I enjoy seeing the articles in cosmetic dentistry in which clinicians recount their creation of magnificent works of art through digital restorative dentistry. In most of the case studies I’ve read, I am sure the patient fees reach well over US$15,000 or more.
Let me ask you this: what percentage of your patients whose fee is US$15,000 or more are ready to start care immediately after you present their treatment plan? I have directed this question to thousands of my dentist audience members over the last decade and the overwhelming response is “fewer than 5 %”. Is this because patients do not understand dentists’ treatment recommendations? Or is it that the fee does not fit into their budgets? Chances are that both these apply.
embedImagecenter("Imagecenter_2_193",193,"small");
As dentists we are pretty good at helping patients understand us and our treatment recommendations. What we are not good at is understanding our patients and the manner in which our treatment recommendations must fit into their lives. If you have heard it once, you have heard it a thousand times: the key to case acceptance is patient education. Go to dental seminars, read journals, listen to consultants; most of it sounds the same―educate, educate, educate. Now let me ask you this: is it true? Is patient education the solution to case acceptance?
If it is, then why do many new patients who have been thoroughly examined, educated and offered comprehensive treatment plans leave your practice and never return for care? Is it that you did not educate them sufficiently? Or is it that in the challenge of case acceptance, patient education is not the only answer?
Let’s consider the new patient process and case presentation and learn when patient education works for us and when it chases patients out the door.
Inside-out versus outside-in
How do we get patient education to work for us? Let’s first make the distinction between an inside-out versus outside-in new patient process. The traditional new patient process is inside-out. It begins by studying the inside of the patient’s mouth―the examination, diagnosis and treatment plan. It is after this inside look that we educate the patient with regard to all his/her problems―how he/she got them and what we can do about them, for example case presentation. After case presentation, we quote our fees and discuss financial arrangements. It is only once we have gone through our inside process that we discover what is happening outside the patient’s mouth―his/her budget, work schedule, time and significant life issues.
The flow of conversation starts with inside-the-mouth conditions and ends with outside-the-mouth issues. I label this traditional way of managing the new patient the inside-out process (Fig. 1).
For patients with uncomplicated dental needs―fees of US$3,500 or less―the inside-out approach with appropriate patient education works well. Here’s why:
First, patients with minimal clinical needs are often unaware of them. Patients with conditions such as periodontal disease, asymptomatic peri-apical abscesses and incipient carious lesions must be made aware of them and educated regarding their consequences. Patient education is the driver of case acceptance when patients are unaware of their conditions.
Next, the inside-out process works well for patients with fees of US$3,500 or less because the outside-the-mouth issues―fees, time in treatment and life issues―are such that most patients can proceed with your treatment without undue hardships or inconvenience. Dental insurance reimbursements, patient payment plans such as CareCredit and credit cards usually sooth the sting of fees for US$3,500 or less. Fees at this level are not insurmountable and usually do not anger or embarrass patients out of your office. But what if you present complex dentistry for more than US$3,500?
Let’s suppose your fee is US$10,000 and it involves multiple, long appointments and your patient would lose time from work? Do outside-the-mouth issues get in the way of case acceptance now? Yes, they do. Does patient education make the unaffordable affordable? No, it does not. How do I know? You have proven it, have you not?
It is with the patient whose fee is greater than US$3,500 that I recommend an outside-in approach. Employing an outside-in approach involves initiating your new patient procedures with conversations―telephone and the in-office new patient interview―that focus on understanding what is happening outside the patient’s mouth, such as significant life issues, budget and work obligations. Later in this article, I’ll show you how.
After we have an understanding of outside-the-mouth issues, we do our examination. Then, during the post-examination conversation and case presentation, we link our treatment recommendations to the realities of their outside-the-mouth issues. Let me show you how.
The flow of conversation starts with outside-the-mouth issues and ends with inside-the-mouth treatment recommendations. I label this an outside-in process (Fig. 2). An excellent example of an outside-in process is the purchase of a home. Imagine you and your spouse decide to buy a new house. You go to a real estate agent and, just a few minutes into the conversation, you talk about price range, neighbourhood, schools, proximity to work, financing and down payment. These are all big picture, outside-the-home issues. Once you settled on the broad outside-the-home issues then, and only then, does it make sense to begin discussing the detailed inside-the-home issues, such as room size, carpet and tile selection, lighting, etc. Good estate agents discover what the suitability factors of home buying are (price, down payment, monthly payments, location, etc.) before they get into the inside details. In other words, the flow of conversation is outside-in.
Now imagine you and your spouse go to the estate agent, but this time she is a former dentist and uses the traditional inside-out process she used as a dentist. As soon as you sit down she begins educating you on the inside-the-house issues―the difference between cement slabs versus crawl space foundations and vinyl siding versus brick exteriors. She goes as far to recommend another appointment with her so she can show you how to keep your house clean before you buy one. She does all this before she has any idea of what you can afford and where you want to live. What would you think? You would think about finding another estate agent, would you not?
