In recent years, the technology associated with endodontic therapy has undergone a veritable revolution. For years, intraoral radiographs were used as the basis for diagnosis and for planning root canal therapy, despite the fact that these images did not provide a faithful reproduction of the endodontic anatomy. This created a series of technical problems, which, although they could be partly overcome by the operator’s personal experience, to some extent remained unresolved, especially in the field of diagnosis.
I personally started using cone beam computed tomography (CBCT) for endodontic purposes more than ten years ago. Although the machines that I used then were far from ideal for this specific purpose, the possibilities offered today by increasingly sophisticated technologies have greatly improved my diagnostic and interventional capabilities. In order to make an accurate diagnosis, an endodontist needs to perform a highly detailed assessment of the canal and pulpal anatomy, which requires high-definition examination techniques and software that enables the endodontist to rotate the tooth accurately and easily. This may seem obvious and trivial, but is not. Indeed, over the past ten years, I have had the opportunity to work with a large number of devices and dozens of software programmes, but only very few have proven to be suitable for endodontic purposes. For a few years now, I have been using ACTEON’s trium technology, with extremely satisfactory results. The imaging is very accurate and highly detailed, and above all, the user friendliness of the ACTEON Imaging Suite makes it possible to identify even slight differences between the different radiographic slices, differences that are of paramount importance for making a correct endodontic diagnosis and for the therapeutic decision-making process itself. Clinician experience alone is not sufficient for establishing the correct approach to be adopted in the case of endodontic disease, and very often clinical cases that were initially scheduled for orthograde treatment, after CBCT assessment, turn into cases for endodontic surgery or vice versa. We can therefore state that the capability we have now of performing these studies in a quick and easy manner has drastically reduced the number of incorrect diagnoses and, consequently, the number of clinical errors.
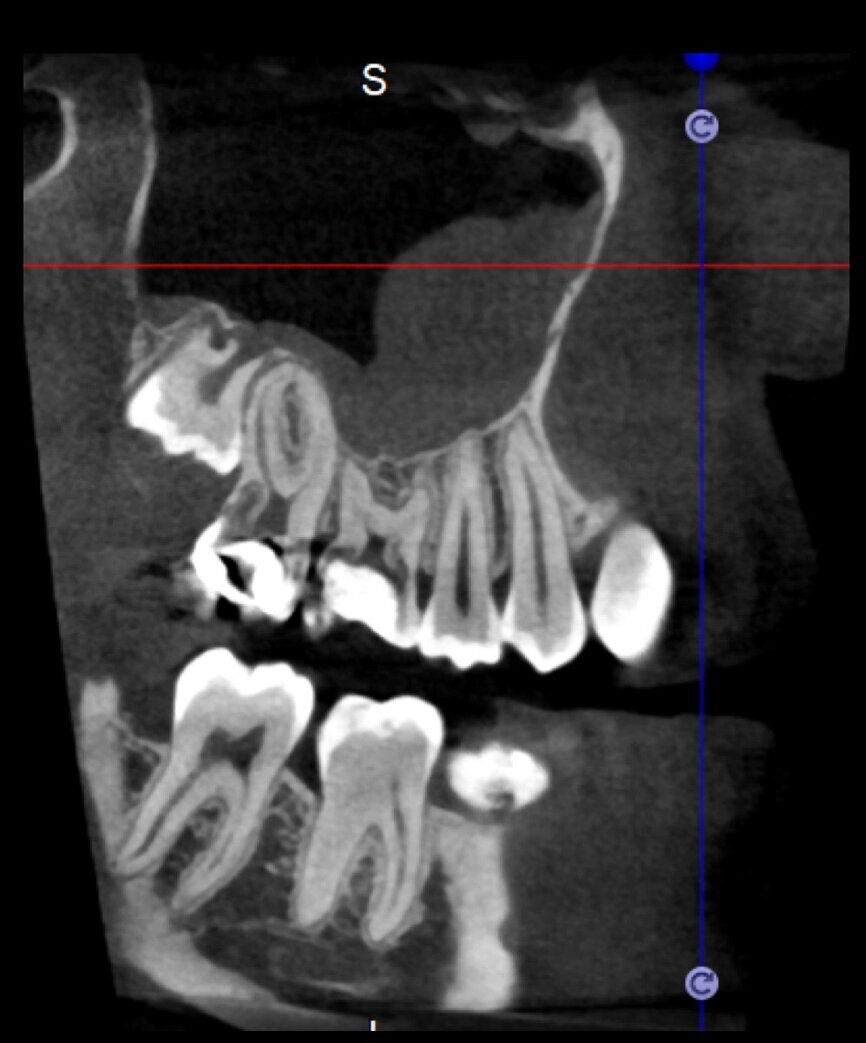
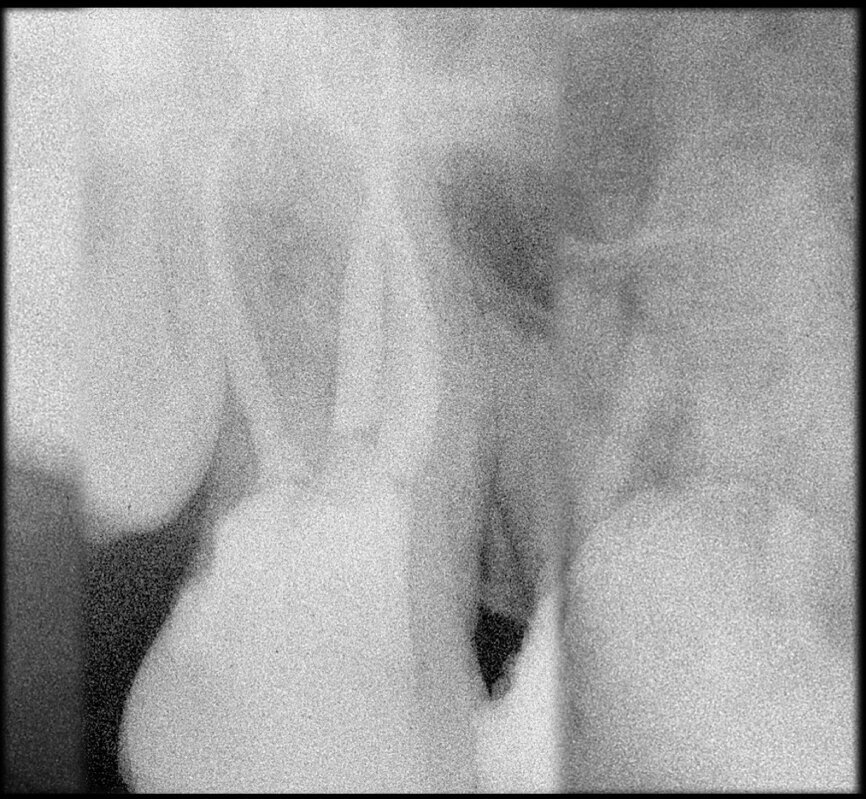
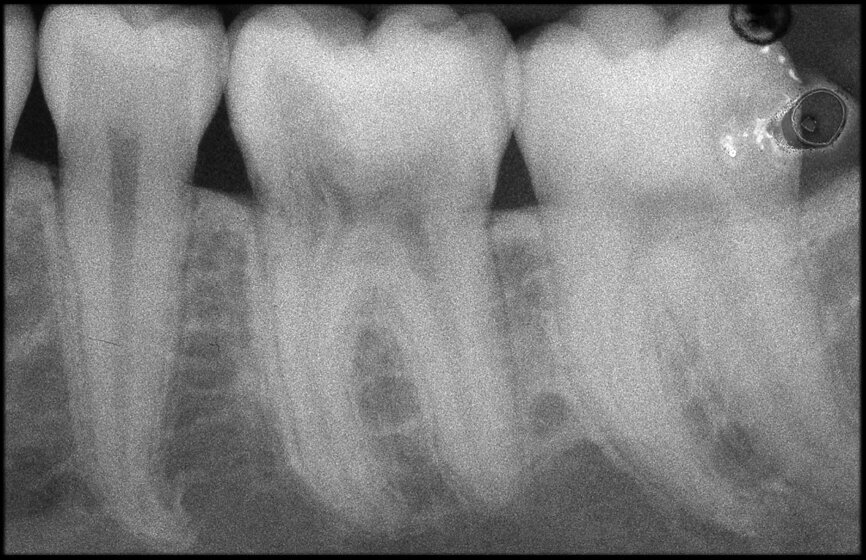
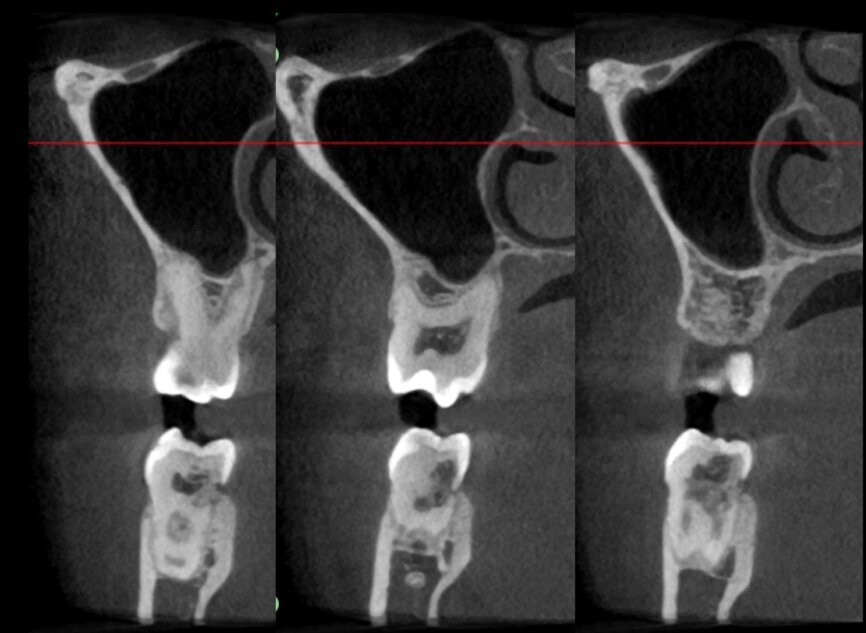
The case with which I would like to start my clinical review is a perfect example of how difficult it is to establish the origin of the patient’s symptoms on the basis of an intraoral radiograph alone. Not only does the 2D study fail to establish with certainty the presence of a lesion, but more importantly, it is impossible to establish the size, morphology and type of the lesion. An analysis of the 3D imaging, however, provides a clear picture of the clinical situation: the coronal and sagittal slices revealed the presence of a large lesion extending from the apex of the mesial root of this molar to the furcation, while the axial slices allow us to conduct a precise analysis of the endodontic anatomy and, in particular, the shape of the mesial root, which in this case was fused with the palatine root. A full overview of the case can, therefore, guide the decision-making process and direct the treatment plan towards a specific type of treatment (Figs. 1–4).
