Our collaboration with speech therapists is yet to be well defined, but great efforts are being made in this regard.2 Often, we receive requests for expansion of the palate because it is not wide enough to accommodate the tongue, bite closure is impeded because of incorrect lingual posture and swallowing is difficult. Especially jaw alignment, closure of excessive overjet (often due to poor oral habits) and intervention for reverse overjet are required. 3
Recently, sleep medicine has made orthodontists more aware of the importance of having an adequate lingual frenulum, both because a short frenulum is now considered a risk factor for the onset of obstructive sleep apnoea and because this is closely correlated with contraction of the maxillary inter-canine diameter.4 Dysfunctional swallowing and all forms of orofacial muscle dysfunction are now considered causative factors of malocclusion at an early age.5 At the same time, malocclusion, that is, the reduction of upper diameters, inversion of the posterior or anterior bite, open bite or closed bite, is considered to be the cause of inadequate mandibular and lingual movements that often result in phonological disorders,6, 7 which at early age are not self-resolving. Indeed late-talkers remain stigmatised well into adulthood. 8, 9
All this has led a group of us at the Consorzio Universitario Humanitas, a consortium of educational institutions, to try to define a diagnostic protocol to be shared by speech therapists and orthodontists10 and a decision making scale11 for early orthodontic and logopaedic intervention. These two tools are now being studied and endorsed as part of European paediatric deglutology projects.
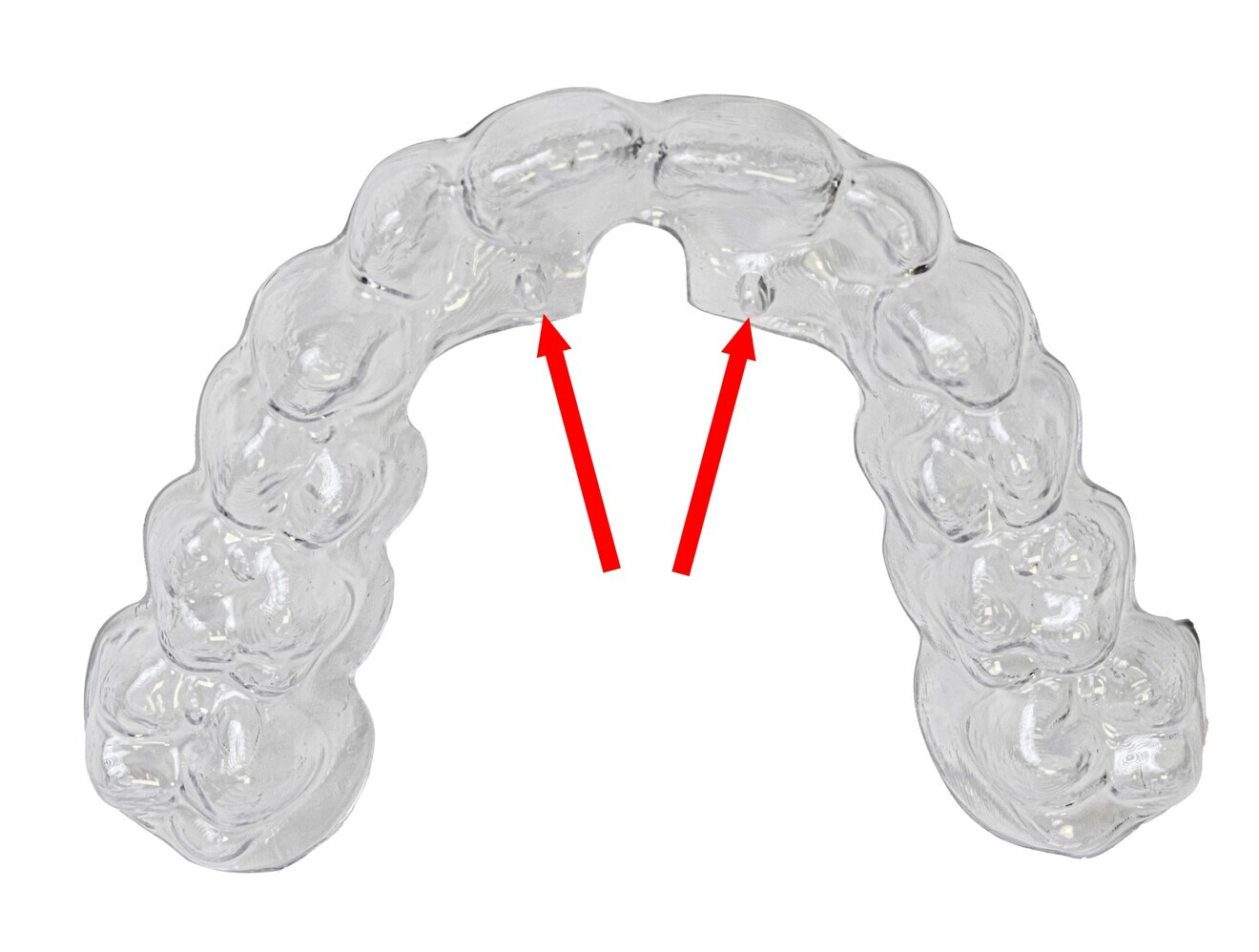
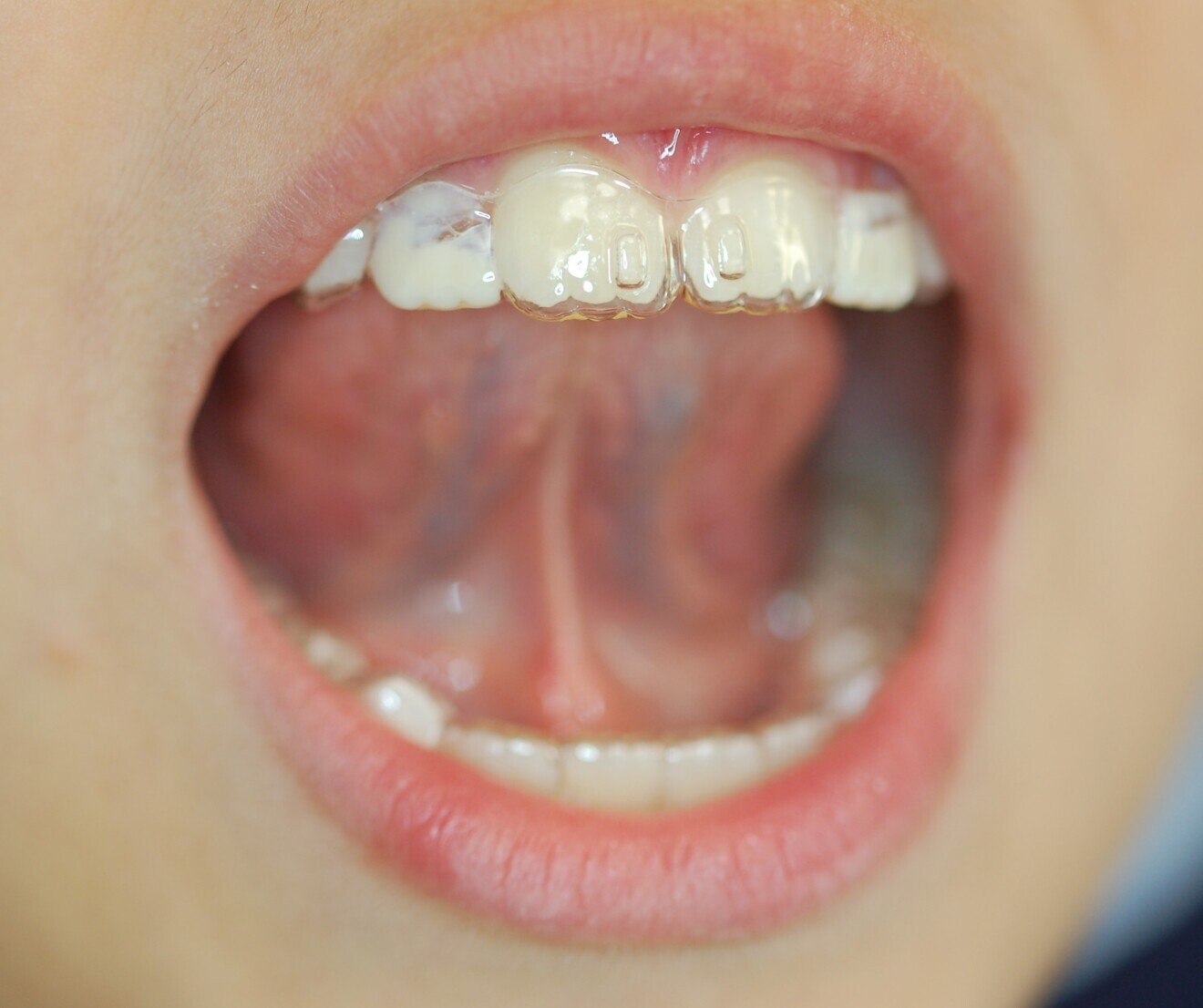
Orthodontic diagnosis and treatment thus have to involve new dynamic and functional considerations as well