Historically, when a patient’s dental condition reached a state of total tooth loss, treatment was limited to a complete denture with no hope of improving that status. The greatest challenge, particularly when working with a lower jaw, was providing a denture with reasonable stability and retention.[1] Success was greatly dependent upon the skill of the practitioner but also on the neuromuscular ability of the patient, their supporting structures and a philosophical attitude toward their condition.[2] Treatment for patients suffering complete edentulism has been revolutionised by the ongoing success of dental implants so that the standard of care for the mandible is an implant overdenture.
The spectrum of prosthetic modalities developed since the acceptance of endosseous implants to the dental market ranges from the very simple to the astoundingly complex. Once directed by specialists, this field of study has evolved into a mainstay of the general practice, and so favour of expeditious and reproducible methods has gained dominance over complex therapies. Implant overdentures and fixed hybrid prostheses are choices typically offered by the dentist based on a patient’s financial ability. While both are generally successful, the overdenture and the hybrid prosthesis are not without pitfalls.
The implant-retained overdenture
The implant-retained overdenture is described as a prosthesis that covers, and is supported by, the natural tissues retained by the dental implant; the design is considered implant-assisted rather than supported.[3] Placement of two to five implants is commonly found for the edentulous mandible with emphasis on creating a large anteroposterior (AP) spread between the endosseous pillars. If more than two implants are clustered in a small AP range, the prosthesis cannot move freely about a single axis of rotation and the denture may dislodge during function.
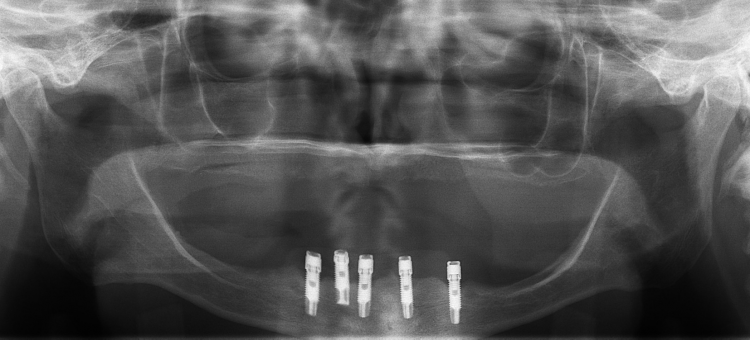
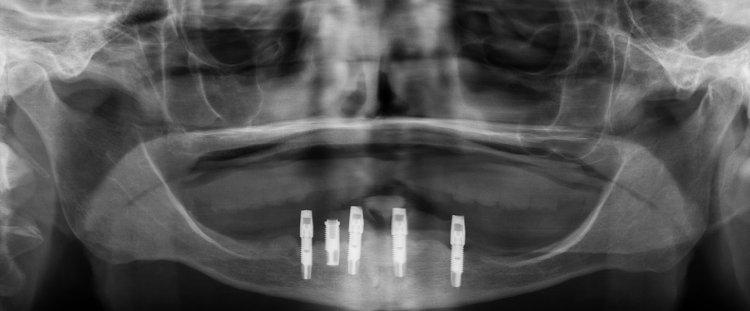
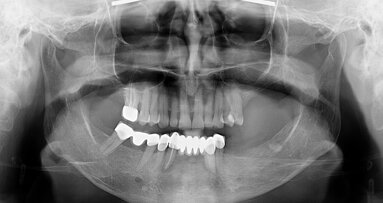
Fig. 1: Pre-treatment radiograph showing five implants clustered in the anterior mandible.
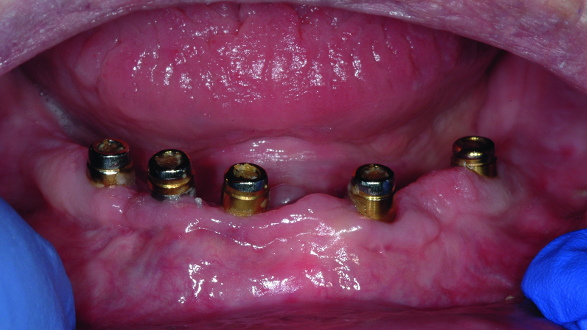
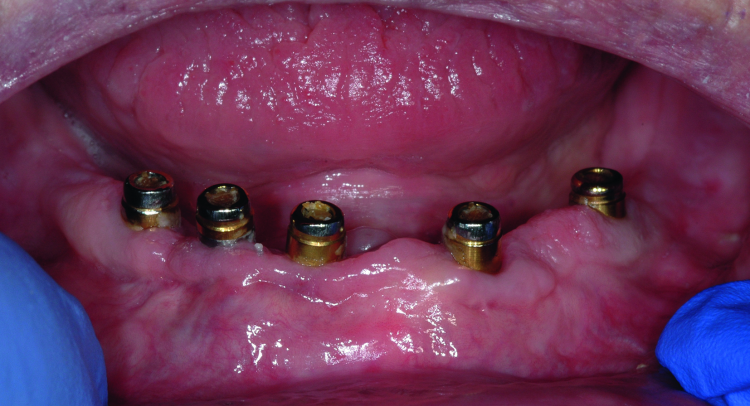
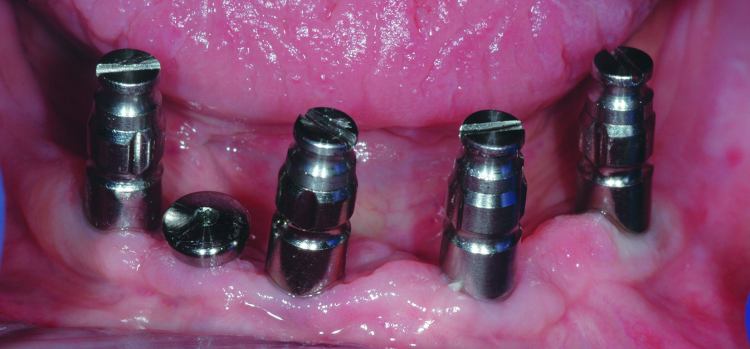
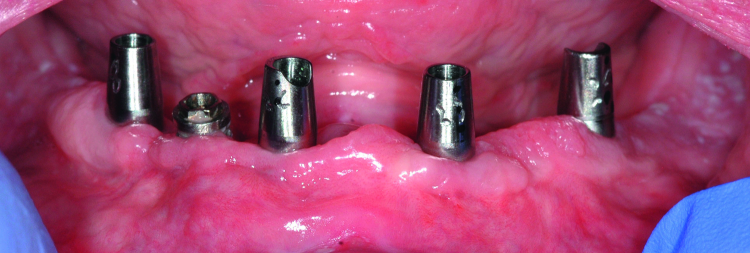
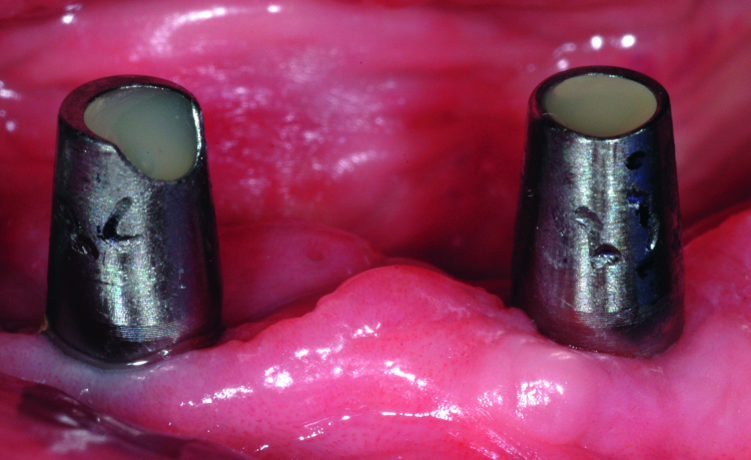
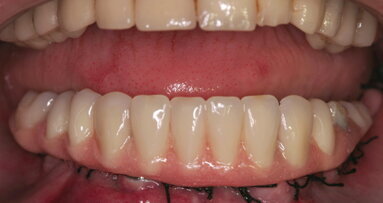
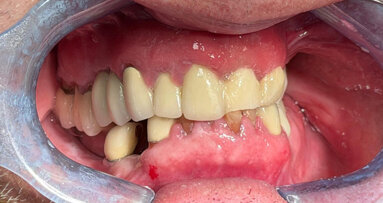
Fig. 2: Clinical image of patient. Note the wear of the metal abutments due to disengagement of the nylon retention inserts as a result of fulcrum during function.
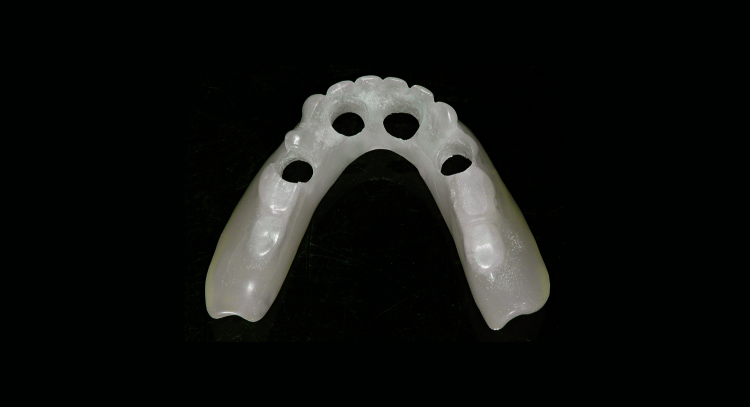
Fig. 3: Duplication of an acceptable denture serves as a custom tray. Holes of sufficient diameter to accommodate impression copings have been prepared.
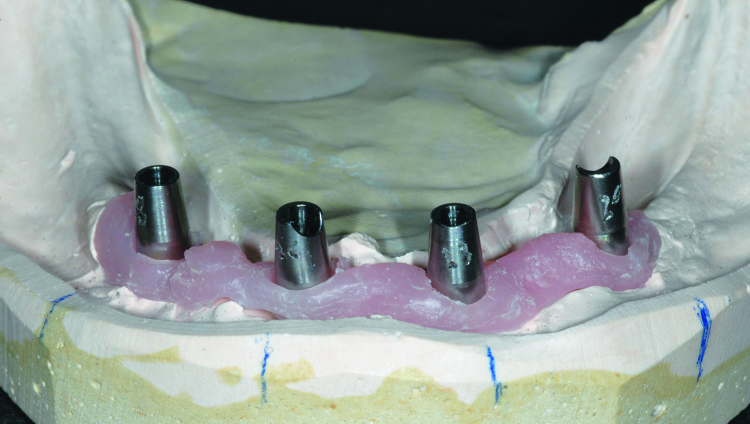
Fig. 4: Open tray impression copings seated on the dental implants. One implant is selected for disuse and covered with a transmucosal abutment.
