Like most materials used in healthcare, denture materials have evolved profoundly over the last 300 years or so. For centuries now, people desiring to replace all their teeth have searched widely—often futilely—for biocompatible, comfortable, aesthetically appealing and long-lasting materials. Early dentures were more often than not embarrassing, unattractive and barely functional replacements of natural teeth.
In the pre-industrial world, before the 1800s, dentures were predictably primitive. Removable oral prostheses were often studded with genuine human teeth, sometimes reclaimed from cadavers. Otherwise, false teeth were typically made from natural materials like wood or animal bone. Some historical dentures were carved entirely from ivory, but they required a high-skill, time-intensive process only accessible to the wealthy.1 While these devices could be relatively convincing, they were held in place crudely (i.e. painfully and unreliably) with springs and weights and prone to staining and decay.2
Denture access finally democratised in the middle of the nineteenth century, when Charles Goodyear developed vulcanite, which quickly became the preferred material for fabricating dentures and held its position through the first third of the 1900s. Of course, polymethylmethacrylate (PMMA) has been the industry standard for denture base fabrication since its introduction in the late 1930s.3 Over the decades since, while manufacturing processes have been refined and new innovations have come and gone, PMMA has remained the most widely used denture material.
With the benefit of historical perspective, we can now look back on early devices and understand them as unsophisticated, unhygienic and otherwise limited. In a few years’ time, I contend we ought to similarly appraise removable prosthodontics from earlier this century.
The analogue to digital evolution
In 1994, the first digital denture study appeared in the International Journal of Prosthodontics.4 The paper introduced a novel process wherein the authors used a laser scanner to take denture impressions and 3D-printed a tooth and base contour jig, which allowed a denture to be fabricated using photopolymerising resin. While the ideas in the study were groundbreaking, 3D printing at the time was frankly not mature enough for clinical use, so the emerging digital dentures industry focused instead on CAD/CAM milling. A proof of concept detailing a technique for milling a denture duplicate out of wax was published in the Journal of Oral Rehabilitation in 1997.5
The first commercial digital denture was not produced until 2011—well over a decade later. Global Dental Science designed and fabricated the device, which it marketed as AvaDent Digital Dentures. AvaDent remains as an authority in the current digital denture system market, alongside options from competitors like Ivoclar, Dentsply Sirona, SprintRay, VITA Zahnfabrik (Vita Vionic) and Merz Dental (Baltic Denture System).6
Milled denture manufacturers developed and standardised PMMA pucks to place in computer numerical controlled mills. The first milled dentures still involved a significant amount of technical, hands-on work, as fabricators were able to mill the denture base only; they bonded carded denture teeth into the base one by one. Over time, dental laboratories developed improved systems which allowed a full set of teeth to be milled as a single piece. This piece would then be bonded with a separately milled base and returned to the mill for finalisation (Ivoclar’s oversize milling process). Today, the best milled denture systems fabricate one-piece monolithic dentures. 3D printing is now playing a greater role in denture fabrication owing to its already low cost and impressive scalability. In recent years, the development of novel photopolymers and sophisticated fabrication techniques has lowered the cost of entry to this exciting technology significantly, such that it has become a viable option for working laboratories. Today, properly equipped laboratories can print a denture base in a pink material which is then bonded to a carded denture teeth or a monolithic or segmented printed tooth material arch. Such systems include the Lucitone Digital Print Denture System (Dentsply Sirona) and the SprintRay High Impact Denture Solution.