as address the arising therapeutic challenges using the most effective and tolerable instruments from an early age. The challenge is to identify devices that not only correct form but also enable function. The use of paediatric aligners is now a reality that has attracted great attention from clinicians in recent years.12–17 In this article, we would like to illustrate a case report describing the potential of an innovative treatment which combines aligners, Nuvola Junior (Nuvola World), with the simultaneous use of a myofunctional device, Intercept (Nuvola World).11
Materials and methods
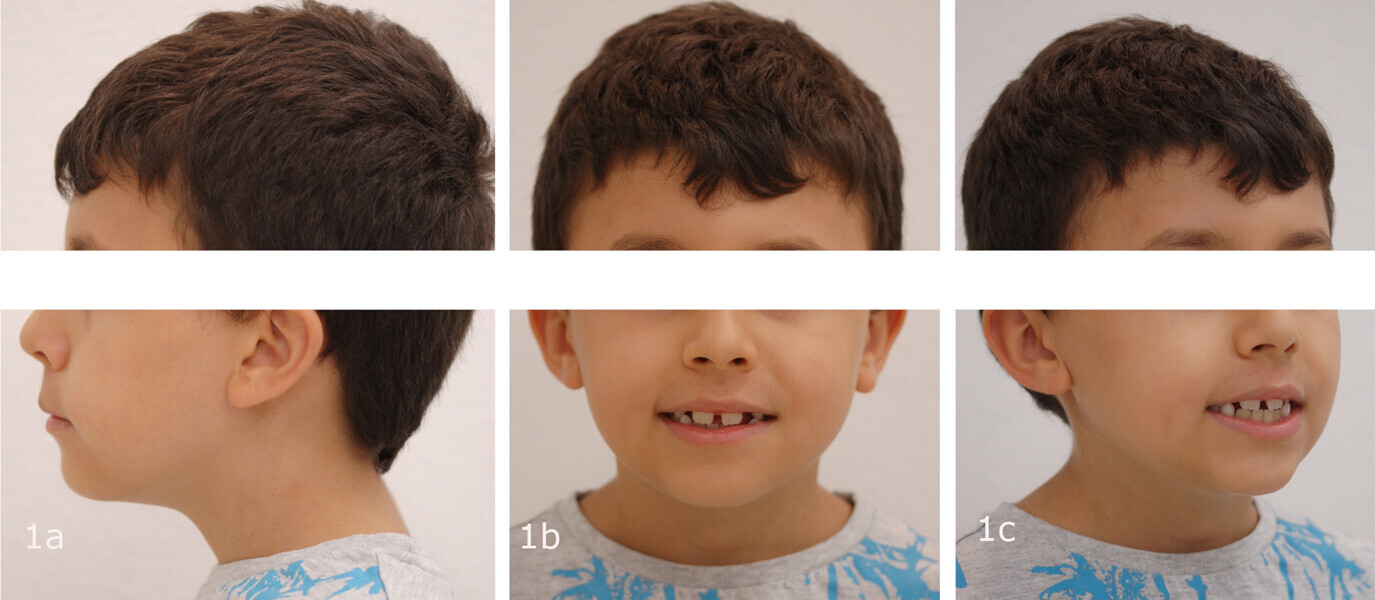
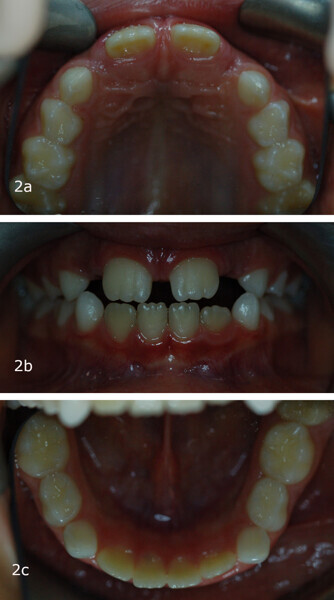
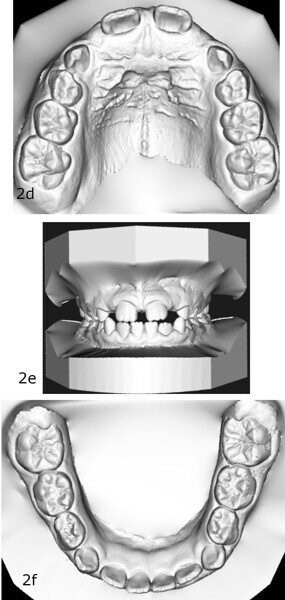
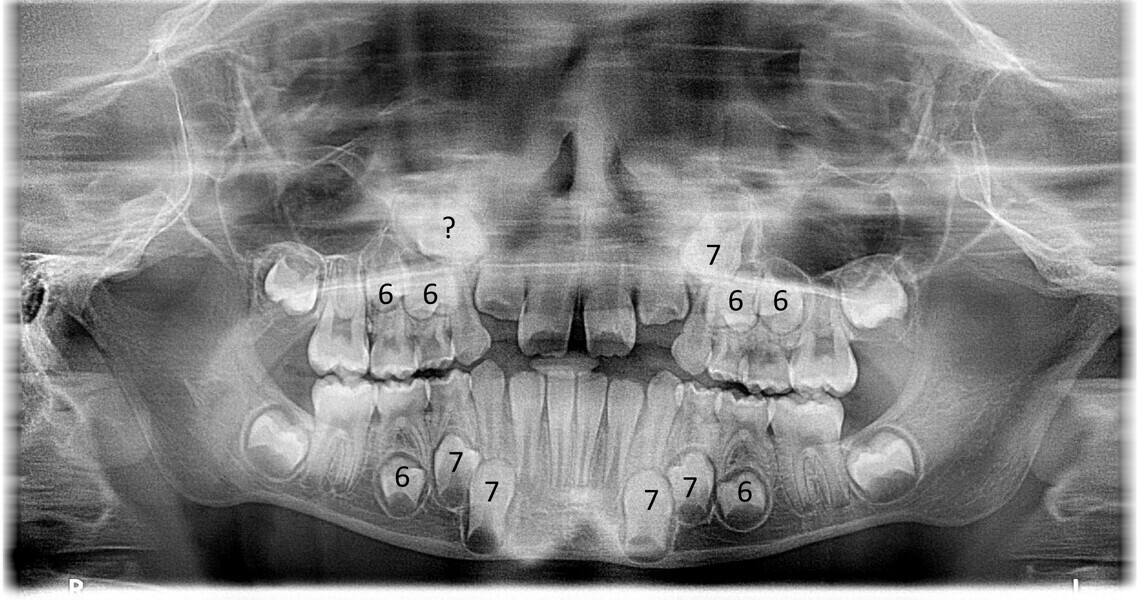