How many of your complex-care patients, after experiencing your inside-out process, find another dentist for the most likely reason that you spent a bunch of time educating them on inside-the-mouth details before you had any idea what was suitable for them? You educated them right out your door.
An outside-in process works best for complex-care patients. Here patient education is not the driver of case acceptance. This is why: first, patients with complex needs often come into your office with a specific complaint―embarrassment about their appearance, aggravation by their dentures or fear of losing their teeth. They do not need to be educated about their chief complaint. They may not be aware of all their conditions, but it is most likely that they have lived with the complaint that brought them into your office for a long time.
Next, many complex-care patients have heard the patient education lecture about plaque, pockets and sugar many times before. It’s old news and thus not a subject that distinguishes you. For many patients, patient education efforts bounce off like BB’s fired at icebergs. Expecting to influence them into a US$10,000 treatment plan that does not fit into their budget by showing them how to floss well is naïveté.
Let me be clear at this point: we are going to spend some time on the patient education process with complex-care patients, it is just not one of the first conversations we will have.
The first conversations we will have with complex-care patients are about discovering outside-the-mouth issues—just like the suitability conversation with the estate agent. The outside-the-mouth issues of budget, time, work schedule, health issues are what I call fit issues. These are the issues into which your treatment plan must fit. Become good at discussing fit issues and you will save an incredible amount of time, you will sell much more dentistry and you will no longer blow patients out of the water―and out of your practice.
Fit versus change
The earlier influencers in my dental career emphasised that a significant part of being a good dentist is to get patients to change. Change the way they clean their teeth, change what they eat and change the priorities in their life and put dental health at the top. It took me ten years and thousands of patients to realise that patients change when they are ready, not when I tell them to.
I learned to replace the concept of change with the concept of fit. Instead of telling patients they need to change to accommodate my treatment plan, I learned to accommodate my treatment plan to fit their life situation. Patients, especially the more mature, complex-care patients, have complex fit issues. These include finances, family hassles, work schedules, special current events, travel, stressors, health factors, significant emotional issues; in short, any issues dominating the patient’s energy and attention. When you present complex-care dentistry, it has to fit into the patient’s life.
Think about it. If you offer most patients a US$10,000 treatment plan, something in their life has to happen. People need to wait to receive their tax refund, wait for a child to graduate from college, become more settled in their new job, or take a much-needed vacation. Knowing the manner in which your complex-care treatment plans fit into the current or foreseeable circumstances of your patient’s life is a mandatory skill for practising complex-care dentistry. Without fit, there is no case acceptance, regardless of the level of dental IQ or your zeal for patient education.
Discovering fit issues
Your team often knows what is going on in the patient’s life. How do they know? They talk―they chit-chat with the patients and they make friends. Another purpose of chit-chat is to learn about those fit issues in your patient’s life impacting their treatment decision. When chit-chat is intentional, I call it fit-chat―an indirect way of discovering patient fit issues.
When you fit-chat, be curious and listen more than talk. Listen to the manner in which patients spend their time and what’s creating stress in their life―health, money and/or family issues. If they mention something you believe may influence a treatment decision, be curious, listen attentively and encourage them to talk more about it. Through indirect fit-chat, you’re going to discover what’s going on in patients’ lives.
Some patients do not fit-chat well. They are simply not talkers. I am that way. When I get my hair cut, the last thing I want is a chatty experience. When you have a complex-care patient who will not fit-chat, you can try a more direct approach to discovering fit issues.
Here is an example of a direct approach: “Kevin, I know from the line of work you are in that you are busy and travel quite a bit. I also know you are aggravated by food trapping around your lower partial denture. Let’s talk about your choices and how we can best fit your dentistry into what is going on in your life. Is now a good time to talk about this?”
Here is another example of a direct approach: “Kevin, most people like you are busy, on-the-go and have lots of irons in the fire. I need to know if any of these irons are affecting the amount of stress you are under, the amount of time you can spend here with us, or if there are financial issues I need to consider when planning your care. I want to reassure you that I am very good at helping patients fit their dentistry into what is going on in their life.”
Whether you are using an indirect fit-chat or a direct approach to discovering fit issues, an absolute prerequisite to a comfortable conversation is for you to have a connected communication style. This means you hold good eye contact, listen carefully and patiently; you maintain a conversational tone of voice and your speaking rate is relaxed. Be sure to pause long enough to let what you are saying sink in.
If you attempt to use a direct approach to fit issues but have a disconnected style (do not look the patient in the eye, speak too quickly, do not listen attentively), your conversation may be perceived as being inappropriate, unprofessional and seeking to diagnose their pocketbook sneakily.
