction,” was published in the July 2019 issue of the Lancet Digital Health.
Tags:
COVENTRY, UK: The impact artificial intelligence is having on the healthcare industry is becoming more and more evident on a daily basis. In dentistry, some...
For those who have been paying attention to the latest news in the technology space, you will most certainly have noticed that OpenAI recently launched ...
The May 2019 edition of The Atlantic magazine contained an article titled “The truth about dentistry”. In it, the author visualised dentists—not a ...
NEW YORK, U.S.: Artificial intelligence (AI) has broken free from the pages of science fiction to become fact. Machines and software that can think and ...
BASEL, Switzerland: The application of artificial intelligence (AI) in dentistry is still in its early stages; however, more development is starting to take...
3D printing, commonly referred to as additive manufacturing (AM), is transforming many industries, including dental, biomedical, aerospace, construction and...
Artificial intelligence (AI) has moved from theory into daily prosthodontic practice, reshaping diagnosis, treatment planning and design workflows. My ...
“I hate the dentist” is an all-too-common refrain from patients. This is to be expected when, according to some studies, as many as 60% experience ...
COLOGNE, Germany: The integration of artificial intelligence (AI) has accelerated in many industries in recent years, and dentistry is proving to be no ...
FARMINGTON, Conn., US: Many factors may influence therapeutic decisions in orthodontics. For example, orthodontists may sometimes inaccurately interpret ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






































To post a reply please login or register