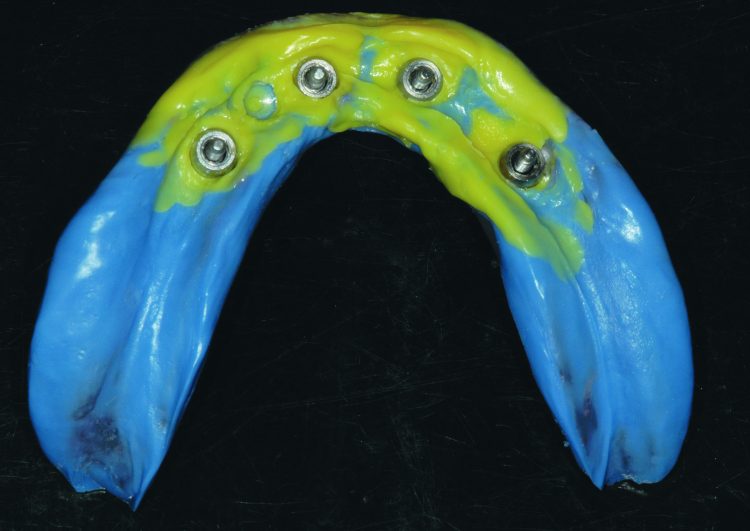
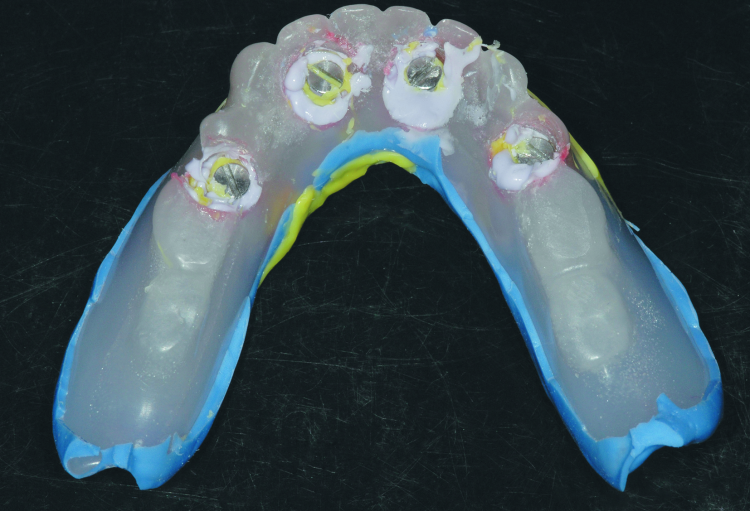
Fig. 5: Completed final impression using the custom tray and light body and medium body PVS, as well as rigid bite registration material around the impression copings to eliminate any movement of the copings.
Fig. 6: Completed final impression using the custom tray and light body and medium body PVS, as well as rigid bite registration material around the impression copings to eliminate any movement of the copings.
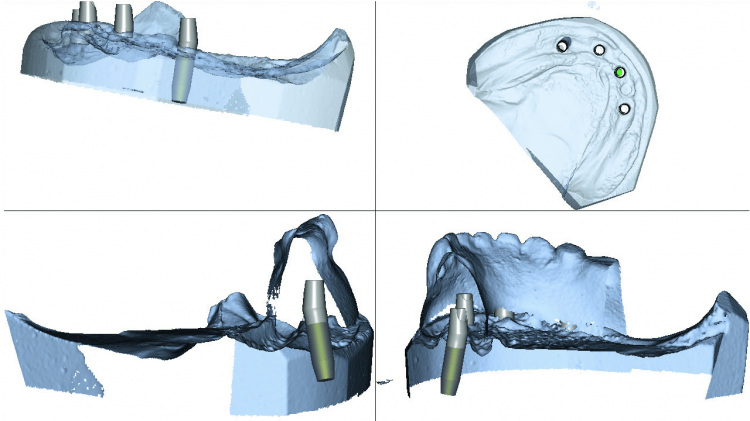
Fig. 7: Design images showing the contour and tooth position of the duplicate denture and proposed design of the Atlantis Conus Abutments.
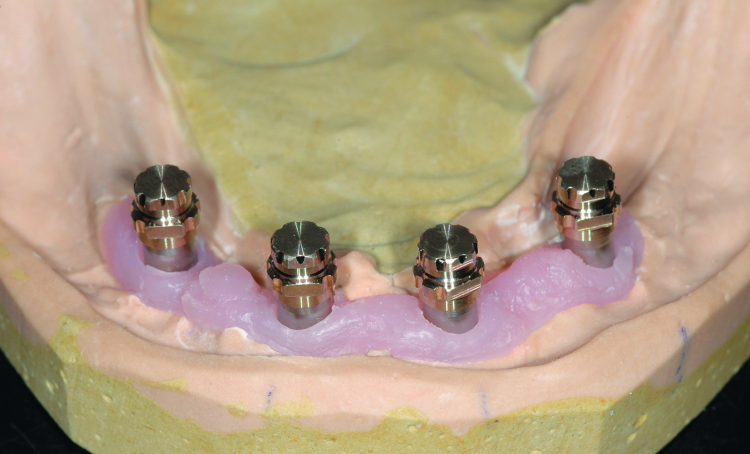
Fig. 8: Atlantis Conus Abutments on the working cast. Each abutment has the tooth number location scribed on the buccal-facing surface.
Fig. 9: SynCone caps seated on the abutments on the working cast. An impression of this arrangement is made to fabricate a cast metal frame to reinforce the final restoration.