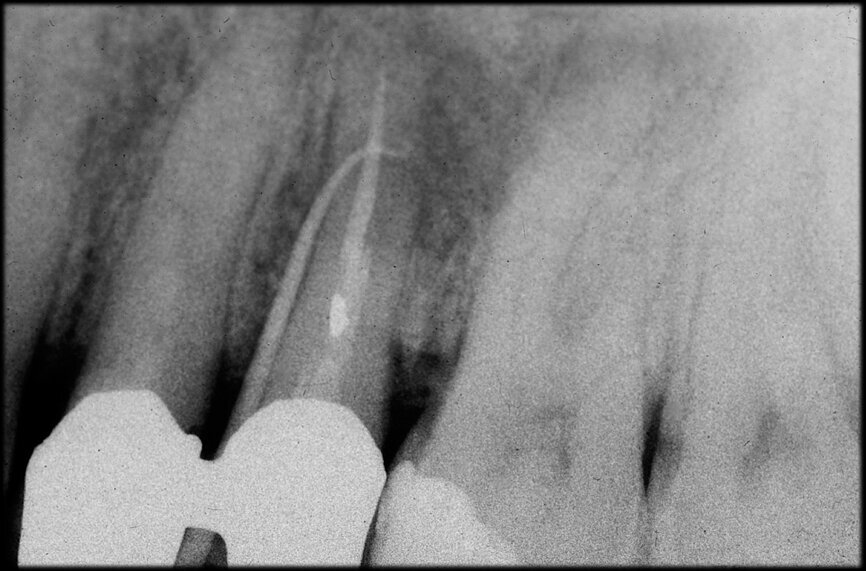
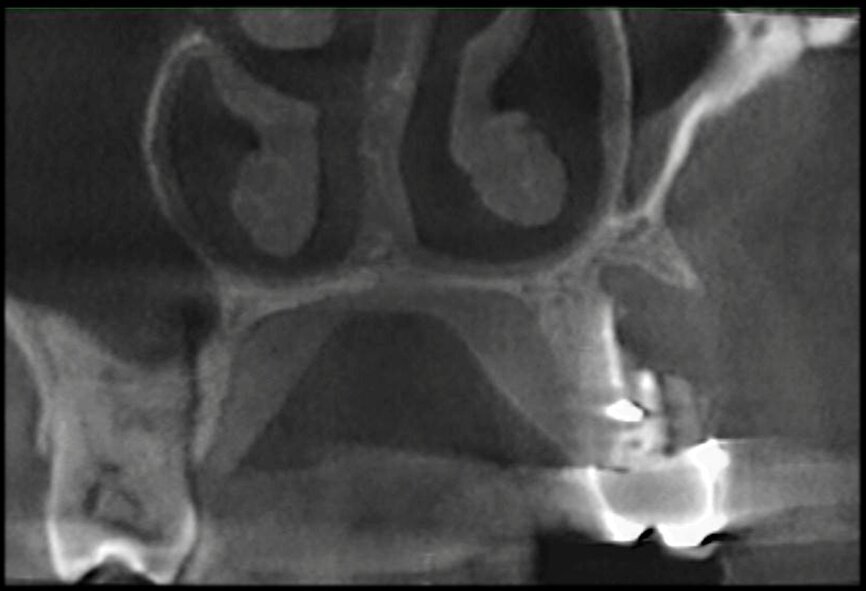
In the maxillary premolar shown in Figures 5 and 6, the fistulogram revealed the presence of an apical lesion that extended coronally to approximately the middle third of the root. The clinical decision could, therefore, propend towards orthograde retreatment; however, CBCT gave us a very different view of the situation compared with the radiograph, as it indicated that a prior treatment had irreversibly damaged the tooth, which would therefore have to be extracted.
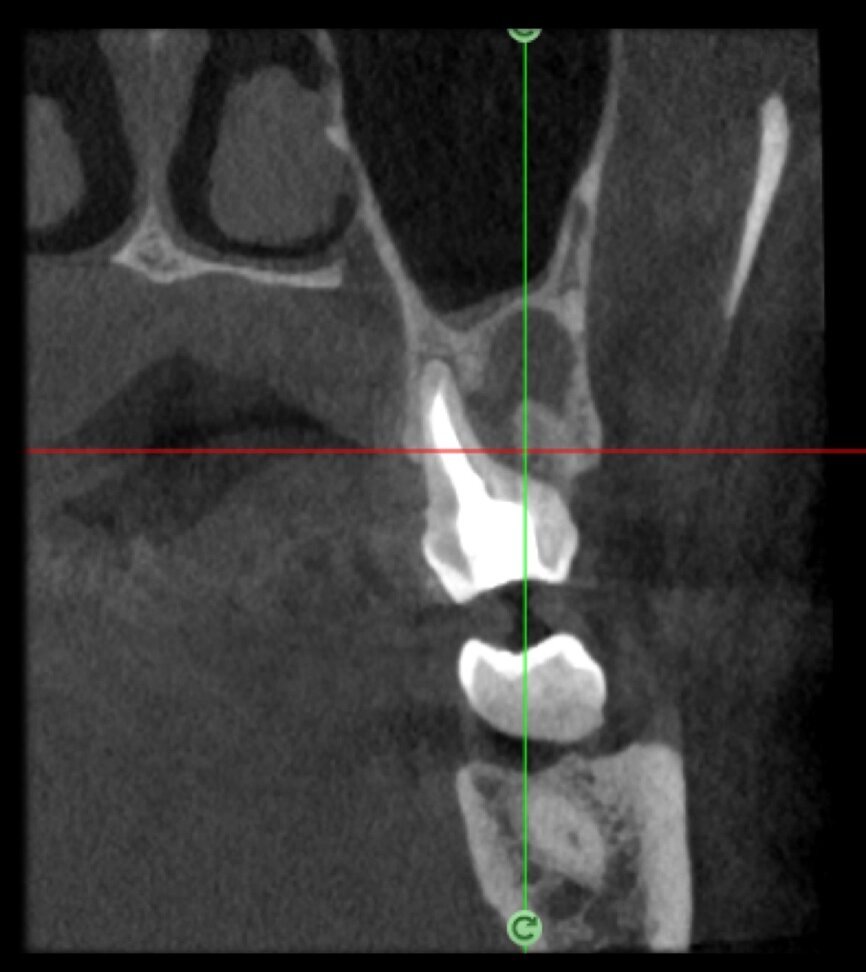
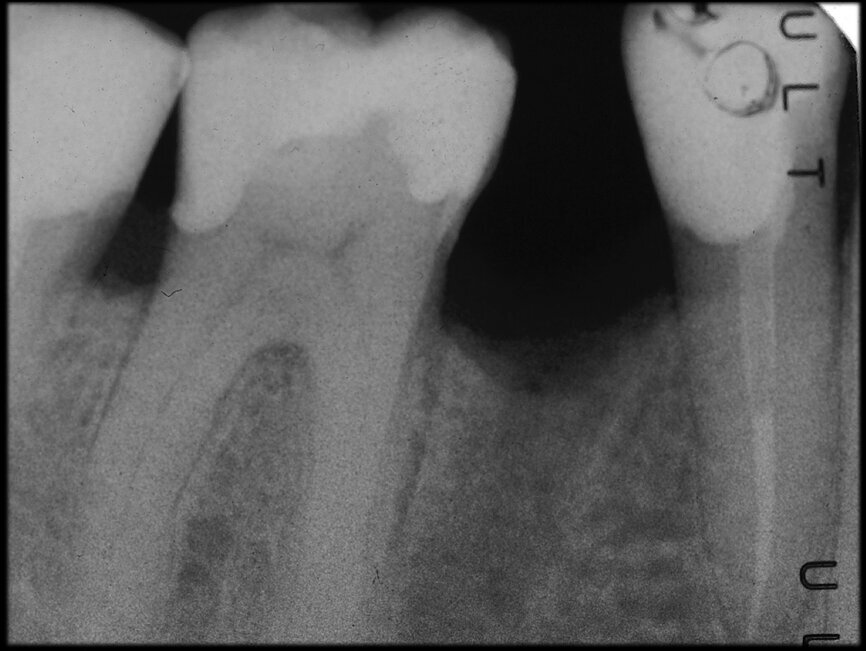
