The digital revolution has changed the world and dental medicine is no exception. We live in the digital era: we have the materials and techniques that allow us to develop a totally digital workflow, allowing dental medicine to grow to a new level, becoming faster and more efficient, when combined with scientific and clinical knowledge. There are numerous technologies that simplify the daily work, such as intraoral, extraoral and face scanners, CBCT (cone beam computed tomography) with a low radiation dose, and software processing and production, better known as CAD/CAM (computer-aided design and manufacturing), which together with new aesthetic materials and prototyping tools (milling machines and 3-D printers) are radically transforming dental medicine. This case report has the aim of presenting an example of prosthetic digital workflow, with the integration of several technologies that help us achieve treatment success.
Clinical case
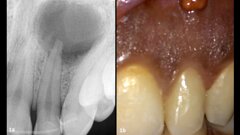
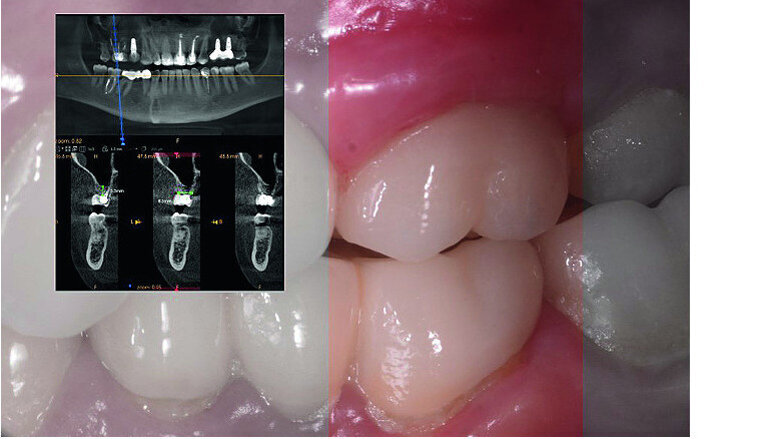
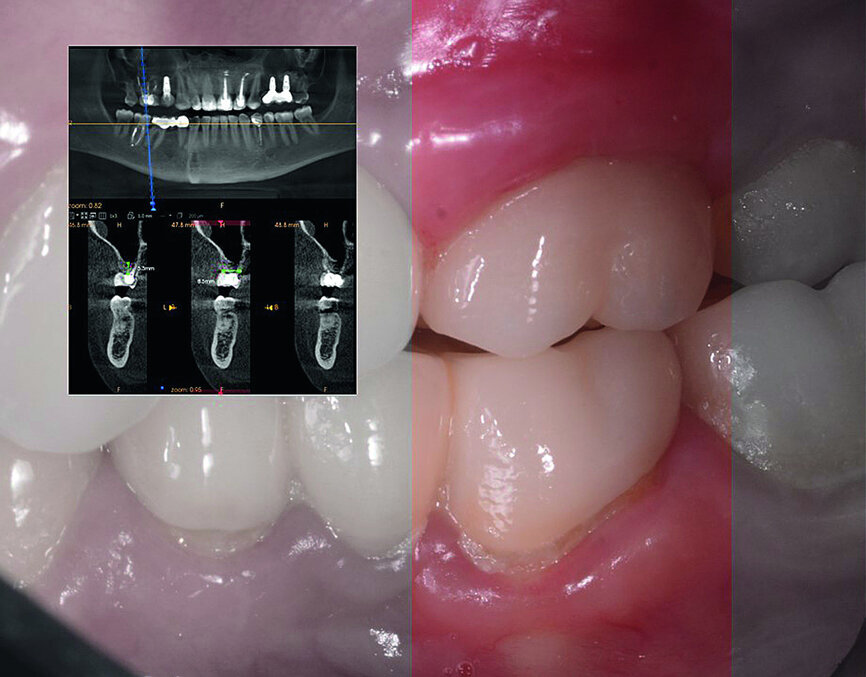
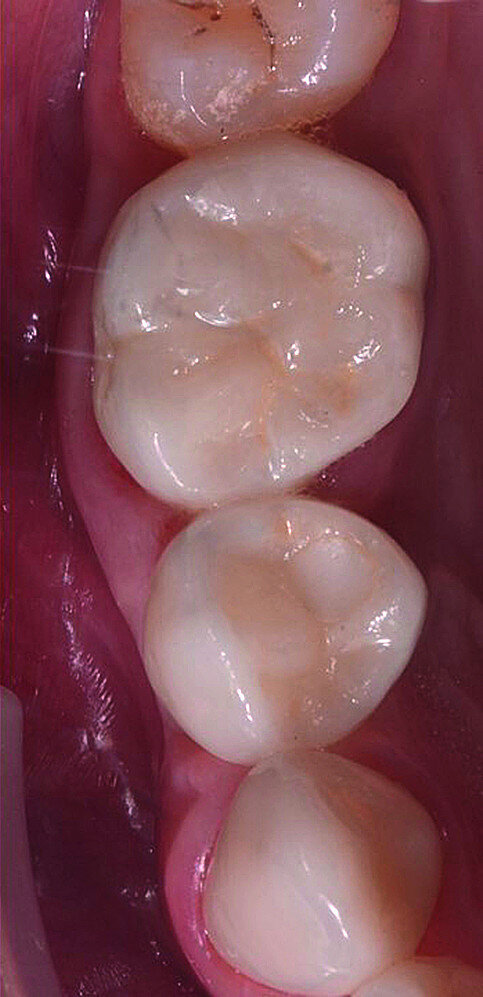
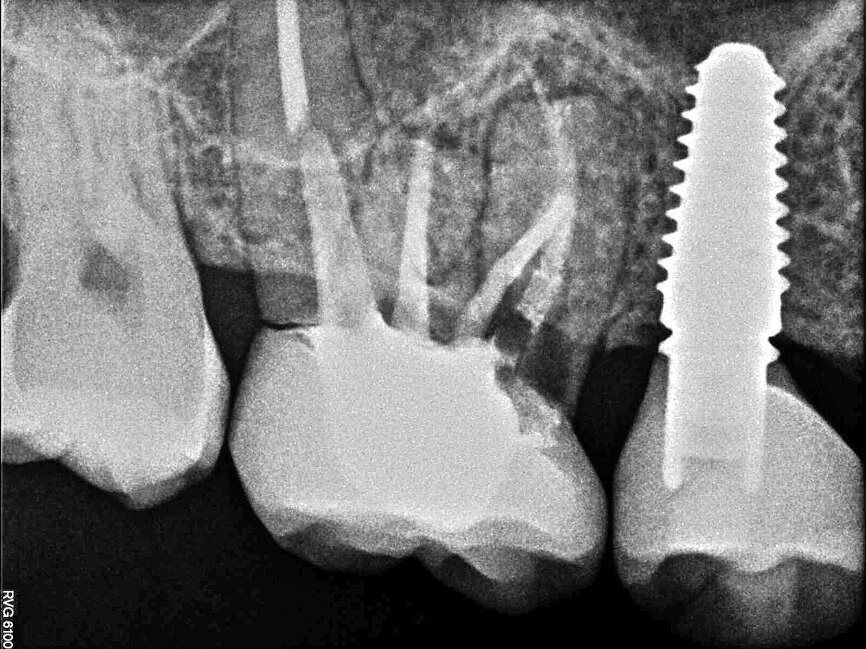
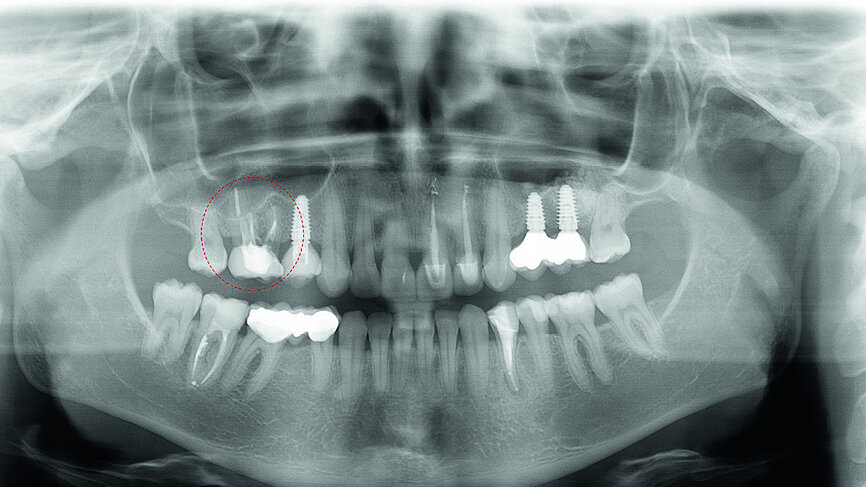
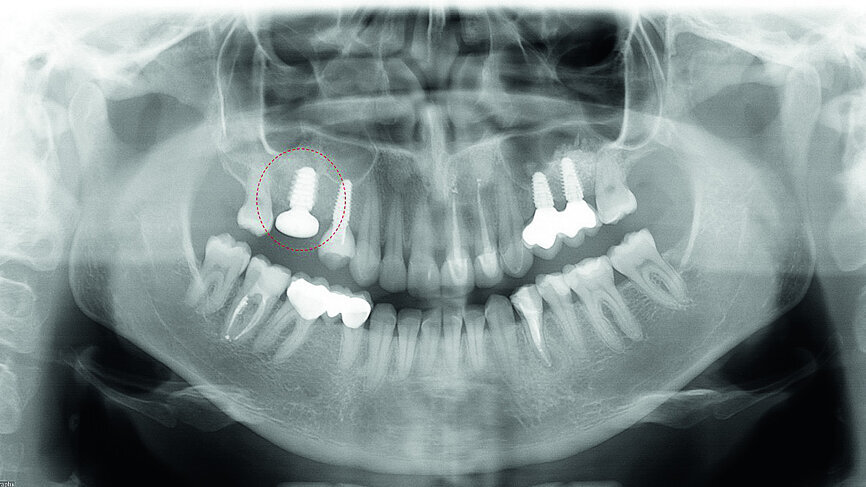