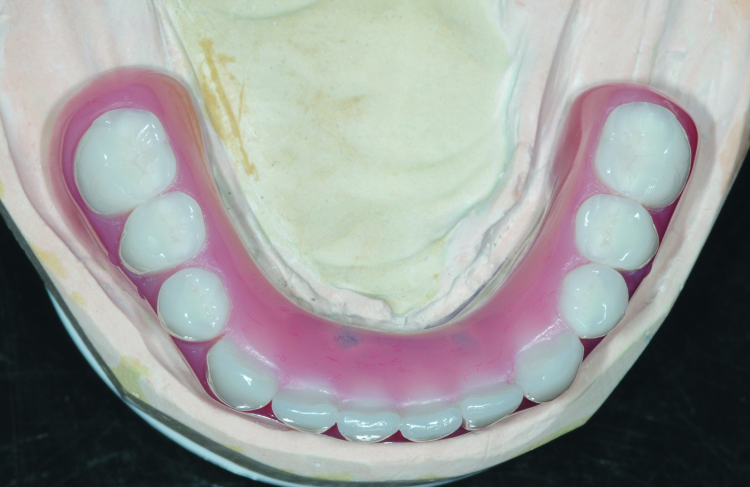
Fig. 10: Completed laboratory restoration; note the termination the arch at the first molar to avoid excessive cantilever length. The chrome frame is opaqued on the functional side to prevent gray show-through.
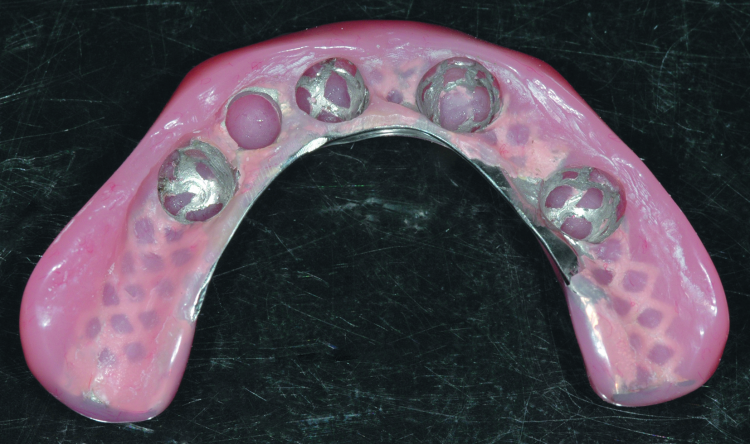
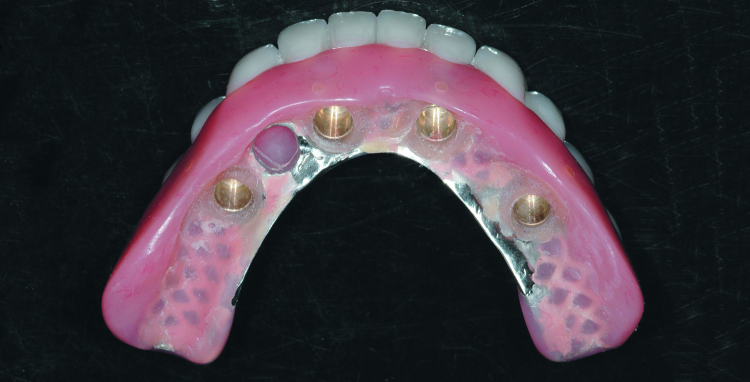
Fig. 11: Completed laboratory restoration showing the metal frame and recessed area to receive the SynCone caps.
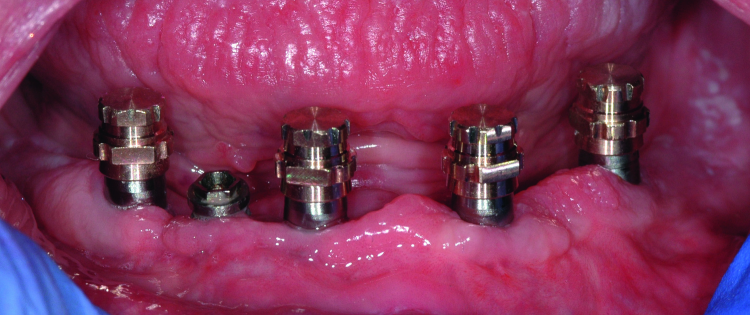
Fig. 12: Atlantis Conus Abutments seated. Note the “margins” of the abutment, and the point where the parallel preparation begins, is supra-gingivally positioned.
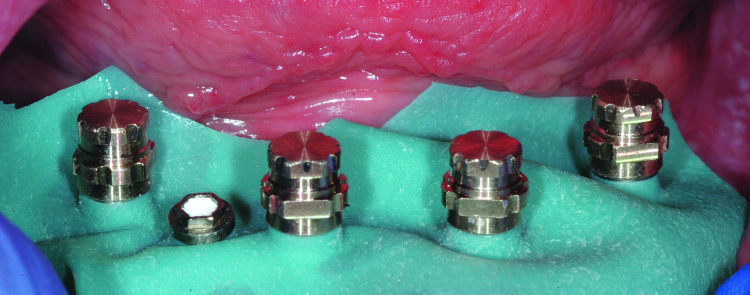
Fig. 13: SynCone caps are fitted to the abutments to verify unobstructed and complete seating.
Fig. 14: Rubber dam is placed over the abutments to prevent pick-up material from locking into undercut areas below the prepared margin. SynCone caps are seated and ready to be captured into the prosthesis.
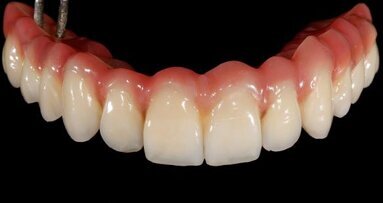
Fig. 15: Completed bridge with SynCone caps processed in position. Because they have been processed intraorally, there is no error in fit, these caps are extremely retentive allowing only vertical displacement of the prosthesis.
Fig. 16: Completed restoration. Note the absence of screw access holes for a prosthesis that looks like a denture yet fits like a bridge.