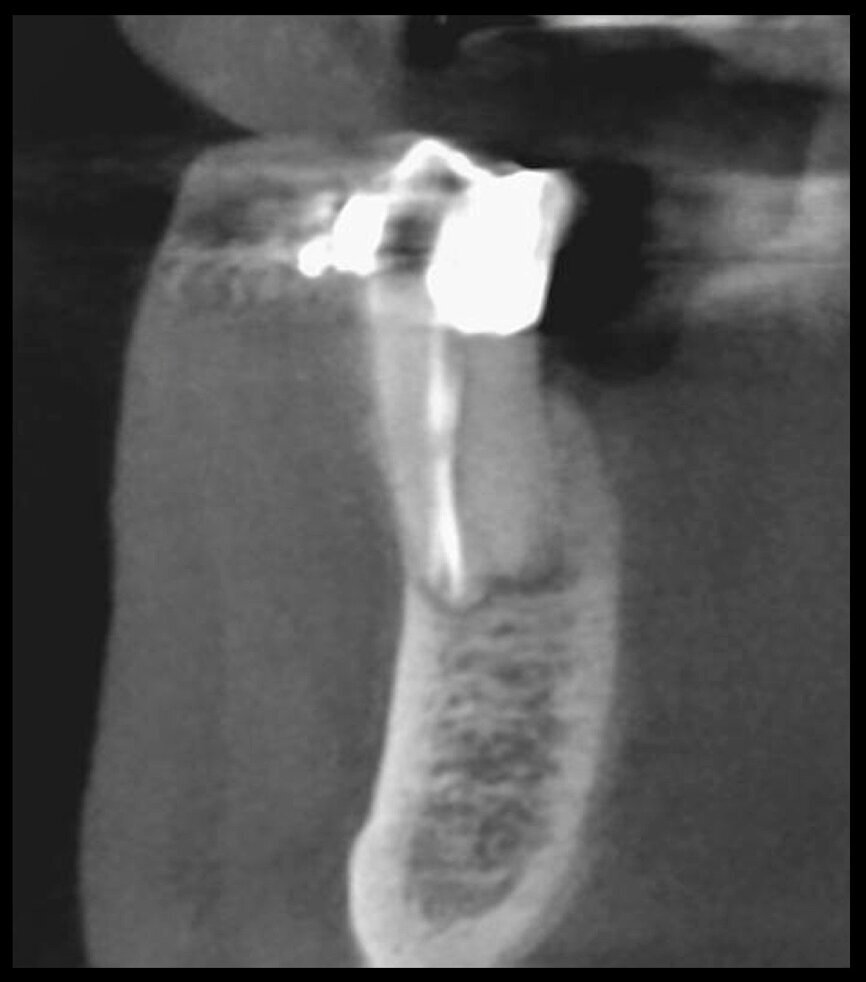
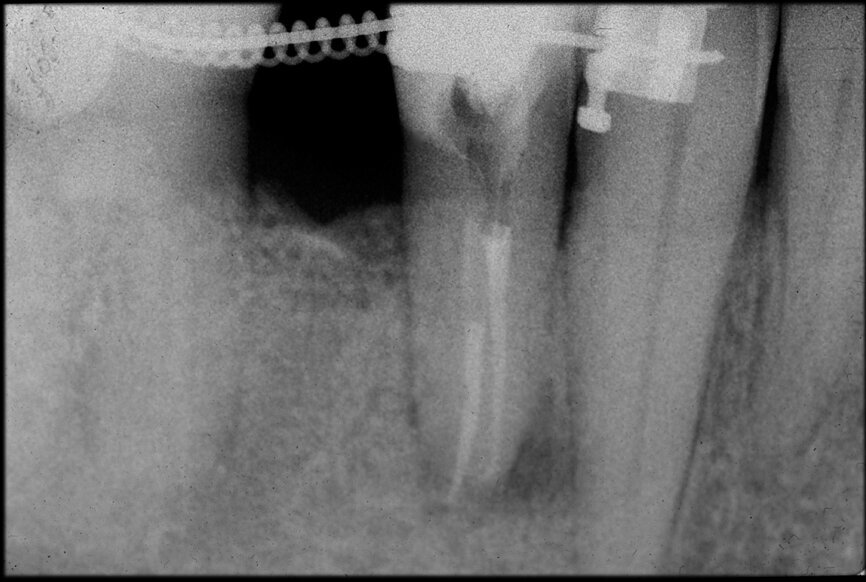
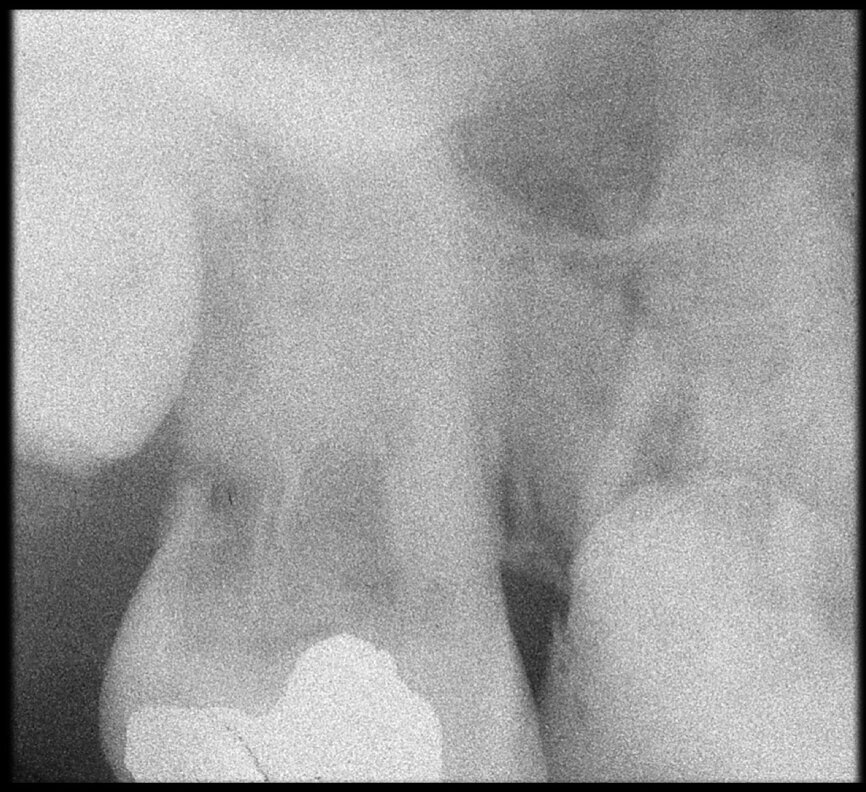
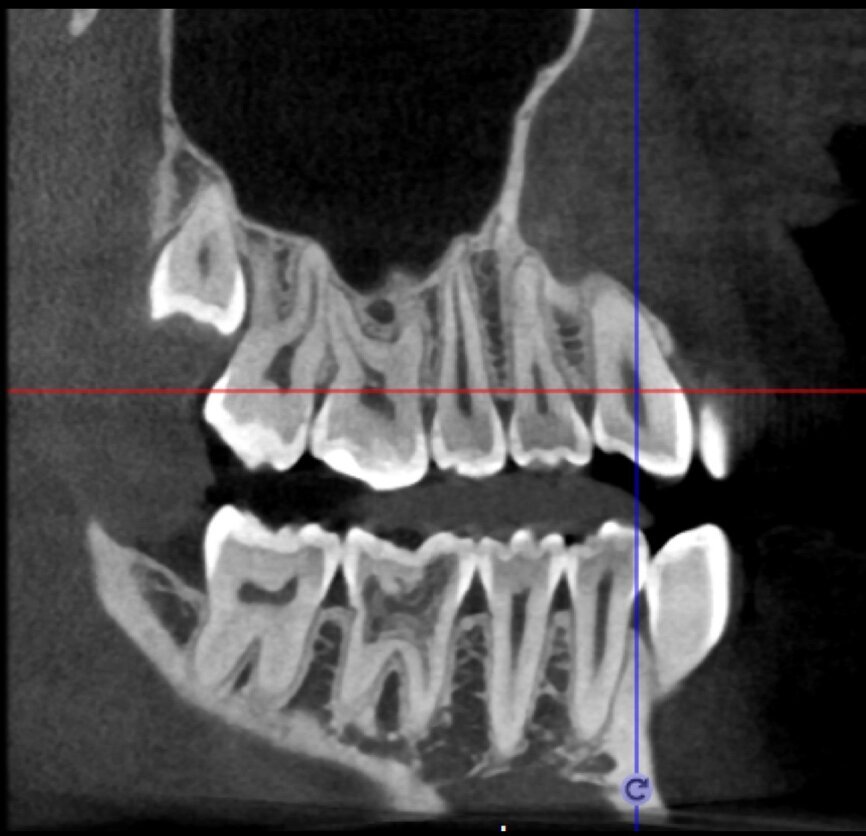
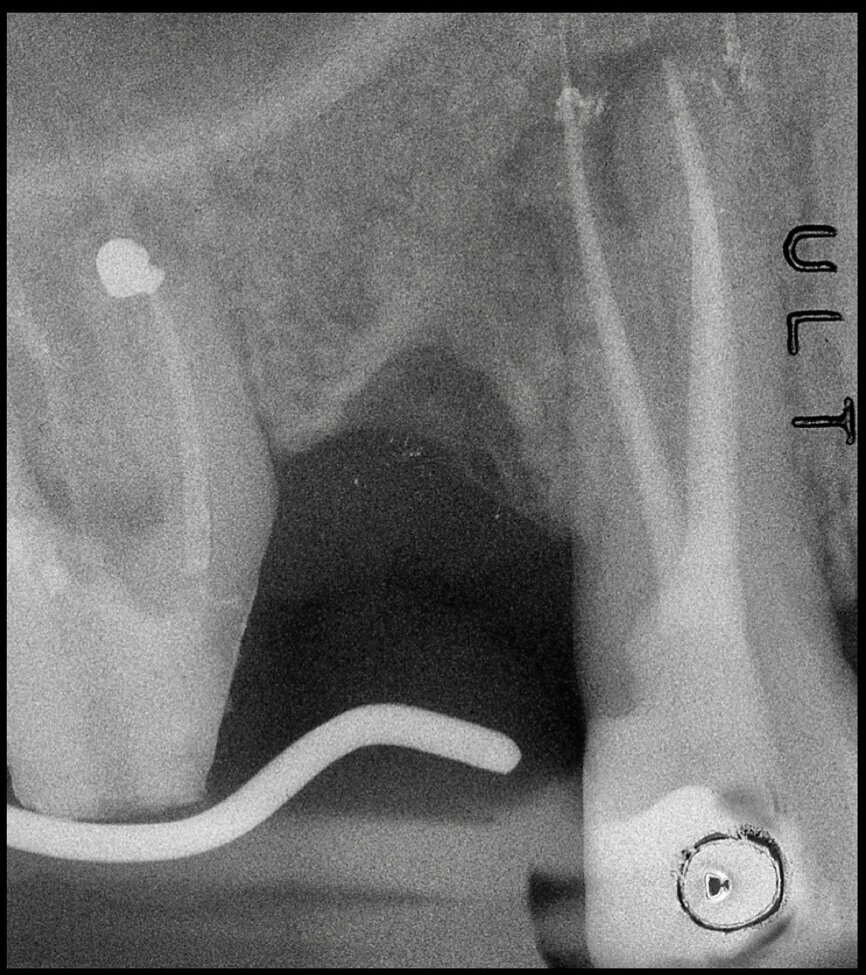
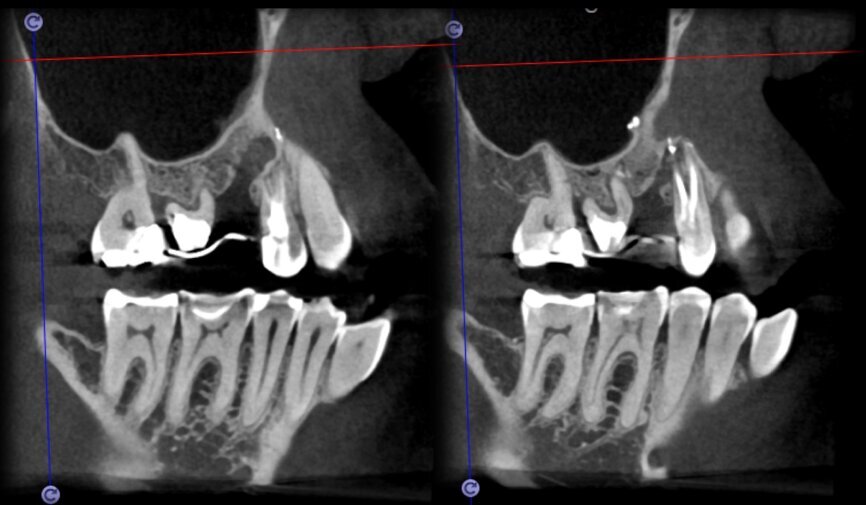
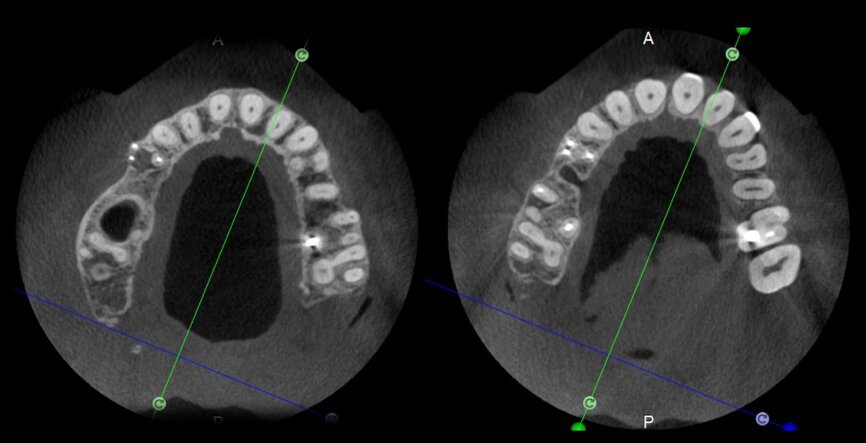
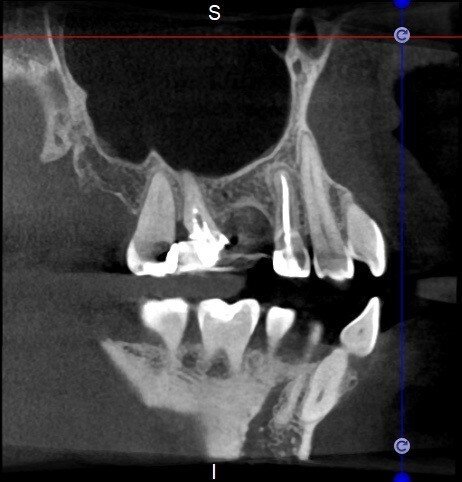
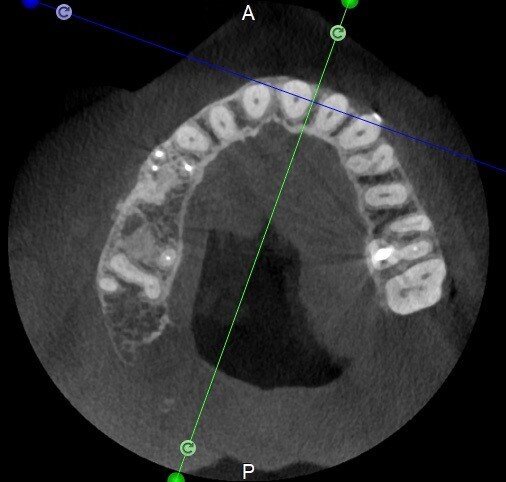
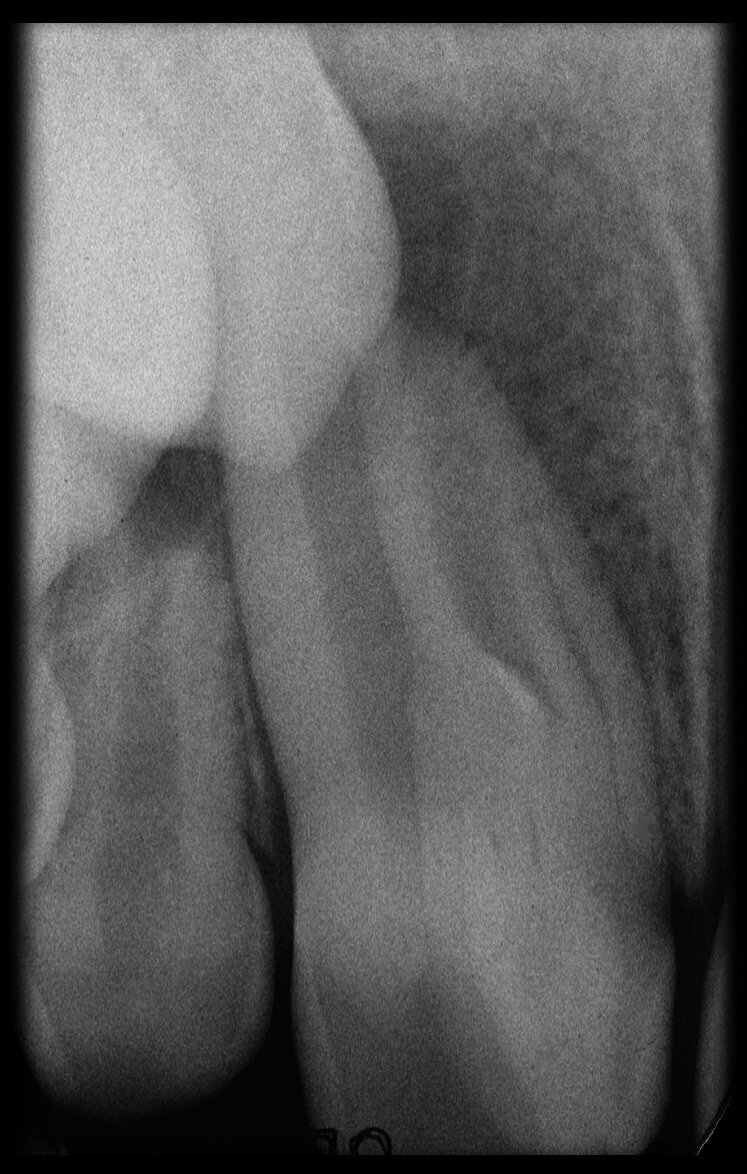
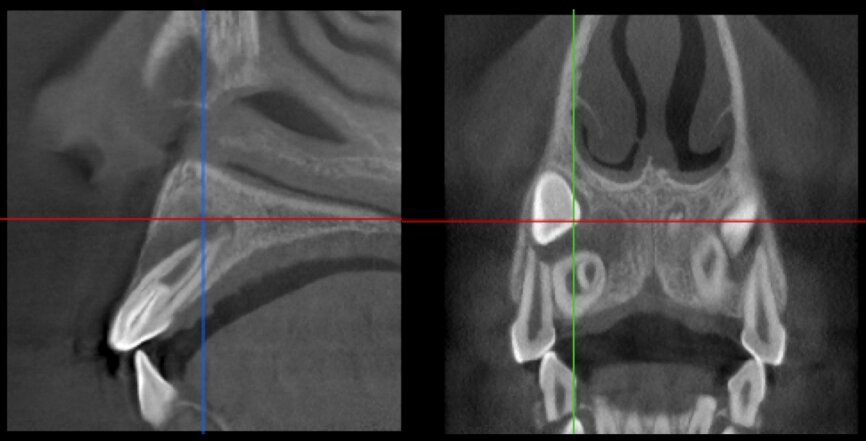
The situation was entirely different for the mandibular premolar shown in Figures 7 to 9, where, in the absence of any radiological signs of a lesion and despite the apparently correct endodontic approach adopted by another colleague, the patient complained of persistent pain which was both spontaneous and triggered by percussion of the tooth. In this case, the previous excellent root canal therapy would suggest an endodontic surgery approach, which could guarantee a higher success rate than retreatment. Given this diagnostic doubt, it was decided to perform a 3D study, which revealed an endodontic lesion caused by an untreated lingual canal. This correct diagnosis, thus, made it possible to perform selective intervention on the remaining pulp, leading to successful treatment of the untreated canal.