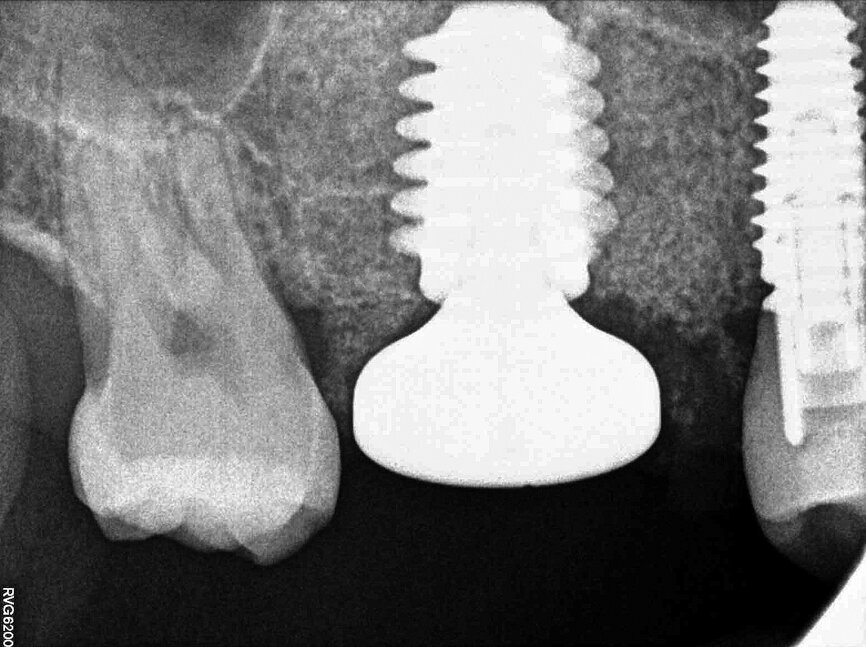
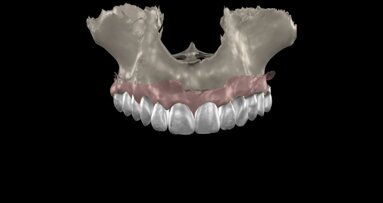
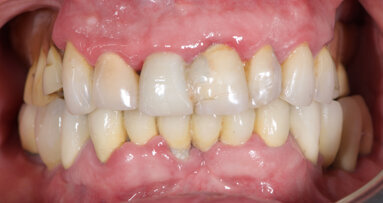
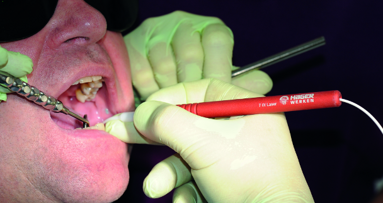
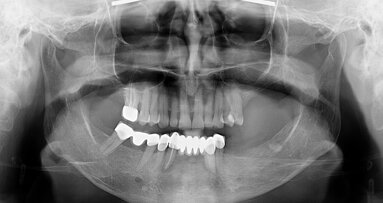
In November 2017, a 39-year-old female patient came to an initial appointment at White Clinic owing to tooth pain (tooth #16). A clinical and radiographic examination were performed, including a periapical radiograph, CBCT scan (Carestream 9500, Carestream Dental), and intra- and extraoral photographs (Figs. 1–3).
In the clinical and radiographic evaluation, it was observed that tooth #16 presented an invasive cervical resorption at the mesiobuccal root. The treatment plan established was dental extraction with immediate implant placement. The tooth had been previously re-treated endodontically and restored with a definitive ceramic crown. Due to the current situation of the tooth, although the protocol in White Clinic is to preserve teeth, it had indication for immediate extraction. Also due to the lack of time, our digital team was not able to produce a surgical guide for the implant placement. Therefore, the treatment plan included a surgical phase and a digital prosthetic phase.
