The efficacy of dental implant treatment is well-documented and its further development includes protocols for simplifying the procedures. The immediate function protocol is a powerful simplification as it allows the complete rehabilitation to be finalized within the same procedure.1–29 The fact that four implants is an optimal number for complete-arch prosthesis is an important further simplification. Provided the implants are placed as 'cornerstones'—two posteriorly and two anteriorly30,31—and they are well-anchored, the probability for success is high.32,33 It has also been demonstrated that tilting of implants might be advantageous as longer implants may be placed with good cortical anchorage in optimal positions for prosthetic support and reducing the length of the cantilever.34–36
Based on these principles the All-on-4 concept was developed for safe and simple treatment of totally edentulous mandibles and maxillas and has been shown to be a viable option. The advantage of the All-on-4 for the edentulous mandible is it avoids the use of bone graft or nerve transposition techniques even in severely resorbed situations. In the edentulous maxilla, where insufficient residual bone volume often makes implant placement posterior to the canine/first premolar impossible, the All-on-4 concept offers solutions in situations where otherwise bone grafting would have been indicated.
This paper aims to explain the indications for the All-on-4 system treatment, which maneuvers around the anatomical limits and risks and allows in a small amount of time to accurately perform implant treatments for fully edentulous jaws
Materials and methods
The All-on-4 concept is based on the optimal number of four implants for supporting an edentulous jaw with a complete arch prosthesis. The concept benefits from posterior tilting of the two distal implants, which offers a minimum of 10 teeth in the immediately placed prosthesis with a maximum of a one-tooth distal cantilever. The procedures are described elsewhere32,33 and here we offer a summary of the protocol.
• Inclusion/exclusion criteria
The patients undergo medical history, clinical observation and complementary radiographic exams of panoramic X-ray (bone height) and a CT-scan (bone quality and bone volume). For the mandible, the anatomical inclusion criterion is a bone ridge of a minimum 4 mm width and maximum 8 mm height in the inter-foramina area.
For the edentulous maxilla, the height and width of the residual crest bone available between the anterior walls of the maxillary sinus for the maxilla and between the mental foramina for the mandible will establish the type of All-on-4 surgical approach: All-on-4 Standard, All-on-4 Hybrid or All-on-4 Extra-Maxilla.
For the All-on-4 Standard, the anatomical inclusion criterion is a bone ridge of a minimum 4 mm width and maximum 10 mm height from canine to canine. The All-on-4 concept can be used at different degrees of maxillary atrophy as the position of the posterior implant is the determining factor for the inter-implant distance.
Depending on the degree of resorption, the posterior implant head will emerge at different positions at the bone crest, normally between the first premolar [high resorption (Fig. 1)] and the first molar [moderate resorption (Fig. 2)]. If the above criteria are not met, then an All-on-4 Hybrid or All-on-4 Extra-Maxilla should be considered. In the All-on-4 Hybrid rehabilitation, maxillary anchored implants are used in conjunction with extra-maxillary anchorage implants (anchored in the zygomatic bone) (Fig. 3), whereas in All-on-4 Extra-Maxilla, only four extra-maxillary anchorage implants are used (Fig. 4).
Surgical protocol
• Medication
The surgical procedures for both jaws were performed under local anesthesia with mepivacaine chlorhydrate with epinephrine 1:100,000 (Scandinibsa 2 per cent, Inibsa Laboratory). All patients were sedated with diazepam (Valium 10 mg, Roche) prior to surgery. Antibiotics (amoxicillin 875 mg and clavulanic acid 125 mg, Labesfal) were given one hour prior to surgery and daily for six days thereafter.
Cortisone medication (prednisone [Meticorten Schering-Plough Farma], 5 mg,) was given daily in a regression mode (15 mg to 5 mg) from the day of surgery until four days postoperatively. Antiinflammatory medication (ibuprofen, 600 mg, Ratiopharm) was administered for four days postoperatively starting on day four. Analgesics (clonixine [Clonix, Janssen-Cilag Farmaceutica], 300 mg,) were given on the day of surgery and postoperatively for the first three days if needed. Antacid medication (omeprazole, 20 mg) was given on the day of surgery and daily for six days postoperatively.
