Dr Elham Kateeb’s professional career has been devoted to dentistry: She is an associate professor of dental public health and the dean of scientific research at Al-Quds University in Palestine, an elected member of FDI World Dental Federation’s Public Health Committee and a health service researcher, to name but a few of her responsibilities. She is also involved in the education of a future generation of dentists, an undertaking which is not without its challenges. The ongoing COVID-19 pandemic, in particular, has had a great impact on the way she and her students work and learn together. In an interview with Dental Tribune International, Kateeb spoke about these difficulties and of how there could be a positive outcome for the whole of dentistry.
Dr Kateeb, you have recently contributed to a study that concerns dental students and their readiness to tackle the COVID-19 pandemic during the early days of their profession. What motivated you to investigate this topic?
Being a faculty member at Al-Quds University College of Dentistry, I witnessed the panic we went through during the first days of the total lockdown. We had to make the right decisions about the training of our dental students. Like many institutions around the world, Al-Quds University closed down its physical campus on 5 March 2020 and switched to online learning. After recommendations from the U.S. Centers for Disease Control and Prevention and the World Health Organization, the Palestinian Ministry of Health restricted the work of private dental clinics to only urgent dental care carried out under very strict infection control measures.
Thus, in our dental outpatient clinics, we had no choice other than to shut down our services completely and send the students home. We switched to online education and tried to keep the students engaged through weekly meetings via Zoom in which we discussed clinical issues related to our clinical work and patient cases or watched videos that demonstrated clinical procedures. This took place while the world was exploring the nature of this virus, its transmission modes and ways to control it. Nothing was clear, but the first impression was that dental clinic settings with all their aerosol-generating procedures were areas of the highest risk for SARS-CoV-2 transmission. Al-Quds University College of Dentistry was one of the first dental schools to announce a return to clinical training in June 2020. After having had very limited clusters of cases in the first wave and after securing good supplies of advanced personal protective equipment for the dental students, it was reasonable for the college administration to take such a decision.
However, from being in close contact with the students through the Zoom meetings, I sensed how hesitant and fearful they were about this decision. Since there were all these uncertainties about the virus—its virulence, severity, fatality and lack of straightforward treatment options—students thought that it was too soon to go back to seeing patients. Therefore, I decided to survey our students and assess how they felt about going back to seeing patients in outpatient clinics. I thought that this kind of information could be helpful for administrations and dental schools throughout the world. We examined issues related to the students’ readiness to treat patients during the COVID-19 pandemic, their preparedness and their training in infection control measures. It was important to build trust, provide information and care for the students’ psychological status.
This study was conducted in May 2020, just a few weeks before they actually returned to their clinical training.
“Now everything is different, starting from very strict measures imposed by the dental clinic’s administration and ending with close follow-up on students’ adherence to these new protocols”
In the study, it says that the dental students perceived the standard infection control protocols used prior to the COVID‐19 pandemic to be inadequate and were therefore less confident in handling patients because of transmission risks. In what ways were these protocols inadequate and what is different now?
The infection control measures used by students before the pandemic were the standard ones used in most parts of the world: surgical masks, gloves, white lab coats, wrapping dental surgeries, changing gloves and masks between patients, autoclaving all instruments and handpieces and wiping benches and dental chairs with alcohol. The problem was with adherence to the clinic’s rules. A quick survey that was conducted among students in autumn 2018 showed that students were reluctant to comply with some practices such as the wearing of face shields, the wearing of disposable gowns over their white coats or the using of mouth rinse for patients.
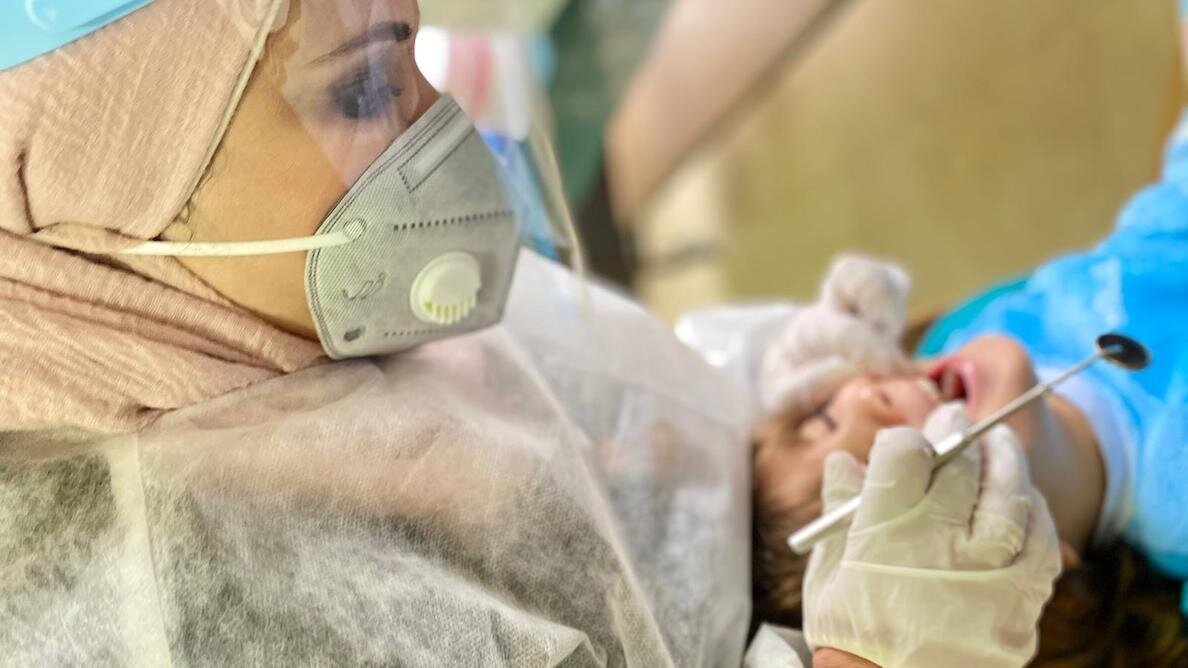
Now everything is different, starting from very strict measures imposed by the dental clinic’s administration and ending with close follow-up on students’ adherence to these new protocols. New strict measures include advanced personal protective equipment, such as face shields, N95 masks, head covers, shoe covers and disposable gowns, as well as stricter clinic sterilisation and ventilation and physical distancing between surgery areas. In addition, very strict protocols were imposed for the handling of instruments and materials and for the disinfection of dental surgeries and benches. Patient temperature screening on arrival at the clinic’s reception area was added to the routine history taking of patients. After having implemented these measures, it will be interesting to reassess the students’ level of confidence about dealing with COVID-19 patients.