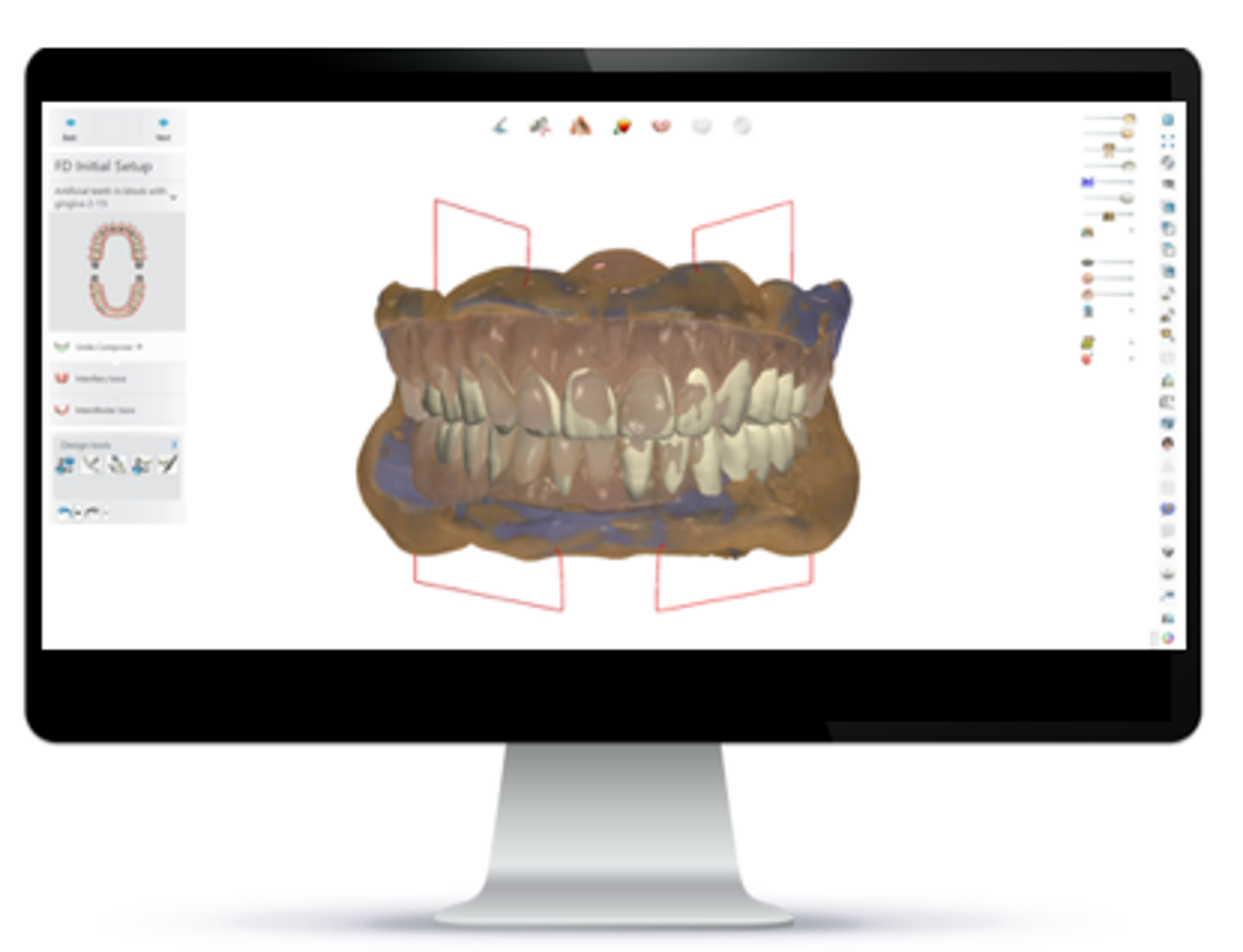
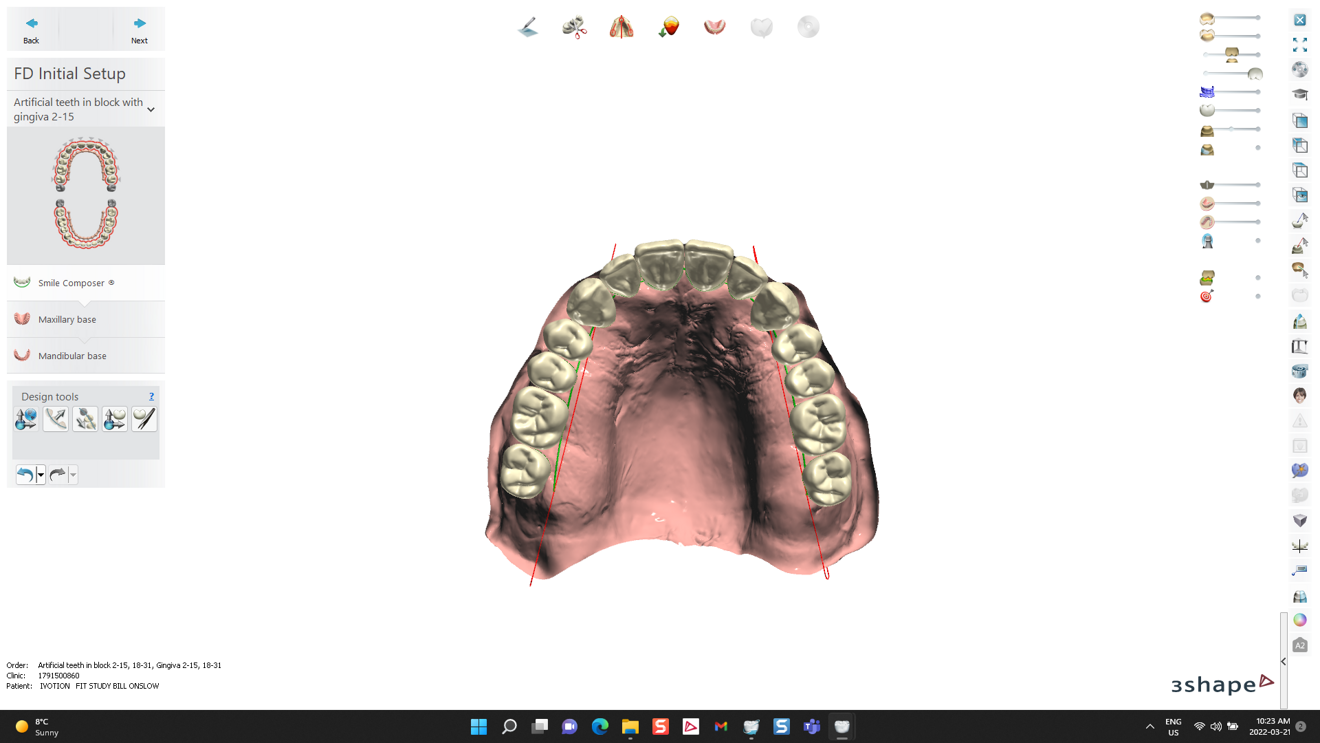
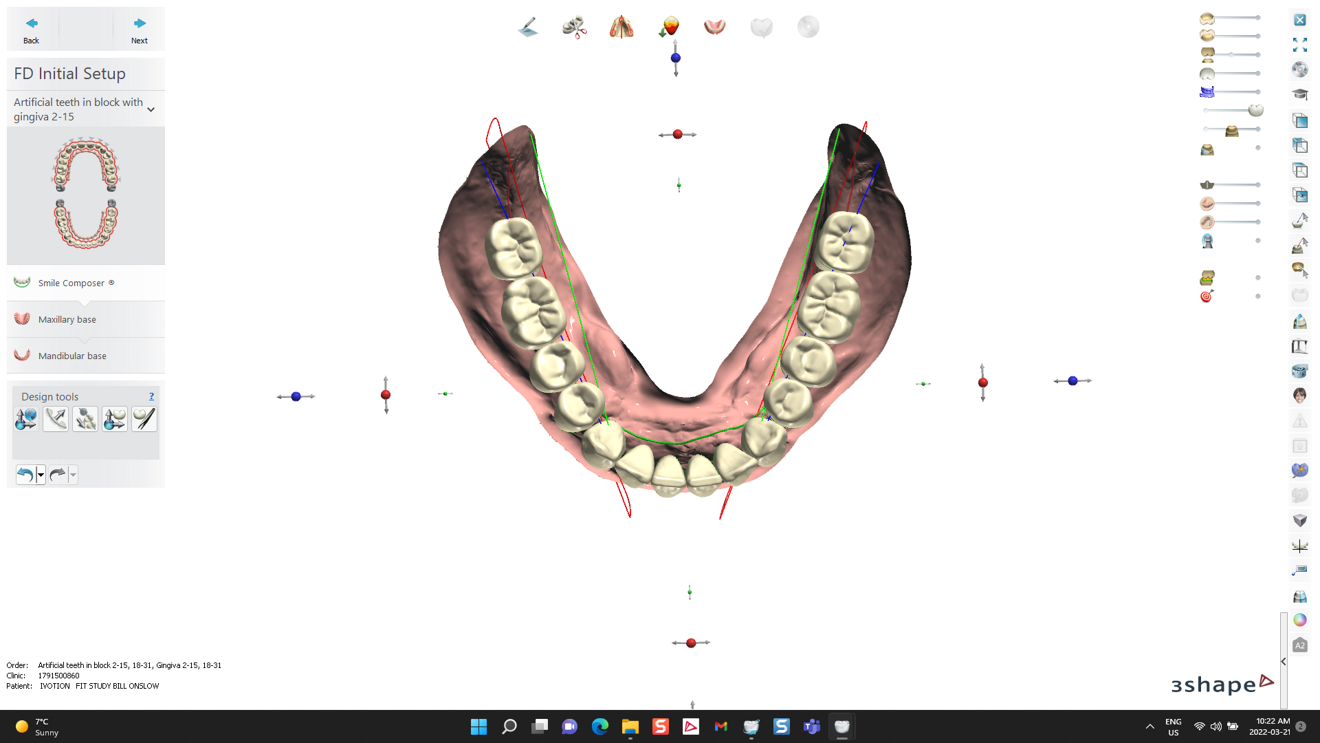
The development of dedicated digital denture design software was another groundbreaking innovation. In some cases, commercially available software systems were proprietary suites custom-designed for digital denture fabrication (e.g. AvaDent Connect). Elsewhere in the industry, leading companies like Ivoclar use 3Shape-built specialised modules to extend the capacities of pre-existing dentistry design software.
