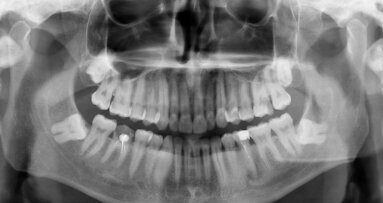
Endodontic treatment can attain success rates of between 85 and 97%.1 Adequate treatment protocols, knowledge and infection control are essential to achieving such rates (Figs. 1a–d).2 It is well known that apical periodontitis is caused by the communication of root-canal micro-organisms and their by-products to the surrounding periodontal structures. Exposure of dental pulp directly to the oral cavity or via accessory canals, open dentinal tubules or periodontal pockets is the most probable route of the endodontic infection.2,3
Clinically, apical periodontitis is not evident as long as the necrotic tissue is not infected with micro-organisms.4–6 There are up to 40 isolated species of bacteria present in the root canal. Cocci, rods, filaments, spirochaetes, anaerobic and facultative anaerobic are frequently identified in primary infection. Fungus can also be isolated.2,7 Endodontic microbiota can be found suspended in the main root canal, attached to the canal walls and deep in the dentinal tubules at a depth of up to 300µm (Figs. 2a–c). The absence of
cementum dramatically increases bacterial penetration into dentinal tubules.8–11
It has been shown that bacteria can also been found outside the root-canal system, located at the apical cementum and as an external biofilm on the apex.12–15 Following conventional endodontic treatment, 15 to 20% of non-vital teeth with apical periodontitis fail.16–18 The presence of bacteria after the decontamination phase or the inability to seal root canals after treatment are reasons for failure.2 The remaining contamination in endodontically treated teeth continues the infectious disease process in the periapical tissue.
Retreatments are the first choice for failed root canals. The microbiota found in persistent infections differ from that in primary infection (Figs. 3a–c). Facultative anaerobic Gram-positive (G+) and -negative (G-) micro-organisms and fungi are common.19–21 Special attention is given to Enterococcus faecalis, a resistant facultative anaerobic G+ cocci, identified in a much higher incidence in failed root canals.22–25 The importance of bacterial control plays a significant role in endodontic success. Adequate and effective disinfection of the root-canal system is necessary.
Endodontic therapy
The bacterial flora of the root canal must be actively eliminated through a combination of debridement and antimicrobial chemical treatment. Mechanical instrumentation eliminates more than 90% of the microbial amount.26 An important point to note is the adequate shaping of the root canal. Evaluating the antibacterial efficacy of mechanical preparation itself, Dalton et al.27 conclude that instrumentation to an apical size of #25 resulted in 20% of canals free of cultivable bacteria. When shaped to a size of #35, 60% showed negative results.
Irrigating solution has been used with mechanical instrumentation to facilitate an instrument’s cutting efficiency, remove debris and the smear layer, dissolute organic matter, clean inaccessible areas and act against micro-organisms. Sodium hypochlorite is the most common irrigant used in endodontics.28 It has an excellent cleansing ability, dissolves necrotic tissue, has a potential antibacterial effect and, depending on the concentration, is well tolerated by biological tissues. When accompanied by mechanical instrumentation, it reduces the number of infected canals by 40 to 50%.
Other irrigating solutions are also used during endodontic preparation. EDTA, a chelating agent used primarily to remove the smear layer and facilitate the removal of debris from the canal, has no antibacterial effect.29 Chlorhexidine gluconate has a strong antibacterial effect on an extensive number of bacterial species, even the resistant E. faecalis, but it does not break down proteins and necrotic tissue as sodium hypochlorite does.30
As mechanical instrumentation and irrigating solutions are not able to eliminate bacteria from the canal system totally—a requirement for root-canal filling—additional substances and medicaments have been tested in order to address the gap in standard
endodontic protocols. The principal goal of dressing the root canal between appointments is to ensure safe antibacterial action with long-lasting effects.31 A great number of medicaments have been used as dressing material, such as formocresol, camphorated parachlorophenol, eugenol, iodine-potassium iodide, antibiotics, calcium hydroxide and chlorhexidine.
Calcium hydroxide has been used in endodontic therapy since 1920.31 With a high pH at saturation (pH above 11), it induces mineralisation, reduces bacteria and dissolves tissue. For extended antibacterial effectiveness, the pH must be kept high in the canal and in the dentine as well. Sustaining the pH depends on the diffusion through dentinal tubules.32
Although most micro-organisms are destroyed at pH of 9.5, a few can survive a pH of 11 or higher, such as E. faecalis and Candida.21 Because of the resistance of some micro-organisms to conventional treatment protocols—and the direct relation between the presence of viable bacteria in the canal system and the reduced rate of treatment success—additional effort has to be made to control canal system infection.