• Flap procedure
The implants and abutments are placed in one position at a time, starting with the two posterior locations. The implant placement is assisted by a special guide, designed by the author (P.M.) (Fig. 5). The guide is placed into a 2 mm hole made at the midline of the jaw and the titanium band is bent so the occulsal centerline of the opposing jaw was followed. By this, it is possible to guide the implants to be placed in the center of the opposing prosthesis and at the same time to find the optimal position and inclination for best implant anchorage and prosthetic support.
The insertion of the implants (Brånemark System; Nobel Speedy, Nobel Biocare) follows standard procedures, except that under-preparation is used when needed to get a final torque of more than 40 Ncm before the final seating of the implant. Countersinking is used only when needed to create space for the head of the tilted implants and/or to secure both buccal and lingual cortical bone contact at the implant head in thin bone crests. The preparation is typically done by full drill depth with a 2 mm or a 2.5 mm twist drill (depending on bone density), followed by a widening of the entrance in the cortical bone with a 3 mm twist drill and an adjustment with the countersink, if needed.
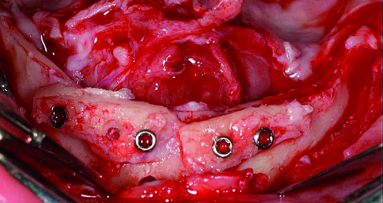
The implant neck is positioned at bone level, and bicortical anchorage is established whenever possible (Fig.6). The length of the implants varies from 10 mm to 18 mm. In case of immediate extraction, the sockets are made free from soft tissue remnants and cleaned to avoid infection. In case of periodontitis on the lower incisors, extraction, curettage and bone shaping is performed and virtually no socket is left. After closing and suturing the flap with 4–0 non-resorbable suture, the access to the abutments is opened by a punch and impression copings are placed.
Implant placement in the mandible: In the mandible, a mucoperiosteal flap is raised along the top of the ridge in the intermentonian area. The two most anterior implants follow the jaw anatomy in direction, which in severe resorption cases means a posterior tilting. Two additional implants are inserted just anterior to the foramina and tilted distally about 30 degrees relative to the occlusal plane. This arrangement allows for good implant anchorage, short cantilever length and large inter-implant distance. The posterior implants typically emerge at the second premolar position.
The posterior implants are of 4 mm diameter, while the anterior ones are either 4 or 3.75 mm in diameter. Angulated abutments (Brånemark System, Nobel Biocare) are used. The angle is either 17 degrees or 30 degrees at the anterior implants and always 30 degrees at the posterior implants (Fig. 7). These abutment angulations were chosen such that the prosthetic set screw access holes were in an occlusal or lingual location.
Implant placement in the maxilla: In the maxilla, the posterior implant tilting allows a position shift on the implant head from a vertically placed implant in the canine/first pre-molar region to a tilted implant in the second pre-molar/first molar region, following the anterior sinus wall with about 45 degrees of inclination.
Thirty-degree angulated abutments are placed on the implant correcting the inclination to a maximum of 15 degrees. The posterior implants are 4 mm in diameter
The anterior implants are oriented vertically by a guide pin replacing the special surgical guide (Fig. 8). Care has to be taken in the selection of the anterior positions not to come in conflict with the apex of the tilted posterior implants, which normally reach the canine area. The anterior implants are either 4 or 3.75 mm in diameter and typically placed in lateral or central incisor positions. This implant arrangement allows for good implant anchorage, a large inter-implant distance and short cantilever length with the posterior implants typically emerging at the second premolar/first molar position.
