Successful immediate implant placement associated with immediate loading remains one of the greatest clinical challenges. In addition to the placement of an implant immediately into the socket, the creation of an immediate screw-retained CAD/CAM temporary restoration is critical for an optimal aesthetic outcome. When using a conventional approach, the procedures require an extensive number of patient appointments and chair time for the dentist and the patient. Fortunately, nowadays digital workflows can be implemented, allowing treatments to be considerably shortened.
This case report describes how a full-arch rehabilitation employing digital planning (coDiagnostiX, Dental Wings) and guided surgery with the Straumann system to provide immediate implant placement and immediate screw-retained CAD/CAM provisionalisation led to an outstanding treatment outcome. The digital workflow allowed us to develop an efficient and predictable treatment protocol for the immediate implant placement and the prosthetic design, including the individual emergence profiles prior to the surgery. This also led to an excellent patient experience and satisfaction. The goal of this clinical report is therefore to introduce an innovative one-surgery approach for immediate screw-retained CAD/CAM provisionalisation by using the latest technological improvements in prosthetic and surgical planning software and seamlessly integrating the dental technician into the development of the digital treatment planning and new prosthetic options.
Initial situation
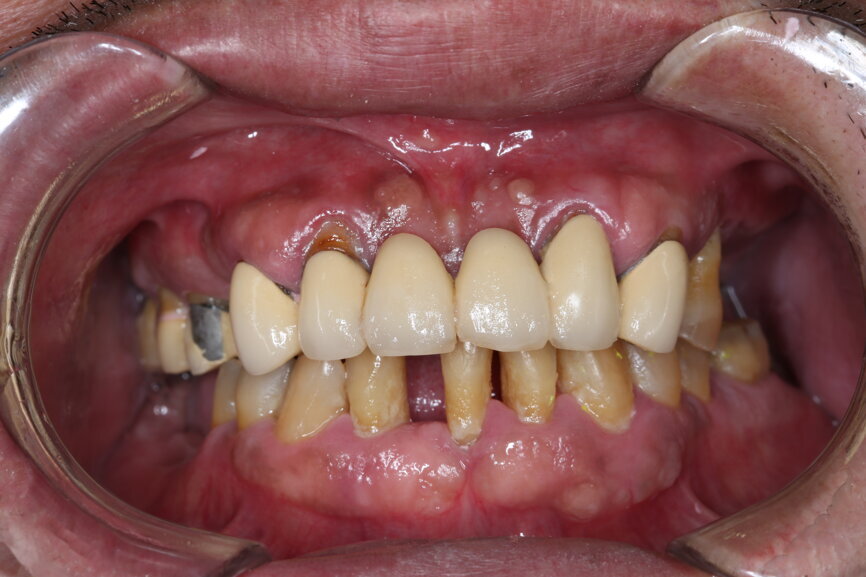
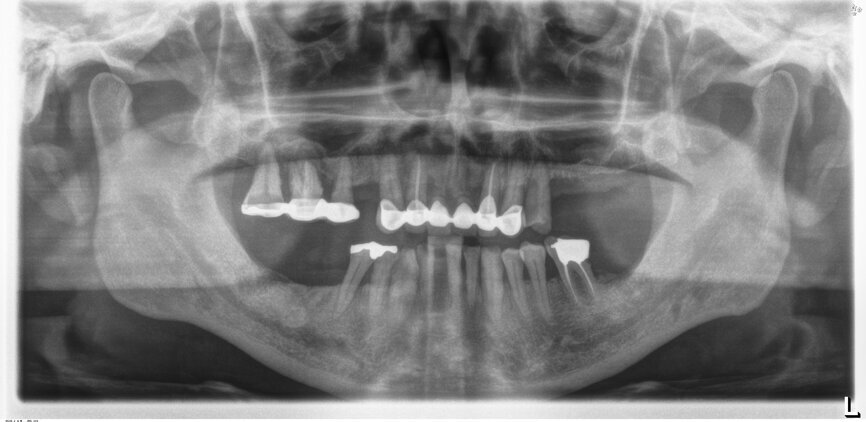
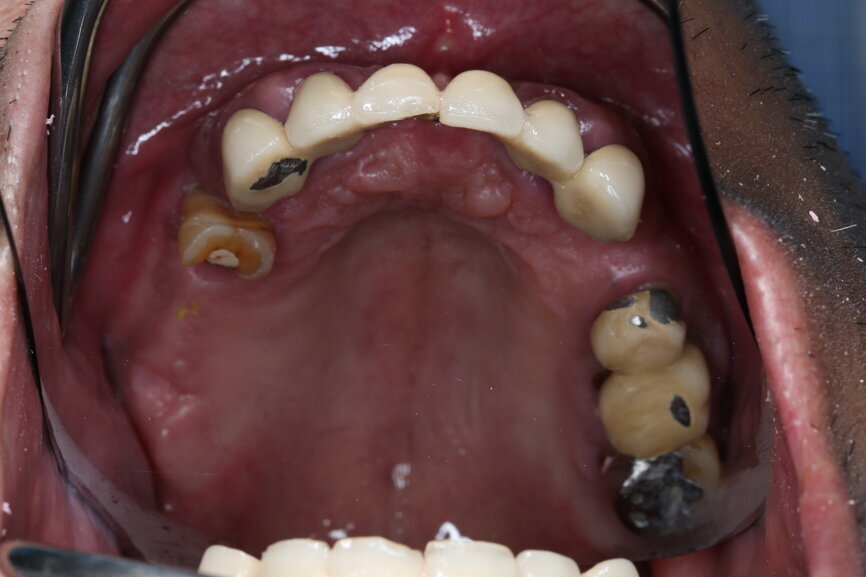
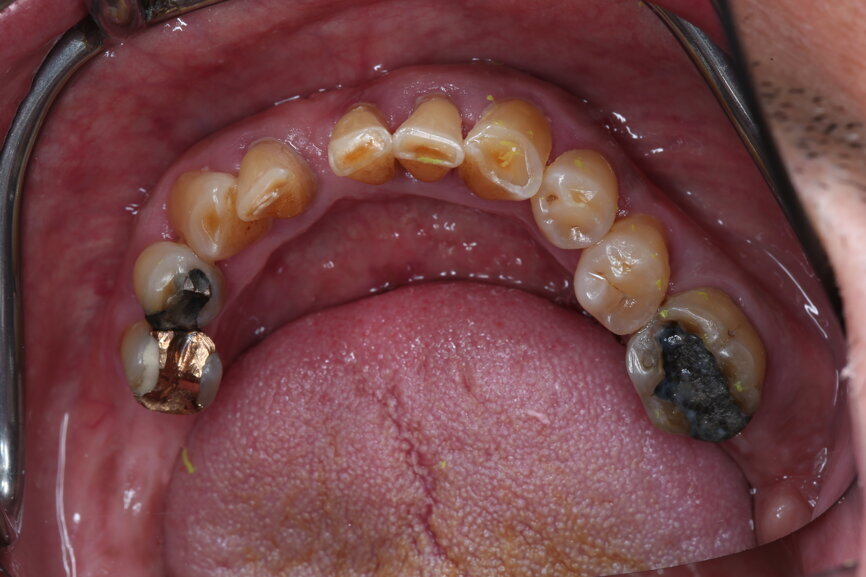
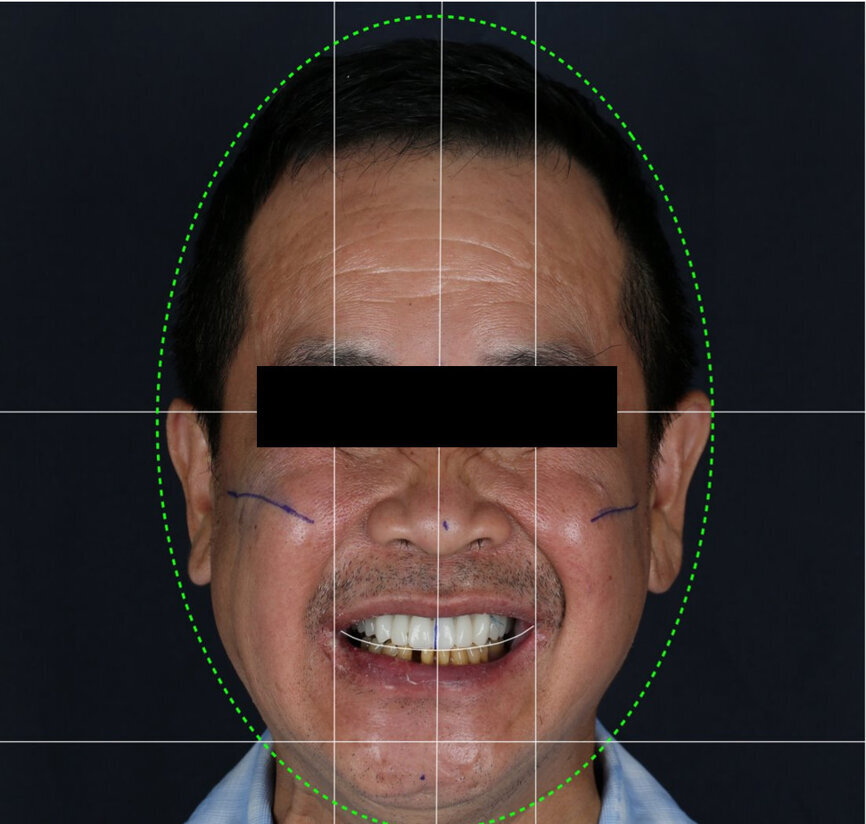
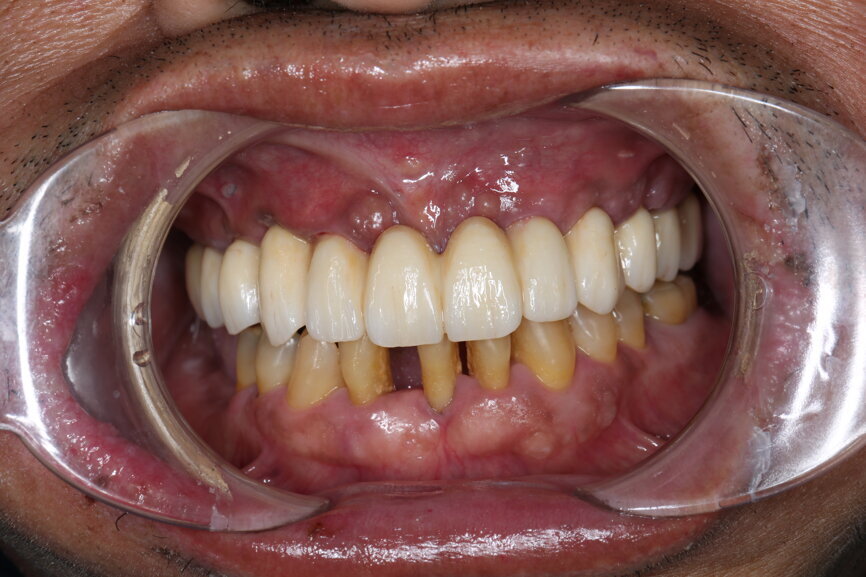
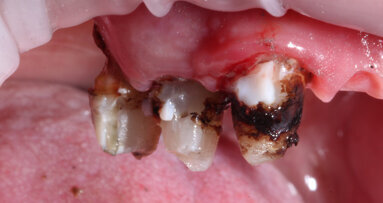
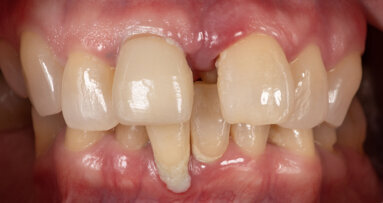
A 51-year-old male patient who was a smoker (< 10 cigarettes per day) and in good general health presented to the clinic with missing molars in the second and fourth quadrants, Grade III mobility of teeth #24 and 17, decayed roots and gingival inflammation, and without abscess or sinusitis of tooth #16. The anterior zone showed different extents of recession, bone resorption and deep periodontal pockets around teeth #12 and 22, which led to the patient complaining about an aesthetically unsatisfying restoration (Figs. 1 & 2).
Treatment planning
After the clinical and radiographic assessments, the patient was offered two different treatment options. The first one would include the maintenance of the maxillary canines by treating their recession and bone resorption, which had exposed more than half of the roots, implant placement in the maxillary incisor region with soft-tissue grafting, and extraction of the remaining maxillary posterior teeth and implant treatment after guided bone regeneration and sinus lift. Moreover, the definitive restoration would be an implant-supported bridge in regions #14–16, 12–22 and 24–26 and crowns on teeth #13 and 23 after three months.
The second treatment option would entail extraction of all the remaining maxillary teeth and restoration of the full arch according to the Straumann Pro Arch concept. This would entail placement of four Straumann BLX implants immediately after extraction in regions #15, 12, 22 and 25 employing a fully digital approach and guided surgery and placement of a preoperatively fabricated screw-retained CAD/CAM restoration that would be functional and aesthetic right after surgery and a definitive restoration placed six to 12 months later.
The first option would take one year and eight months to complete, resulting in a higher number of visits, longer chair time and higher costs in comparison with the second option. The reliable and short treatment protocol and the patient’s unavailability for clinic visits for a considerably long period led to the patient choosing the second option. A holistic treatment approach for the mandibular dentition was envisioned; however, the COVID-19 situation forced a delay in treatment.