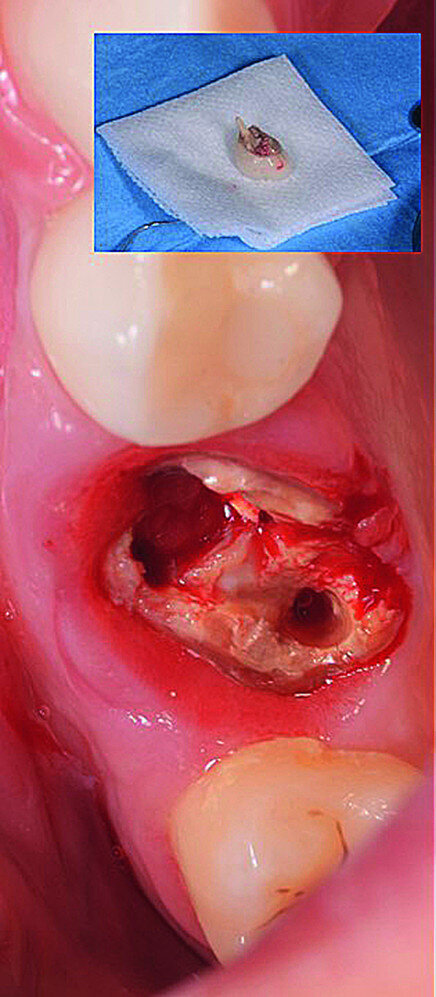
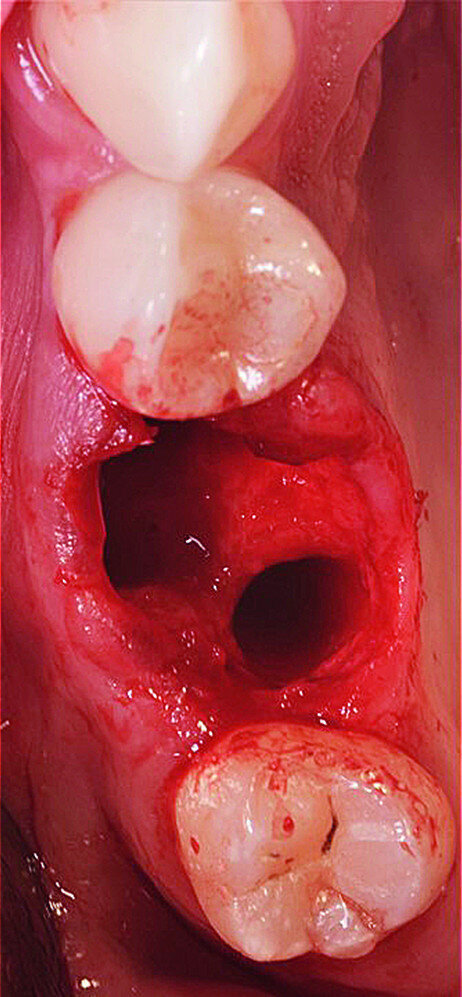
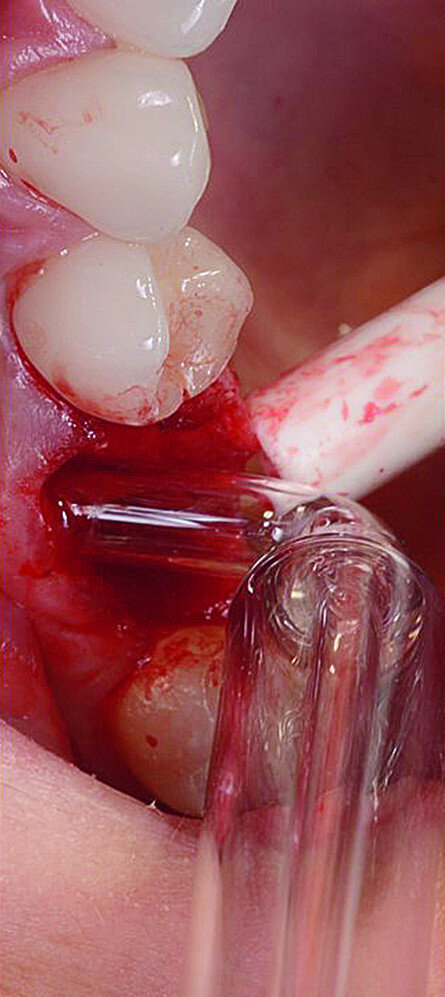
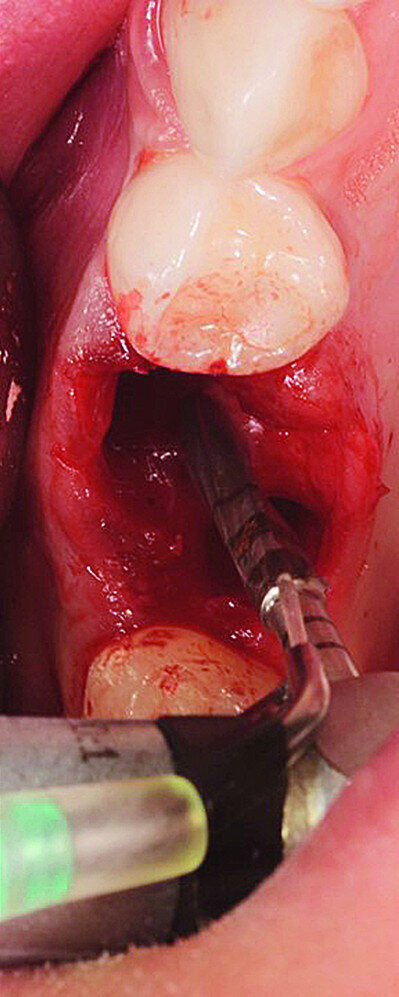
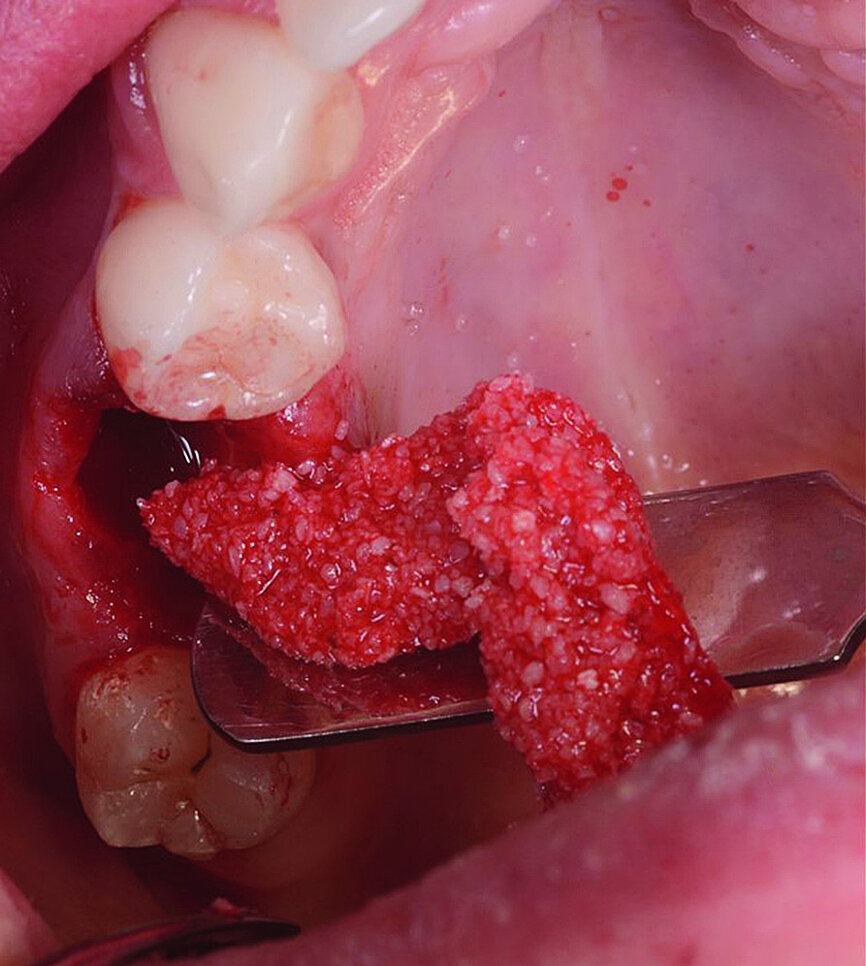
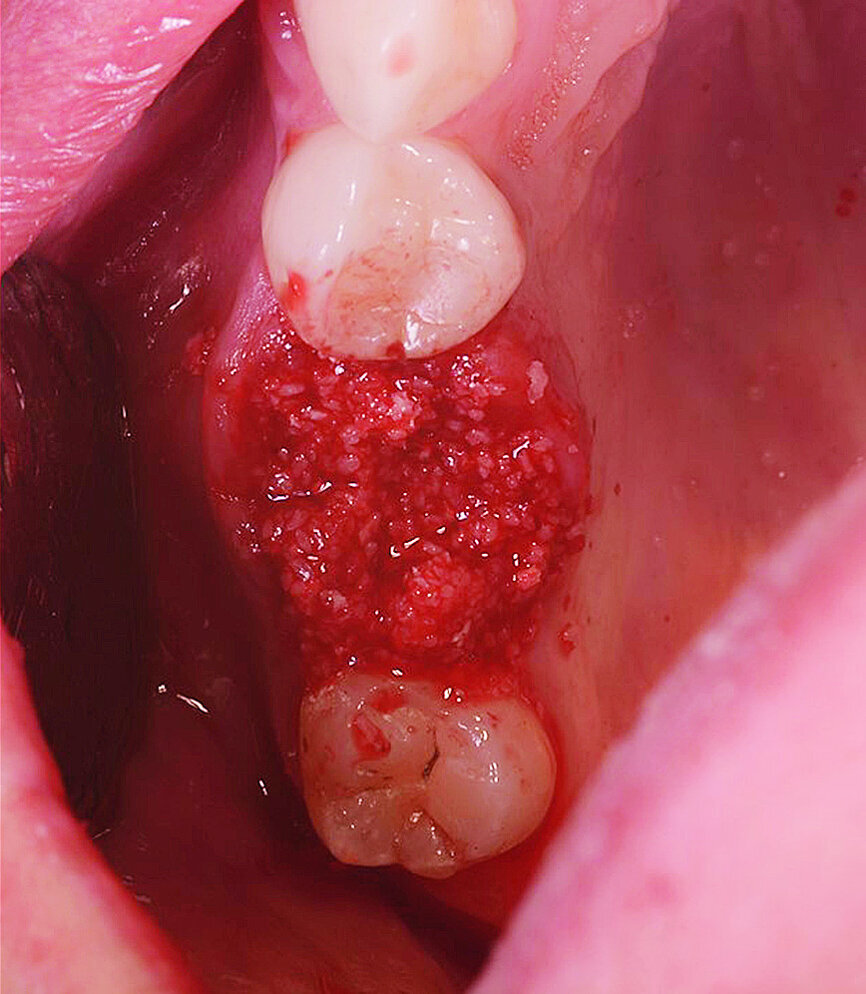
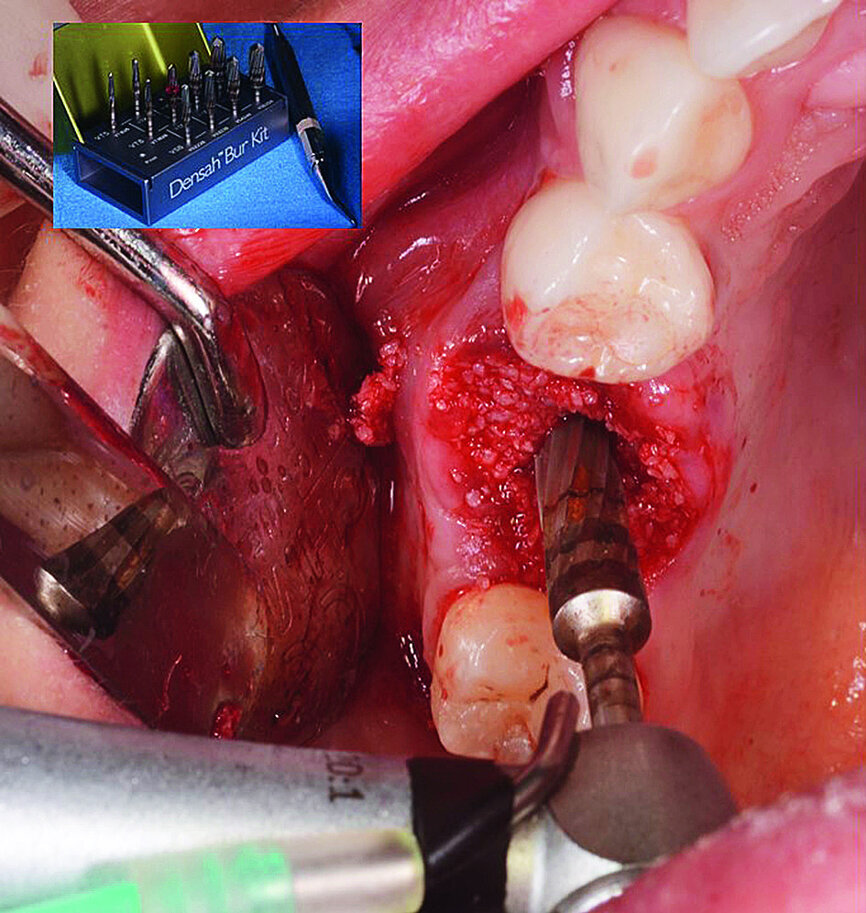
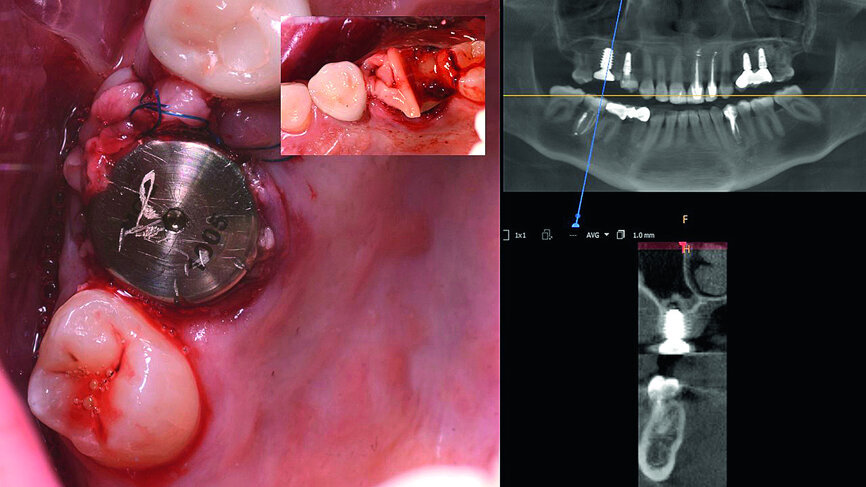
The surgical treatment phase started with extraction of tooth #16, followed by excision of the root cyst and alveolar curettage (Figs. 4a & b). For good disinfection of the alveolus, ozone therapy (Ozone DTA, Apoza) was applied (Fig. 4c), taking into account the antimicrobial action of ozone, which prevents the development of the inflammatory process, favouring cellular recovery and consequently improving the postoperative healing. Once the alveolus had been disinfected, the implant bed was prepared with a sequence of implant drills from the AnyRidge surgical system (AnyRidge Surgical Kit, MegaGen; Fig. 4d). The bone defects were filled with a bone xenograft of porcine origin (Gen-Os, OsteoBiol), mixed with i-PRF (injectable platelet-rich fibrin; PRF process by Choukroun; Figs. 5a & b). Afterwards, bone densification was performed through a sequence of Densah drills (Densah Burs, Versah; Fig. 6a). This type of drill allows the clinician to perform a bone densification process.
