In recent decades, we have witnessed the substantial development and expansion of the use of fixed orthodontic appliances. While their application has many advantages, several problems related to the health of the soft tissue may sometimes appear during treatment. In fact, the use of fixed orthodontic appliances may provoke labial desquamation, [1] erythema multiforme, [2] gingivitis [3] and gingival enlargement. [4]
Gingival enlargement is a very common complication during orthodontic treatment, [5] but fortunately, it seems to be transitory and generally resolves after orthodontic therapy, even if sometimes incompletely. Gingival overgrowth induced by orthodontic treatment shows a specific fibrous and thickened gingival appearance, different from fragile gingiva with marginal gingival redness common in allergic or inflammatory gingival lesions. [6]
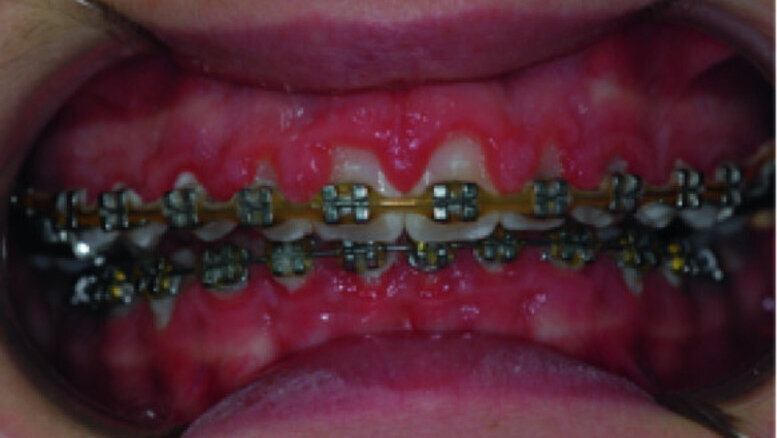
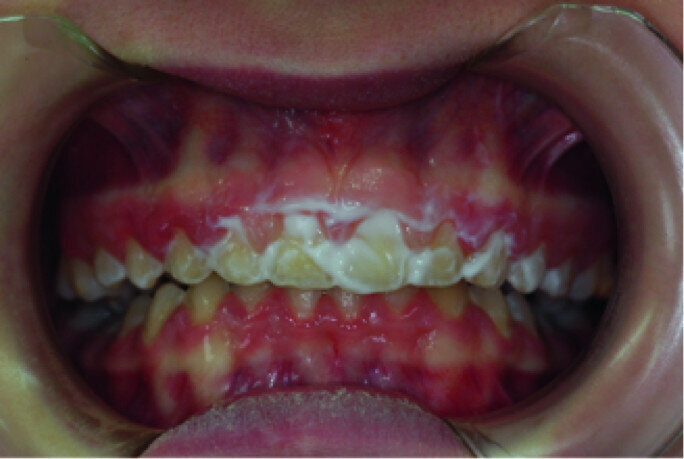
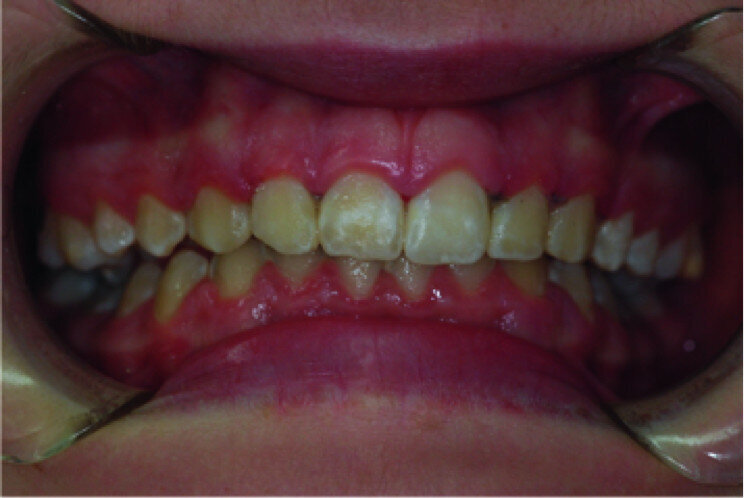
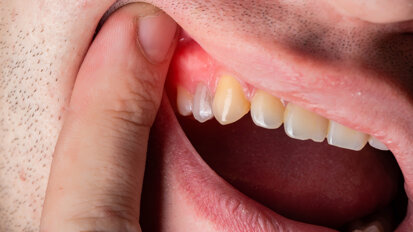
Clinical view, showing gingival enlargement, just before the debonding procedure.