Implant placement planning
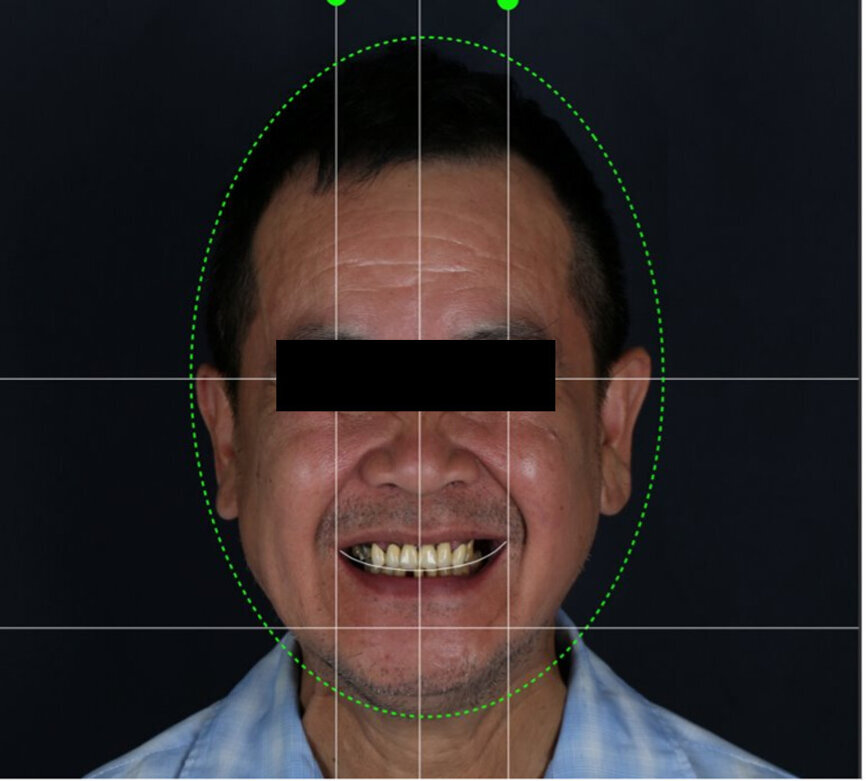
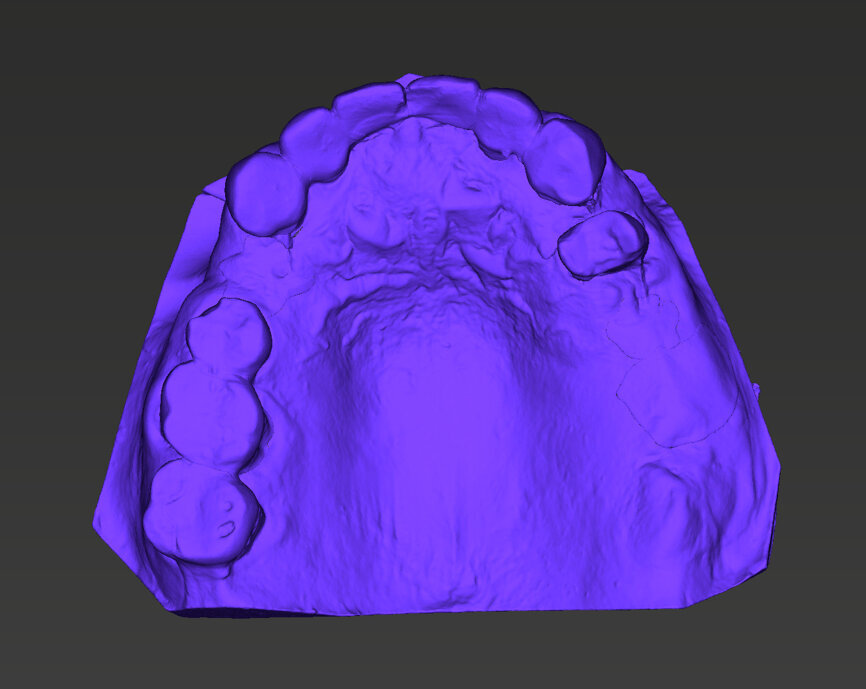
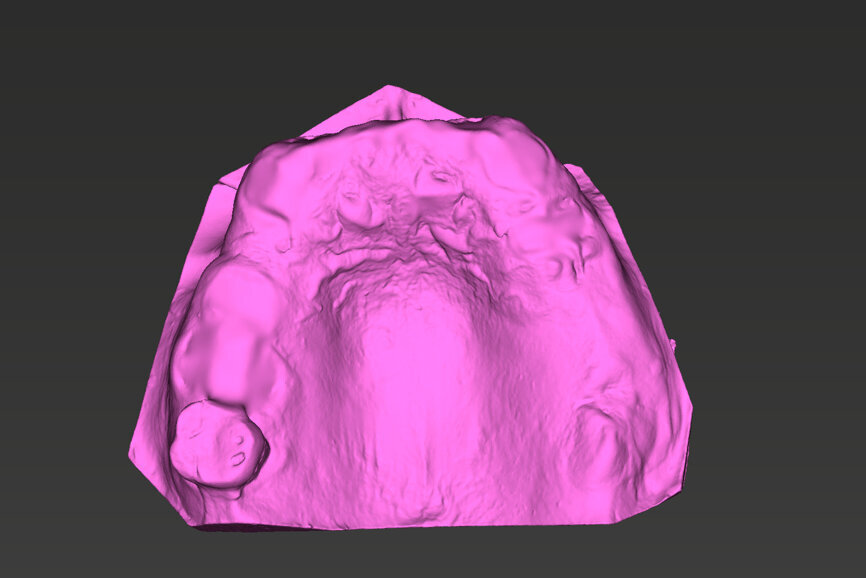
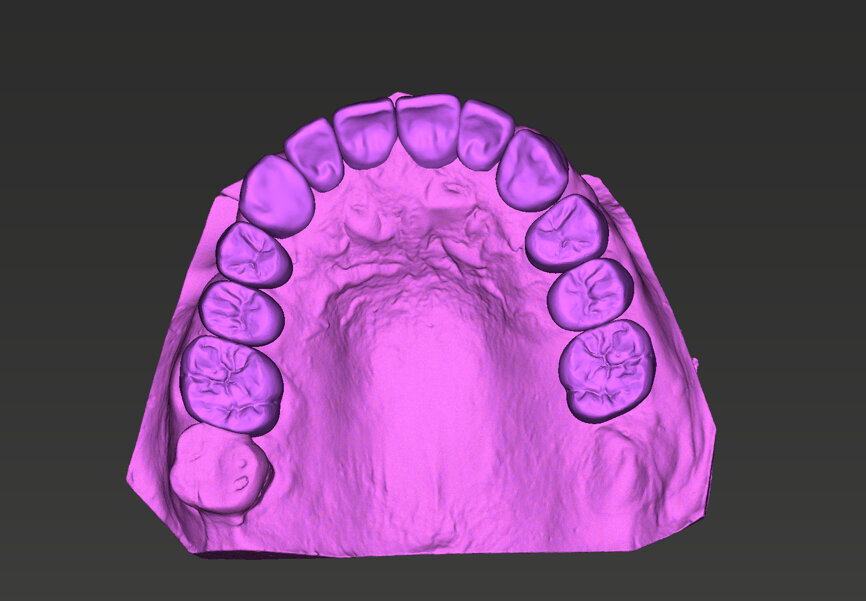
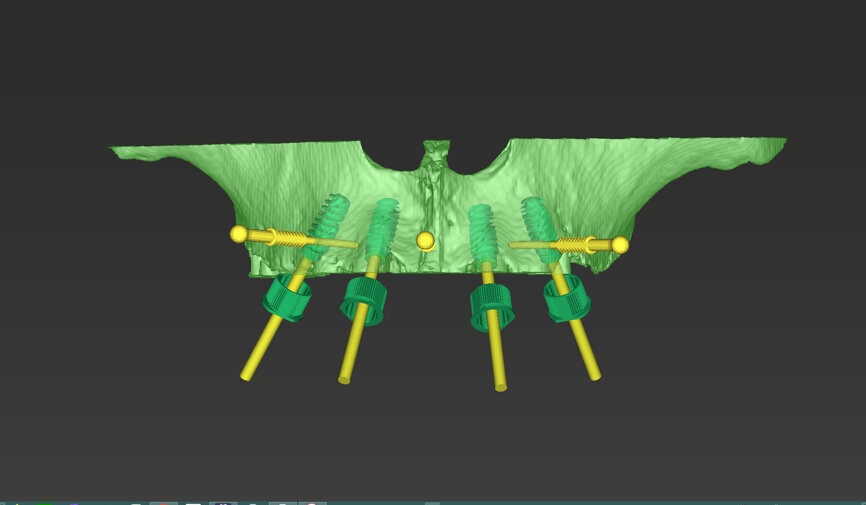
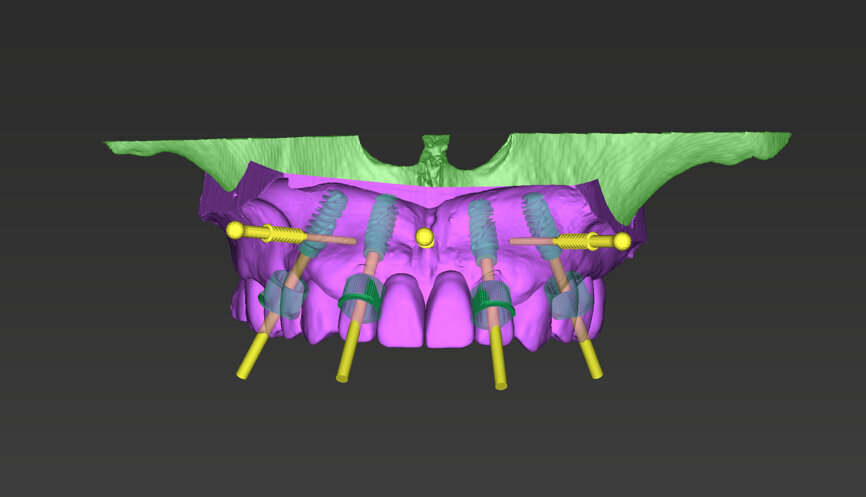
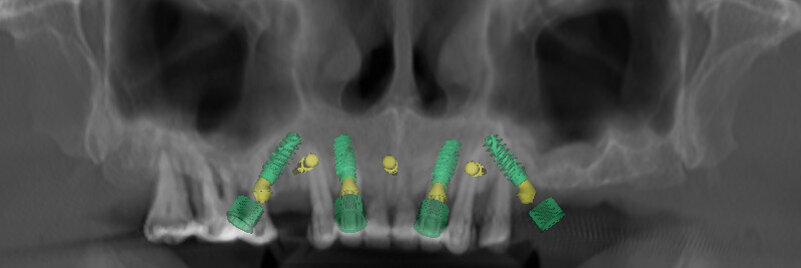
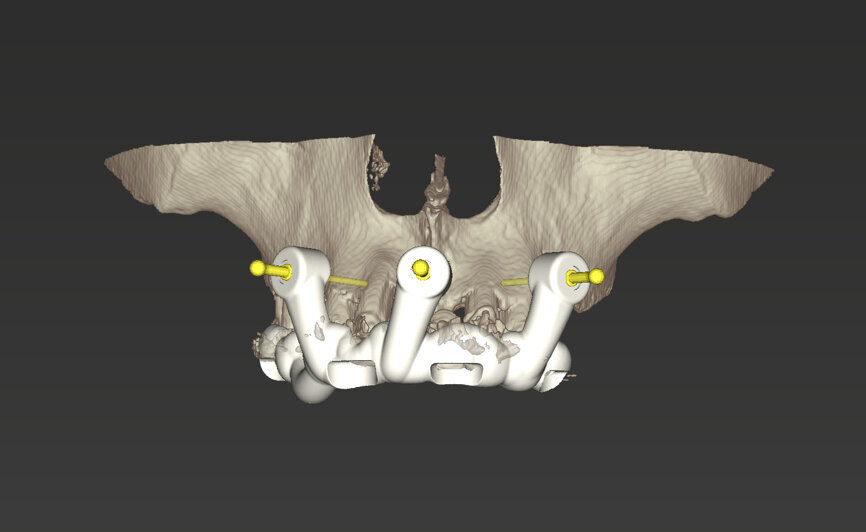
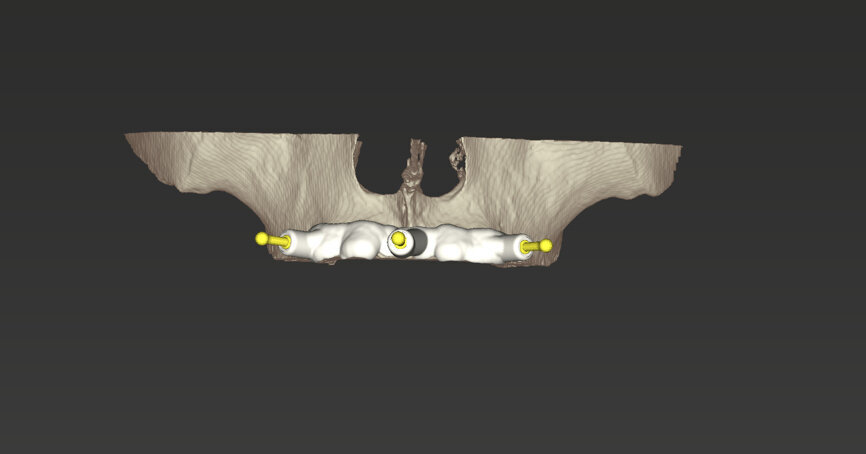
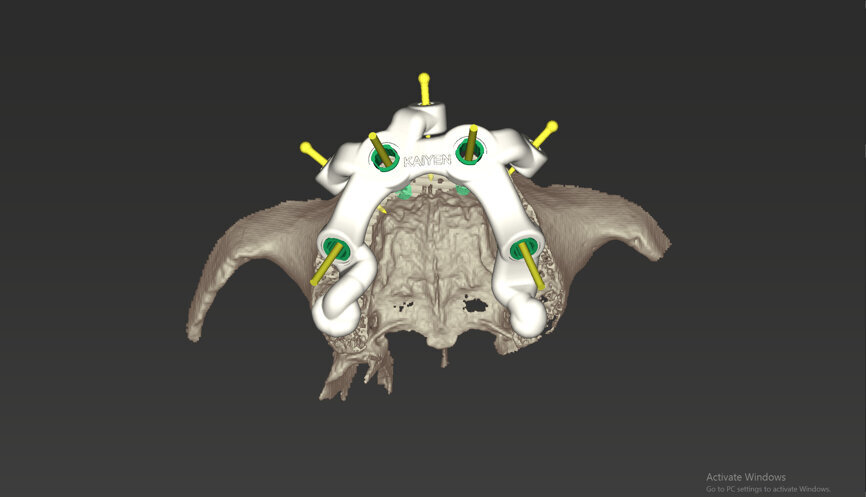
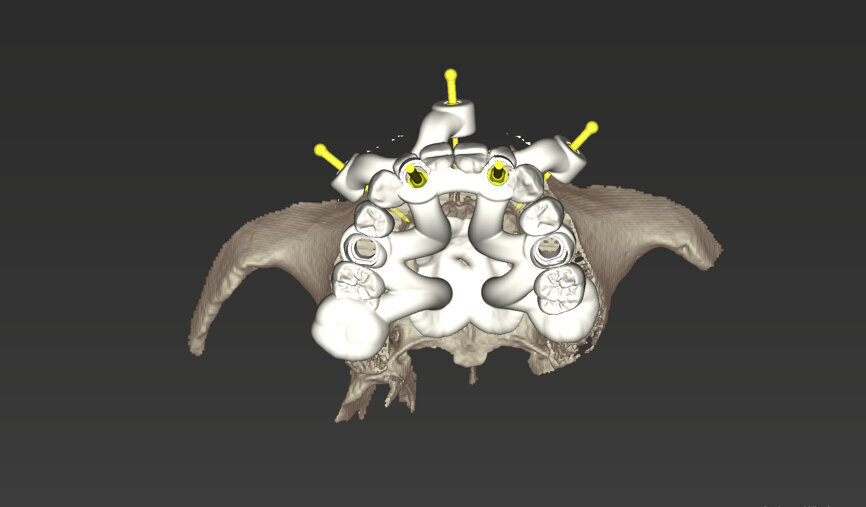
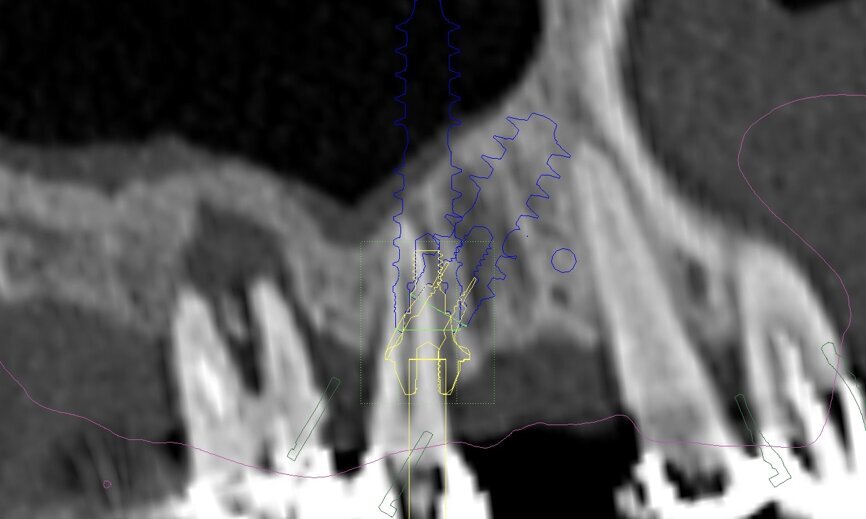
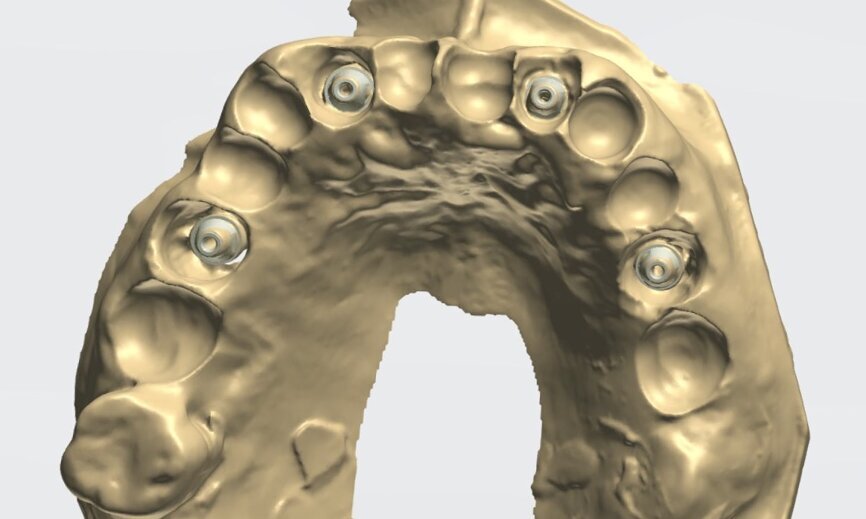
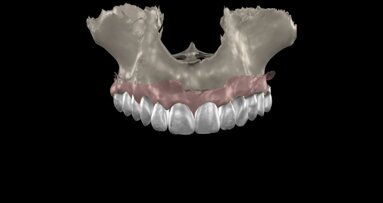
An intra-oral scan was taken to record the patient’s current oral situation, and the resulting STL file and the DSD fil (2D smile design image) were used to create the future prosthetic design with software for the laboratory (Figs. 3–6). The 3D radiographic DICOM data and the prosthetic design