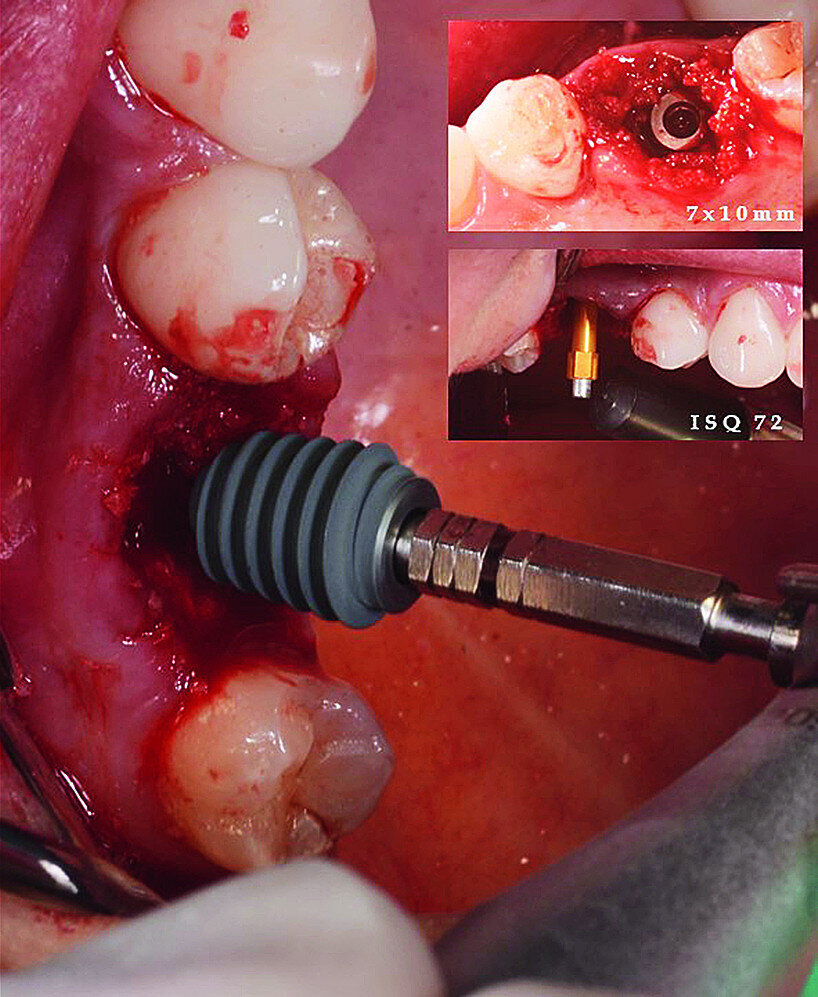
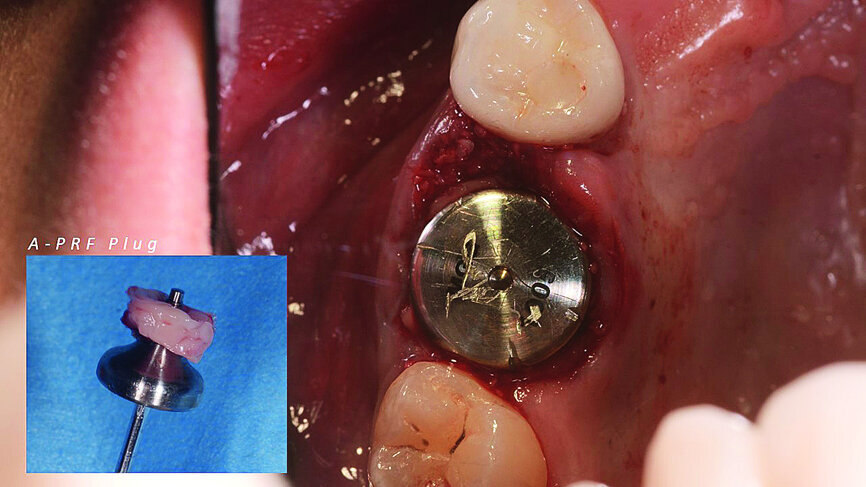
Once the implant bed had been prepared, a 7 × 10 mm implant (AnyRidge) was placed. After placement, the ISQ (Implant Stability Quotient) was measured with a stability meter (Mega ISQ, MegaGen), and the value was 72. According to the ISQ scale, this represents high stability (Fig. 6b). A 10 × 7 mm healing screw (AnyRidge) was placed, along with a plug of A-PRF (advanced platelet-rich fibrin; PRF process by Choukroun) in order to accelerate the healing process, and sutured with 4/0 polypropylene (Hu-Friedy; Figs. 7–10). After the surgical procedure, the White Clinic postoperative protocol was applied: application for eight minutes of the ATP38 laser (Swiss Bio Inov), based on the principle of Low Level Laser Therapy that acts