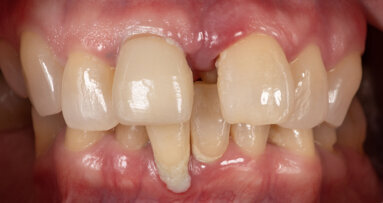
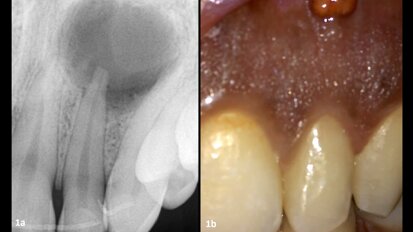
The main problem that brings patients to our surgery is an edentulous maxilla, which motivates the patient to want a functional restoration, with particular attention to the aesthetic result. The evaluation of the soft tissues of the face, from front and side view, shows a big reduction of the labial support induced by a centripetal bone retraction. More than that, the lack of sagittal and vertical bone support reduces the degree of dental- gingival exposure in case of peri-prosthetic crestal design (Figs. 1 & 2).
Considering the above parameters, to centre the aesthetic requirements it is proposed to the patient a removable implant-prosthetic rehabilitation; the goal is to achieve, with the prosthetic flange, a “prosthetic reconstruction” of the atrophic bone, thus favouring a suitable labial support with a correct teeth set-up.
The operating sequence therefore seeks to verify the soft tissues’ support by using an intraoral try-in of the set-up made on a model from a preliminary impression in alginate (Fig. 3).
The aesthetics were controlled and also confirmed by the patient’s involvement and approval who wanted a removable prosthetic solution without the palate area, and still have a good stability.
Guided by the duplication of the teeth set-up (replica), the implants were placed in the most suitable position and in a sufficient number to build a stable, aesthetic removable prosthesis without the palate. During the osseointegration period, the patient was provided with a temporary prosthesis in the zones adjacent to the implants. After the period of osseointegration, the implants were inspected and the gums had healed. The final phase also followed all the directions given to the patient about her experience with the temporary restoration.
All this information is critical to improving the aesthetics and the functional aspects in the final phase. For this reason, a new alginate impression was taken to produce an individual tray in order to produce an edentulous model and a preliminary registration rim for the mounting of the models in the articulator using a face bow. After the first phase was achieved, a teeth set-up restoring the aesthetics and the correct function was created (Fig. 5). Once these parameters were determined, the teeth set-up was duplicated using the silicone masks with a transparent resin (Fig. 6). The replica was perforated to correspondence with the implants in order to take a definitive impression in the centric relationship and with the same vertical dimension of the teeth set-up (Figs. 7 & 8).
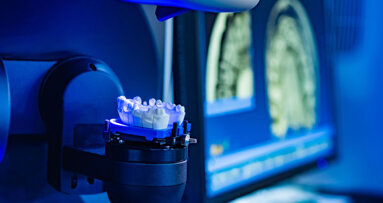
After the production of the master model, a resin jig was created by screwing the transfers on the model and by connecting them with resin that was cut around each implant; the dentist reconnected it in the mouth, assuring the correct impression position of the implants. When the jig was returned to the laboratory, a small model was created with the new analogues; this is an important model for the verification of the passivity and the precision of the structures (Figs. 9 & 10). With the same model, the accuracy of the position of the analogues in the master model was verified. At this stage the models, the implants and the teeth set-up were scanned in order to have all the information to verify the available spaces, and the number and position of the implants; only now is it possible to correctly plan a suitable prosthetic project, according to the available spaces; this also means choosing the correct attachments that will guarantee a good retention without modifying the project carried out with the teeth set-up (Figs. 11–21).
The file was sent to the New Ancorvis milling centre for the production of a Cr-Co bar. After a few days, the bar was returned to the laboratory, and tried first on the replica model to ensure its accuracy and passivity (Fig. 22); then the bar was positioned on the master model to verify it was a good fit even compared to the soft tissues, the cuff height and the correct spaces for hygiene (Figs. 23 & 24). After that the bar was sent to the dentist to double check the precision, passivity, correct spaces for hygiene, with the help of X-rays (Figs. 25–28). After those checks had been carried out, the bar was finished and polished. At this stage, the attachments were chosen accordingly to the type of prosthesis and the project and screwed into the structure (Fig. 29).