Fig. 17: Atlantis Conus Abutments torqued to specified level, obturated with Teflon tape and composite resin.
Fig. 19: Panoramic radiograph of the abutments seated on the four selected implants. Because the restoration is fully implant-supported, gradual diminution of the residual ridge will present no consequence to the patient.
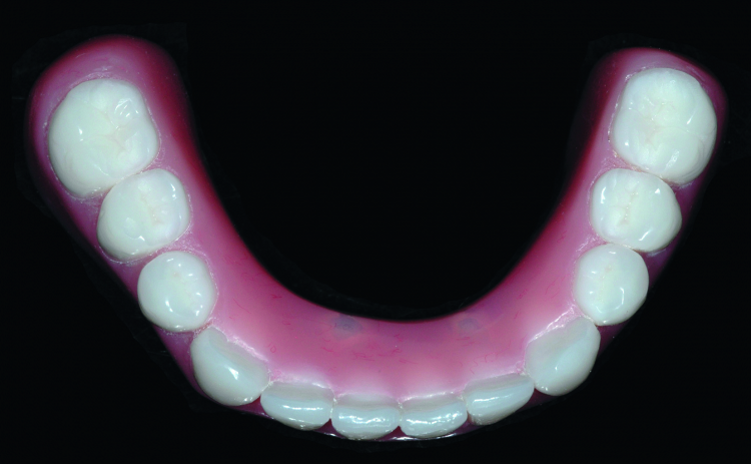
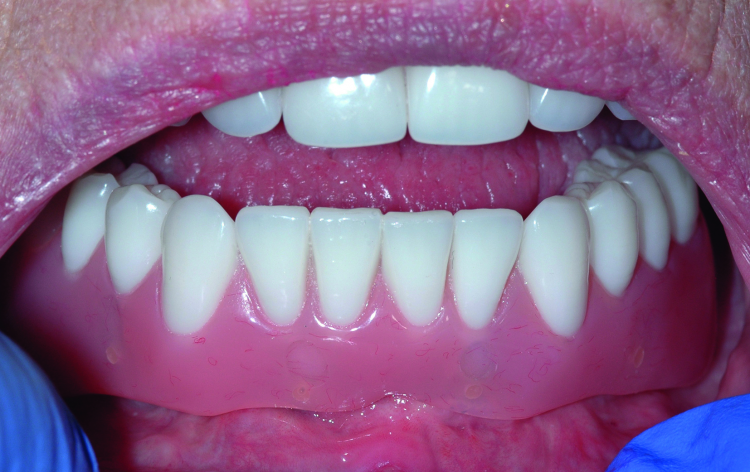
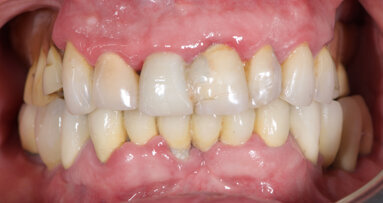
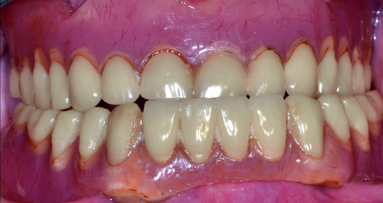
Fig. 20: Completed bridge in place showing flange length suitable to prevent food entrapment and support the lip and cheeks. Because the restoration remains removable, these flanges do not prevent excellent home care.
Fig. 18: Laboratory processed, clear duplicate prosthesis with siliconised reline material to improve retention; to be used as a night-time appliance to protect the tongue from the sharper edges of the abutments.
By creating the fulcrum on the most posterior overdenture abutments, the denture will pivot in function resulting in disengagement from the attachment mechanism and cause premature wear of the retentive components. Therefore, an increase in the number of implants beyond two does not necessarily provide a linear increase in retention and stability. In fact, the opposite may be true. Because support is provided by the mandible itself, resorption of the supporting structure will result in increased tipping of the denture during function, resulting in dislodgement. Therefore, the dentist and patient must be cognisant of the need for relining of the prosthesis periodically to assure optimal performance.[4-7]
The recommendation is, therefore, placement of two implants in the anterior mandible to allow one axis of rotation. These implants should also be positioned so that future implants may be considered should the patient wish for an implant-supported alternative.
The hybrid prosthesis
The screw-retained hybrid prosthesis is a fully implant-supported structure and, therefore, is not affected by incremental resorption of the residual ridges. It has gained popularity as the technically difficult and costly gold frameworks have been replaced by CAD/CAM titanium structures, and by proven success of angled implant placement to increase the AP spread. Because the restoration has a metal substructure, it is possible to cantilever posterior to the terminal abutment, increasing the length of the functional arch.
However, the aesthetic component of the restoration—namely the denture teeth and acrylic resin matrix—are inherently weak materials originally intended for use in complete and partial dentures where functional load is comparatively low. If insufficient interarch space is available, the risk of fracture or displacement of denture teeth or resin base is high as the materials will be too thinned to withstand forces generated during function and especially parafunction.
Unfortunately, this is an increasingly common occurrence, especially in restoration of the maxilla with a fixed hybrid prosthesis. Inconvenient screw-access holes may further weaken the prosthetic teeth. Repair of a fractured or lost tooth requires removal of the hybrid prosthesis and correction in the dental laboratory.
The dentist must be prepared to remove the structure and later re-seat it once the repair is completed. The patient must accept they will be without “teeth” for the length of time required for the technician to fix the problem. Attempts to prevent fracturing by increasing the thickness of the resin is limited by the space available to do so. If inadequate interarch space is encountered, correction cannot be achieved by adding more material. Rather a change in design to a different and possibly more expensive restoration may be needed. When hybrids are used in the maxilla, conflict may arise in attempting to improve the aesthetic and phonetic result by use of ridge lapping and the limitations such shapes impose on proper oral hygiene.