• Immediate prosthetic protocol
Provisional complete-arch all-acrylic prostheses are delivered on the day of surgery. A pre-made impression tray is used. Small volumes of silicon are placed around the copings, followed by complete filling with soft putty. After removal of the copings, protection caps are placed to support the periimplant mucosa during the manufacturing of the prosthesis. Based on the impression, a high-density baked all-acrylic prosthesis with titanium cylinders is manufactured at the laboratory and most often delivered to the patient within two to three hours (Fig. 9). The provisional prosthesis should not have more that one cantilever tooth and consequently the number of immediate teeth varies from ten and up, depending on the degree of resorption. (The final prosthesis may have two cantilever teeth, though.)
• Flapless procedure
The positions of the implants are the same as for the flap procedure, but the planning is made in a computer on a 3-D model of the patient’s jaw. At surgery the implants are oriented by a precision guide (NobelGuide, Nobel Biocare) based on the planning data,27 and a pre-surgery manufactured prosthesis is immediately delivered after surgery (Figs. 10 & 11).
• All-on-4 Hybrid/ All-on-4 Extra-Maxilla
An alternative solution for oral rehabilitation in the atrophied maxilla is the use of implants placed in the zygomatic bone, alone or in conjunction with regular implants.37–39 However, the placement of zygomatic anchored implants through the standard technique often causes the implant heads to emerge too palatal for an optimal prosthetic solution (especially in cases of extreme atrophy), as the bone ridge retracts palatally when it atrophies.40
The extra-maxillary anchorage technique aims to eliminate these difficulties by placing long implants external to the sinus, anchored in only the zygomatic bone and covered by soft tissue after emerging from the bone.
By doing so, the implant head will be positioned in a prosthetically correct position. The implants emerge in the positions between the lateral incisor and the first molar, on the crest at the ideal prosthetic position, while the foreseen prosthetic screw exits localize on the occlusal surfaces of the prosthetic teeth or on the internal wall of the bridge through the false gingiva.
As in the standard All-on-4 technique, complete-arch all-acrylic prostheses are delivered on the day of surgery.
Two clinical situations representing two patients eligible for a complete edentulous maxillary rehabilitation through the All-on-4 Hybrid and All-on-4 Extra-Maxilla solution are presented (Figs. 12–15). The extra-maxilla technique complements the All-on-4 concept by replacing one to four standard implants with an extra long implant placed in the zygomatic bone only, making it fit to rehabilitate any degree of maxillary bone atrophy.
• Maintenance protocol
The patients are instructed to have a soft food diet for two months. Ten days after surgery, the sutures are removed (if used), and hygiene and implant stability are checked. The procedure is repeated two and four months after surgery is performed until stability is achieved.
• Final prosthetic protocol
Final prostheses are delivered at six months (Fig. 16). If an adjustment of the angulated abutment was needed for better positioning of the screw access hole, the impression for the final prosthesis is taken at implant level. The abutment position is then decided at the laboratory and is adjusted in the patient’s mouth.
• Implant survival criteria
Survival was based on function, individual implant stability (checked manually), absence of pain and infection, and radiographic analysis at time of evaluation.
• Marginal bone level
The marginal bone level relative to the implant platform was read from periapical radiographs taken at the time of last follow-up within the study frame and at the additional follow-up for the present study. A conventional radiograph holder was used, and its position was manually adjusted for an estimated orthognathic position of the film. For a few patients, panoramic radiographs were used due to access problems.
Results
• Implant survival
The implant survival rates are presented in life tables. Tables I and II show the results for the All-on-4 standard, for the rehabilitation in the mandible and maxilla, respectively. The data concerns the routine groups as presented in the previous clinical studies32,33 plus the result from the subsequent follow-up until today.
These results show the incidence of implant losses for both the maxilla and mandible rehabilitations are low and decrease dramatically after the first six months of function, rendering high survival rates.
The preliminary results for the cumulative survival rate of the extra-maxillary anchorage implants are shown in Table III. The results indicate high survival rates with a follow-up of up to two years for the All-on-4 Hybrid and All-on-4 Extra-Maxilla implants.
• Marginal bone level
The average bone levels relative to the implant platforms at one year of follow-up were 0.9 mm (SD 1.0 mm) for the maxilla and 0.7 mm (SD 0.5 mm) for the mandible. The average bone levels for the mandible at five years of follow-up were 1.7 mm (SD 1 mm).