Lasers in endodontics
Lasers were introduced to endodontics as a complementary therapy to conventional antibacterial treatment. The antibacterial action of Nd:YAG, diodes, Er:YAG and photoactivated disinfection (PAD) have been explored by a number of investigators. In the
following section, each laser is evaluated with the aim of selecting an adequate protocol with a high probability of success in teeth with apical periodontitis.
Nd:YAG laser
The Nd:YAG laser was one of the first lasers tested in endodontics. It is a solid-state laser. The active medium is usually yttrium aluminium garnet (Y3Al5O12), where some Y3+ ions are replaced by Nd3+ions. It is a four-level energy system operating in a continuous wave or pulsed mode. It emits a 1,064nm infra-red wavelength. Thus, this laser needs a guide light for clinical application. Flexible fibres with a diameter between 200 and 400µm are used as delivery systems. The laser can be used on intra-canal surfaces, in contact mode (Figs. 4a & b).
The typical morphology of root-canal walls treated with the Nd:YAG laser shows melted dentine with a globular and glassy appearance, and few areas are covered by a smear layer. Some areas show dentinal tubules sealed by fusion of the dentine and deposits of mineral components.33,34 This morphological modification reduces dentine permeability significantly.35,36 However, because the emission of the laser beam from the optical fibre is directed along the root canal, not laterally, not all root-canal walls are irradiated, which gives more effective action at the apical areas of the root.37 Undesirable morphological changes, such as carbonisation and cracks, are seen only when high energy parameters are used.
One of the major problems regarding intra-canal laser irradiation is the temperature increase at the external surface of the root. Laser light exerts a thermal effect when it reaches tissue. The heat is directly associated with the energy used, time and irradiation mode. An increase in temperature levels above 10°C per minute can cause damage to periodontal tissues, such as necrosis and anchylosis.
Lan38 evaluated in vitro the temperature increase on the external surface of the root after irradiation with a Nd:YAG laser under the following energy parameters: 50, 80 and 100mJ at 10, 20 and 30 pulses per second. The increase of temperature was less than 10°C. The same results were obtained by Bachman et al.39, Kimura et al.40 and Gutknecht et al.41
In contrast to the external surface, the intra-canal temperature rises dramatically at the apical area, promoting effective action against bacterial contamination. For the Nd:YAG laser, 1.5W and 15Hz, are safe energy parameters for temperature and morphological changes.33,41
The primary use of the Nd:YAG laser in endodontics is focused on elimination of micro-organisms in the root-canal system. Rooney et al.42 evaluated the antibacterial effect of Nd:YAG lasers in vitro.
Bacterial reduction was obtained considering energy parameters. The researchers developed different in vitro models simulating the organisms expected in non-vital, contaminated teeth. Nd:YAG irradiation was effective for Bacillus stearothermophilus,43,44 Streptococcus faecalis, Escherichia coli,45 Streptococcus mutans,46 Streptococcus sanguis, Prevotella intermedia47 and a specific micro-organism resistant to conventional endodontic treatment, E. faecalis.48–50 Nd:YAG has an antibacterial effect in dentine at a depth of 1,000µm (Fig. 5).50
Histological models were also developed in order to evaluate periapical tissue response after intra-canal Nd:YAG laser irradiation. Suda et al.51 demonstrated in dog models that Nd:YAG irradiation at 100mJ/30 pulses per second for 30 seconds was safe to surrounding root tissues. Maresca et al.,52 using human teeth indicated for apical surgery, corroborated Suda et al.’s51 and Ianamoto et al.’s53 results. Koba et al.54 analysed histopathological inflammatory response after Nd:YAG irradiation in dogs at 1 and 2W. Results showed significant inflammatory reduction at four and eight weeks compared with the non-irradiated group.
Clinical reports published in the literature confirm the benefits of intra-canal Nd:YAG irradiation. In 1993, Eduardo et al.55 published a successful clinical case that combined conventional endodontic treatment with Nd:YAG irradiation for retreatment, apical periodontitis, acute abscess and perforation. Clinical and radiographic follow-up showed complete healing after six months.
Similar results were shown by Camargo et al.56 Gutknecht et al.57 reported a significant improvement in healing of laser-treated infected canals, when compared with non-irradiated cases.