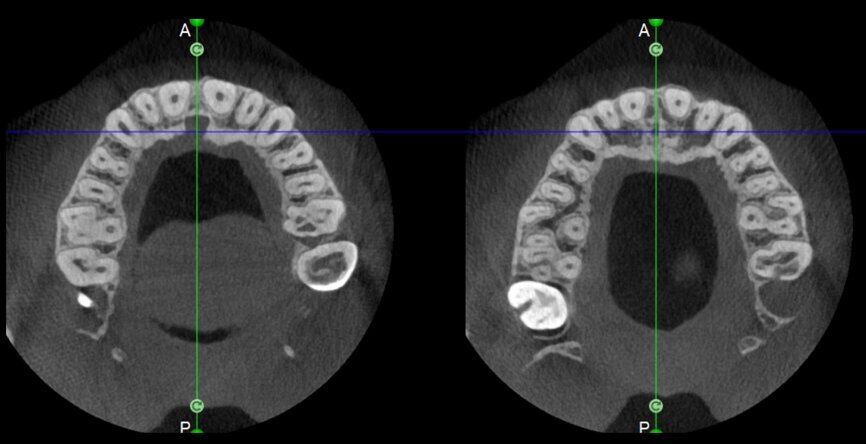
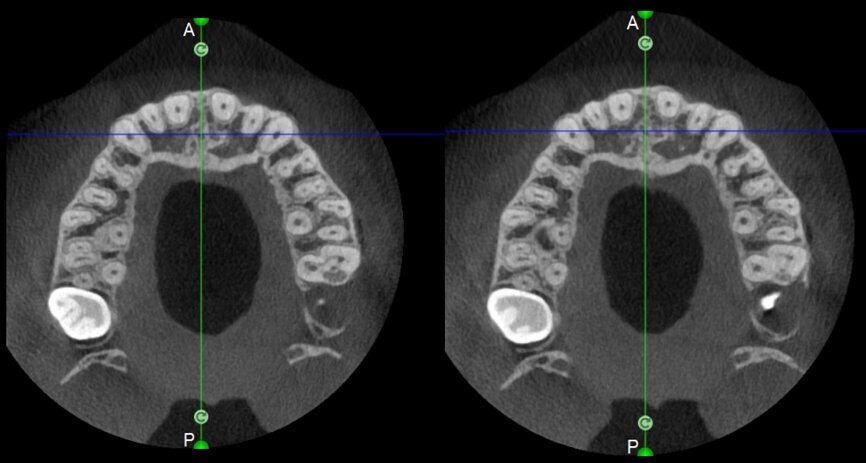
Undeniably, one of the most complex conditions to treat is external invasive root resorption, where the extent of the defect affects the treatment options. It therefore becomes sensible to perform a preoperative evaluation of the location and extent of the resorption, and the potential for recovery, thus, depends on correct 3D planning of the procedure, which can only be achieved after examination of the CBCT images. It is very important to be able to view the slices of the tooth correctly in all three planes, focusing in particular on the axial slices, which will prove to be strategic from an endodontic diagnosis point of view.
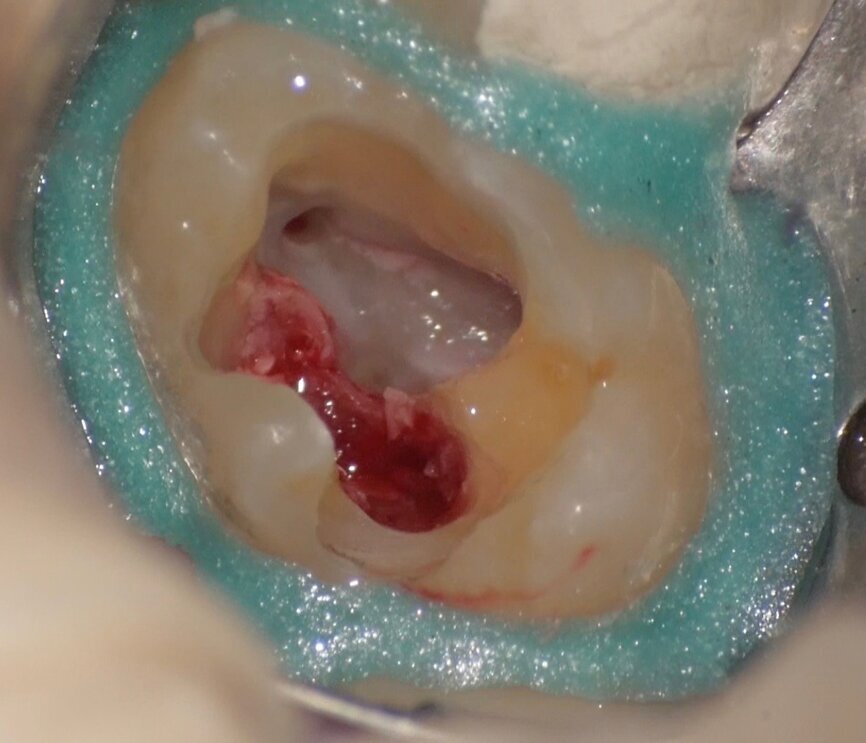
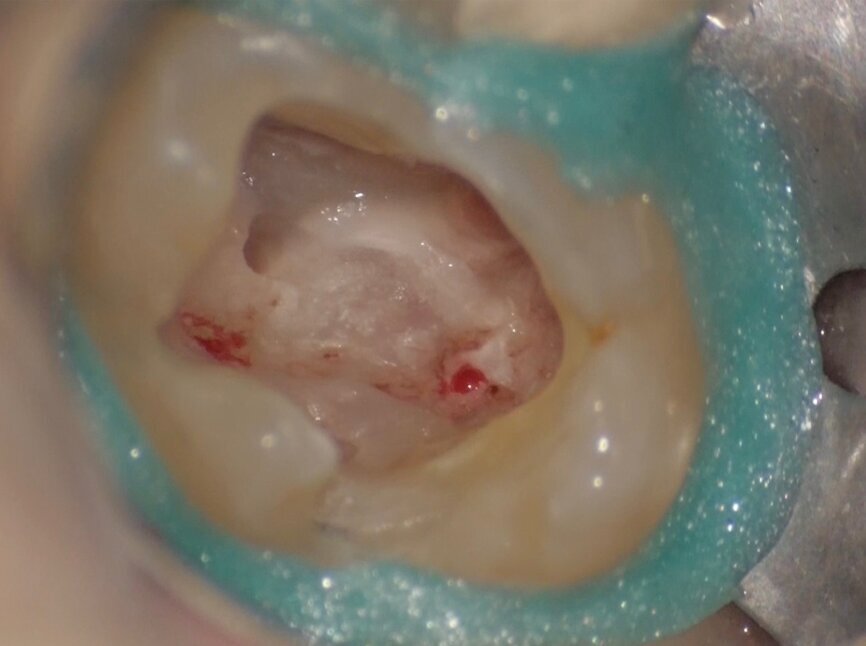
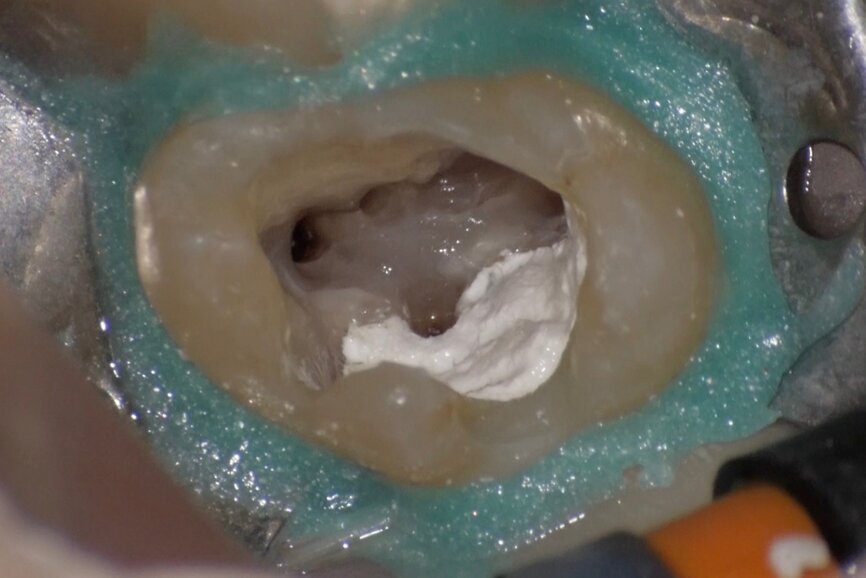
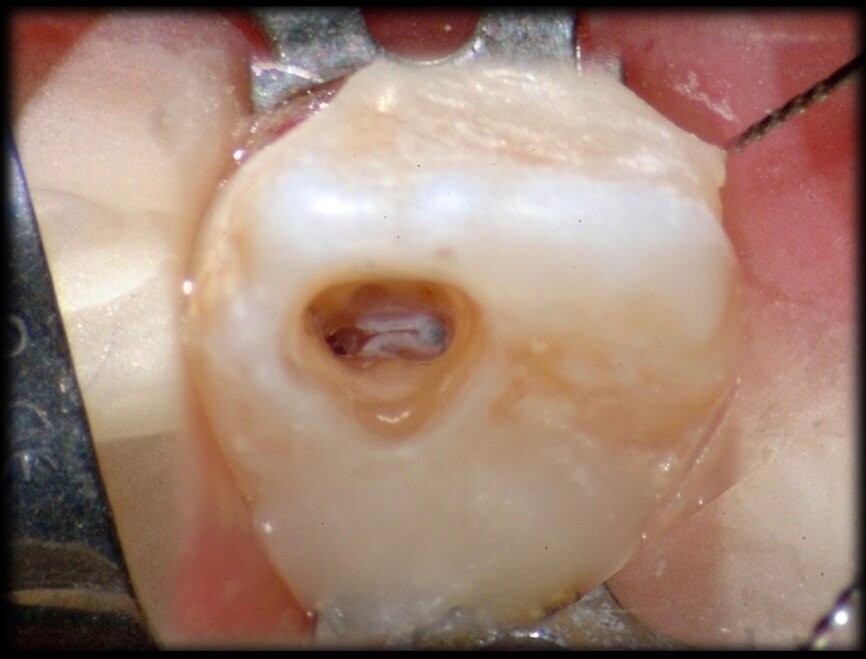
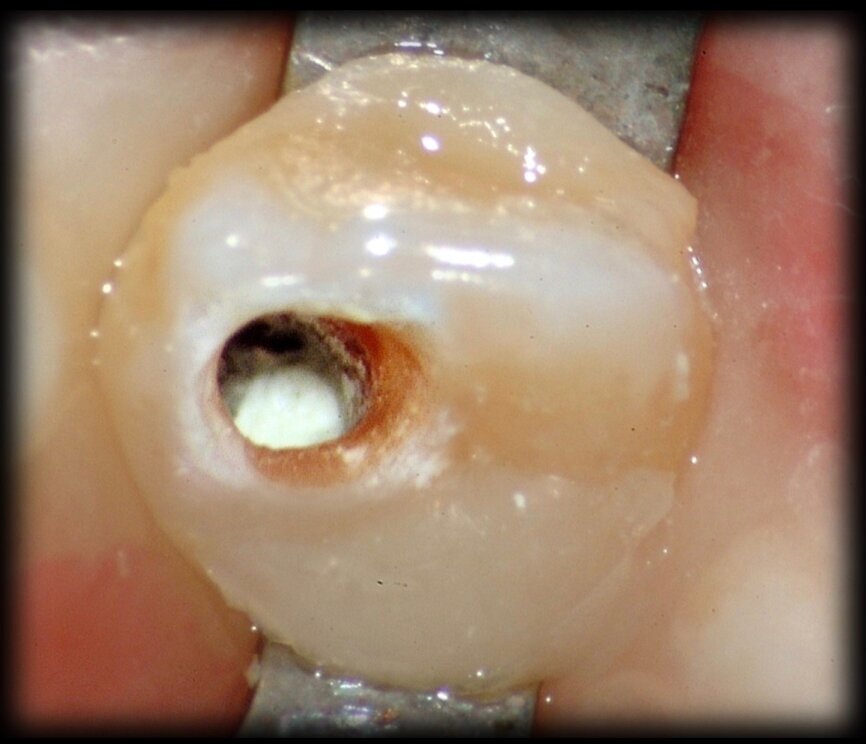
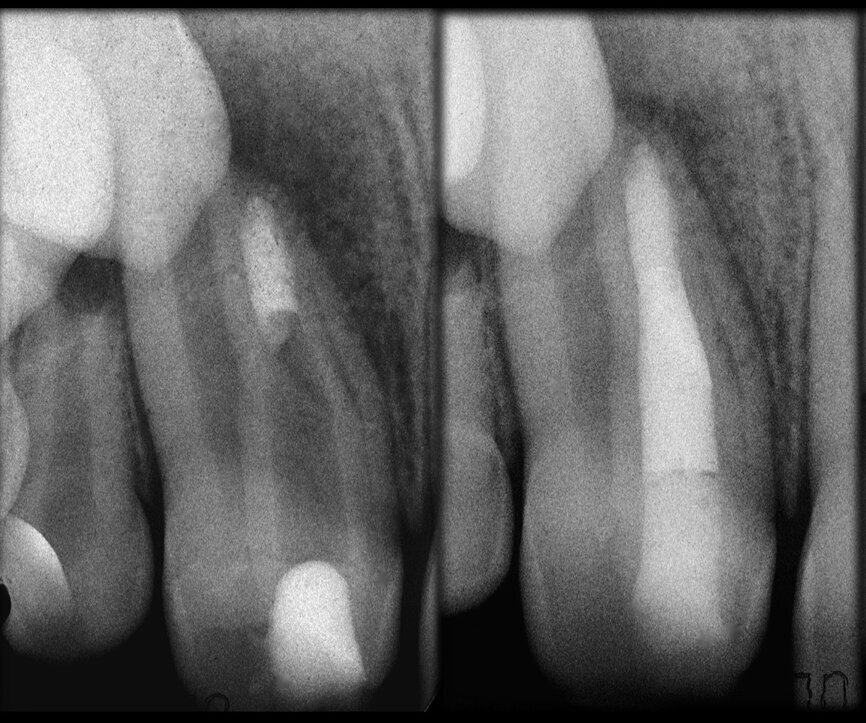
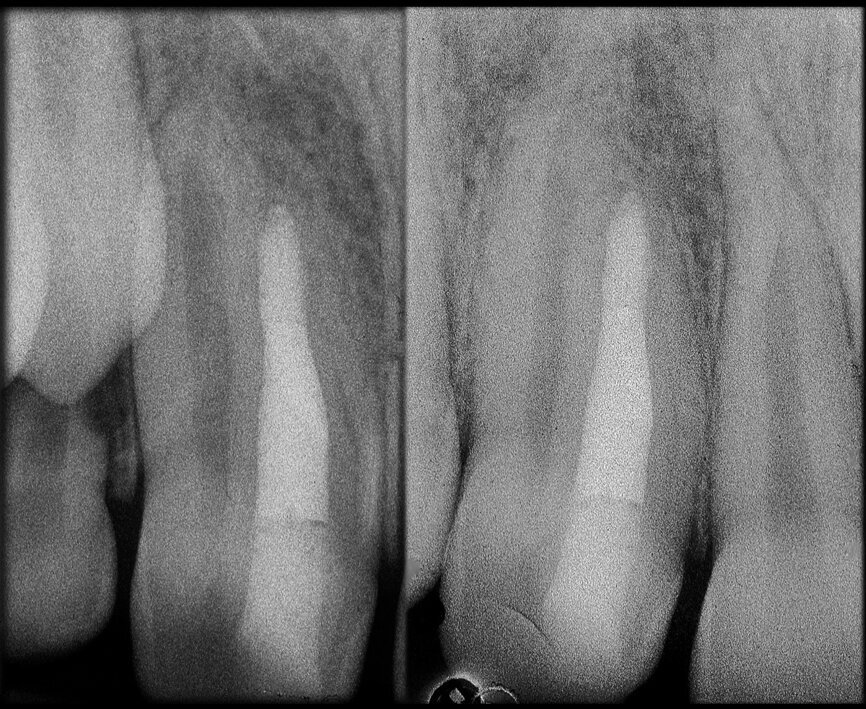
Comparing the two teeth shown in Figures 10 to 22 demonstrates just how important it is to analyse all the slices of the CBCT study correctly. We can see that, in the maxillary molar, the lesion penetrates into the pulp chamber, starting from the root’s distal surface, but remains within the coronal third of the tooth, without significantly affecting the integrity of the pulp chamber floor (Figs. 10–15). The clinical images illustrate the operative treatment phases, from resorption debridement through to repair using bioceramic cement (Figs. 16–19). The final radiographic images confirm the validity of the conservative and endodontic treatment of the tooth. The situation is completely different for the mandibular molar, where the evaluation of the CBCT scan clearly reveals the extent of the resorption, which invades the pulp chamber floor until the furcation, a situation that cannot be determined from observing the preoperative radiograph alone (Figs. 20–22).