The varied benefits of digital dentures
The tech industry favours the word “disruption” to describe paradigm-shifting changes in methodologies—and I’ve been guilty of using it myself. Lately, I find it more productive to shift my focus away from how digital dentures destroy old ways of doing work and instead foreground how digital dentures actively benefit clinicians, patients and laboratories alike.
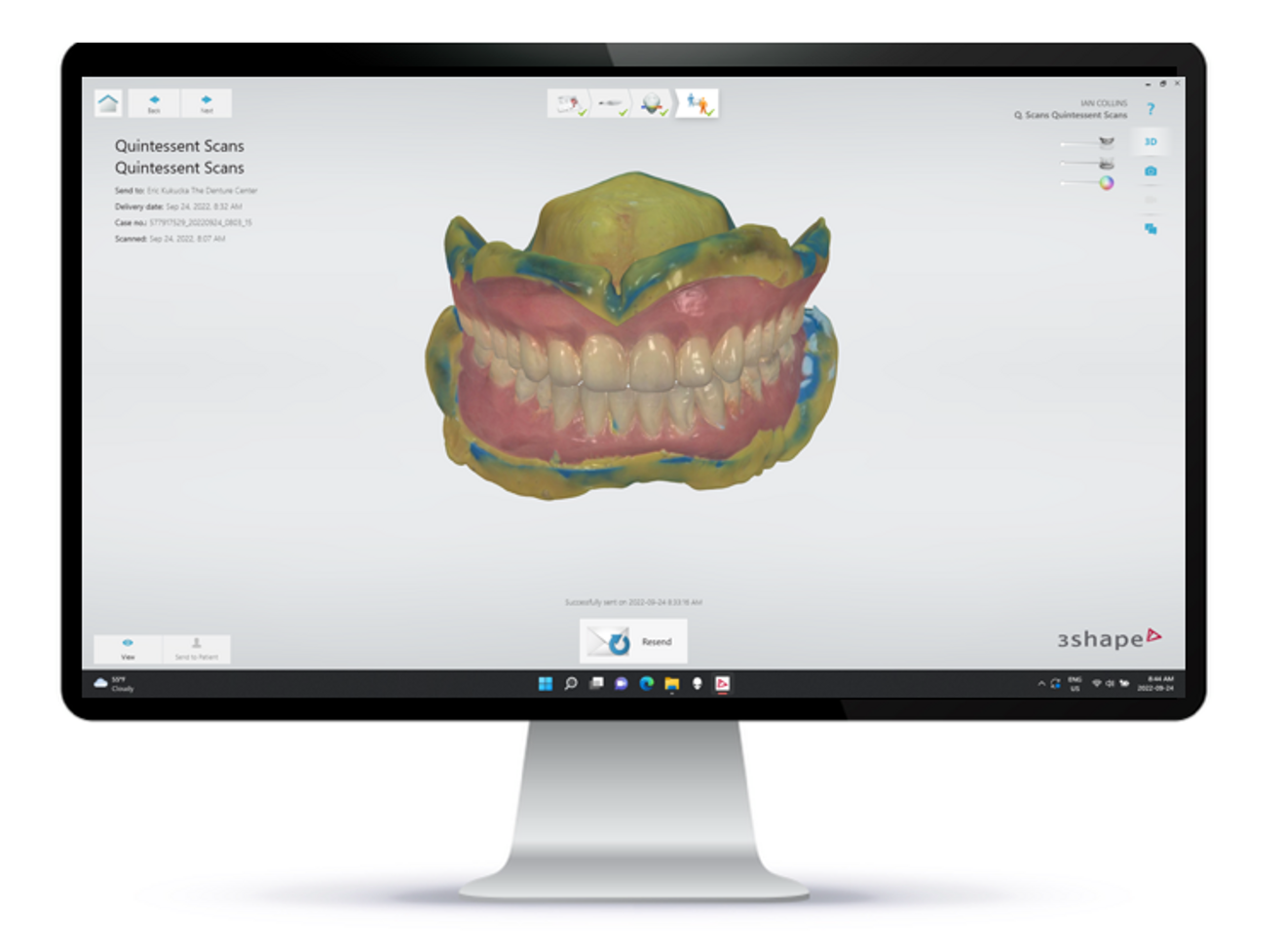
Many leading clinicians are already taking advantage of digital technology, which makes design and prostheses infinitely reproducible. In basic terms, modern digital dentures replace error-prone plaster moulds with precise computerised data sets, allowing sufficiently trained dental professionals to scan a patient’s mouth or physical impressions or casts, transform them into computerised 3D renderings and initiate a precise CAM process at the push of a button—all while improving a denture’s aesthetic dimensions and fit, if a patient so desires.
Digital modalities simplify several potential points of friction in the reference denture workflow. The analogue reference denture workflow is popular in part because it condenses clinical steps and allows clinicians to use past experience as indicators of complexity, measurably improving predictability.7 However, clinicians using conventional laboratory techniques have often been unable to accurately reproduce complex existing dentures.8 Importantly, for inexperienced clinicians, digital workflows mitigate the intimidation factor that can accompany complete denture therapy in general. With traditional methodologies, a single mistake can send a clinician back to square one; this reality generates a significant fear factor. Because digital workflows preserve patient records perfectly, clinicians gain peace of mind, allowing them to do better work unencumbered by trepidation.
In almost all cases, digital denture workflows require fewer and shorter appointments—including postoperative visits.9, 10 While the advantages of reduced in-office hours should be obvious to clinicians, we must not overlook the potentially profound benefits to patient access. Statistically, patients requiring removable complete dentures are disproportionately likely to have complex medical profiles and/or difficult socioeconomic circumstances. Specifically, they are less likely to have private transport, more likely to experience mobility issues and less likely to live near a dental practice. As a general rule, we should not take these patients’ ability to come into the office for granted.