Discussion
These results and the outcome from the present study indicate that immediate function for the maxilla and mandible can be highly predictable treatments (high survival rates and low marginal bone resorption), provided an optimal placement of the implants. The All-on-4 concept with implant tilting utilizes the load carrying capacity of the bone in an optimal way; the implants are spread anteriorly-posteriorly, giving an optimal prosthetic base and are well anchored in dense bone structures (anterior bone with higher density) due to the freedom of tilting.
By reducing the number of implants to four, each implant can be optimally placed without any compromise to adjacent implants. The data supports that this biomechanical optimization of the implant positions is clinically effective. The fact that the prostheses survival could be kept at 100 per cent, even with less than four implants supporting the prosthesis, also demonstrates the efficacy of the implant positions.
Moreover, using finite element analysis, it is possible to conclude that there is a biomechanical advantage in using splinted, tilted distal implants rather than axial implants supporting distal cantilever units when comparing the coronal stress.41
The use of only four implants simplifies many aspects of the treatment: a more aesthetic prosthesis can be manufactured, it simplifies the manufacture of the prosthesis, it reduces the risk for prosthetic complications, and it simplifies the patient’s dental hygiene procedure.
Conclusions
In conclusion, the All-on-4 immediate function concept for completely edentulous jaws has proven to be clinically effective, patient pleasing and applicable in many situations where otherwise more complicated procedures would have been indicated.
It is a standardized treatment procedure than can be routinely applied to most edentulous patients with a short treatment procedure and prostheses in place and functional a few hours after the start of surgery.
It’s well adapted to further simplifications such as flapless surgery based on computer planning and can be recommended as a method of choice for rehabilitation of completely edentulous jaws.
This article was originally published in Implant Tribune Vol. 3, Issue 11, 2008.
Dr Malo can be contacted in care of Miguel Nobre at mnobre@maloclinics.com.
Autogenous bone block grafts, bone grafting material or a combination of both can be used to restore an implant site of adequate dimensions in an atrophied ...
Historically, when a patient’s dental condition reached a state of total tooth loss, treatment was limited to a complete denture with no hope of ...
Because the long-term success of implant treatment depends on various factors, including oral hygiene, lifestyle habits and health conditions, it is vital ...
An 82-year-old patient presented for complete rehabilitation. The existing maxillary bridge showed Grade III mobility and the residual mandibular teeth ...
Implant planning and placement in the completely edentulous maxilla can present challenges both surgically and prosthetically whether a removable or fixed ...
Rehabilitation of the edentulous jaw can be achieved with various treatment modalities. Removable implant-supported overdentures can provide a comfortable, ...
In recent years, manufacturers have developed increasingly advanced composite materials, offering improvements in aesthetics, handling and mechanical ...
An adequate bone volume at the future implant site is a prerequisite for ideal implant placement and implant success. A residual bone with a vertical ...
Objective: All-on-4 treatment concept is widely applied for complete-arch rehabilitations. Nevertheless, minor technical and biological complications can ...
BOSTON, US: Around 120 participants from 27 countries gathered in Boston from 16 to 18 June for a landmark moment in implant dentistry, the first ...
Live webinar
Wed. 8 April 2026
1:00 pm EST (New York)
Live webinar
Thu. 9 April 2026
1:00 pm EST (New York)
Live webinar
Thu. 9 April 2026
2:00 pm EST (New York)
Prof. Moritz Kebschull, Cat Edney
Live webinar
Fri. 10 April 2026
10:00 am EST (New York)
Live webinar
Fri. 10 April 2026
11:00 am EST (New York)
Dr. med. dent. Henrik-Christian Carl Hollay
Live webinar
Fri. 10 April 2026
12:00 pm EST (New York)
Prof. Dr. Ali Murat Kökat
Live webinar
Fri. 10 April 2026
12:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





























To post a reply please login or register