The benefits of the fixed hybrid prosthesis are clearly improved function and minimal post-treatment complications as long as the patient is able to properly clean it and breakage is avoided. Because it is fixed, the patient cannot remove it to clean away entrapped debris and properly remove plaque. Repair or replacement of the resin teeth requires removal and re-seating by a dentist.
Atlantis Conus concept: the removable implant-supported bridge
As described above, the tissue-supported overdenture performs best with only two implants placed in the anterior region. When more than two implants are placed, the goal should be to provide a complete implant- supported result.[4-5] The Atlantis Conus concept (Dentsply Sirona) provides the optimal functioning convenience of a fixed hybrid, but also allows patient retrievability for unobstructed oral hygiene practice, regardless of the degree of ridge lap. It is, in effect, a prosthesis that can be removed by the patient, with the stability of a fixed bridge.
The concept centres around patient-specific abutments, each milled to a 5-degree convergence, and parallel to each other in the dental arch. The recommendation is for at least four implants in the mandible and four to five implants in the maxilla.
These uniquely designed, conical abutments are fitted by corresponding metal SynCone caps (Dentsply Sirona), which are incorporated into the prosthesis. The result is a friction-fit, stable, retentive and fully implant-supported bridge that remains removable by the patient.[6] No special latches or plunger attachments are necessary to retain it. The patient merely slides the bridge in vertically onto the abutments and removes it in the opposite way. Because the abutments are a part of the Atlantis (Dentsply Sirona) portfolio, it is available for all major systems.
In addition, because each abutment is custom-made, correction of angled implant placement is possible up to 30 degrees. Two major requirements are necessary: the dentist must make an accurate, implant-level impression and a scan must be made of either an approved denture set-up or of a completed denture to be retro-fitted. The Atlantis Conus Abutments are then designed to be positioned optimally within the denture confines. The fixed yet removable prosthesis offers the advantages of excellent chewing function, improved aesthetics and fracture resistance (as no screw access holes are present) and optimally facial supporting contours, without compromising cleaning by the patient.
Case report
A 73-year-old woman with a history of 11 years of complete edentulism of the maxilla and mandible, and five endosseous implants in the anterior mandible, presented with a chief complaint of a non-retentive and unstable lower denture. The implants were standard diameter, externally hexed, Brånemark fixtures. She had moderate resorption of both the maxillary and mandibular residual ridges (Fig. 1).
The patient had bone loss involving the implant bodies but comparing the radiographic evidence available, documenting her condition through the years, it appears the bone loss occurred soon after implant placement and no appreciable change was seen thereafter.
During those 11 years, her treatment history included initial restoration of the implants with a complete denture retained by the LOCATOR Attachment System (Zest Dental Solutions); and the maxilla was restored with a complete denture. She advised that the result was unsatisfactory as the lower denture displaced during function.
Her history further reveals that the Locators were replaced with PRECI-CLIX attachments (Ceka Attachments) with no demonstrable improvement. The patient was later re-treated by the author, with new maxillary and mandibular complete dentures and new Locator attachments used to retain the lower prosthesis. The attachment male components were secured intraorally using auto-polymerising resin to eliminate the possibility of laboratory error.
The patient continued to experience problems with the lower denture coming loose during function and required frequent replacement of the nylon male inserts; replacement with Extended Range inserts did not vary performance. The metal abutments demonstrated considerable wear as well (Fig. 2). Relining the lower denture did not improve the performance of the anchor system.
At the subsequent appointment, the patient was presented with the Atlantis Conus concept as a potential solution to her ongoing dilemma. Treatment options were presented as well including a fixed hybrid prosthesis and a 2-in-1 bar overdenture. These were rejected as interarch space was less than optimal, requiring compromise to the strength of the design. The patient also expressed a desire for a removable design as she was concerned with having adequate facial support and wished to be able to remove the prosthesis for proper hygiene and maintenance. It was agreed that a new maxillary and mandibular complete denture would be fabricated, and Atlantis Conus Abutments would be made to secure the lower restoration.
Clinical and laboratory procedures
Because the existing dentures were made within the last five years and were acceptable with regard to tooth position and vertical dimension, it was decided that clear, acrylic resin duplicates of each denture would be made to serve as custom trays.[7] Double-sided impressions of each denture were made and delivered to the dental laboratory for fabrication of the duplicates. Once processed, the copy denture borders were shortened by 2 mm to allow border moulding. The duplicate of the mandibular denture clearly showed the position of each Locator housing and therefore the position of the dental implants. Holes of adequate diameter to allow the duplicate denture to be placed in the patient’s mouth over impression copings were prepared (Fig. 3). The intaglio surface of both the upper and lower duplicate denture were relieved to allow for a wash impression.
The patient returned for final impressions, and the Locator abutments were removed and kept in appropriate order to avoid confusion when reseating them at the appointment completion. Open tray impression copings were connected to each of the four dental implants to be restored and tightened into place; one implant with greater bone loss and placed significantly more shallowly than the rest was omitted (Fig. 4). Light-body polyvinyl siloxane (PVS) was injected around the base of each impression coping and medium-body PVS was placed in the custom tray.
The tray was seated, ensuring that the impression copings were completely accessible through the holes previously prepared. The patient was instructed in facial and tongue movement to achieve proper peripheral border extension. Regisil Rigid (Dentsply Sirona) bite registration material was injected around each impression coping to rigidly adhere them to the impression tray. This step is critical as reliance on flexible impression material may allow transfer error when constructing the working cast.