project STL file were superimposed in coDiagnostiX (Figs. 7–9) The fixation pin guide, bone reduction guide, surgical guide and bite registration guide were designed with coDiagnostiX (Figs. 10–13) and produced using 3D printing technology.
Prosthetic design planning
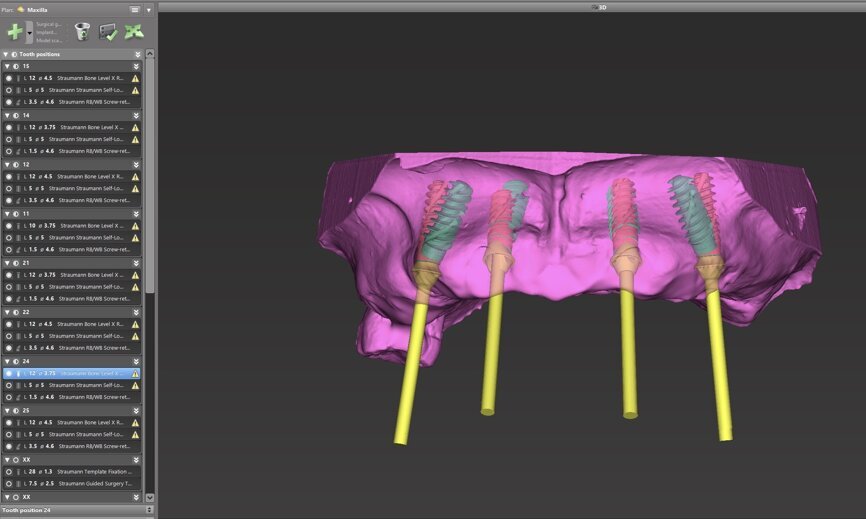
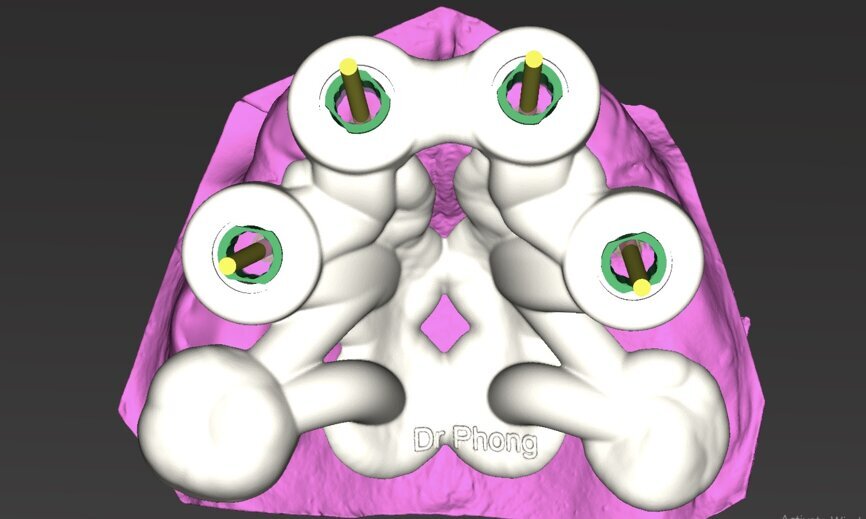
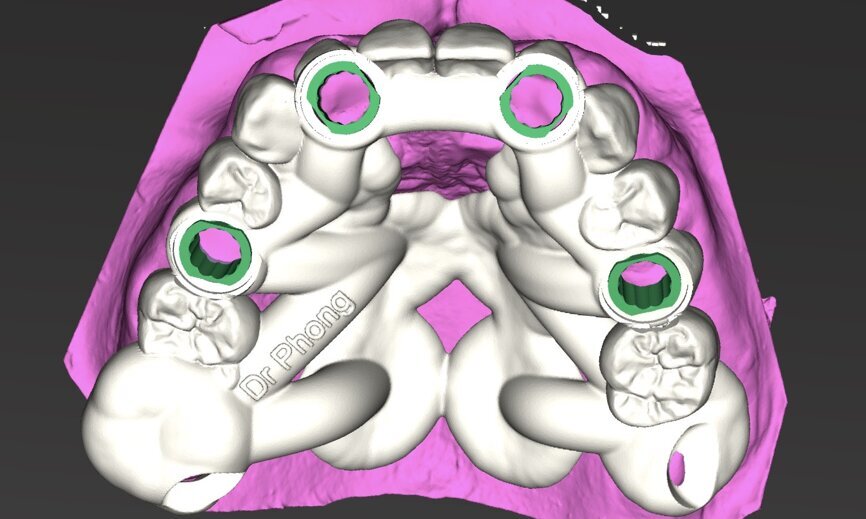
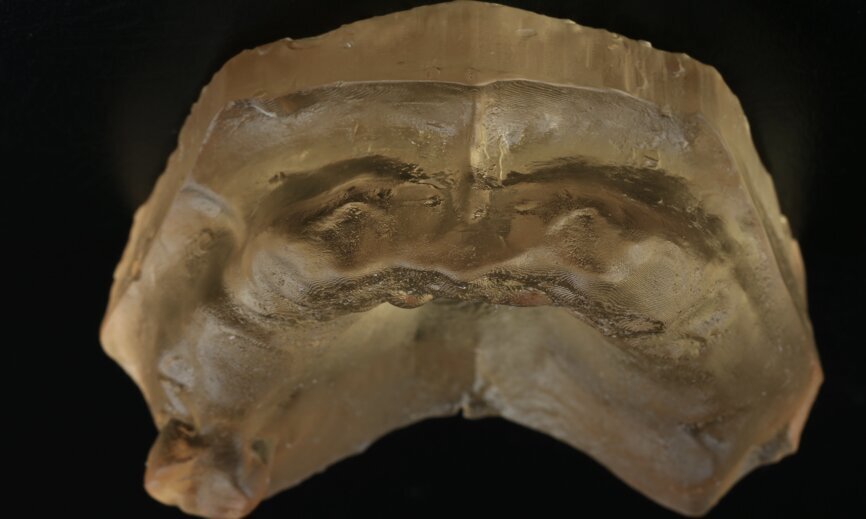
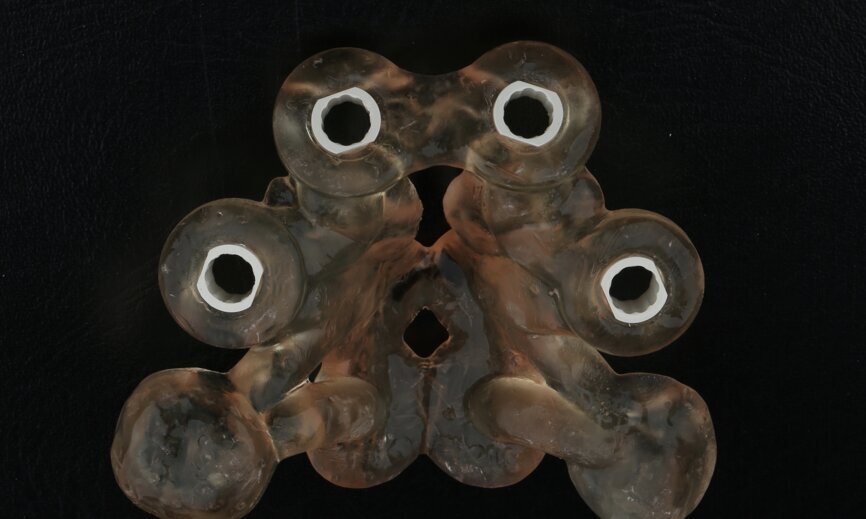
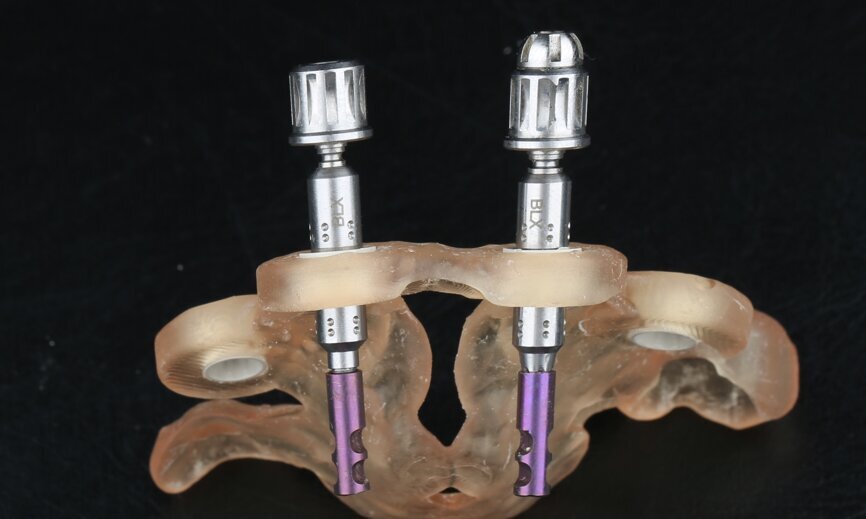
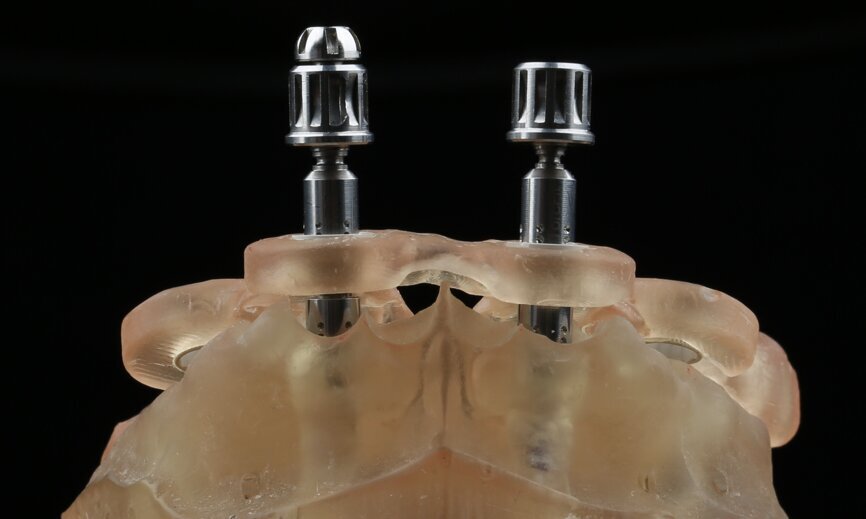
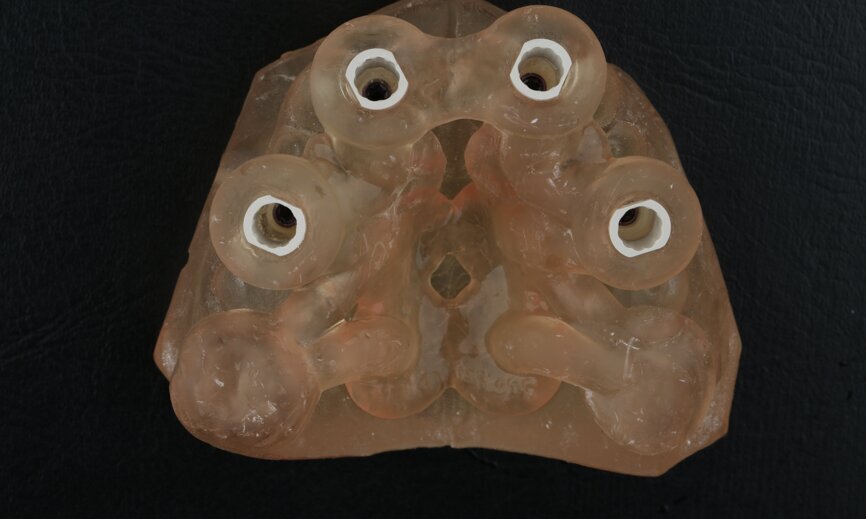
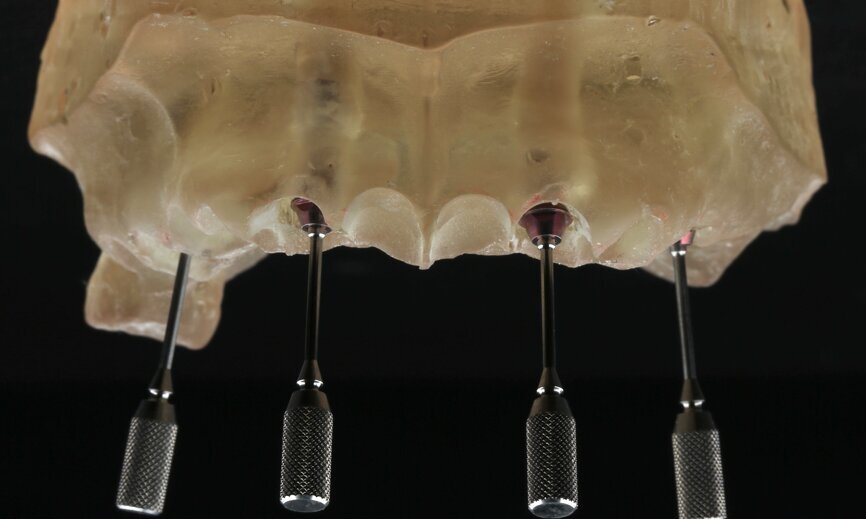
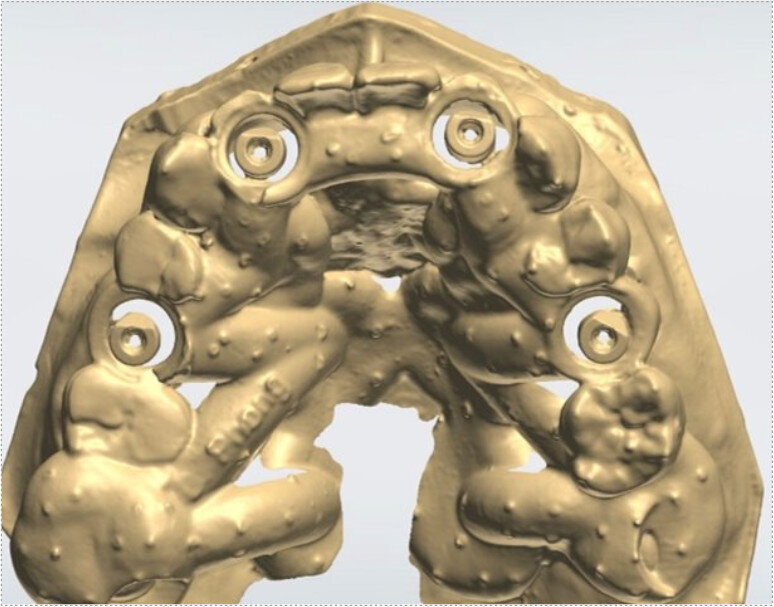
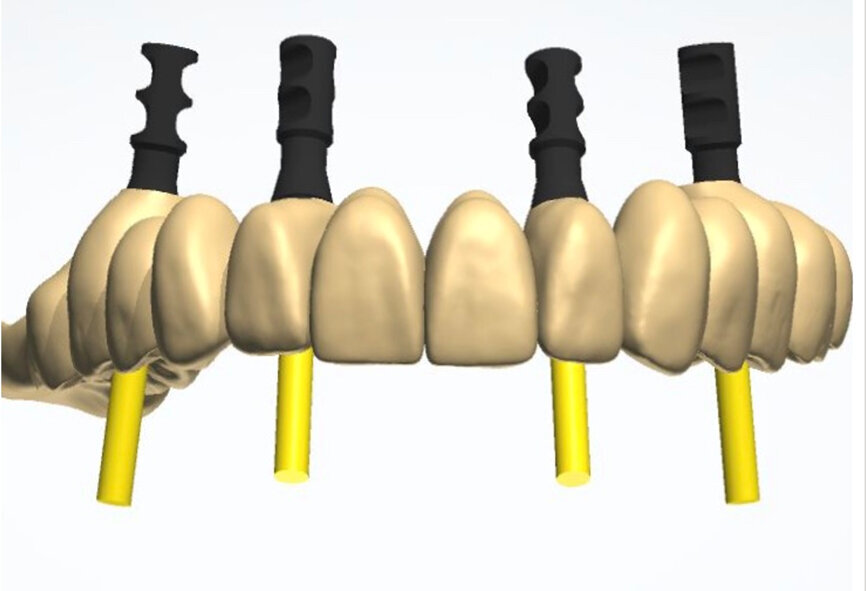
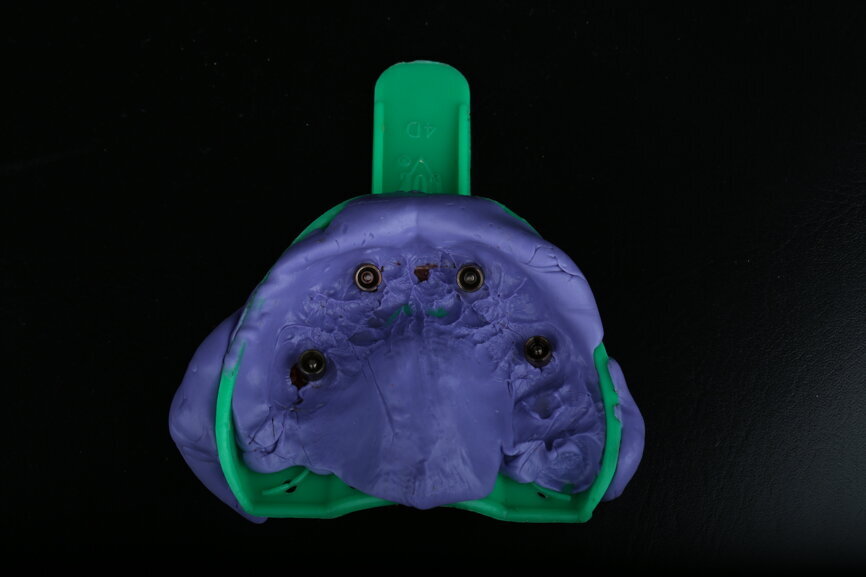
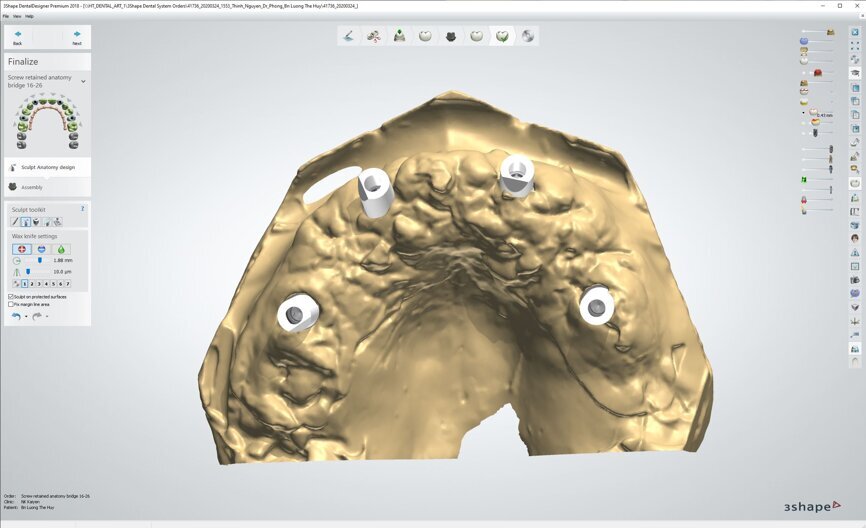
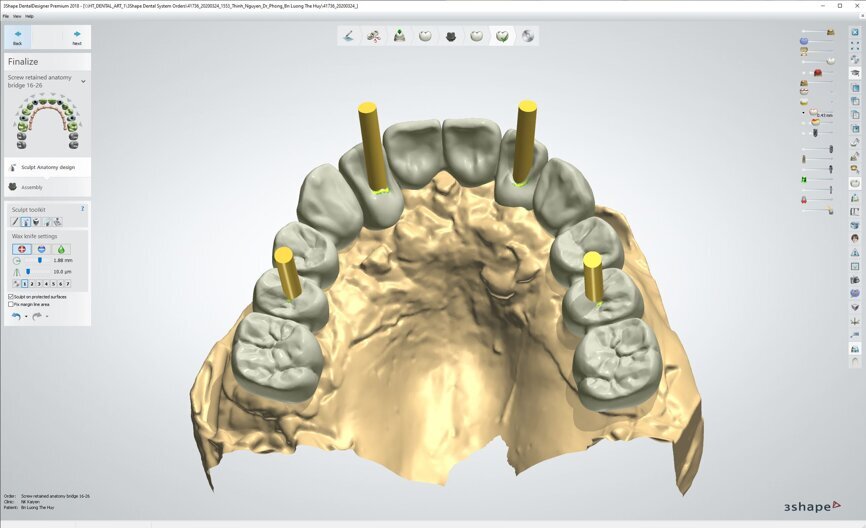
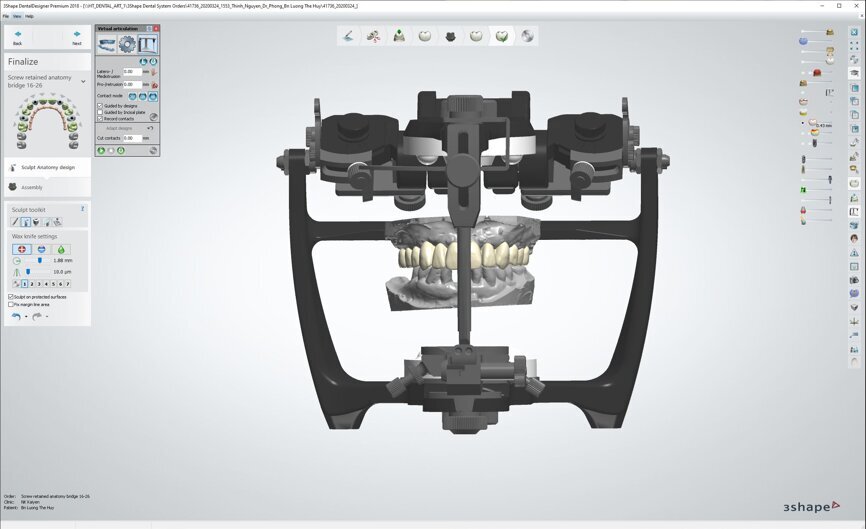