Camargo et al.58 compared in vivo the antibacterial effects of conventional endodontic treatment and the conventional protocol associated with the Nd:YAG laser. Asymptomatic teeth with apical radiolucency and necrotic pulps were selected and divided into two groups: conventional treatment and laser irradiated. Microbiological samples were taken before canal instrumentation, after canal preparation and/or laser irradiation and one week after treatment. The results showed a significant antibacterial effect in the laser group compared with conventional treatment. When no other bactericidal agent was used, it was assumed that the Nd:YAG laser played a specific role in bacterial reduction for endodontic treatment in patients.
Diodes
The diode laser is a solid-state semiconductor laser that uses a combination of gallium, arsenide, aluminium and/or indium as the active medium. The available wavelength for dental use ranges between 800 and 1,064nm and emits in continuous wave
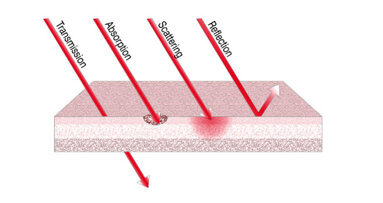
and gated pulsed mode using an optical fibre as the delivery system (Figs. 6a & b). Diode lasers have gained increasing importance in dentistry owing to their compactness and affordable cost. A combination of smear layer removal, bacterial reduction and reduced apical leakage are advantages of this laser and make it viable for endodontic treatment. The principal laser action is photo-thermal.
The thermal effect on tissue depends on the irradiation mode and settings. Wang et al.59 irradiated root canals in vitro and demonstrated a maximum temperature increase of 8.1°C using 5W for seven seconds. Similar results were obtained by Da Costa Ribeiro.60 Gutknecht et al.61 evaluated intra-canal diode irradiation with an output of 1.5W and observed a temperature increase of 7°C in the external surface of the root using a 980nm diode laser at a power setting of 2.5W at a continuous and chopped mode, and found that the temperature increase never exceeded 47°C, which is considered safe for periodontal structures.41
Clean intra-canal dentinal surfaces with sealed dentinal tubules, indicating melting and recrystallisation, were morphological changes observed at the apical portion of the root after intra-canal diode irradiation.62 In general, near infra-red wavelengths, such as 1,064 and 980nm, promote fusion and recrystallisation on the dentinal surface, sealing dentinal tubules.
The apparent consensus is that diode laser irradiation has a potential antibacterial effect. In most cases, the effect is directly related to the amount of energy delivered. In a comparative study by Gutknecht et al.,63 an 810nm diode was able to reduce bacterial contamination by up to 88.38% with a distal output of 0.6W in continuous wave mode.
A 980nm diode laser has an efficient antibacterial effect of an average of between 77 to 97% in root canals contaminated with E. faecalis. Energy outputs of 1.7, 2.3 and 2.8W were tested. Efficiency was directly related to the amount of energy and dentine thickness.64
Er:YAG laser
Er:YAG lasers are solid-state lasers with a lasing medium of erbium-doped yttrium aluminium garnet (Er:Y3Al5O12). Er:YAG lasers typically emit light with
a wavelength of 2,940nm, which is infra-red light. Unlike Nd:YAG lasers, the output of an Er:YAG laser is strongly absorbed by water because of atomic resonances. The Er:YAG wavelength is well absorbed by hard dental tissue. This laser was approved for den-
tal procedures in 1997. Smear layer removal, canal preparation and apicoectomy are indications for endodontic use (Fig. 7).
The morphology of a dentinal surface irradiated with an Er:YAG laser is characterised by clean areas showing open dentinal tubules, free of a smear layer, in a globular surface. Bacterial reduction using the Er:YAG was observed by Moritz et al.65
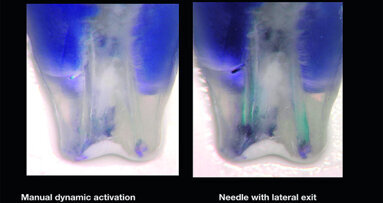
Stabholz et al.37 describe a new endodontic tip that can be used with an Er:YAG laser system. The tip allows lateral emission of the radiation rather than direct emission through a single opening at the far end. It emits through a spiral tip located along the length of the tip. In examining the efficacy of the spiral tip in removing the smear layer, Stabholz et al.66 found clean intra-canal dentinal walls free of a smear layer and debris under SEM valuation.