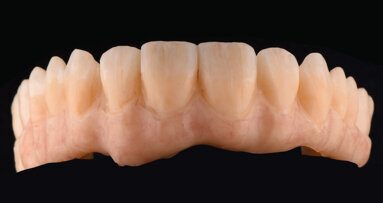
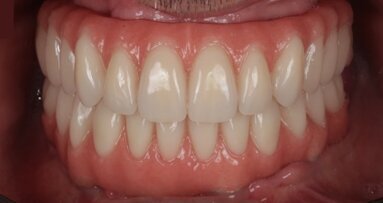
Once the attachments were screwed in, the bar was thoroughly polished (Fig. 30). The counter-bar was produced, polished and the retentive caps were inserted (Figs. 31 & 32). With the help of silicone masks, the teeth were repositioned and waxed on the superstructure, for the final try-in in the mouth (Figs. 33–35). A final check that everything had been completed was carried out, including: the phonetics, aesthetics and the correct support of the soft tissues. Once the pink flange was finished, the prosthesis was positioned in the muffle furnace for the curing steps (Fig. 36). These systems provide a good precision and an excellent detail reproduction. Once cured, the prosthesis was extracted and finished (Fig. 37) and then to the final polishing prior to the delivery (Figs. 38–40). Finally, the superstructure and the prosthesis were placed in the mouth (Figs. 41–43), verifying the good aesthetics, function and also the satisfaction of the patient (Figs. 44–46).
Conclusion
The teeth set-up, and digital systems allow us to accurately design a complete rehabilitation, and is important in highlighting from the very early stages which solution (fixed or removable) is most suitable for the patient. In this case, the solution of a removable prosthesis made possible an optimal functional and an aesthetic result.
Editorial note: A list of references is available from the publisher. This article was published in CAD/CAM international magazine of digital dentistry No. 02/2017.
Transitioning from analogue to digital dentures has significant benefits for oral healthcare professionals, laboratories and patients. The implementation of...
Implant treatment for full-arch fixed restorations has been around for decades now.1–3 The treatment usually involves four to six implants placed in ...
ORLANDO, Fla., US: GPS Digital RPD is a Florida-based dental laboratory specialising in high-quality partial frameworks and flexible partial dentures. ...
MUNICH, Germany: Additive manufacturing is rapidly gaining importance in removable prosthodontics. To inform clinicians, a recent review has provided an ...
Improvements in digital technologies in recent years have transformed several industries, including implant dentistry. These novel methodologies have ...
When COVID-19 affected the European dental prostheses and digital dentistry markets—including in countries such as Austria, Belgium, France, Germany, ...
Dental implants have become one of the most predictable treatment alternatives for patients who are missing teeth. Despite the high success rates, which are...
IOANNINA, Greece: Numerous finishing techniques are available for zirconia-based screw-retained implant-supported prostheses; however, most of them are ...
I have been a registered denturist for over 20 years. At our laboratory and clinic, we specialise in removable prosthetic solutions: partial dentures, ...
There is increased interest in the long-term clinical outcomes and quality of life of patients treated with full-arch implant-supported dental prostheses ...
Live webinar
Thu. 30 April 2026
1:00 pm EST (New York)
Live webinar
Sun. 3 May 2026
12:00 pm EST (New York)
Dr. Rickard Brånemark MSc, MD, PhD, Dr. Robert Gottlander DDS
Live webinar
Sun. 3 May 2026
8:00 pm EST (New York)
Live webinar
Tue. 5 May 2026
10:00 am EST (New York)
Live webinar
Tue. 5 May 2026
12:00 pm EST (New York)
Live webinar
Tue. 5 May 2026
1:00 pm EST (New York)
Dr. Maximilian Dobbertin M.Sc
Live webinar
Tue. 5 May 2026
3:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East































To post a reply please login or register