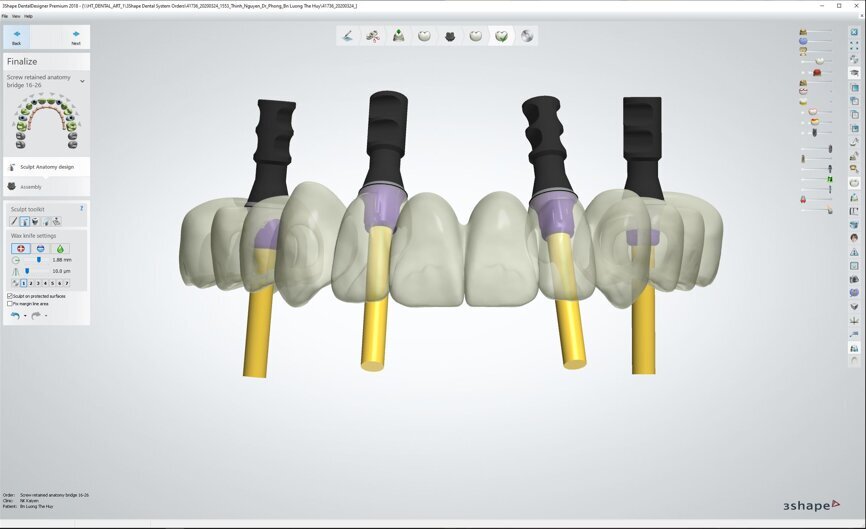
To design the prosthesis digitally, we first selected the screw-retained abutment (SRA) angle and gingival height (Fig. 14) and then we created the patient model on which we could connect the BLX implants with the SRAs selected from the Straumann library (Fig. 15). The implant placement guide was on the model, leveraging the high stability that we could gain from palatal support (Figs. 16 & 17). After printing the model, the BL implant analogues were positioned using the template for navigation. The digital planning using coDiagnostiX (Version 9.14) allowed the dental technician to identify all the necessary parameters related to implant position (Figs. 18–22). Emergence profiles were set-up on the model (Fig. 23). The model was scanned using scan bodies, and a CAD/CAM temporary restoration was designed and milled in a PMMA-based restorative material (Figs. 24–29).
