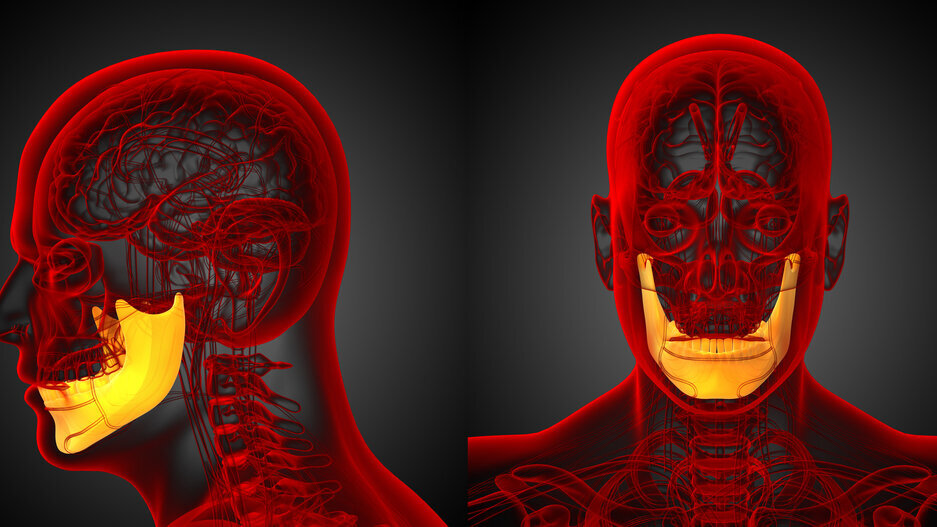
HOUSTON, U.S.: Patients who suffer loss of mandibular bone because of cancer, infection, trauma or congenital disease are left with bony defects that are both esthetically and functionally challenging. Researchers from Rice University have developed a technique to generate engineered tissue customized to the specific defect: implanting a 3-D printed bioreactor against a rib. The stem cells and blood vessels from the rib grow a natural bone material that is tailored to the patient and can be transplanted to the mandible.
The goal of the research was to advance craniofacial reconstruction by taking advantage of the body’s natural healing powers. The technique has been developed to replace current reconstruction techniques that use autogenous bone graft tissue harvested from different areas, such as the lower leg, hip and shoulder.
“A major innovation of this work is leveraging a 3-D printed bioreactor to form bone grown in another part of the body while we prime the defect to accept the newly generated tissue,” said co-author Dr. Antonios Mikos, Louis Calder Professor of Bioengineering and Chemical and Biomolecular Engineering at the university.
The researchers made a rectangular defect in the mandibles of sheep. They created a template for 3-D printing and printed an implantable mold and a spacer, both made of PMMA, also known as bone cement. The goal of the spacer was to promote healing and prevent scar tissue from filling the defect site.
They removed enough bone from the animal model’s rib to expose the periosteum, which served as a source of stem cells and vasculature to seed scaffold material inside the mold. Test groups included crushed rib bone and synthetic calcium phosphate materials to make the biocompatible scaffold.
The mold, with the rib side open to create a tight interface, stayed in place for nine weeks before removal and transfer to the site of the defect, replacing the spacer. In the animal models, the new bone knitted to the old and soft tissue grew around and covered the site.
“We chose to use ribs because they’re easily accessed and a rich source of stem cells and vessels, which infiltrate the scaffold and grow into new bone tissue that matches the patient,” Mikos stated. “There’s no need for exogenous growth factors or cells that would complicate the regulatory approval process and translation to clinical applications.”
According to Mikos, using PMMA for the mold and spacer was a simple decision, as it has been regulated as a medical device for biological applications for decades. In World War II, when PMMA was used as a windshield for fighter planes, doctors noticed that shards embedded in injured pilots did not cause inflammation and thus considered it benign.
“We’re delighted to bring together this diversely talented team and deliver promising outcomes to the future healing of the wounded warrior and other patients in need of advanced treatments for the jaw and face,” Mikos said.
The study, titled “Biomaterials-aided mandibular reconstruction using in vivo bioreactors,” was published online in Proceedings of the National Academy of Sciences of the United States of America on March 18, 2019, ahead of inclusion in an issue.
Tags:
LEIPZIG, Germany: Robotic computer-assisted technologies are beginning to reshape dental implant surgery, although their use remains limited. A recent ...
The use of 3D imaging has become the standard of care for diagnosis and treatment planning for many medical and dental procedures. Such imaging was first ...
Conducted in collaboration with the Medical University of Graz in Austria, a new independent study followed patients treated with the two-piece Patent ...
Just like every inventor needs a laboratory, Curaden needs the Holford Partners Curaden Dental Clinic. Located in the heart of London, the clinic serves as ...
The aim was to evaluate the three-year outcome of nonsubmerged dental implants with buccal periimplant defects treated with a guided bone regeneration ...
Orthognathic surgery has been performed routinely since the mid- 1970s to correct severe skeletal malocclusion. Since its inception, various forms of ...
DUBAI, UAE: Augmentation of an insufficient bone volume is indicated before or in conjunction with implant placement to gain long-term functioning and an ...
HANNOVER, Germany: Researchers in Germany are developing customised dental implants designed to match each patient’s individual jaw structure. The ...
Modern endodontics is no longer an isolated discipline. It marks the start of a restorative process that extends all the way to the final composite layer. ...
VÄSTERÅS, Sweden: According to a report to the Swedish health care authorities, a 3 cm-long dental drill bit had to be removed from a female patient’s ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



































To post a reply please login or register