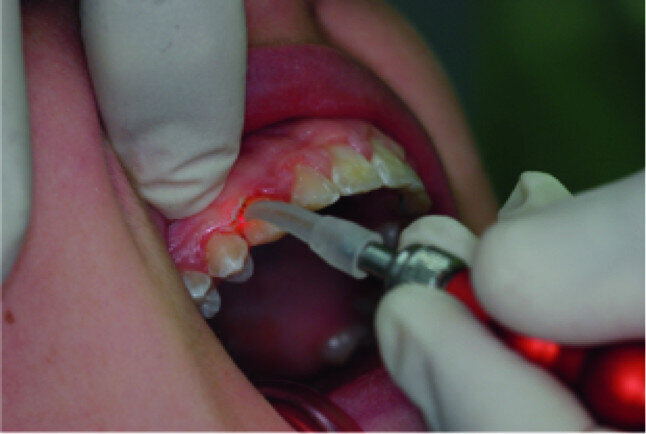
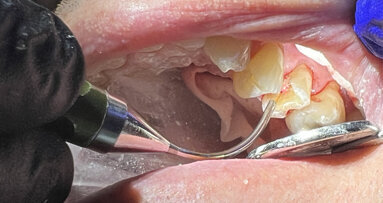
Application of a topical anaesthetic.
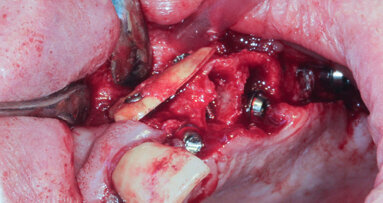
Surgical laser-assisted treatment via laser gingivectomy.
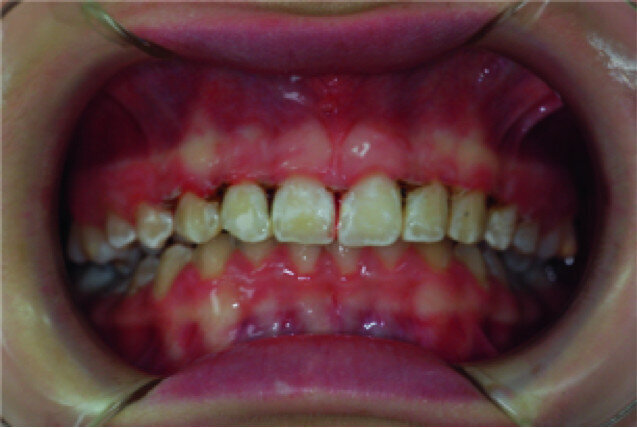
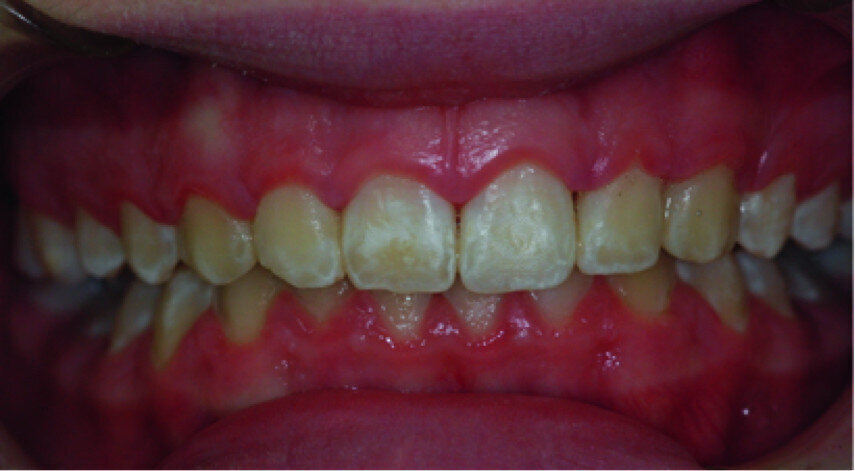
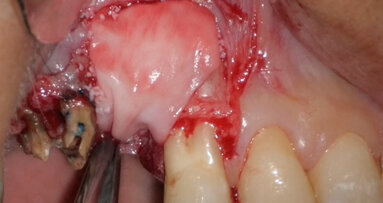
Clinical view just after surgery.
Healing five days after surgery.
Several clinical studies suggest that orthodontic treatment may be associated with a decrease in periodontal health, causing a hypertrophic form of gingivitis. However, the actual pathogenesis of gingival enlargement is not yet completely understood, although probably involves increased production by fibroblasts of amorphous ground substance with a high level of glycosaminoglycans. Increases in mRNA expression of Type I collagen and up-regulation of keratinocyte growth factor receptor could play an important role in excessive proliferation of epithelial cells and increased development of gingival enlargement, on the basis of some studies, in cases of poor oral hygiene status.[7] However, there is no clear definition on its aetiology, although it is probably associated with the inflammatory response induced by the corrosion of orthodontic appliances, particularly those of nickel,[8] linked to an inflammatory response considered a Type IV hypersensitivity and manifested as nickel-induced allergic contact stomatitis, even if its aetiology has not yet clearly been defined.[9]
The treatment of these conditions is surgical. Histological and histochemical studies have demonstrated that the removal of the gingival papilla can promote the formation of normal connective tissue.[10] Because the classic intervention performed by scalpel has some disadvantages, mainly linked to the discomfort for the patient (e.g. anaesthesia by injection and sutures), there has been great interest in the utilisation of laser technology.