Guided surgery
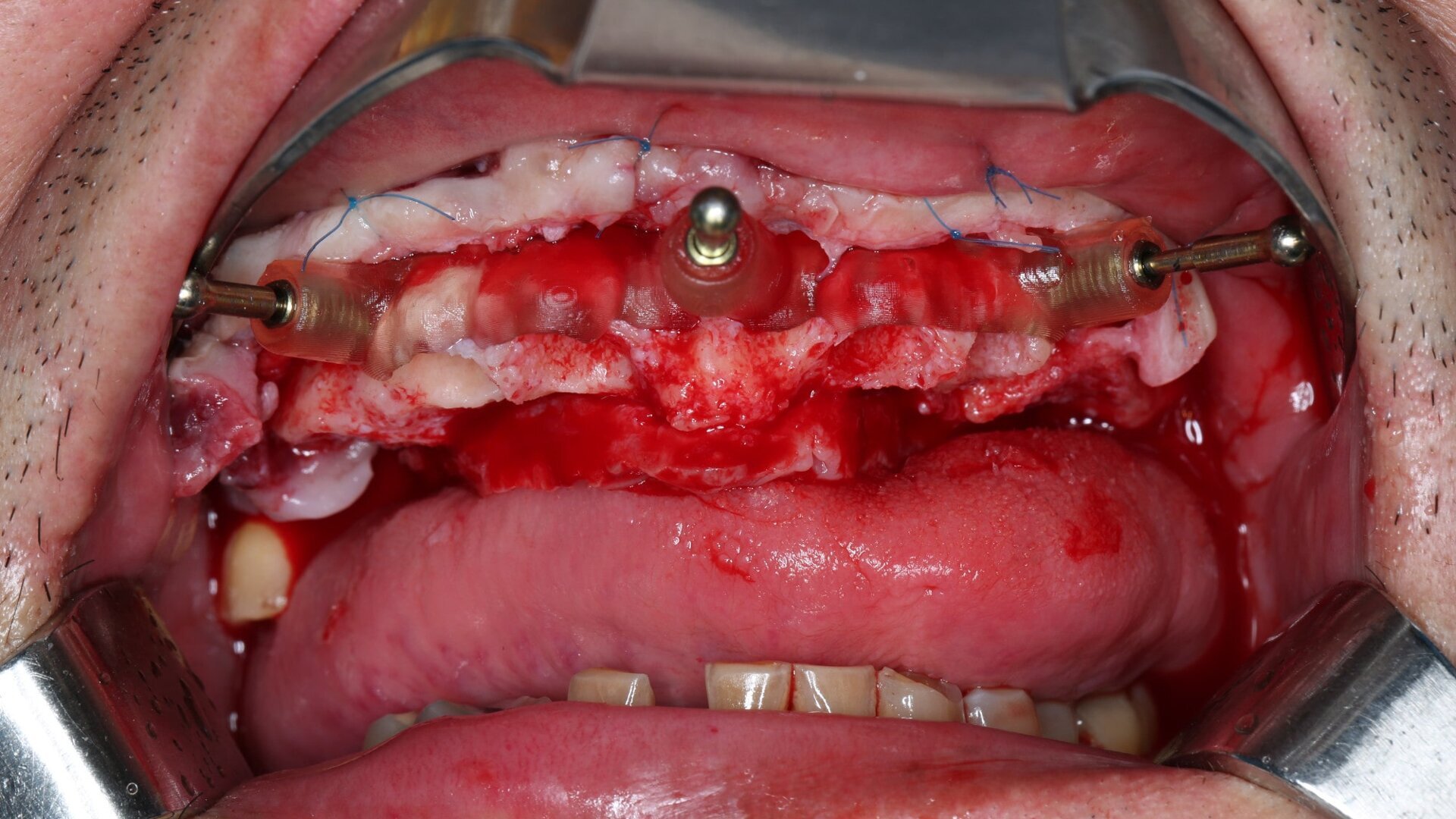
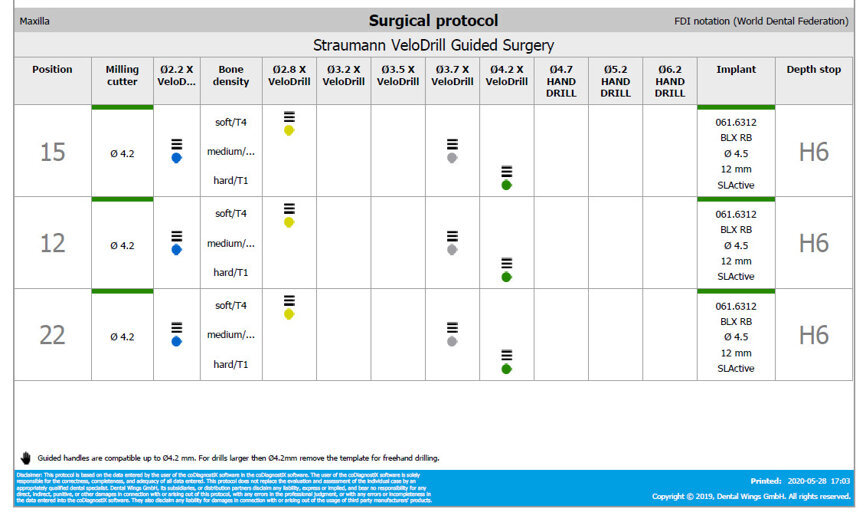
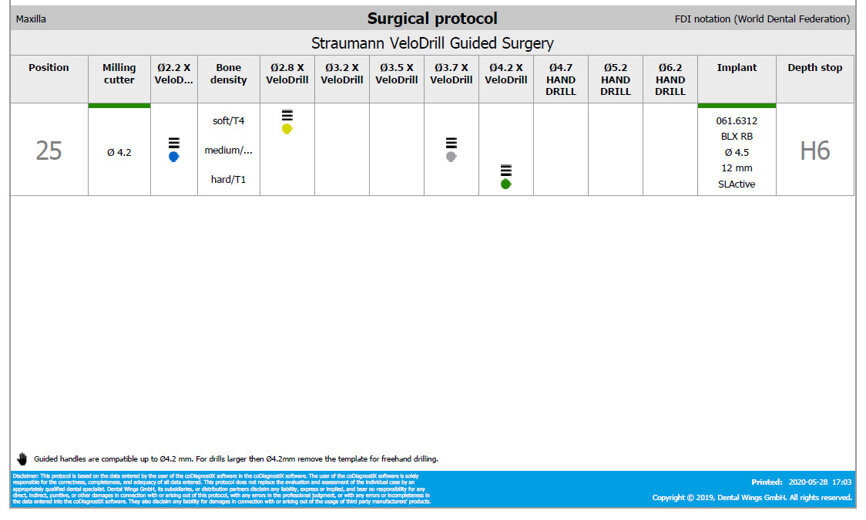
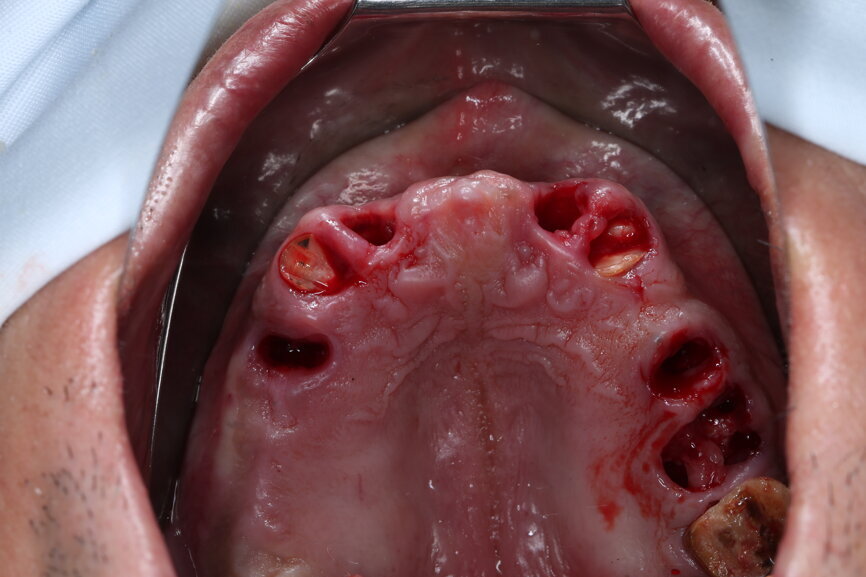
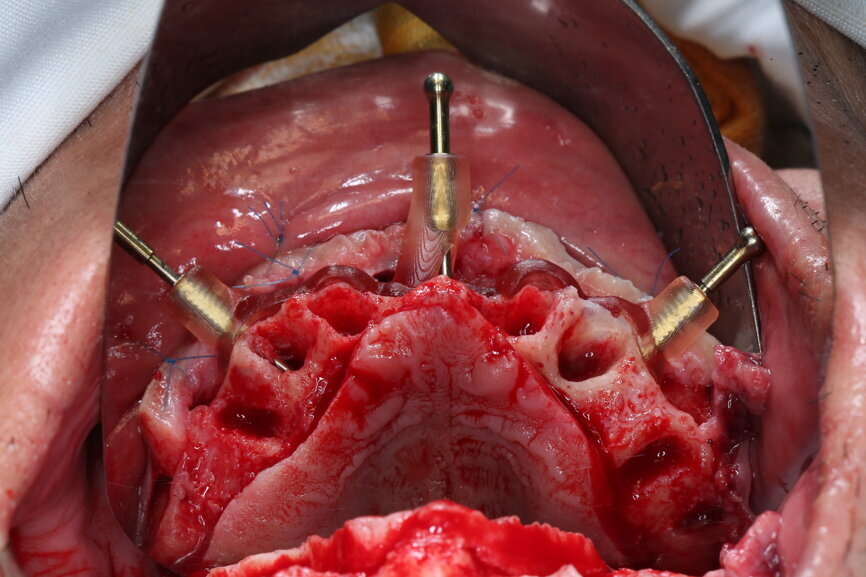
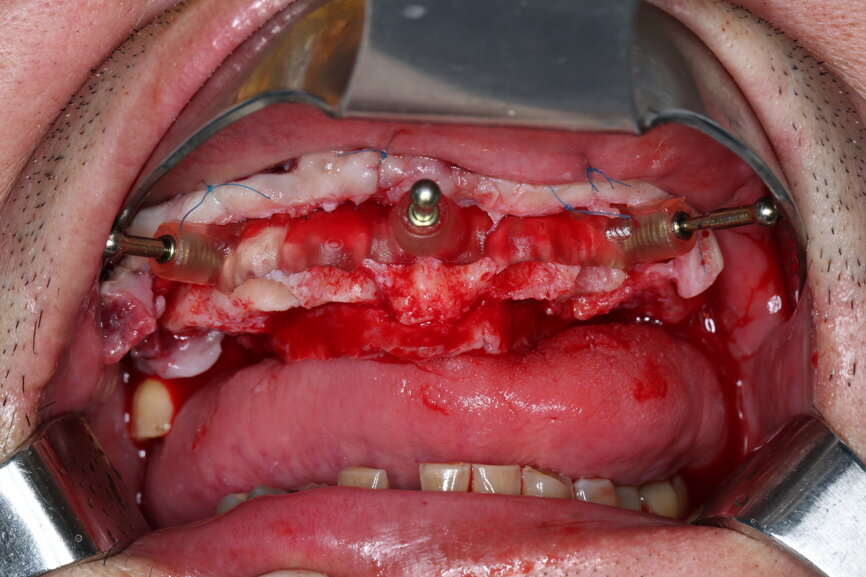
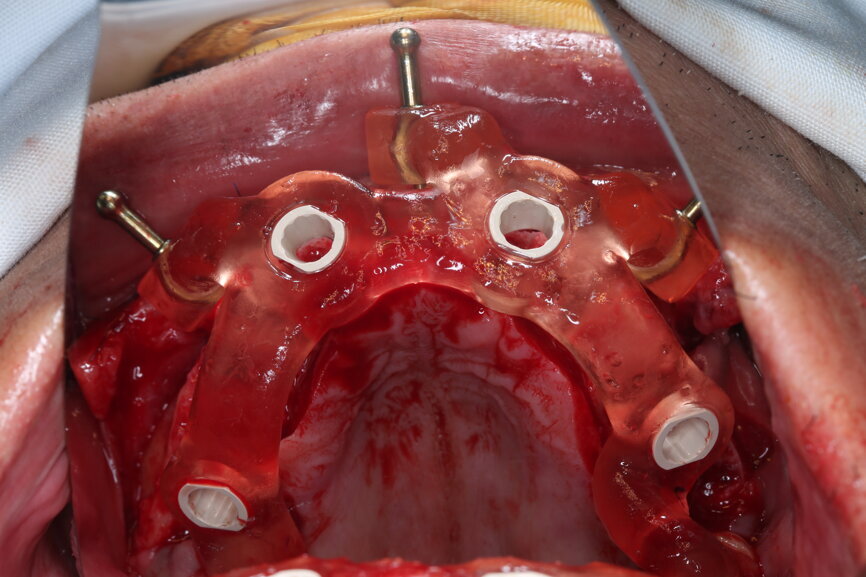
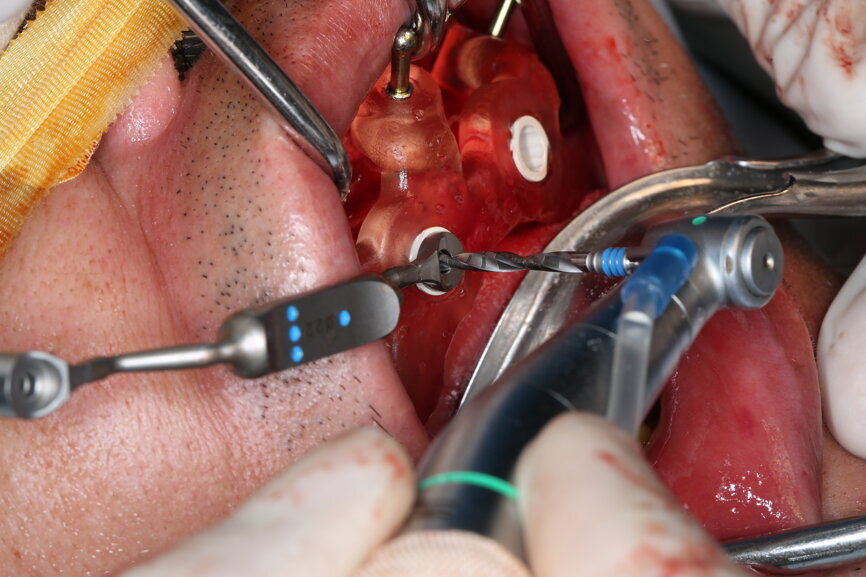
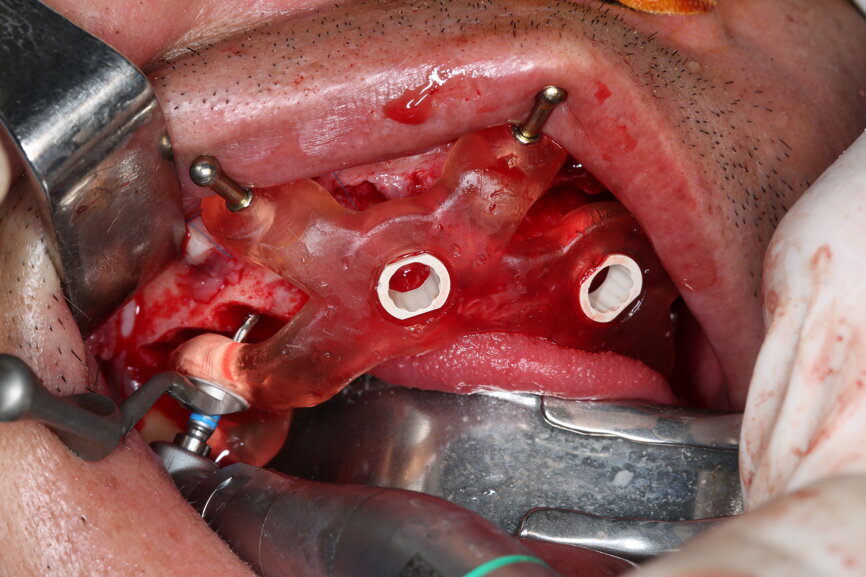
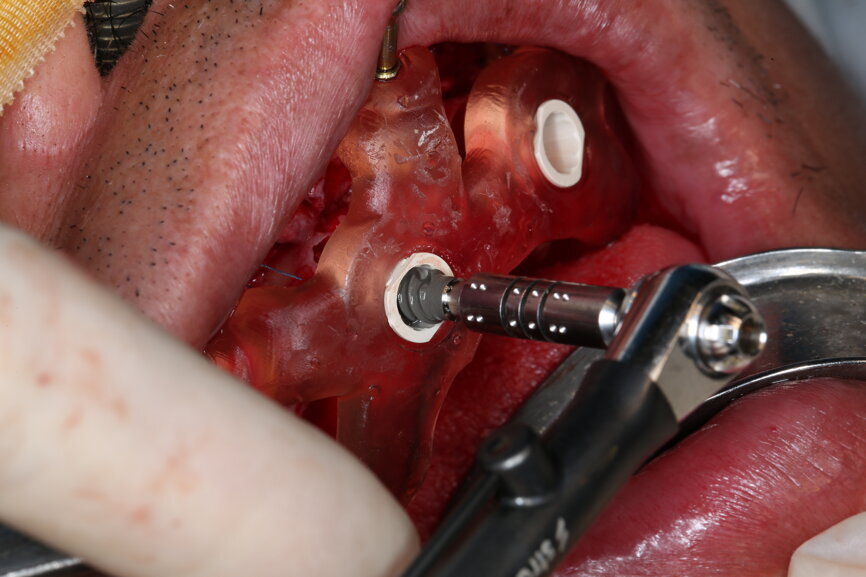
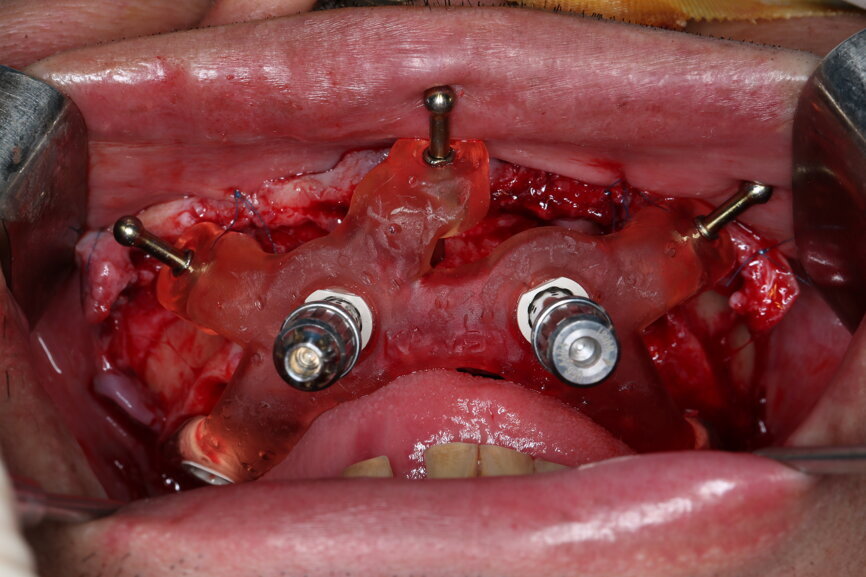
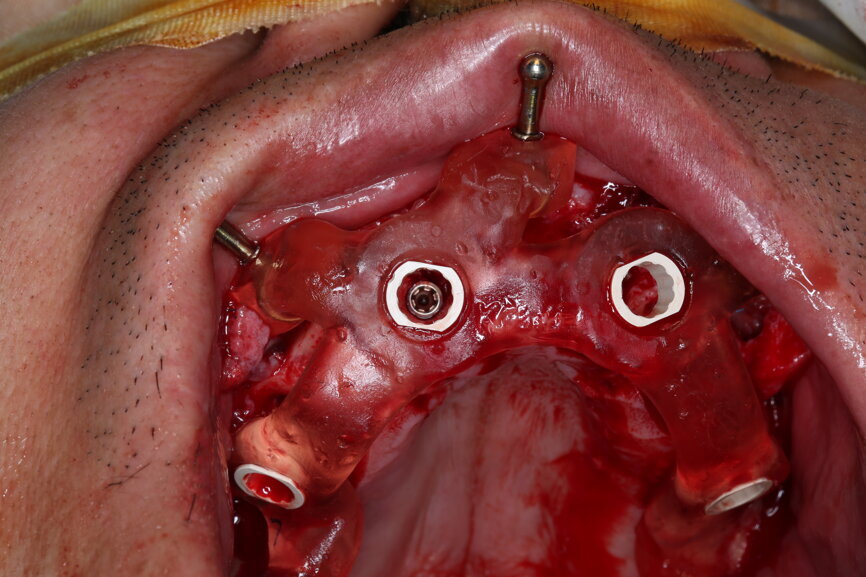
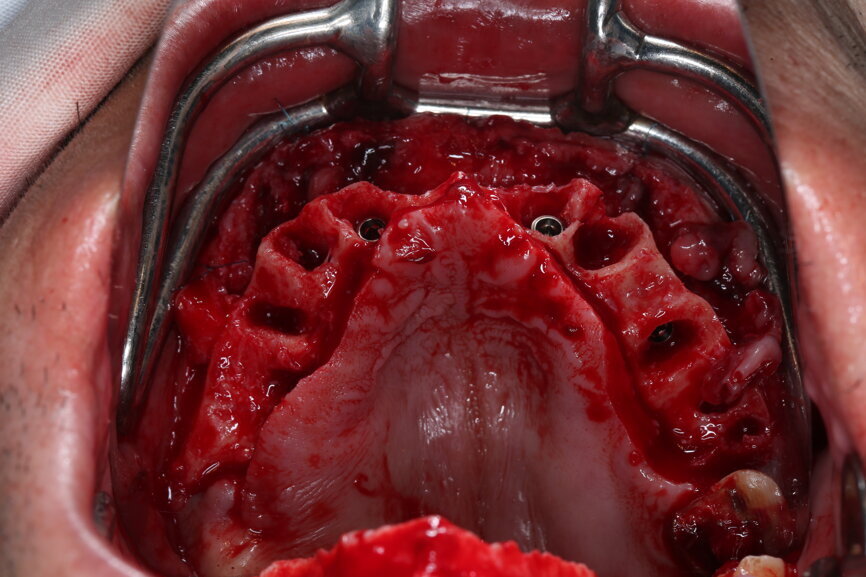
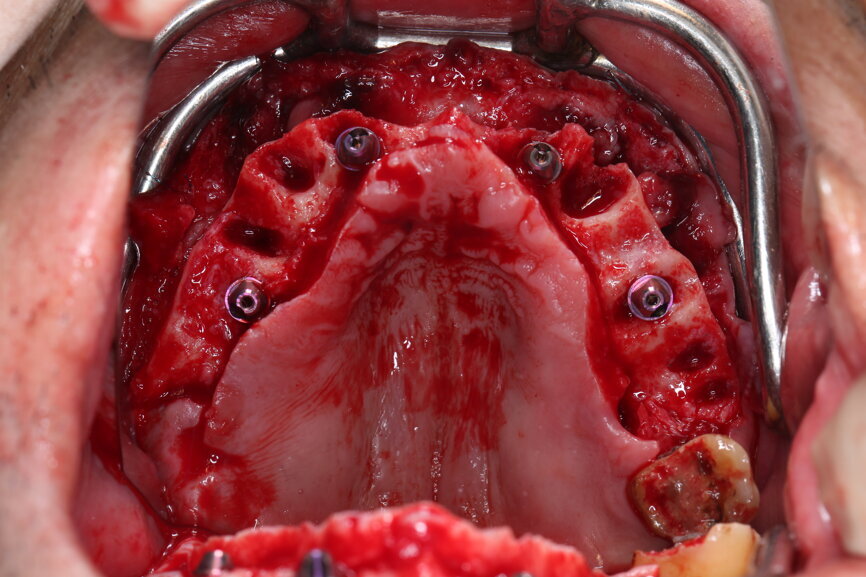
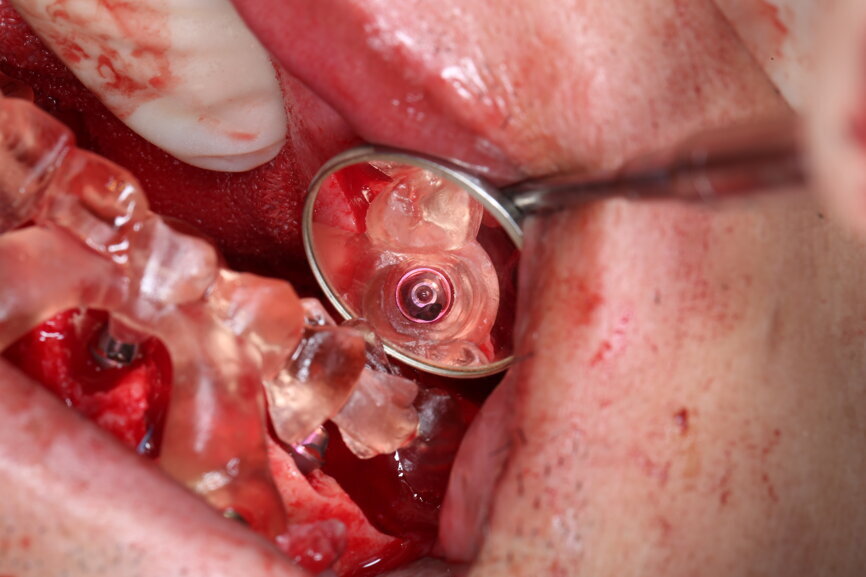
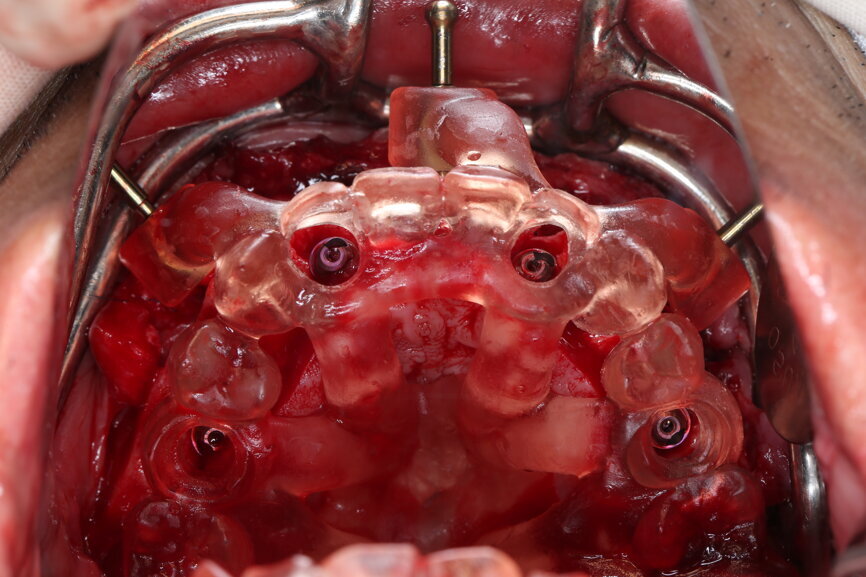
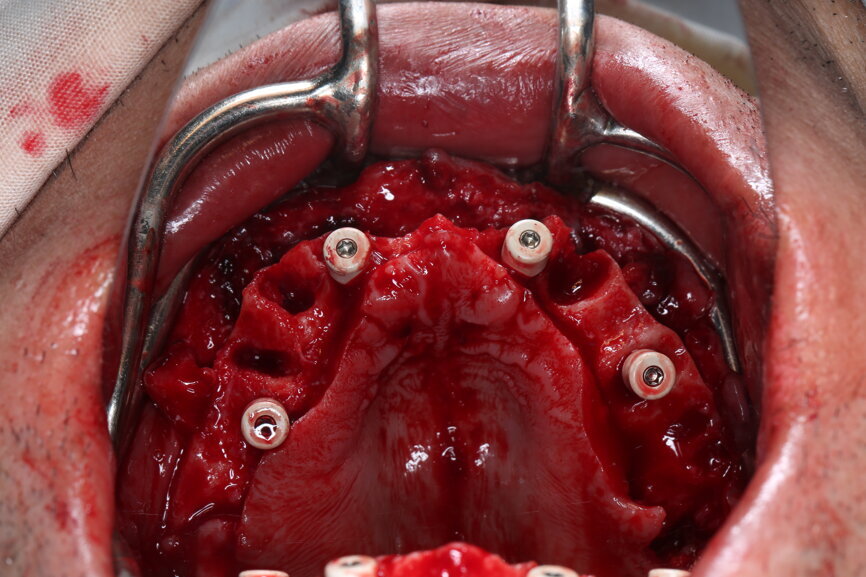
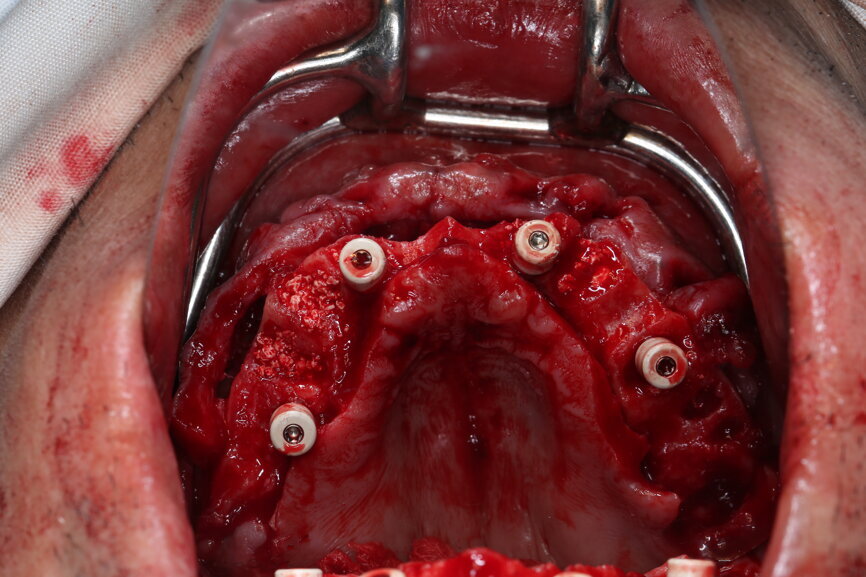
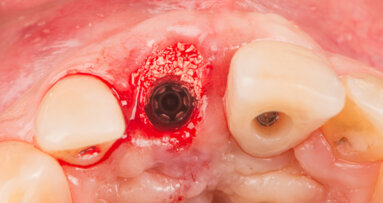
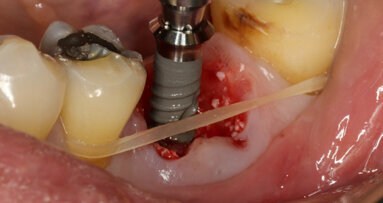
