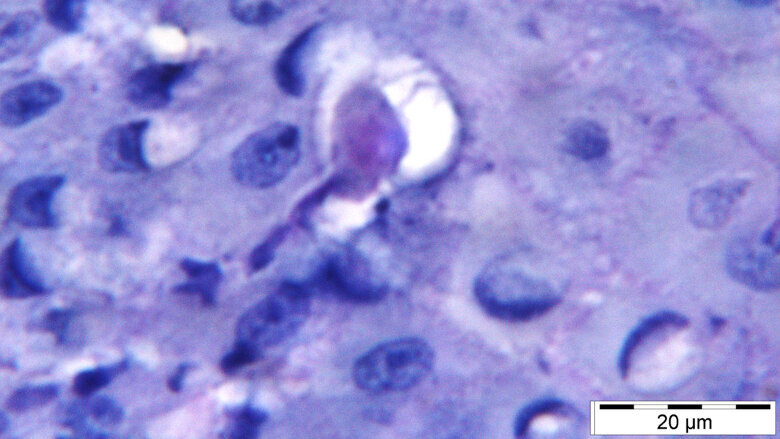
BERLIN, Germany: For the first time, researchers from Charité—Universitätsmedizin Berlin have shown that the amoeba Entamoeba gingivalis, commonly found in the oral cavity, plays a role in both severe tissue inflammation and tissue destruction. Once the parasite has invaded the gingival tissue, it feeds on its cells and causes tissue destruction. According to the study findings, most patients with severe and recurrent periodontitis showed an increased presence of the unicellular organism in their oral cavities.
In Germany, approximately 15% of people are affected by a particularly severe form of periodontitis. The disease has a strong association with arthritis, cardiovascular disease and cancer. In patients with gingival disease, a decrease in the diversity of the oral flora coincides with an increase in the presence of E. gingivalis.
Scientists have long been aware of the virulence potential of this genus of amoebae. The gastro-intestinal parasite Entamoeba histolytica, for instance, causes a disease known as amebiasis, one of the most common causes of death from parasitic diseases worldwide. “We have shown that an amoeba like E. gingivalis, which colonises the oral cavity, will invade the oral mucosa and destroy gingival tissue. This enables increased numbers of bacteria to invade the host tissue, which further exacerbates inflammation and tissue destruction,” said lead researcher Prof. Arne Schäfer, head of the research department in the Department of Periodontology and Synoptic Dentistry at the Institute of Dental and Craniofacial Sciences at Charité.
The researchers are the first to describe the precise role of E. gingivalis in the pathogenesis of inflammation. During their analysis of inflamed periodontal pockets, they detected evidence of the amoeba in approximately 80% of patients with periodontitis, but in only 15% of the control group. Observations revealed that, after invading the gingivae, the parasites migrate inside the tissue, feeding on and killing host cells. Cell culture experiments showed that infection with E. gingivalis slows the rate at which cells grow, eventually leading to cell death.
“This parasite, which is transmitted by simple droplet infection, is one potential cause of severe oral inflammation”
– Prof. Arne Schäfer, Charité Berlin
The researchers concluded that the amoeba’s role in inflammation shows distinct parallels to the pathogenesis of amebiasis. “E. gingivalis actively contributes to cell destruction inside the gingival tissue and stimulates the same host immune response mechanisms as E. histolytica during its invasion of the intestinal mucosa,” explained Schäfer. “This parasite, which is transmitted by simple droplet infection, is one potential cause of severe oral inflammation.”
Treatment success is often short-lived in patients with periodontitis. This might be due to the high virulence potential of this previously unnoticed, yet extremely common, amoeba. “We identified one infectious parasite whose elimination could improve treatment effectiveness and long-term outcomes in patients with gum disease,” said Schäfer. “Current treatment concepts for periodontitis fail to consider the possibility of infection by this parasite or its successful elimination,” he added. A clinical trial to determine the extent to which the elimination of this amoeba might improve treatment outcomes in patients with periodontitis is underway.
The study, titled “Entamoeba gingivalis causes oral inflammation and tissue destruction”, was published online on 5 February 2020 in the Journal of Dental Research, ahead of inclusion in an issue.
Tags:
OKAYAMA, Japan: In a recent study, researchers from Okayama University investigated whether involuntary masseter muscle activity showed any specific pattern...
UMEÅ, Sweden: In the largest study of its kind, researchers from the Institute of Odontology at Umeå University in Sweden and the Bristol Dental School in...
HELSINKI, Finland: Antibiotic overprescribing continues to be a major concern in dentistry. In most cases, readily prescribing antibiotics to patients ...
KNOXVILLE, Tenn., U.S.: The obesity epidemic in the U.S has reached a new level of severity. Supersized food portions and an inactive lifestyle are often ...
BETHLEHEM, Pa., US: Aggressive forms of periodontitis associated with Aggregatibacter actinomycetemcomitans are often difficult to treat with traditional ...
NEW LONDON, Conn., US: Previous clinical studies have suggested that lycopene—a pigment abundant in tomatoes and other red fruits—may improve ...
KUOPIO, Finland: A large Finnish population-based study has assessed periodontitis using salivary biomarkers—rather than clinical and radiographic oral ...
FREIBURG, Germany: Thousands of different bacteria colonise the oral cavity, many of which remain unidentified. Researchers in Freiburg are now using a ...
LOS ANGELES, U.S.: Recent studies showing an increase in patients with periodontitis, as well as studies linking it with Alzheimer’s disease, have led to ...
STONY BROOK, N.Y., US: The applicability and efficacy of artificial intelligence (AI) within dentistry appears to be limitless. With each passing day, ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East


































To post a reply please login or register