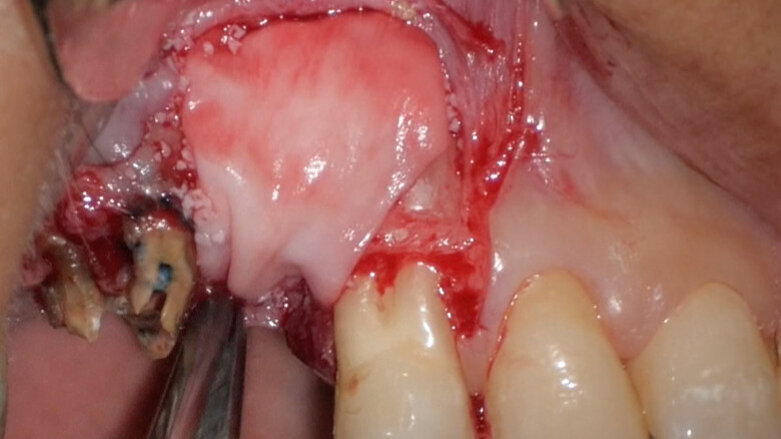
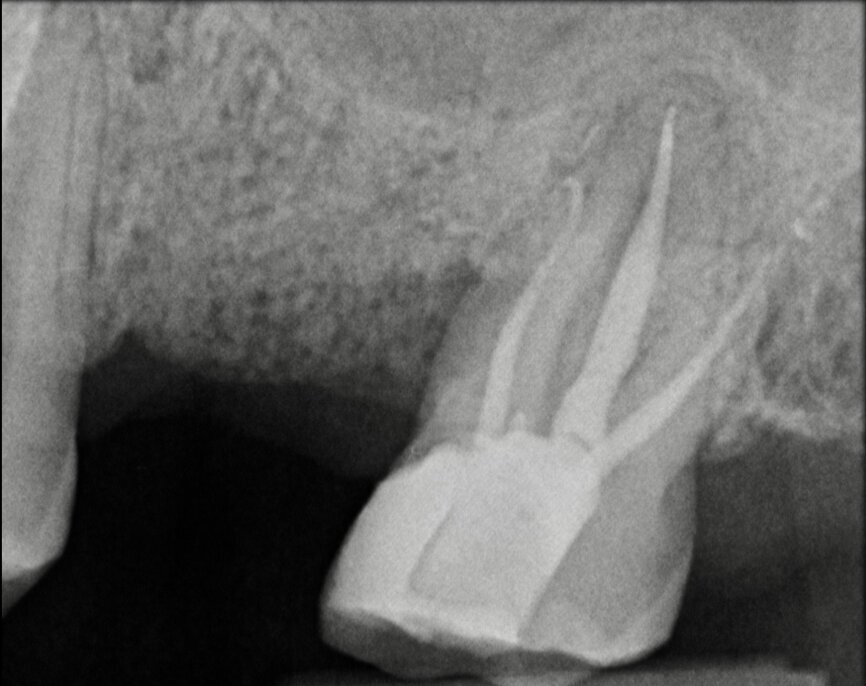
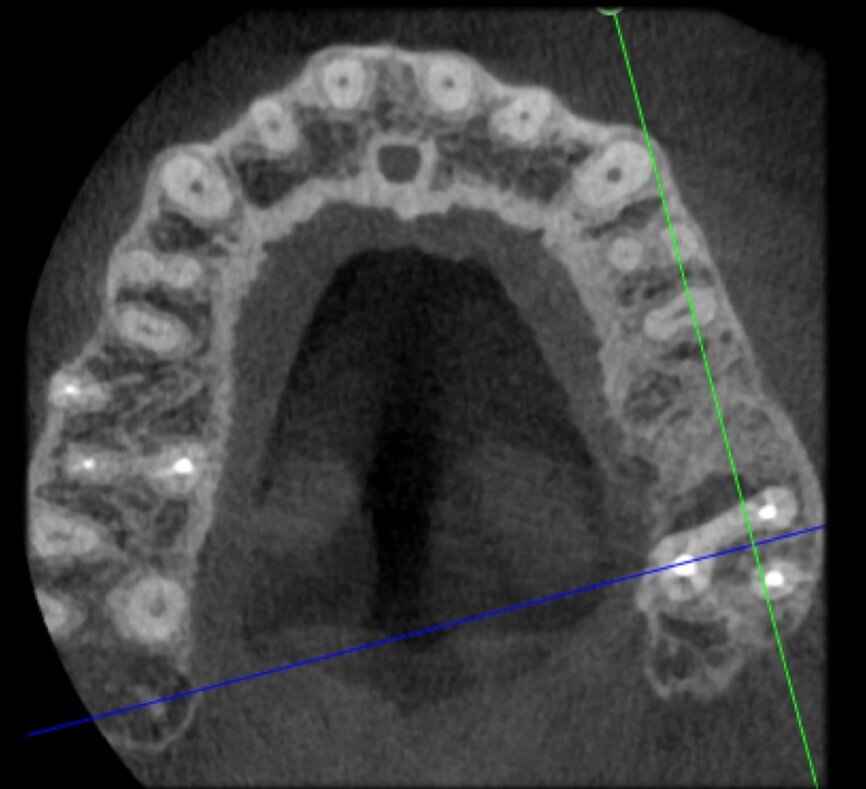
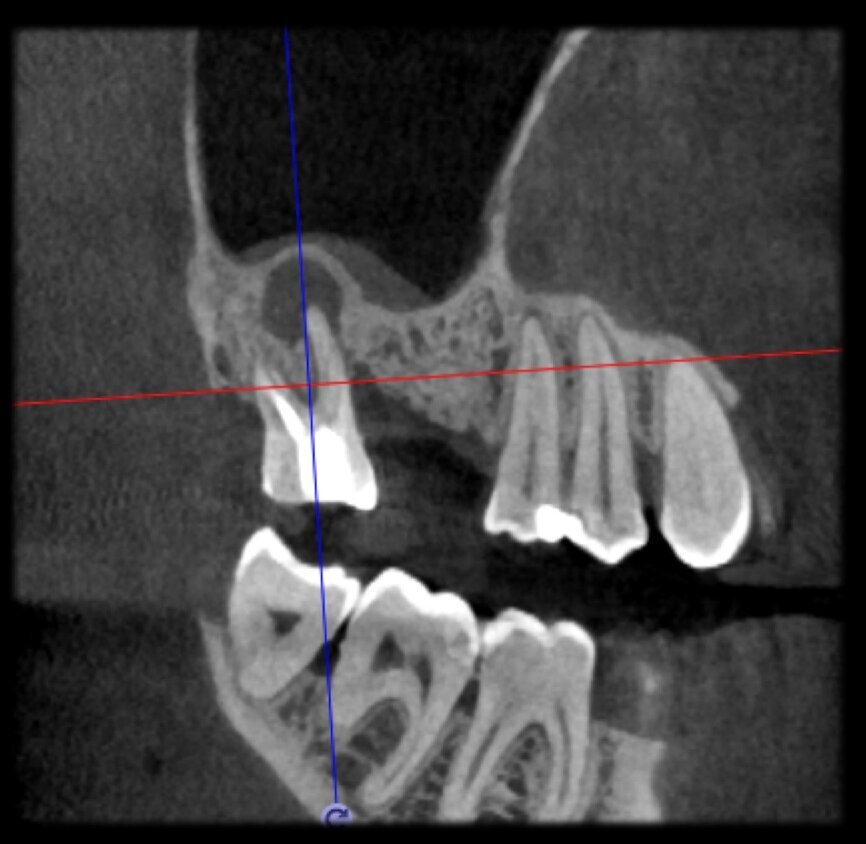
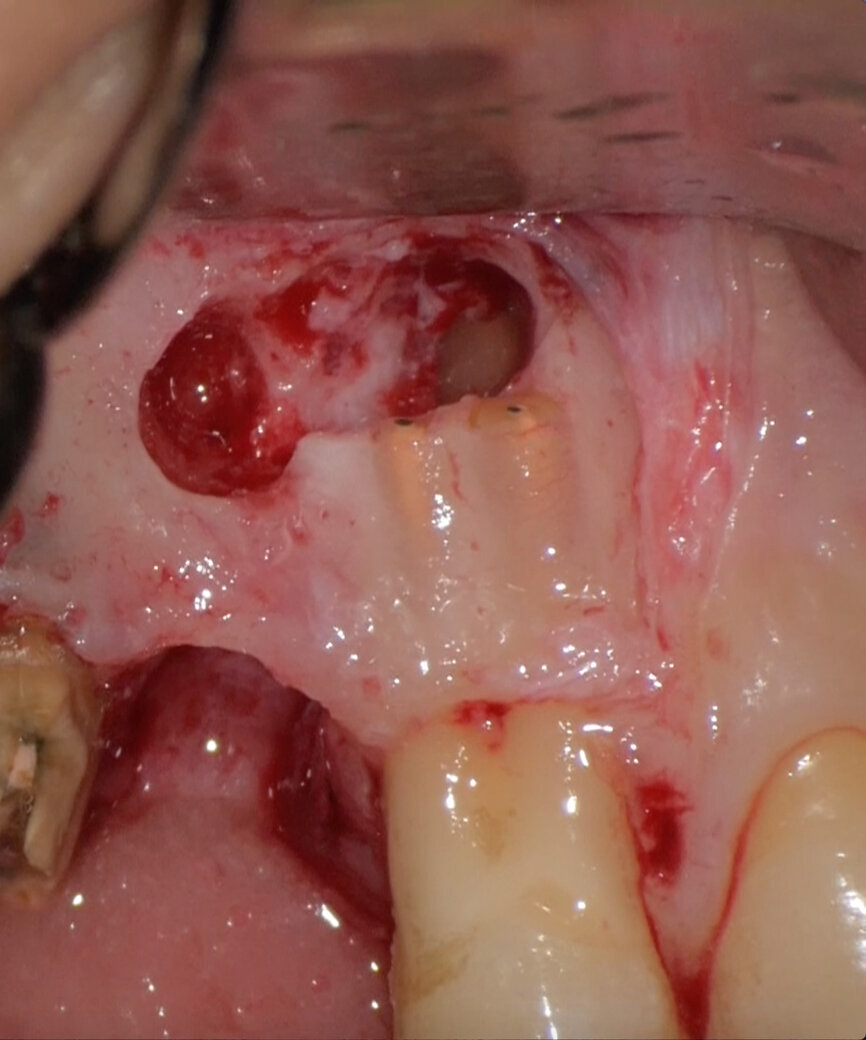
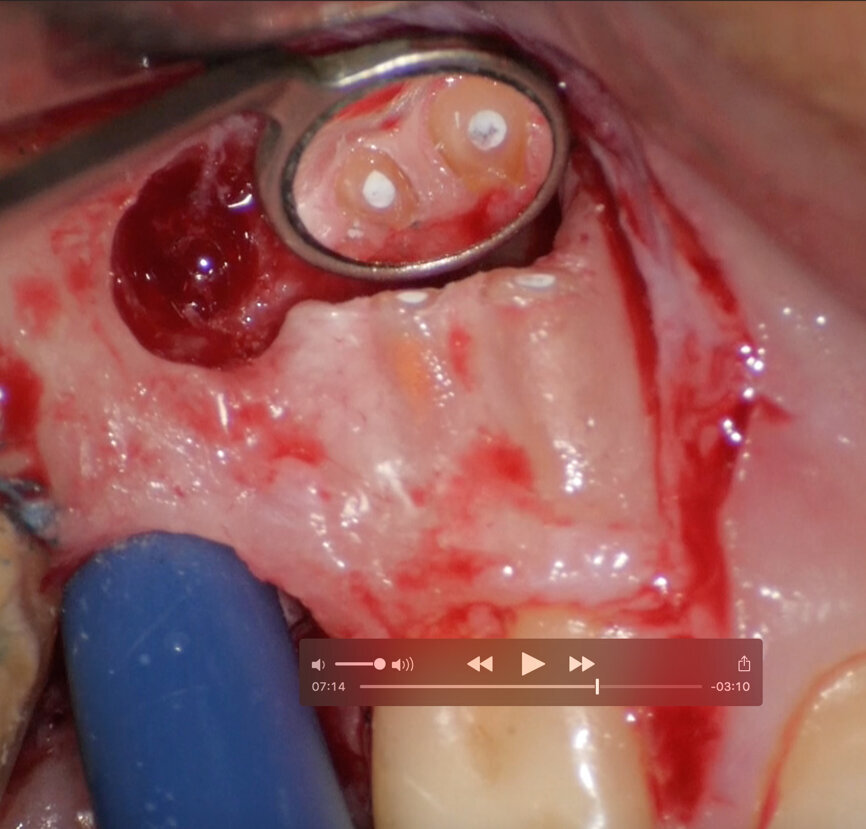
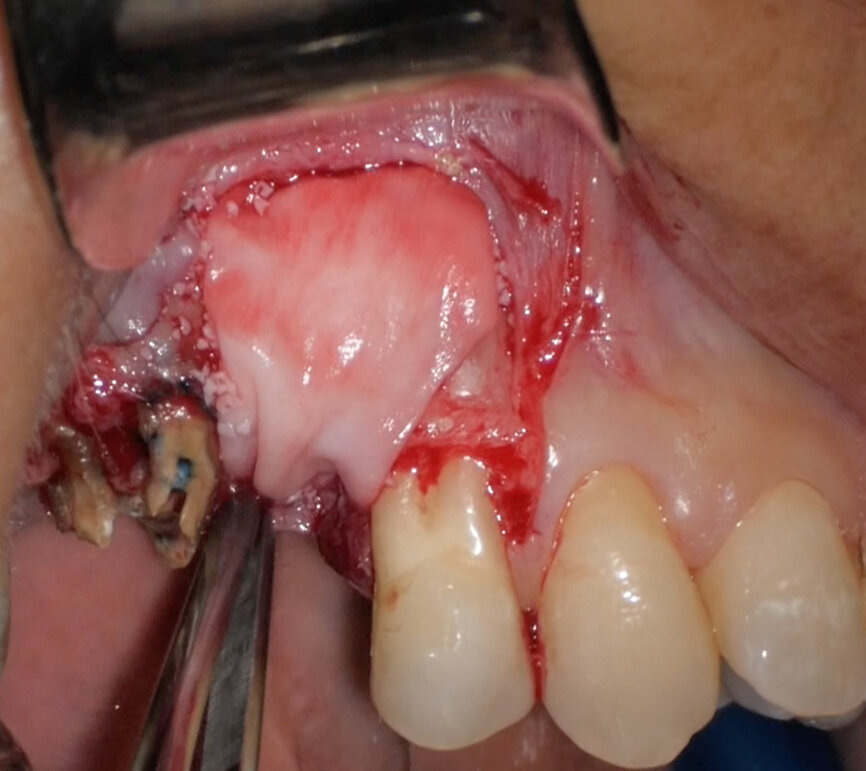
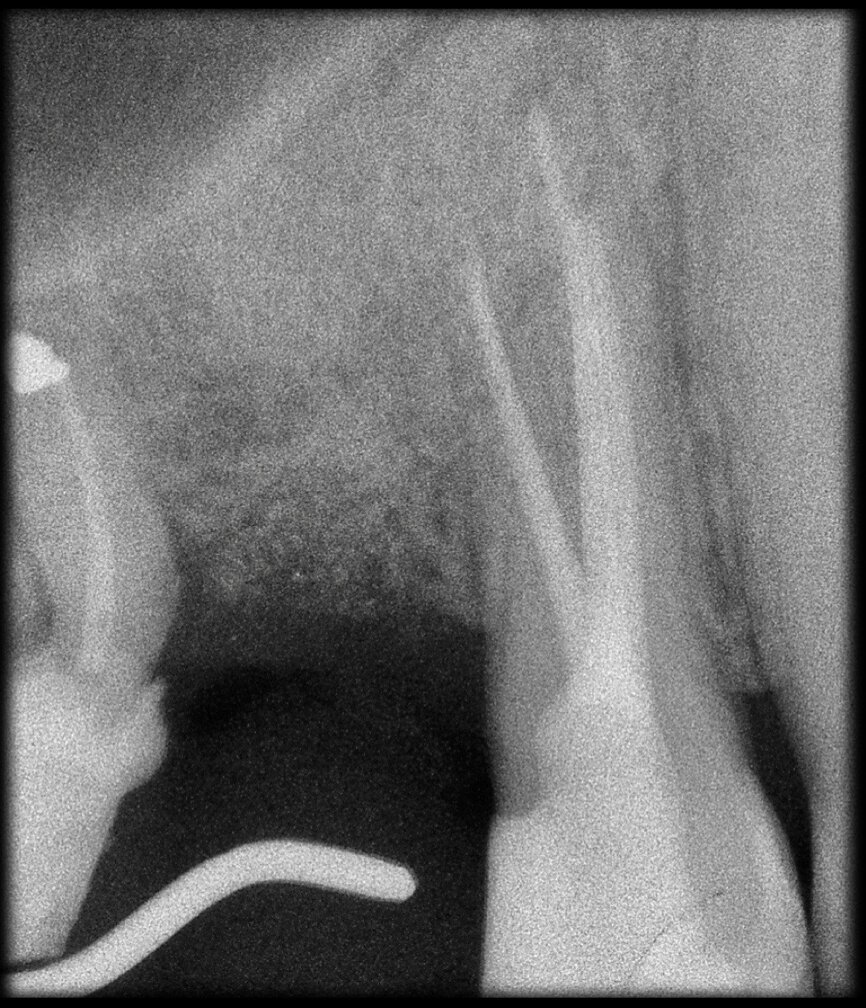
Preoperative CBCT evaluation is useful in cases requiring a surgical approach, not only in order to confirm the presence of a lesion but also to plan the procedure and, in particular, identify the type of surgical incision to be used, based on its size and location (Figs. 23–25). This specific case is characteristic of this situation. The intraoral radiograph did not make it possible to ascertain the extent of the lesion, which involved not only the apical region of the premolar but also a distal edentulous segment. This region would need to be treated with regenerative therapy in order to guarantee correct healing of the area, with subsequent insertion of a membrane, the flap must be protected using a totally different approach to that required for endodontic surgery. The intraoperative images illustrate the various stages of the procedure (Figs. 26–28). The CBCT scan performed 12 months later confirmed complete healing of the apical lesion and perfect graft integration (Figs. 29–31).
Another compelling advantage of this 3D technology is the possibility of using a minimally invasive approach for performing cavity access. For demonstration, the next case involves a dens in dente. The CBCT scan shows a separation between the two canal systems of the canine and the decay involves the portion of tooth where the dens in dente is present. The treatment plan therefore involved root canal therapy for just one portion of the pulp, while the other was to be kept vital. The image sequence of the treatment shows how it was possible, using CBCT and a surgical microscope, to perform a minimally invasive access, which spared much of the canine’s clinical crown and kept the disease-free portion of the tooth vital. The radiographic follow-up confirmed complete healing of the lesion and the vital part of the canine did not present any signs of disease six years later (Figs. 32–37).
Editorial note: This article was published in CAD/CAM - international magazine of digital dentistry No. 02/2019.