On the day of surgery, we prepared for the surgical protocol provided by the implant planning software, which guided us on the drilling sequence and the use of the appropriate instruments for the implant bed preparation (Figs. 30a & b). After the fixation pins had been allocated, teeth #17, 16, 15, 13, 12, 22, 23 and 24 were atraumatically extracted and alveolectomy was performed using a bone reduction guide (Figs. 31–36). Four implants (Straumann BLX; regular base; diameter: 4.5 mm; length: 12.0 mm) were placed, two straight implants in the anterior and two titled implants in the posterior. All the implants were stabilised to a torque of 50 Ncm (Figs. 37–43), and the SRAs were placed on top. The SRAs on the posterior implants had an angulation of 30° (diameter: 4.6 mm; gingival height: 3.5 mm) and on the anterior implants an angulation of 17° (diameter: 4.6 mm; gingival height: 3.5 mm; Figs. 44 & 45).
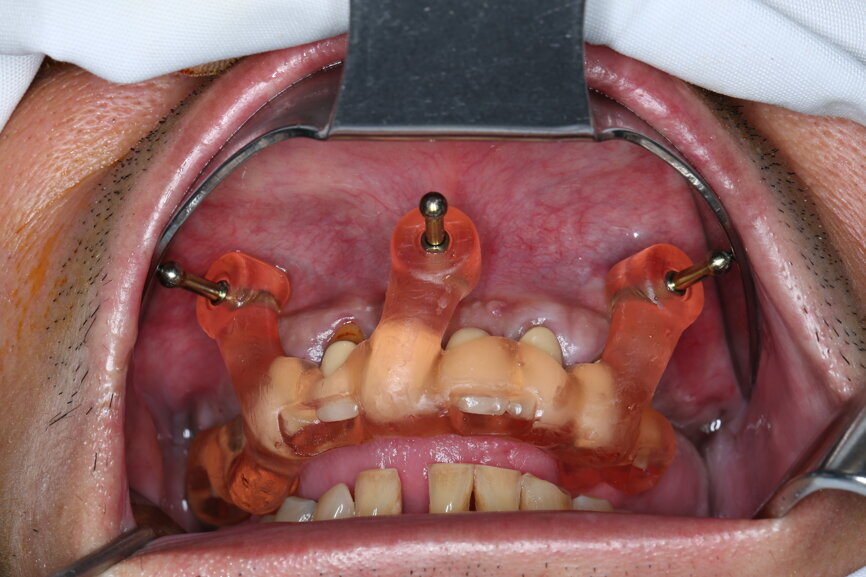
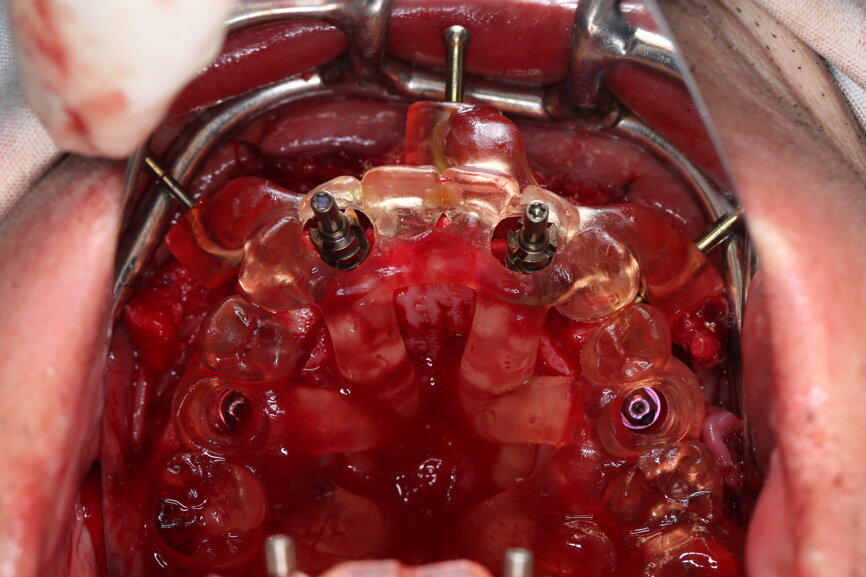
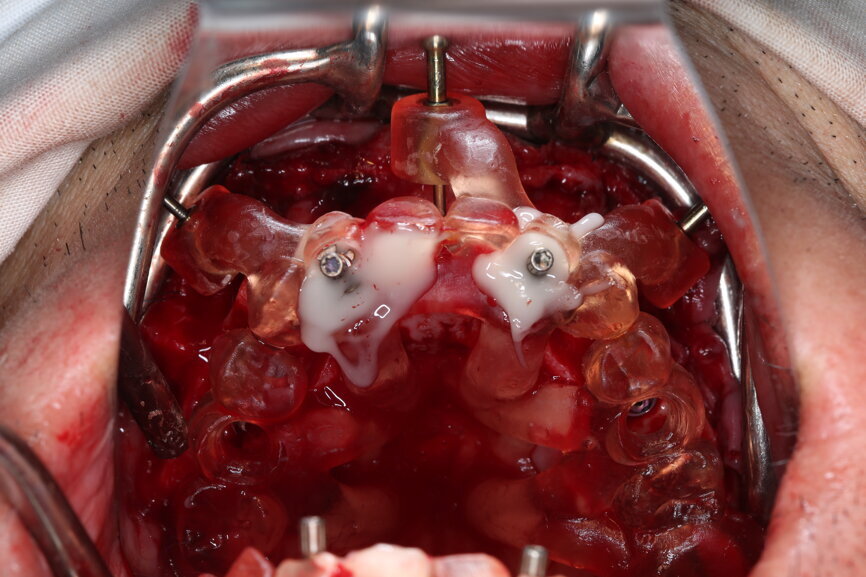
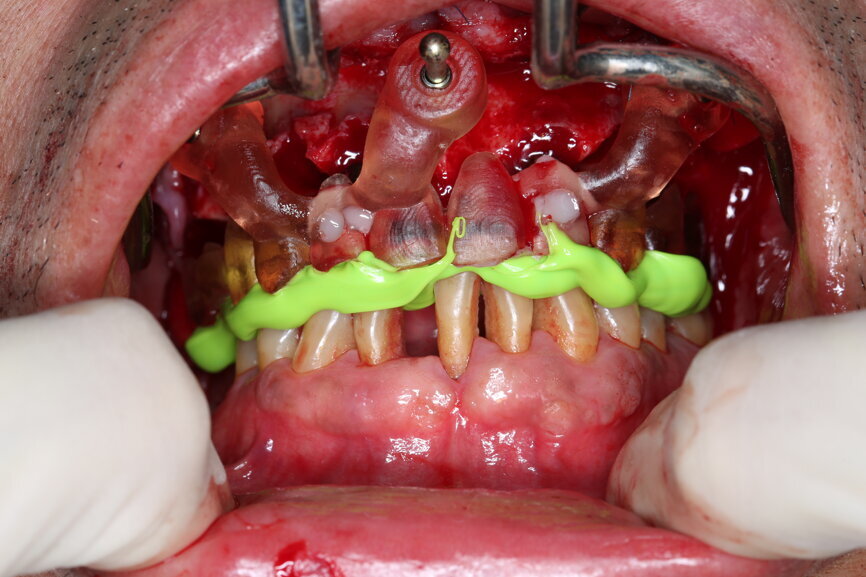
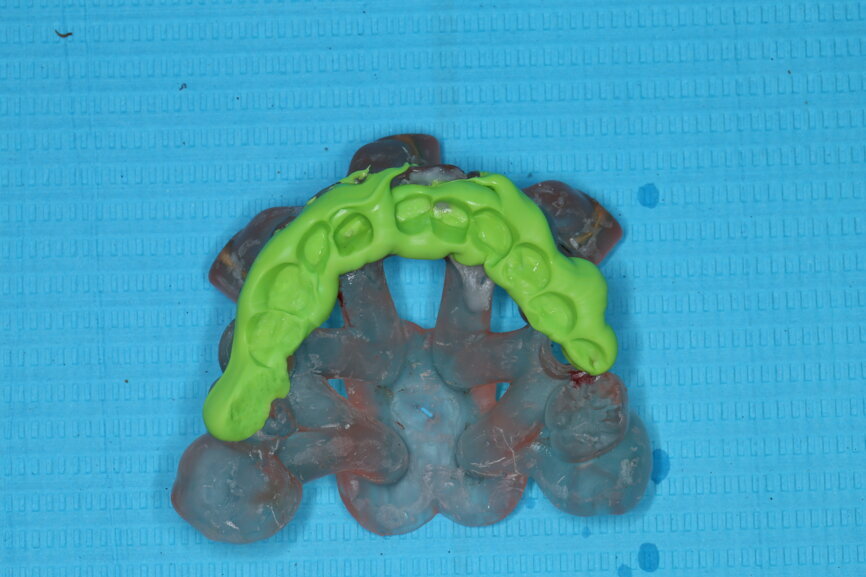
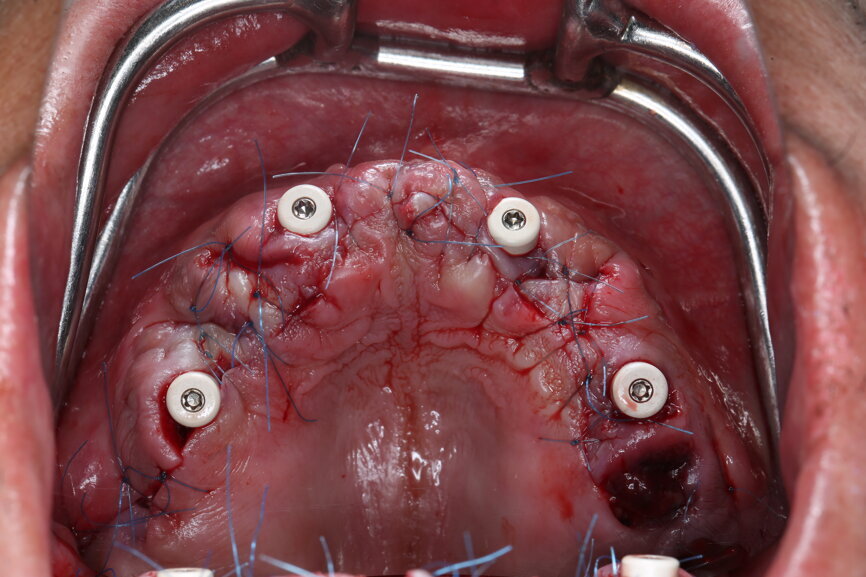
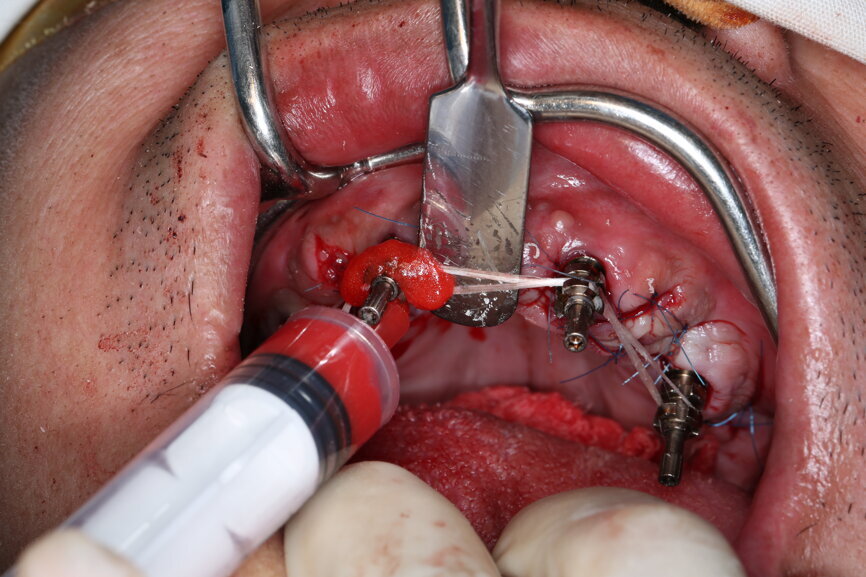
The bite registration guide was fixed with pins, and the open-tray impression copings were placed on the SRAs of the anterior implants, which were fixed with the guide using flowable composite and then sent to the laboratory (Figs. 46–50). Afterwards, we checked the CAD/CAM temporary restoration which had been designed and milled before surgery (Fig. 51), and protective caps were placed on the SRAs, followed by bone grafting using cerabone granules (botiss biomaterials) with a 1–2 mm grain size in the extraction sockets and suturing (Figs. 52–54).