on the cellular metabolism and provides a better and faster postoperative healing. The patient was instructed to use a 0.2% hyaluronic acid gel (Gengigel, Ricerfarma) and 0.1% hyaluronic acid mouthwash (Gengigel First-aid, Ricerfarma) for one week after surgery, with the goal of accelerating the healing process. One week after surgery, the sutures were removed, ozone was used to disinfect the area around the implant, and the ATP38 was applied for eight minutes to promote healing.
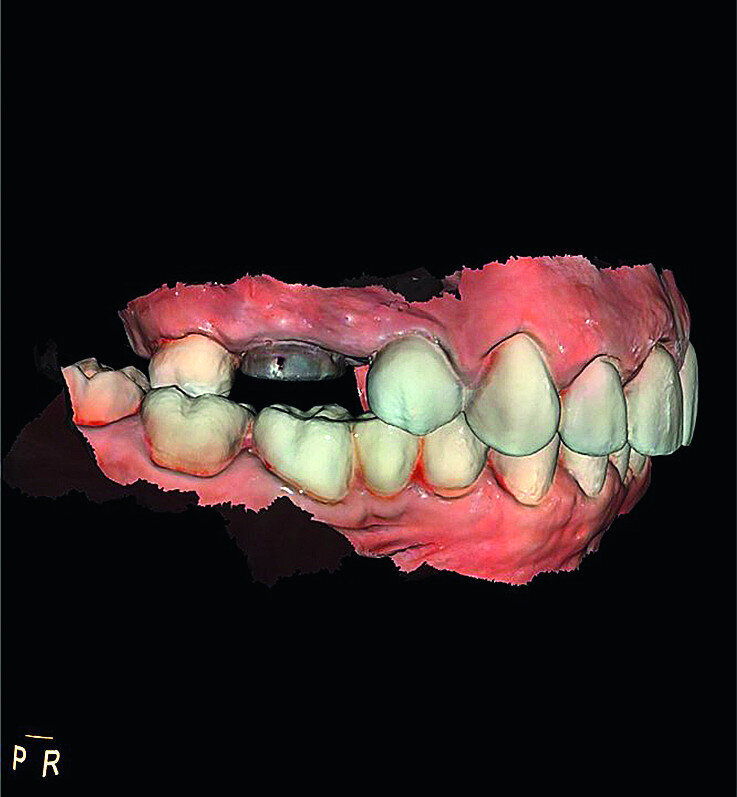
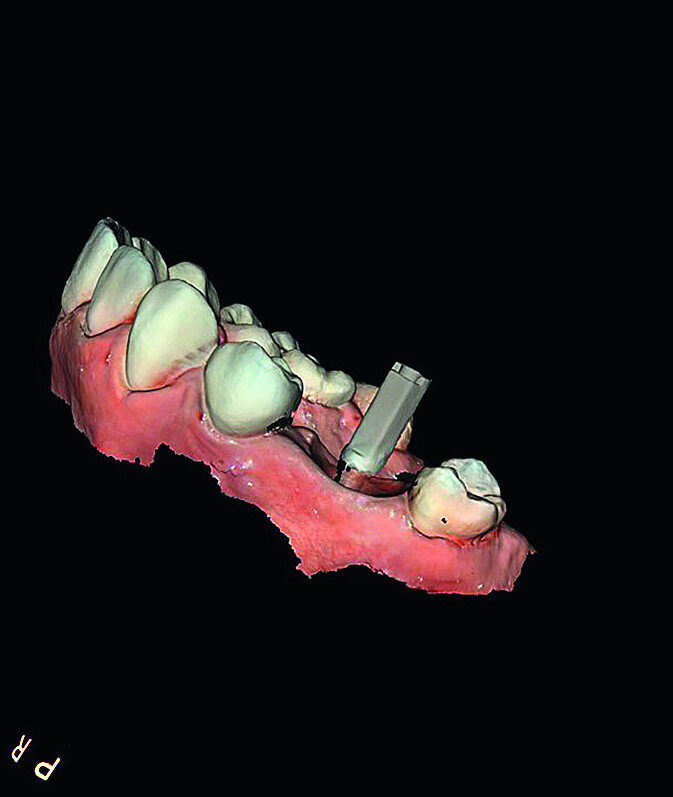
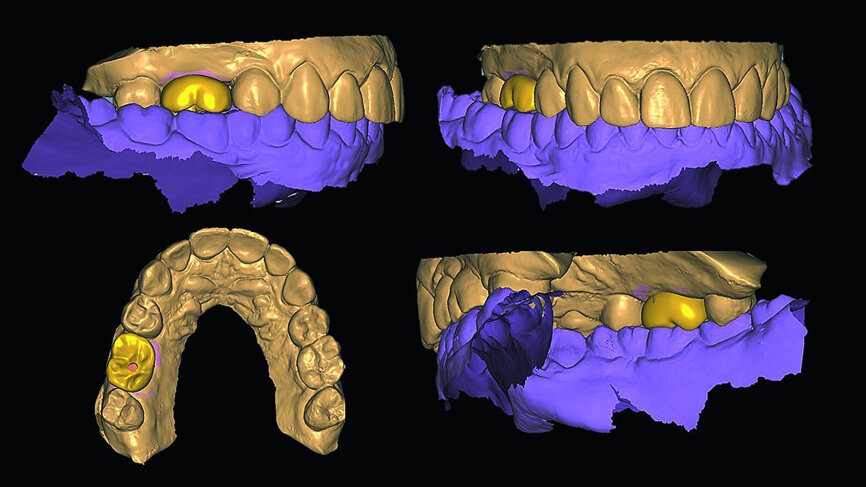
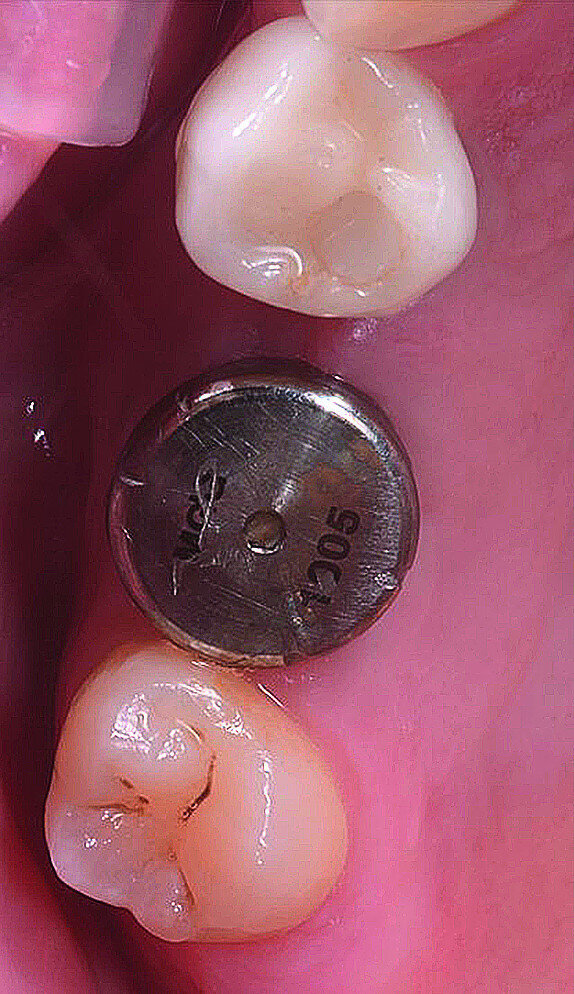
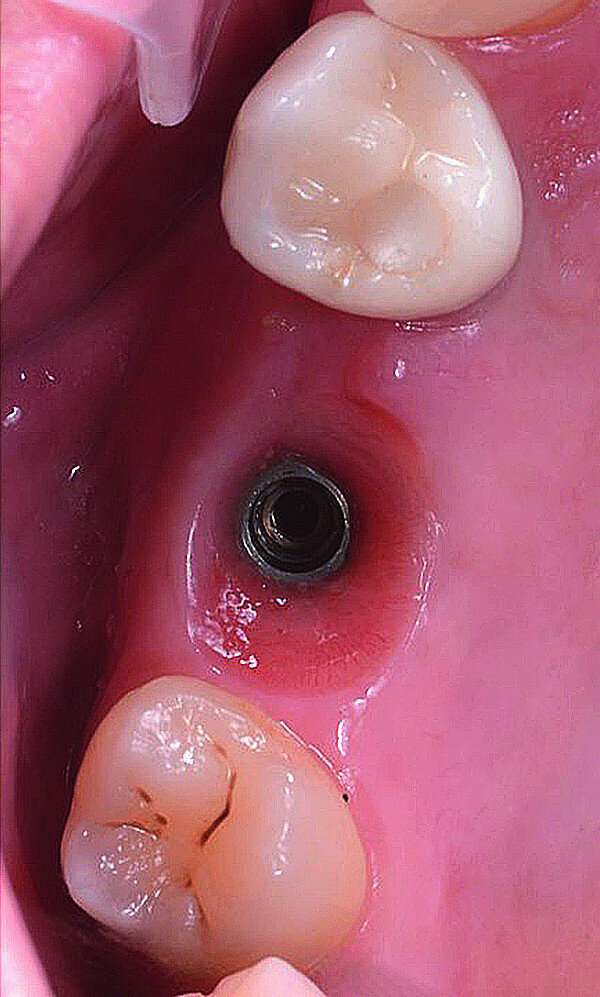
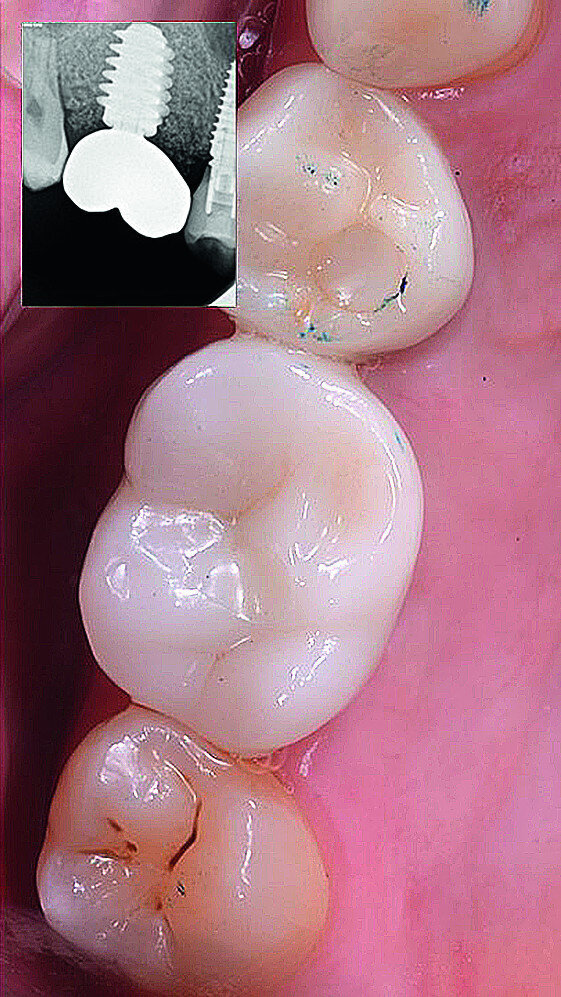
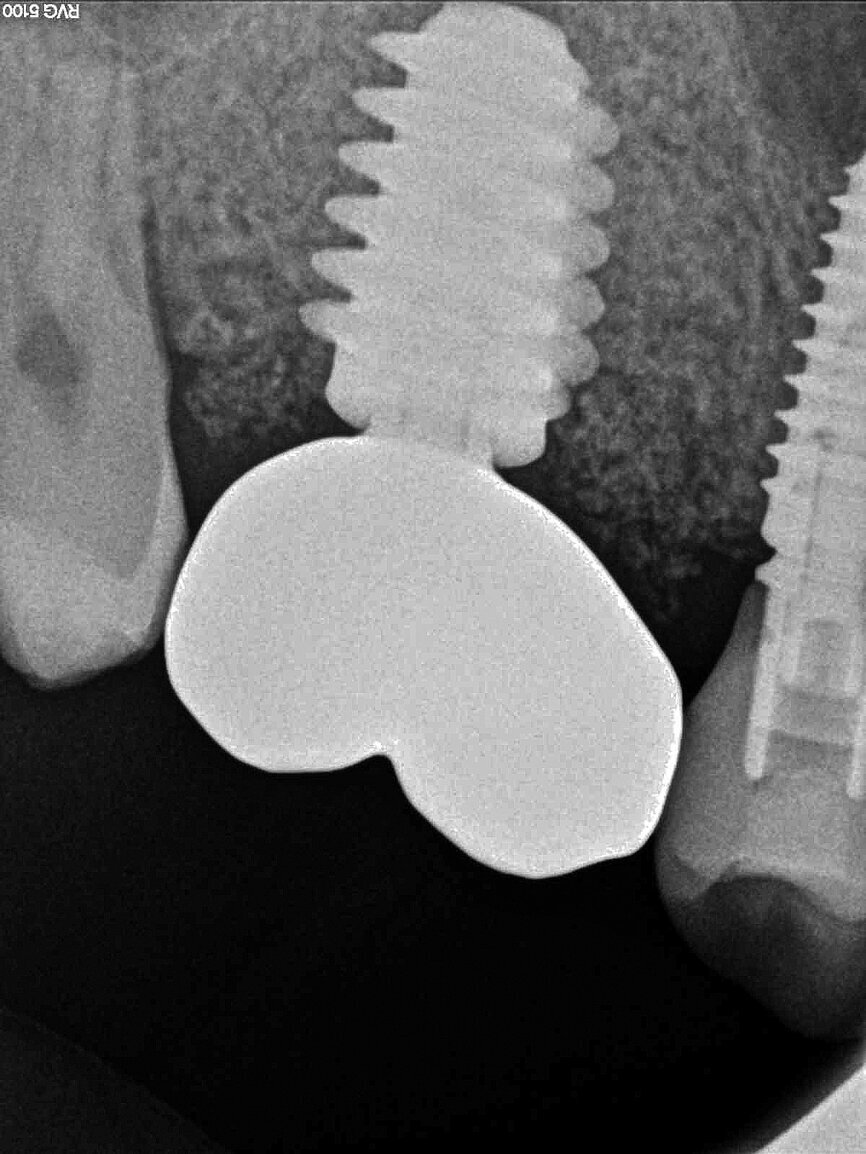
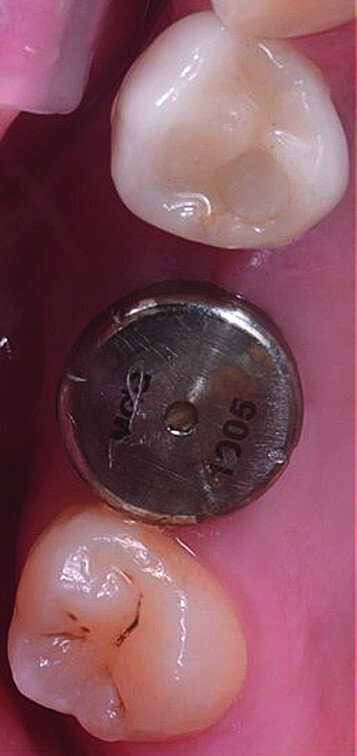