Patients also benefit from digital dentures’ greater degree of precision (meaning better fit) and superior functional quality. According to Drs Brian J. Goodacre and Charles J. Goodacre of Loma Linda University in California in the US, most rigorous comparisons of conventional denture base materials and the milled bases commonly used in digital workflows have concluded that milling produces greater flexural strength and the highest accuracy and trueness,11–15 allowing milled bases to respond more positively to accidental vdamage.
Across-the-board outcomes are likely to improve further as future generations of dentists and technicians enter the workforce familiar with these new workflows. According to Wendy Auclair Clark, clinical assistant professor in prosthodontics at the University of North Carolina at Chapel Hill in the US, digital dentures are now an integral part of complete denture curricula at leading dental schools.
The digital reference denture technique
I have written and lectured extensively elsewhere on the reference denture technique, also called the “denture duplication workflow”. In the right hands, I believe that this seamless and technically and clinically integrated workflow delivers the greatest possible standard of predictable precision care and craft.
The increasingly popular technique is ideal for edentulous patients who are generally satisfied with their existing dentures at the end of their regular lifespan. In appropriate situations, the digital reference denture workflow provides technicians with a sophisticated digital record of a patient’s existing information, allowing clinicians to rehabilitate the patient more confidently, predictably and precisely than would otherwise be possible.
Using traditional methods and materials, reproducing an existing handcrafted denture within acceptable limits—never mind perfectly—is laborious. As I am sure you know, the final quality of an analogue denture is determined largely by the hand–eye coordination and motor dexterity of the person fabricating it. The risks of human error are significant and unavoidable.8



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East







































To post a reply please login or register