Impression taking for the zirconia temporary restoration
Owing to circumstances, the patient was not able to visit the clinic periodically for follow-ups; therefore, we decided to use an immediate PMMA restoration for a short time and design an immediate temporary restoration on zirconia material to optimise the condition and patient experience while he was not able to visit our clinic.
For the impression taking, we used open-tray impression copings (Fig. 55), and the impression and the bite registration were transferred to the laboratory (Figs. 56 & 57). The PMMA restoration was screwed on to the SRAs, and the DSD 2D file was taken (Fig. 58).
Laboratory procedures for the zirconia temporary restoration
After creating the master cast, we were able to scan and design the zirconia restoration (Fig. 59–62). The design of the zirconia frame was done by obtaining the information from the bite registration, the image of the temporary prosthetic design (Fig. 6) and the mock-up copied by DSD based on the PMMA temporary restoration (Fig. 58).
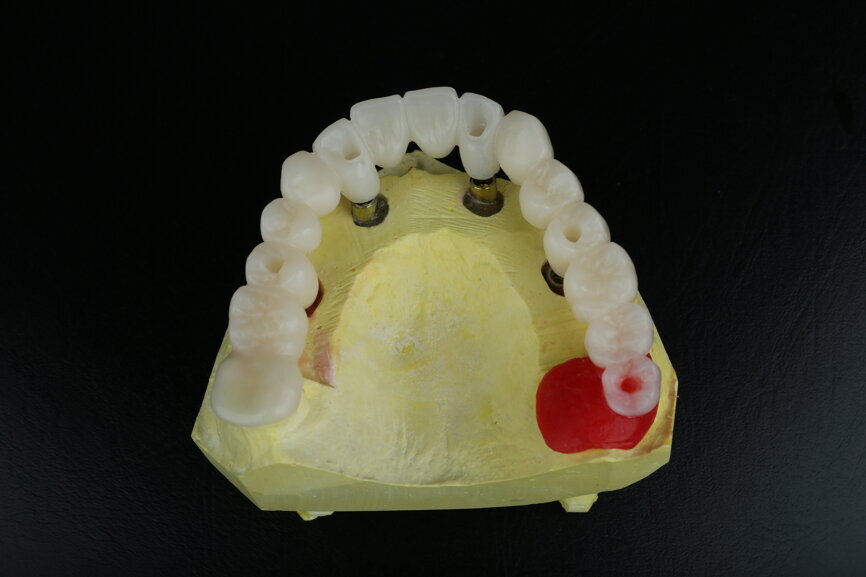
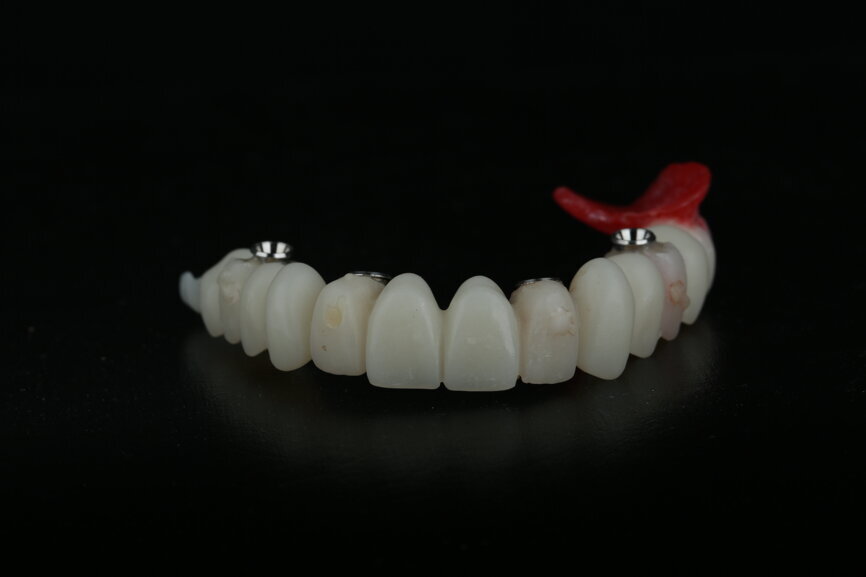
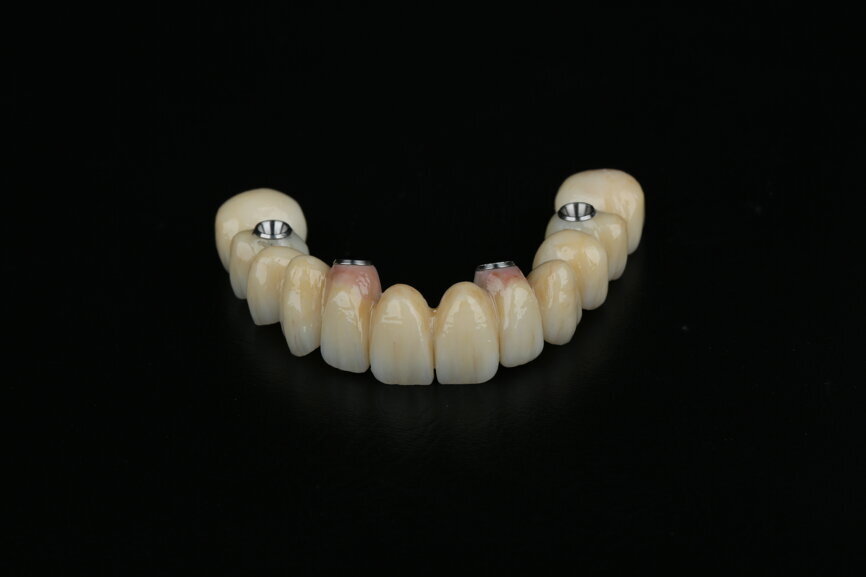
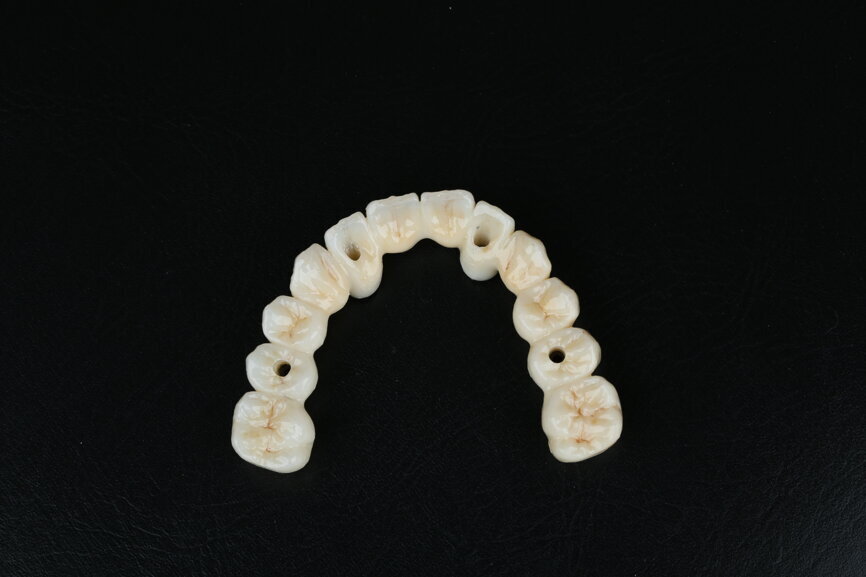
At this time, we were able to make a few modifications to the zirconia frame. The design of the zirconia temporary restoration was sent to the milling unit and produced on a full-contour zirconia disc. The zirconia frame was then cemented on Variobase copings (Straumann) as an interface to be screwed on to the SRAs (Figs. 63 & 64).
Five-day follow-up
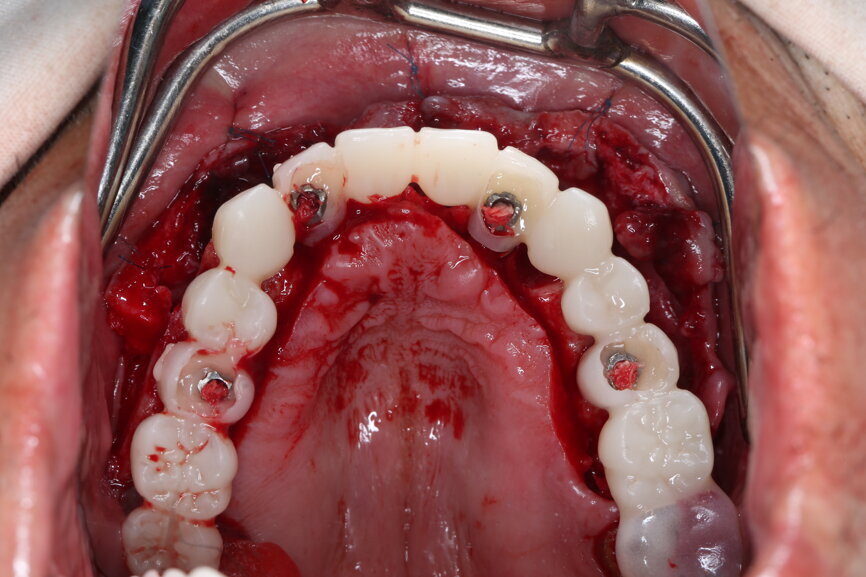
After five days, the patient returned to the clinic, and the PMMA temporary restoration was removed and the zirconia temporary restoration was placed, allowing a passive fit on the abutments with initial hand tightening of each SRA up to 5 Ncm. After the seating had been checked, the torque of each SRA screw was increased up to 35 Ncm, and the restoration was screwed in at a torque of 15 Ncm. The occlusion was checked, and the contacts were inspected. The screw holes were sealed with PTFE and a temporary filling material (Fig. 65). A panoramic radiograph was taken, and the SRA screw positions were evaluated to confirm the perfect fit of the temporary restoration (Fig. 66). Oral hygiene and dietary instructions were given to the patient, and a one-week follow-up appointment was scheduled.
Treatment outcomes
Immediate implant placement associated with immediate loading is a predictable protocol with some variables. The digitally planned tooth extraction was integrated with the production of a screw-retained CAD/CAM temporary restoration prior to the surgery and was successfully achieved. The entire treatment workflow was done fully digitally. Only a single surgical step was required to provide an entire individualised restoration.
Editorial note: A list of references is available from the Publisher. This article was published in CAD/CAM―international magazine of digital dentistry Vol. 11, Issue 2/2020.
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East








































To post a reply please login or register