Photoactivated disinfection
PAD is another method of disinfection in endodontics and is based on the principle that photoactivated substances, which are activated by light of a particular wavelength, bind to target cells. Free radicals are formed, producing a toxic effect to bacteria. Toluidine blue and methylene blue are examples of photoactivated substances. Toluidine blue is able to kill most oral bacteria. In in vitro studies, PAD has an effective action against hotosensitive bacteria such as E. faecalis, Fusobacterium nucleatum, P. intermedia, Peptostreptococcus micros and Actinomycetemcomitans.67,68 On the other hand, Souza et al.,69 evaluating PAD antibacterial effects as a supplement to instrumentation/irrigation of canals infected with E. faecalis, did not prove a significant effect regarding intra-canal disinfection. Further adjustments to the PAD protocols and comparative research models may be required before recommendations can be made regarding clinical usage.
Discussion and conclusion
There are good reasons to focus the treatment of non-vital contaminated teeth on the destruction of bacteria in the root canal. The possibility of a favourable treatment outcome is significantly higher if the canal is free from bacteria when it is obturated. If, on the other hand, bacteria persist at the time of root filling, there is a higher risk of treatment failure. Therefore, the prime objective of treatment is to achieve complete elimination of all bacteria from the root-canal system.2,31
Today, the potential antibacterial effect of laser irradiation associated with the bio-stimulation action and accelerated healing process is well known. Research has supported the improvement of endodontic protocol. Laser therapy in endodontic treatment offers benefits to conventional treatment, such as minimal apical leakage, effective action against resistant micro-organisms and external apical biofilm, and an increase in periapical tissue repair. For this reason, laser procedures have been incorporated into conventional therapeutic concepts to improve endodontic therapy (Figs. 8a–d).
Clinical studies have proven the benefits of an endodontic laser protocol in apical periodontitis treatment. For endodontic treatment, the protocol entails standard treatment strategies for cleaning and shaping the root canal to a minimum of #35, irrigating solutions with antibacterial properties and intra-canal laser irradiation using controlled energy parameters. Ideal sealing of the root canal and adequate coronal restoration are needed for an optimal result.
In practice, little additional time is required for laser treatment. Irradiation is simple when flexible optical fibres of 200µm in diameter are used. The fibre can easily reach the apical third of the root canal, even in curved molars (Fig. 9). The released laser
energy has an effect in dentine layers and beyond the apex in the periapical region. The laser’s effect extends to inaccessible areas, such as external biofilm at the root apex.
The irradiation technique must adhere to the following basic principles. A humid root canal is required and rotary movements from the coronal portion to the apex should be carried out, as well as scanning the root canal walls in contact mode (Figs. 10a–c). The power settings and irradiation mode depend on one’s choice of a specific wavelength.
Nd:YAG, diodes of different wavelengths, Er:YAG, and low-power lasers can be used for different procedures with acceptable results. Laser technology in dentistry is a reality. The development of specific delivery systems and the evolution of lasers combined with a better understanding of laser–tissue interaction increase the opportunities and indications in the endodontic field.
Editorial note: A complete list of references is available from the publisher.
This article was originally published in roots Vol. 8 Issue. 1, 2012. A complete list of references is available from the publisher.
The population is ageing rapidly because of the prolonged life expectancy evident in most industrialised countries in the world. Accordingly, the number of ...
After explaining the basic physics of the laser and its effects on both bacteria and dentinal surfaces, the second part of this article series will analyse ...
FKG Dentaire is considered a leader in innovation, cultivating a company culture defined by creativity and ingenuity. Situated in the heart of the Swiss ...
“Faster, higher, stronger”—this motto certainly no longer applies only to the Olympic Games. How can certain tasks be performed even more precisely, ...
The main goals of endodontic treatment are the effective cleaning of the root-canal system. Traditional endodontic techniques use mechanical instruments, as...
From the early 20th century, when Walter Hess and Ernest Zürcher [1] demonstrated root canal anatomy with an unprecedented visual clarity, its complexity ...
NEW YORK, U.S.: When it comes to endodontic treatment, elimination of the microbial flora from the root canal system is a primary focus. In a free Dental ...
How to achieve greater efficiency, safety and job satisfaction in endodontics—endodontist and trainer Dr Sabine Remensberger has been sharing her ...
Despite being one of the most easily preventable diseases, dental caries still poses a major health concern across all age groups around the world. Very ...
Dental Tribune International (DTI) recently had the opportunity to speak with Dr Sushil Koirala, the founder and chairman of National Dental Hospital and ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





































To post a reply please login or register