Advocacy
Advocacy is the experience of patients when they realise that you are guiding them towards and not selling them into dental health. To be an advocate is to be a guide. To guide patients into complex care effectively you need to take the fit circumstances of their life into account and help them find a way to fix their teeth in light of those circumstances. This may mean fixing their teeth now, later, or over time.
Here is something you say that propels the advocacy experience. It occurs after the examination, but before any detailed conversation about clinical findings. Here is where you link the fit issues you discovered to your clinical findings.
“Kevin, now that I have looked at your teeth, I know I can help you. We treat many patients like you with partial dentures that do not work well. I know I can help. What I do not know is whether this is the right time for you. You mentioned you travel a lot and your company is in the middle of a big reorganisation. Do you go ahead with your treatment now? Do we wait until later? Or do we do it over time? Help me understand how I can best fit your treatment into everything that is going on in your life.”
This advocacy statement leads to a conversation about the patient’s fit issues. This conversation reveals what treatment fits and what does not. You will find that this approach results in many complex-care patients doing their treatment over time, allowing them to stay within the limitations of their fit issues. This is a good thing. I would rather treat two patients for US$5,000 each than no patients for US$10,000. It also yields lifetime patients for you. Patients will exhibit fierce loyalty to you when they experience advocacy.
The decision to educate
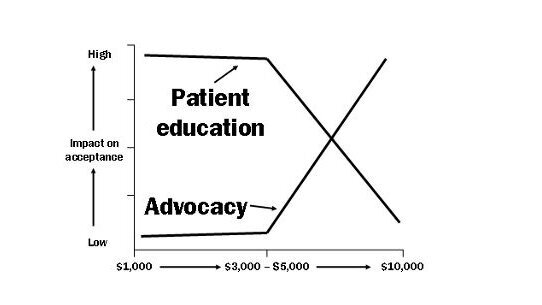
The decision when to educate and when to advocate is situational. Figure 3 demonstrates that the impact of patient education on case acceptance is highest when the complexity of the care (and its associated fee) is minimal. Patient education is the driver of case acceptance when a patient’s conditions and fees are minimal. However, when the complexity of care increases, the role of advocacy takes over. Advocacy is the driver of case acceptance when the patient’s conditions are complex and fees are high. Copy Figure 3 and keep it in area where you will see if often. Then, right before you go into case presentation, look at it and ask yourself: does this patient need education or advocacy? Let the situation guide you. When you do, you will discover how to keep from educating your patients out the door.
About the author
Dr Paul Homoly is a world-class leader in dental education. As a comprehensive, restorative dentist and acclaimed educator for over 25 years, he is known for his innovative and practical approach to dentistry. Dr Homoly is now offering YES! On-Line as the solution for dentists and their teams to excel at case acceptance. This on-line, seven-module curriculum, which is supported by a matching set of DVDs, takes your dental team step-by-step through the essential dental team-patient conversations, and has proven successful for over 30 years.
Distinguished by his focus on outcomes, Dr Homoly is legendary for his ability to teach and lead in a practical and engaging manner. For more information, visit www.paulhomoly.com or call Homoly Communications at +1 800 294 9370.
Everyone wants 2009 to be a better year than 2008. Well, here’s how: improve your system for presenting treatment to patients — especially ...
You might think that in fi nancially challenging times the last thing you need is a new member of staff. For a practice to thrive and prosper in a difficult...
HELSINKI, Finland: Aligners offer a straightforward and efficient orthodontic treatment option that can be used to achieve aesthetic and functional ...
Advances in technology in dentistry have rapidly improved diagnostics, streamlined treatments and made the dental chair a safer, more comfortable place. ...
HAIPHONG, Vietnam: A new case report has demonstrated what a conservative prosthetic pathway can achieve when a patient with a relatively complex anterior ...
FARMINGTON, Conn., US: Many factors may influence therapeutic decisions in orthodontics. For example, orthodontists may sometimes inaccurately interpret ...
The number of universal adhesives being offered by the dental industry nowadays can make it difficult to decide whether it may be worth switching to another...
Bias is an intrinsic aspect of human cognition, and healthcare professionals—including those in dentistry—are not immune to its influence. Understanding...
NEW YORK, US: The Oral Health Workforce Research Center (OHWRC) is responsible for providing research on the oral health workforce in the US and assisting ...
Orthodontic treatment remains the gold standard intervention to improve alignment and functional dynamics without significant biological sacrifice or ...
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 pm EST (New York)
Live webinar
Thu. 11 June 2026
1:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



































To post a reply please login or register