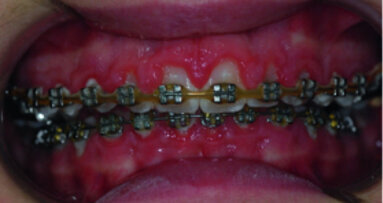
In recent decades, we have witnessed the substantial development and expansion of the use of fixed orthodontic appliances. While their application has many ...
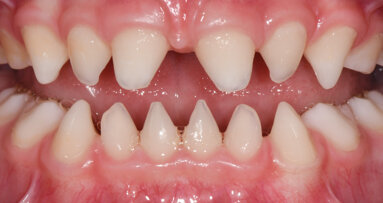
Owing to the introduction of magnification principles in dentistry, new techniques have been implemented for the successful performance of endodontic ...
3D printing has emerged as a disruptive innovation in restorative dentistry, offering a high degree of precision, efficiency and customisation.1, 2 Recent ...
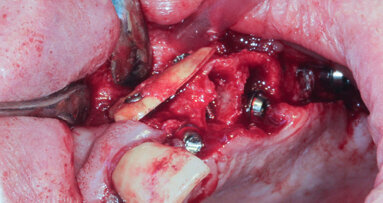
Treating bone insufficiency is a familiar challenge for all implant practitioners. Such insufficiency can compromise the placement of an implant, its ...
BRUSSELS, Belgium: The European Federation of Periodontology (EFP) has announced a new guideline aimed at helping oral health professionals around the world...
EDMONTON, Canada: A team of researchers at the University of Alberta has secured funding to develop a 3D ultrasound device that would allow dentists to ...
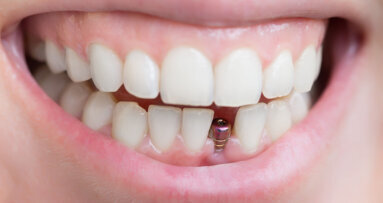
Implant-supported restorations are becoming increasingly popular in contemporary dentistry, and the study of the osseointegration process has led to the ...
Sensitive or traumatised patients require special attention, whether they are adults or children. Sometimes both the clinician and the patient share a ...
Besides running a private practice concentrating mainly on endodontic dentistry, Dr Filippo Cardinali gives lectures in theoretical and practical courses on...
LONDON, England: Driven by the NHS dental crisis, an increasing number of UK patients seeking cheaper dental work overseas are encountering unexpected ...
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 pm EST (New York)
Live webinar
Thu. 11 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 11 June 2026
2:00 pm EST (New York)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Fri. 12 June 2026
8:00 am EST (New York)
Dipl.-Hdl. Joachim Brandes
Live webinar
Mon. 15 June 2026
11:00 am EST (New York)
Dr. Cristian Scognamiglio, Dr. Alessandro Perucchi



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East







































To post a reply please login or register