Once the impression materials were fully set, the screws retaining the impression copings were removed and the final impression and tray were withdrawn from the patient (Figs. 5 & 6). All Locator abutments were reseated and tightened. The final impression of the maxilla was completed with border moulding using modelling plastic and a wash impression with light-body PVS. Upon completion, the patient was dismissed.
In the dental laboratory, implant analogues were secured to the impression posts, gingival moulage was injected around the analogues to an adequate depth to completely cover the coping-analogue interface. The impressions were boxed with wax and poured in vacuum-mixed die stone. After setting, the impression coping screws were removed and the impressions were separated from the hardened casts; standard laboratory procedures were followed in cleaning and trimming the working casts. The base plate and wax rims were made for the continuation of the denture fabrication. The impression materials were removed from the duplicate denture and it was positioned back onto the mandibular cast to be scanned. An online order was completed including identification of the implants involved and the case was shipped to Dentsply Sirona for the design and manufacture of the Atlantis Conus Abutments.
The working cast, implant analogue connections and the denture duplicate were scanned at the Atlantis production site and the abutments were individually designed using Atlantis VAD (Virtual Abutment Design) software to ensure that all abutments were parallel to each other. The restorative margin of each abutment were placed close to the soft tissue height surrounding each implant, but always supragingival to guarantee unobstructed seating of the finished restoration.
Each abutment was milled to a 5-degree taper to match the SynCone caps ensuring an intimate friction-fit. Upon design completion, the images of the abutment designs were made available for review and approval before manufacturing (Fig. 7). Once the design presented was found to be satisfactory, approval for production of the patient-specific abutments was granted. It is important to note that no fees are incurred by the dentist or dental laboratory during this process until a design is agreed upon and authorization to proceed is given. The abutments are custom-designed to fit specifically to the denture set-up or duplicate denture provided; there are no sizes, heights, angles or collars to select from a catalogue and, therefore, no risk of choosing incorrectly.
When received, the Atlantis Conus Abutments were secured to the working cast with abutment screws, along with four prefabricated SynCone caps (Figs. 8 & 9). The caps were seated onto the abutments and sent to the dental laboratory to be impressed. The impression was poured twice, one in improved dental stone and one in refractory material for fabrication of a cast metal frame. While waiting for the frame to be completed, final try-in appointments for the denture set-up were completed, and the patient approved fabrication of the dentures.
The denture set-up with a final bite record were returned to the dental lab, the cast metal frame was seated on the improved dental stone cast and areas around the stone copy of the SynCone caps were blocked out prior to processing. The SynCone caps will be captured intraorally, rather than having them processed in the dental laboratory. All work was completed on the duplicate stone cast rather than the original working cast. The cast metal frame was opaqued to prevent grey show-through. The set-up was transferred to the cast with the metal frame and the dentures were processed (Figs. 10 & 11).
Because the Atlantis Conus concept results in a fully implant-supported prosthesis, the peripheral borders of the finished structure were greatly reduced and the occlusal table was abbreviated at the first molar. The length of functional arch follows the identical AP spread principles used for hybrid prosthetics to avoid excessively long cantilevers.
At this point, the structure is a bridge and not an overdenture. To facilitate seating of the abutments in the patient, a clear matrix was made with the abutments on the original working cast; where they have remained since receipt. Each abutment was identified with one, two, three and four black ink dots respectively, based on their position on the cast. The clear matrix was seated over the abutments and corresponding black dots were drawn on it to line up exactly with those on the abutments. The completed mandibular bridge was double-side impressed by the dental technician and an injection-mould copy of clear acrylic resin was made.
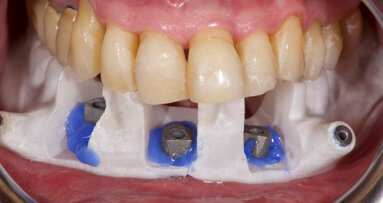
The patient was scheduled for completion of treatment. The Locator abutments were again removed and Teflon tape was placed in the implant excluded from the design. The abutments were seated onto the dental implants (Fig. 12), and the clear matrix was placed to verify that each abutment was correctly orientated by checking that the dots on the matrix superimposed with those on the abutments.
Once verified, the abutments were torqued to 20 Ncm, appropriate for the implants involved. The SynCone caps were placed and viewed with magnification to assure that they were superior to the gingival tissues (Fig. 13). The prosthesis was placed over the caps to verify there was no obstruction of complete seating. The prosthesis was removed and vent holes were drilled through the buccal contours of the acrylic resin to relieve hydraulic pressure during capture of the caps. The SynCone caps were lifted and a rubber dam was placed around the abutments to prevent pick-up resin from locking into undercuts, and the caps were reseated (Fig. 14).
Attachment processing material (Chairside, Zest Dental Solutions) was placed in the reservoirs of the prosthesis and seated over the SynCone caps. The upper denture was placed and the patient was instructed to gently close into full occlusion and to maintain position for two minutes while setting occurred. After two minutes, the excess flow of pick-up resin was checked for hardness and after an additional minute the prosthesis was ready for removal. Removal was uneventful although retention was considerable; removal of the bridge can only occur following the long axis of the abutments, no tipping or rotating is possible (Figs. 15 & 16).