How can control measures be improved, and do you think that they are here to stay or that the standards will go back to the way they were before as soon as the pandemic is under control?
Infection control measures have improved a great deal in our dental clinics, which is very encouraging. I think we intend to keep this as the new standard at least for a while. Face shields and disposable gowns will be the new norm. However, I don’t think the clinic’s administration can afford the physical distancing between patients created by leaving one clinic empty between two working clinics. Therefore, they will need to think about how they can close the open spaces and at the same time retain good ventilation. I think this will be a challenge in the next few months. Our understanding of SARS-CoV-2 transmission is advancing, and these control measures will have to adapt.
However, we need to at least keep the measures such as wearing a face shield, good hand hygiene, changing surgical masks between patients, wearing gloves, wrapping dental surgeries, and disinfecting benches and dental chairs properly. This pandemic has enforced what we always wanted our students to do, but now there is no space for mistakes or refusal to adhere to the protocols. The good thing about this pandemic is how it has increased awareness of the possibility of transmitting infectious diseases in dental settings and of how dental settings can be places of high risk for transmission if strict protocols are not implemented adequately. Among all other healthcare workers, we dentists are experts in infection control. We just need some time to regain confidence in our measures and realise that with good adherence to these measures we can practise safely in order to provide the very important health service of oral healthcare.
“Dental students are in a unique situation, different from that of all other health professions and non-health students”
On top of adapting to the many changes COVID-19 has brought into dental students’ work lives, they have had to adapt academically. What are the greatest challenges there, and what needs to be done in order to overcome them?
Dental students are in a unique situation, different from that of all other health professions and non-health students. Dental students have theory classes in basic sciences, medical sciences and dental sciences, labs in basic sciences and medical sciences, labs in preclinical training, and clinical training in dental outpatients’ clinics. Therefore, Zoom and online learning cannot cover all that. Even when university students return to campus and follow strict safety measures such as mandatory face masks and physical distancing for labs and practical sessions, this solves the problem only in medical, basic science and preclinical lab work but not in clinical training, which remains a challenge.
Dealing with patients from the local community was not easy, as there were increasing numbers of COVID-19 patients. This reached 800 cases a day in the second wave starting at the end of June 2020. Measures such as the triaging of patients by phone, temperature screening at the clinic’s entrance, the introduction of strict infection control measures and the use of advanced personal protective equipment made the conditions a bit better for students and enabled them to complete the summer and part of the autumn training with fewer interruptions. We managed to administer the final exams in person with mask-wearing and physical distancing. Some Zoom sessions were devoted to clinical presentations and patient case discussions. All theory lectures were still on Zoom. We managed to arrange for one outreach community service visit to a refugee camp in November 2020. It was a great experience, and enabled the students to provide care to the community during the pandemic. Personally, I have missed the community outreach visits the most.
What can dental students do to build up their confidence levels during this pandemic and potential future ones?
Some methods that are helpful include:
- periodic training on the implementation of infection control measures;
- providing dental students with courses on infectious diseases;
- empowering dental students to take a full role in diagnosing diseases and identifying symptoms related to infectious diseases and other systemic conditions;
- strengthening components of the dental curriculum related to medicine, medical problems and pharmacology;
- empowering dental students to think not only as interventionists but also as physicians;
- shifting the focus of dental learning from the restorative model to prevention, risk assessment and patient education; and
- changing the focus of clinical training to minimal intervention and procedures generating fewer aerosols such as atraumatic restorative treatment, the Hall technique and the use of silver diamine fluoride.
Is there anything you’d like to add?
I think we need to use this pandemic to restructure our dental education in a way to make it more vital for interprofessional health education. Future dentists need to be equipped adequately with the skills, knowledge and resilience necessary in order to be included in the frontline in any pandemic and to not be sidelined or asked to stay home and not go to work. They need to learn how to defend oral health and oral healthcare as a priority in any health crisis.
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





























Thank you for your comment! We agree: It is really important to not down-play the pandemic and the effect it has on all members of society.
A great read that helps dental students reflect on what has been going on this past year.