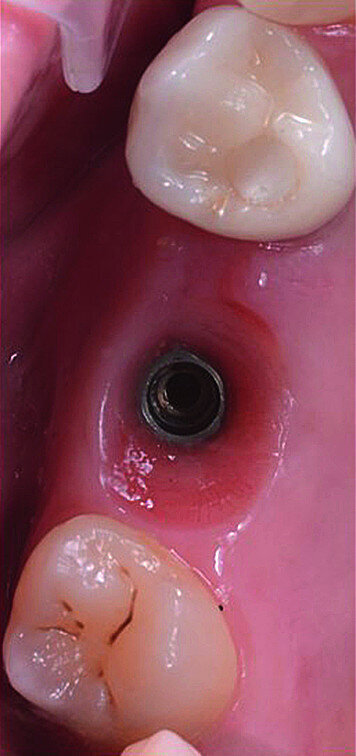
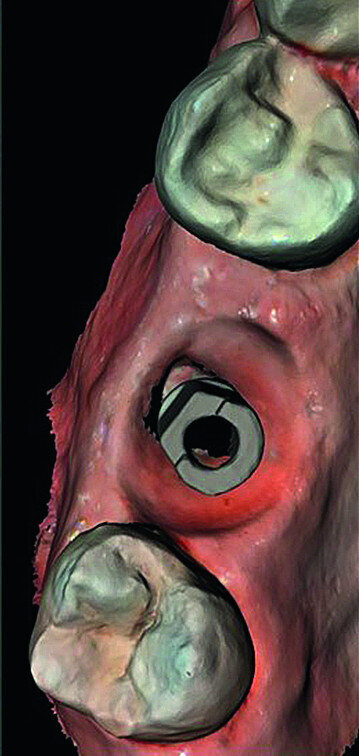
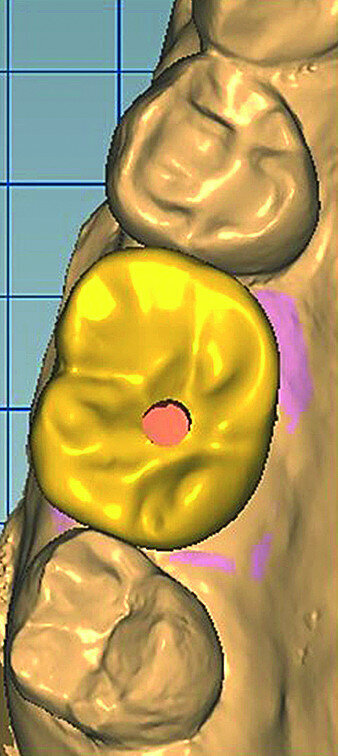
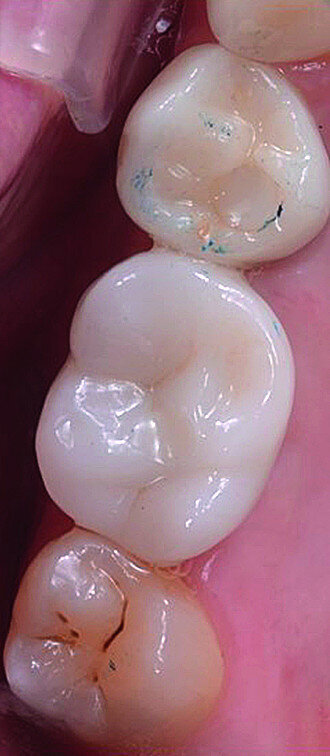
In March 2018, four months after the surgery, the prosthetic phase was started. An impression was taken with an intraoral scanner (CS 3600, Carestream Dental) using scan bodies for an impression at the implant head (MegaGen; Figs. 11a & b). The information was sent to the Anatomic Lab, where a crown was designed using a CAD programme. After the design of the crown had been finished, the information was sent to a milling machine (Amann Girrbach) and the crown was milled (Fig. 12). One week after the preparation, the definitive crown in monolithic zirconia was attached and the occlusion tested using T-Scan technology (Tekscan; Figs. 13a–c & 14).