Case report
A 14-year-old female patient was referred to our department by the orthodontics unit because, at the end of fixed orthodontic treatment, she had developed gingival enlargement in the upper arch (Fig. 1), probably related to the fast closure of the spaces associated with very poor oral hygiene due to bleeding during toothbrushing. Just after the removal of the appliance, a topical anaesthetic (EMLA, AstraZeneca) was applied to the gingivae (Fig. 2) and a gingivectomy was performed using a diode laser (XD-2, Fotona) according to the technique of removal of the inter dental papillae (Fig. 3). The parameters used were as follows: a wavelength of 808 nm, 3 W in continuous wave, a 320 μm fibre in contact mode. The intervention had a duration of 375 seconds, and the patient did not feel any pain (Fig. 4). After the intervention, the patient did not take any kind of pain medication, and the healing process was completed in five days (Fig. 5).
Discussion
The first laser appliance was built by Maiman in 1960, and some years later, it was successfully employed in medicine and in oral surgery with several advantages. It may provide excellent incision performance with sealing of small blood and lymphatic vessels, resulting in haemostasis and reduced postoperative oedema. Furthermore, target tissues are disinfected as a result of local heating and production of an eschar layer, which results in a decreased amount of scarring owing to decreased post-operative tissue shrinkage, allowing one to avoid the use of sutures.
Diodes, the last generation of laser used in dentistry, have several advantages, such as reduced cost and size, and ofer the operator the possibility to work both in continuous and chopped mode. Based on our experience, we can confirm that this technology may represent a new approach to the resolution of gingival enlargement during orthodontic treatment, with better comfort for the patient during and after surgery.
Editorial note: A list of references is available from the publisher. This article was published in ortho - international magazine of othodontology No. 02/2017.
According to the Classification System for Periodontal Diseases and Conditions (1999)(1), drug-induced gingival enlargement belongs to the group of gingival...
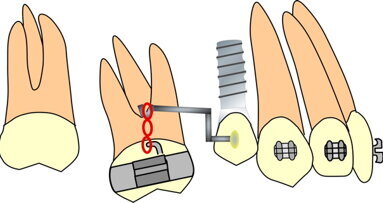
In recent years, the purview of orthodontics has grown to include an increasing number of adult patients, many of whom present with complex malocclusions ...
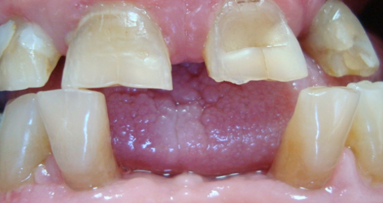
Pulpal exposures are unfortunately a routine occurrence when treating carious teeth and frequently lead to endodontic treatment owing to the size of the ...
Treating bone insufficiency is a familiar challenge for all implant practitioners. Such insufficiency can compromise the placement of an implant, its ...
In recent years, the technology associated with endodontic therapy has undergone a veritable revolution. For years, intraoral radiographs were used as the ...
LONDON, UK: Digital technologies have changed the way in which we live and the ways in which we align teeth. According to leading UK orthodontic specialist ...
A free webinar on 19 June will offer participants an opportunity to learn about how to implement orthodontic treatment as a fundamental tool in the context...
Combining orthodontic treatment and preventive treatment is a key component of the clinical philosophy of Drs Ines Metke and Claudia Mengel, who have run ...
Although orthodontic treatment has become increasingly commonplace, its periodontal side effects are often overlooked. In a free CURADEN webinar on Tuesday,...
LONDON, England: Driven by the NHS dental crisis, an increasing number of UK patients seeking cheaper dental work overseas are encountering unexpected ...
Live webinar
Thu. 2 April 2026
12:00 pm EST (New York)
Live webinar
Wed. 8 April 2026
1:00 pm EST (New York)
Live webinar
Thu. 9 April 2026
1:00 pm EST (New York)
Live webinar
Thu. 9 April 2026
2:00 pm EST (New York)
Prof. Moritz Kebschull, Cat Edney
Live webinar
Fri. 10 April 2026
10:00 am EST (New York)
Live webinar
Fri. 10 April 2026
11:00 am EST (New York)
Dr. med. dent. Henrik-Christian Carl Hollay
Live webinar
Fri. 10 April 2026
12:00 pm EST (New York)
Prof. Dr. Ali Murat Kökat



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East































To post a reply please login or register