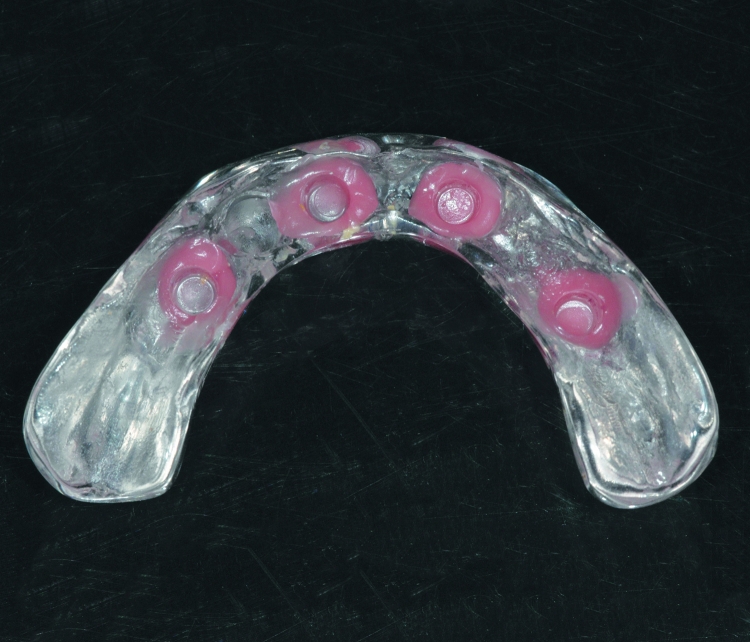
Once removed, the excess pick-up material was removed and the bridge was properly polished where needed. The abutments were packed with Teflon tape to within 3 mm of the surface, and the remaining space was filled with flowable composite resin (Fig. 17). The patient was instructed on placement and removal and repeated the exercise until we were satisfied she would experience no difficulties performing this. The clear, duplicate copy of the bridge was seated onto the abutments using a chairside soft lining material (Fig. 18).
This copy serves as a temporary device for the patient to wear when cleaning the finished bridge or when sleeping to protect the tongue from scraping against the abutments. A panoramic radiograph was taken at completion of treatment (Fig. 19).
The patient returned after one week and again after six weeks, and reported at both visits that the lower bridge did not move at all during function and stayed seated until she removed it. She commented on the ease of cleaning the dental abutments, and she reported no discomfort and no food entrapment. Overall, the patient was very pleased with the result (Fig. 20).
Discussion
The number of implants placed for an edentulous patient should be based upon whether the design is to be implant-assisted or implant-supported. If the goal is a minimalist design utilising the soft tissue for support, two implants using Locator attachments are appropriate to retain a mandibular denture and will provide a predictable outcome. However, when more than two implants using resilient overdenture retainers are employed, there is not a corresponding linear increase in retention of the denture and the result may suffer. Therefore, when at least four implants are planned, the restoration should be designed as implant-supported to maximise the value of the patient’s greater investment.
This article discusses just such a situation where a patient had experienced repeatedly low value from her investment of five implants. By redesigning her treatment to become implant-supported through the use of the Atlantis Conus concept, a successful result was achieved without the greater expense of a fixed hybrid. The final result was functionally comparable to a fixed restoration while providing lip and cheek support of a removable prosthesis without complicating or obstructing oral hygiene.
The telescopic design of the Atlantis Conus concept provides outstanding retention of the prosthesis during function as edentulous patients chew in a relatively flat elliptical pattern and the bridge can only be removed vertically. The abutments themselves are patient-specific and can be made for all major implant systems, allowing rescue of many frustrating results with overdentures.
As long as there is sufficient interarch space (at least 12 mm), existing finished dentures can be retrofit with Atlantis Conus Abutments, reducing patient cost while providing a stable result. Cast chrome frame reinforcement is advised for all new Atlantis Conus prostheses as the tremendous increase in strength of the bridge by the frame more than offsets the slight increase in cost and may actually reduce required inter-arch space.
The clinical procedure is relatively simple and comparable to implant overdentures; however, because the abutments are patient-specific, tooth position must be established before the design of the abutments is begun.
Conclusion
A patient with an 11-year history of frustration with her dental implant investment was treated successfully with the Atlantis Conus concept using patient-specific abutments and SynCone caps, providing an implant-supported, removable bridge with all the benefits of a fixed design and none of the limitations.
Acknowledgements
The author would like to thank Fred Senne, John Bergstresser and Sean Ferguson for their expertise and information. The author would also like to thank Tom Wiand and the talented team at Wiand Dental Laboratory for the laboratory procedures and products described in this article.
Editorial note: A list of references is available from the publisher. This article is the first was published in CAD/CAM international magazine of digital dentistry No. 02/2017.
A 59-year-old male patient was looking for a new fixed restoration for his maxilla. His case history showed no general disease. The patient had been fitted ...
Nowadays, virtual planning and the assisted placement of implants in 3-D positions relative to the bone, soft tissue and final planned prosthesis are ...
An 82-year-old patient presented for complete rehabilitation. The existing maxillary bridge showed Grade III mobility and the residual mandibular teeth ...
The efficacy of dental implant treatment is well-documented and its further development includes protocols for simplifying the procedures. The immediate ...
Implant planning and placement in the completely edentulous maxilla can present challenges both surgically and prosthetically whether a removable or fixed ...
An adequate bone volume at the future implant site is a prerequisite for ideal implant placement and implant success. A residual bone with a vertical ...
Modern dentistry is undergoing a technological revolution, driven by the integration of advanced digital tools in diagnostics, planning and treatment. Among...
Prosthetically driven implant placement has become a fundamental principle in contemporary implant dentistry, particularly in the treatment of edentulous ...
Modern dentistry should strive to preserve all maintainable natural teeth whenever possible, in line with the principles of minimal invasiveness and ...
The combination of advanced materials and manufacturing techniques makes the industrial production of prosthetic components possible for every clinical ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






























To post a reply please login or register