Discussion
The main success indicator for dental implants is primary stability, which is one of the prerequisites for achieving osseointegration. [1] This is affected by factors such as bone quantity and quality, surgical placement procedure, and implant shape and coating. [2]
This stability can be measured with a device that analyses the resonance frequency of the implant after its placement. The software converts the received hertz waves to a numerical value called ISQ on a scale ranging from 1 to 100. The manufacturer’s instructions suggest that a stable implant has an ISQ higher than 65 and an unstable implant less than 50. [3] However, these values differ from one author to another. Nowadays, we have several options that can help us achieve a successful rehabilitation with implants. One of them is the use of a fibrin membrane rich in platelets (PRF). This has the ability to reduce the healing period and improve bone regeneration. The use of PRF as a covering membrane allows rapid epithelisation of the site surface and represents an effective barrier against the penetration of epithelial cells within the bone defect. [4]
Öncü and Alaaddinoğlu evaluated the impact of implant coating with L-PRF (leukocyte- and platelet-rich fibrin). [5] The stability of the implant was measured by ISQ. [5] The use of L-PRF in the implant insertion resulted in statistically significant ISQ values that continuously increased over time. Boora et al. reported early bone remodelling around implants coated or not with L-PRF at the insertion. [6] Implants coated with L-PRF showed 50 per cent less initial bone loss after both one and three months, respectively. [7]
Nowadays, centrifugation protocols have been optimised, called the low speed concept of centrifugation, resulting in A-PRF and i-PRF. These new protocols seek to obtain a greater number of platelets, in order to increase the healing capacity, and leucocytes, therefore also increasing the regenerative capacity. [8]
Furthermore, positive effects on bone regeneration and implant surgery have been suggested when PRF is applied. Given its ease of preparation, low cost and biological properties, PRF can be considered as a reliable treatment option. [7] Although the application of PRF during implant placement or for the treatment of peri-implant defects is quite recent, several studies have already shown clinical benefits, such as higher ISQ values and marginal bone resorption. [7]
Another technique that has proven to be an asset in the success of oral rehabilitation with implants is ozone therapy. This ozone-based tool has an antibacterial effect resulting from the oxidative action on cells, damaging the cytoplasmic membranes of certain organisms, such as bacteria, viruses, fungi and parasites, without, however, the ability to damage healthy human cells. [9, 10] Thus, ozone has the following advantages: accelerates the healing of soft tissue (increases the rate of physiological healing), controls opportunistic infections, reduces scarring time after extraction (forms a pseudomembrane over the alveolus and protects it from physical and mechanical aggression) and aids in bone regeneration. [10 – 12] The literature suggests that the post-extraction socket must be prepared conventionally and disinfected with ozone for about 40 seconds, followed by placement of the implant. In this way, we avoid infections and improve bone regeneration. [10, 13] A further study showed that in ozone-treated implants there was regeneration of periodontal cells similar to those around natural teeth. [10, 14]
In modern digital dentistry, the four basic phases of work are image acquisition (through scanning), data preparation/processing (through CAD software), production (CAM systems), and clinical application on patients. [15] The dental preparation can be scanned outside the oral cavity, on the plaster model, or inside the oral cavity by an intraoral scanning system. [16]
Optical impressions have several advantages over conventional impressions. Among them, the most important is the reduction of patient stress and discomfort. Moreover, they are time-efficient and can simplify clinical procedures for the dentist, especially for complex impressions (in patients with undercuts and/or in oral implantology, when multiple implants are present). In addition, optical impressions eliminate plaster models, saving time and space, and allow for better communication with the dental technician. Finally, optical impressions improve communication with patients and are therefore a powerful marketing tool for the modern dental clinic. [17, 18]
Regarding accuracy as compared with conventional impressions, optical impressions are equally accurate for individual restorations or three- to four-unit bridges on natural teeth and on implants. Conversely, conventional impressions still appear to be the best solution currently for long-span restorations, such as fixed full prostheses on natural teeth and implants (with a higher number of prosthetic abutments). [17] Significant differences in trueness have been found among different optical impressions. For each scanner, the trueness was higher in a partially edentulous model than in a fully edentulous model. [19]
Conversely, the disadvantages of using optical impressions are the difficulty in detecting deep margins in prepared teeth and in the case of bleeding, the learning curve, and the purchasing and maintenance costs. [17]
Nowadays, we also have the possibility to superimpose the information related to the teeth and gingivae, received from the intraoral scan, over the bone-related information acquired with CBCT. It is therefore possible to plan the optimal positioning of implants with software to guide the surgery. Planning data is transferred to a surgical template that can be physically fabricated in various ways and with different materials. This guide will help the surgeon correctly position the implants without needing to raise a flap. [18]
After obtaining the digital model, we proceed to the preparation of the virtual part through the CAD software that defines the geometry of an object, while CAM programming directs the fabrication process. [20] The CAD/CAM process eliminates current conventional processes, such as the melting and subsequent manipulation of the material after the mechanical working of the same. Pieces made by the CAD/CAM process have a more precise fit compared with conventional methods for dental prosthetic manufacture.[21]
The main concern with CAD/CAM restorations lies in the marginal fit. However, nowadays CAD/CAM parts show an adaptation with gaps of only around 40 μ. [16, 22, 23]
Conclusion
The use of new technologies in dentistry, such as the application of PRF, ozone therapy and intraoral scanners, has contributed significantly to the success of rehabilitation with dental implants, reducing the time for implant placement and for their restoration.
Editorial note: A list of references is available from the publisher. This article was published in CAD/CAM—international magazine of digital dentistry No. 03/2018.
Tags:
As an oral surgeon and prosthodontist specialising in full-mouth rehabilitation, I have consistently sought to integrate advanced technologies into my ...
In March last year, Dr Ahmad al-Hassiny, director of the Institute of Digital Dentistry, noted that over 90% of US dental laboratories and nearly 50% of ...
Modern dentistry is undergoing a technological revolution, driven by the integration of advanced digital tools in diagnostics, planning and treatment. Among...
“Digital Workflow” has become an established term in present-day dentistry, helping to solve problems in dental technology which would have been...
Modern dentistry should strive to preserve all maintainable natural teeth whenever possible, in line with the principles of minimal invasiveness and ...
This year, the International Dental Show’s (IDS) centenary year, the 40th edition of IDS, the world’s leading trade fair for dentistry, will focus on ...
Successful immediate implant placement associated with immediate loading remains one of the greatest clinical challenges. In addition to the placement of an...
In recent years, the field of dentistry has undergone a profound transformation with the widespread adoption of digital technologies, particularly in the ...
CZĘSTOCHOWA, Poland: Pixel Clinic is a modern dental clinic in Poland with a strong focus on aesthetics and digital workflows. At the clinic, the most ...
FREIBURG, Germany: In order to offer dental professionals the opportunity to enhance their skills in reconstructive dentistry with digital solutions, the ...
Live webinar
Thu. 30 April 2026
1:00 pm EST (New York)
Live webinar
Sun. 3 May 2026
12:00 pm EST (New York)
Dr. Rickard Brånemark MSc, MD, PhD, Dr. Robert Gottlander DDS
Live webinar
Sun. 3 May 2026
8:00 pm EST (New York)
Live webinar
Tue. 5 May 2026
10:00 am EST (New York)
Live webinar
Tue. 5 May 2026
12:00 pm EST (New York)
Live webinar
Tue. 5 May 2026
1:00 pm EST (New York)
Dr. Maximilian Dobbertin M.Sc
Live webinar
Tue. 5 May 2026
3:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East

































To post a reply please login or register