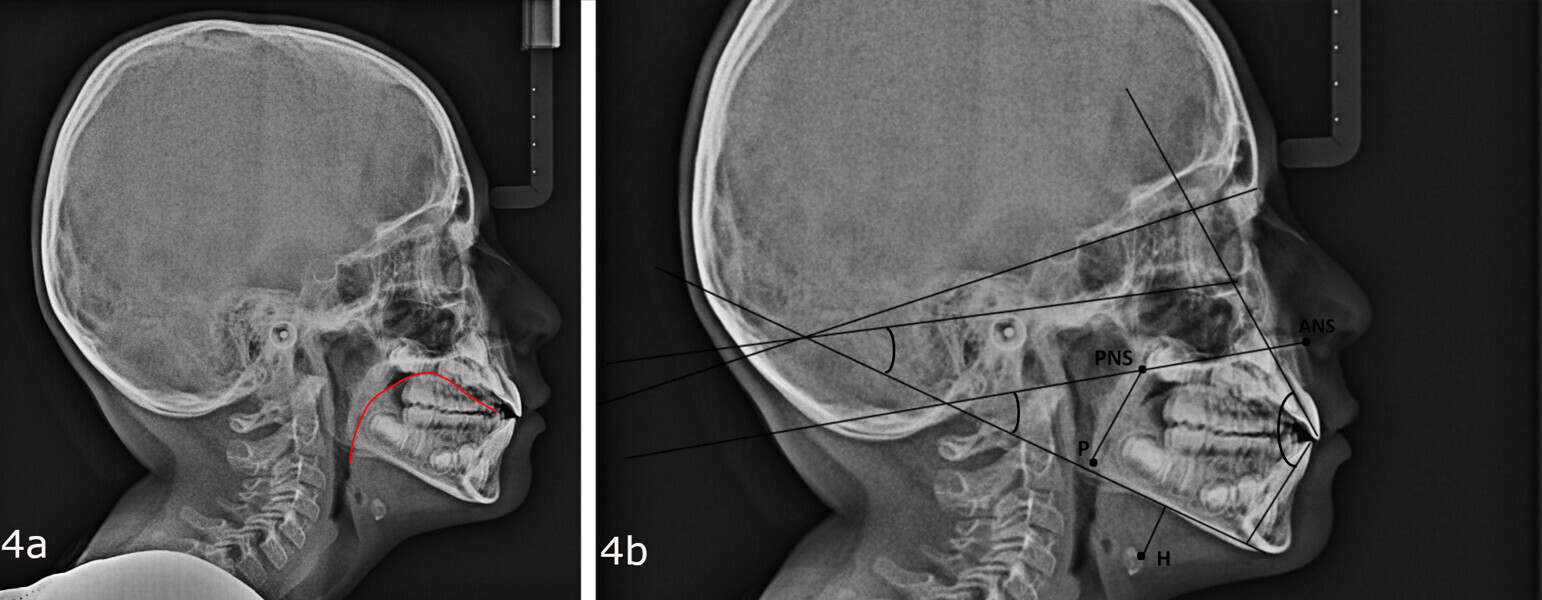
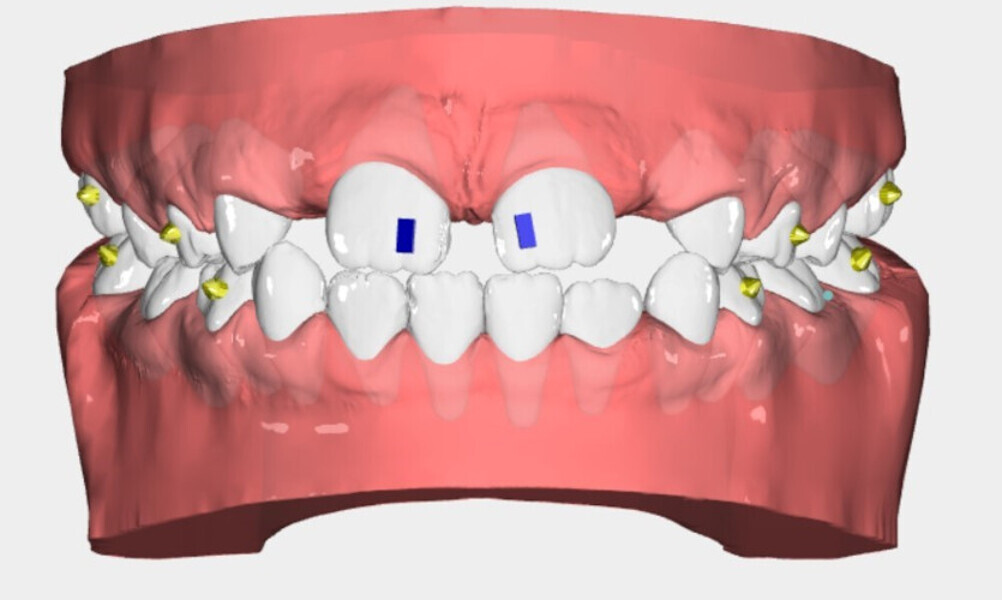
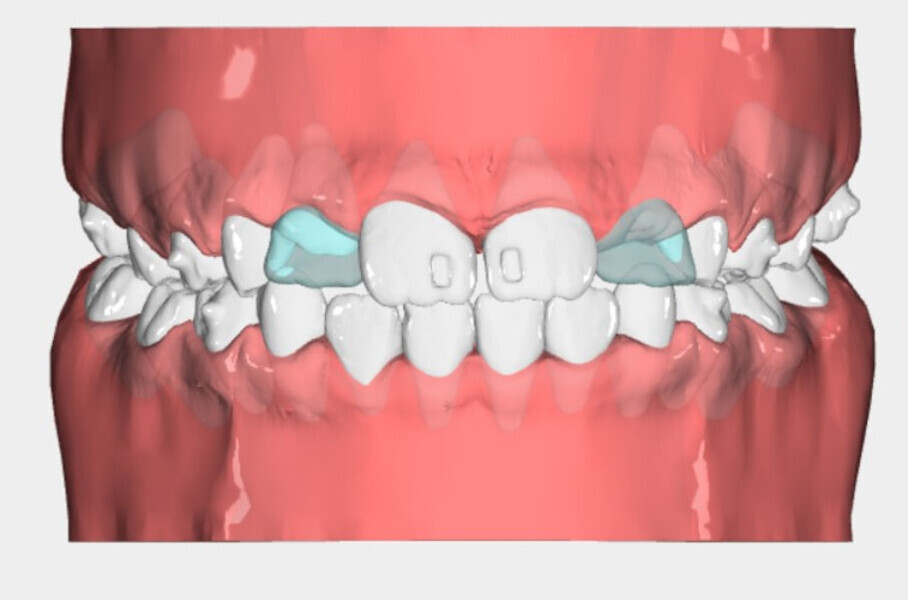
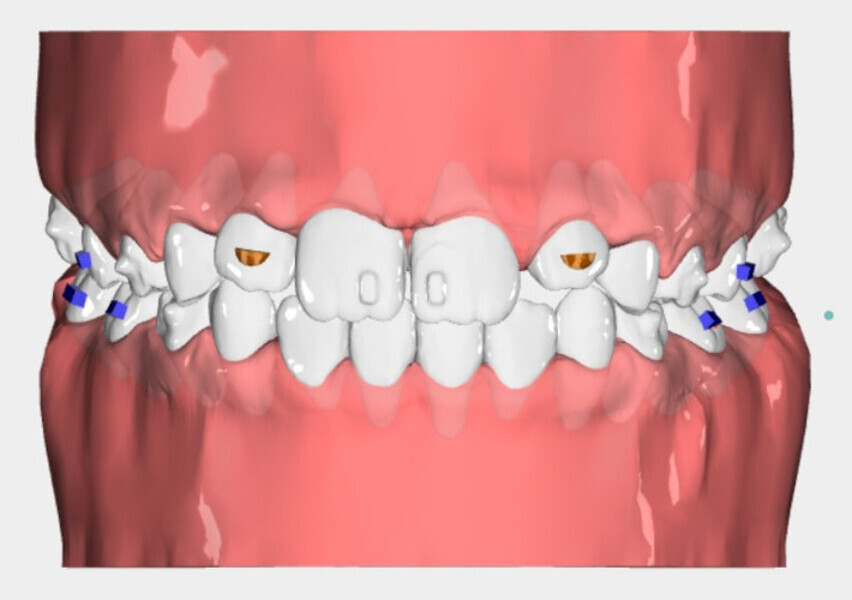
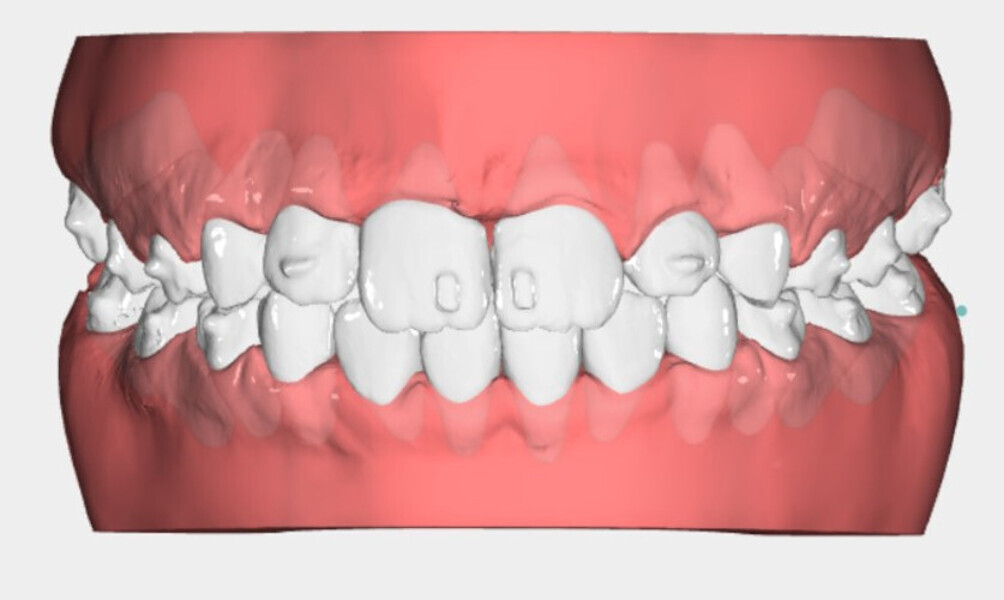
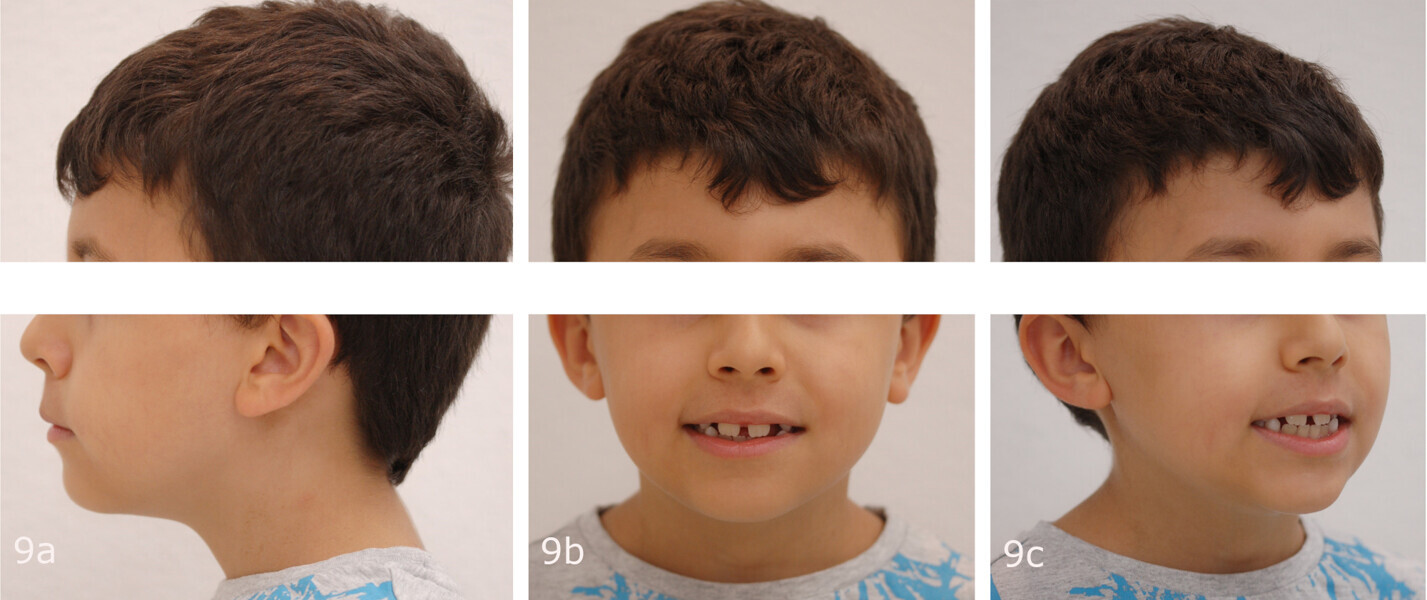
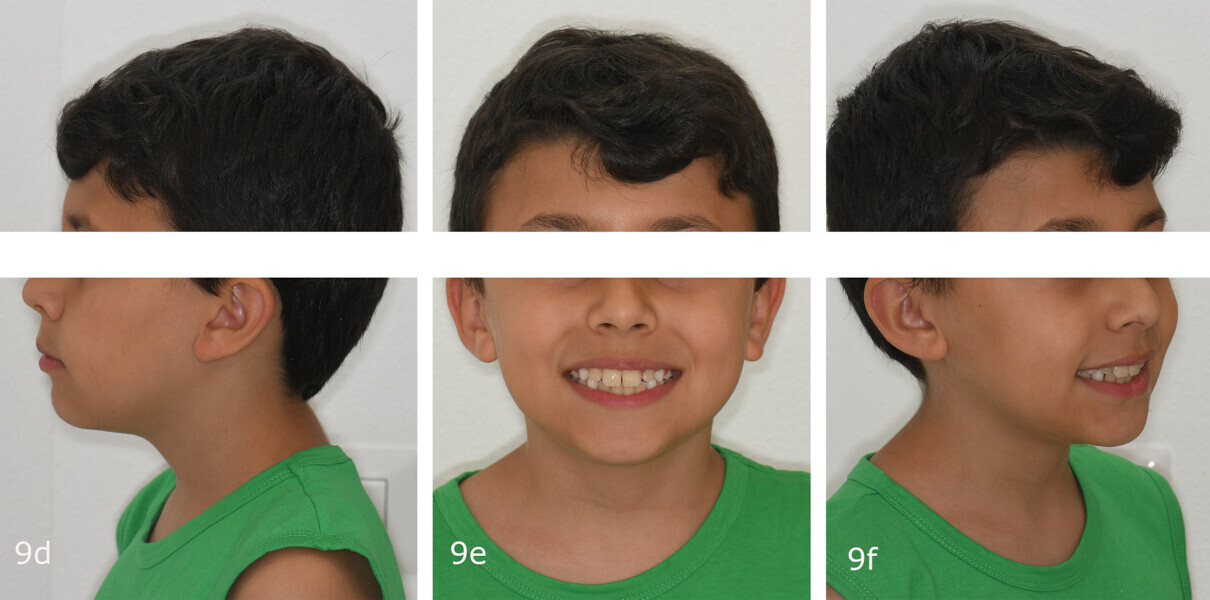
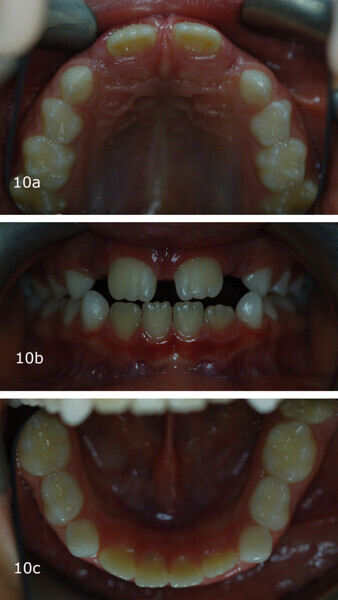
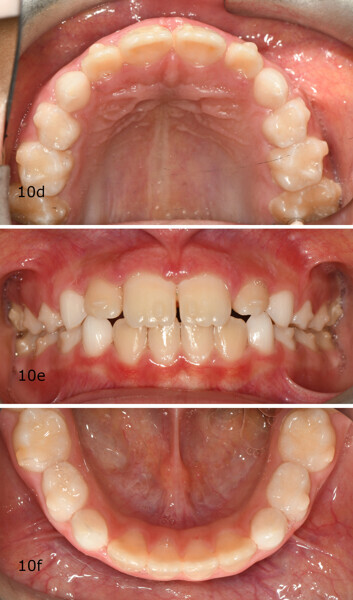
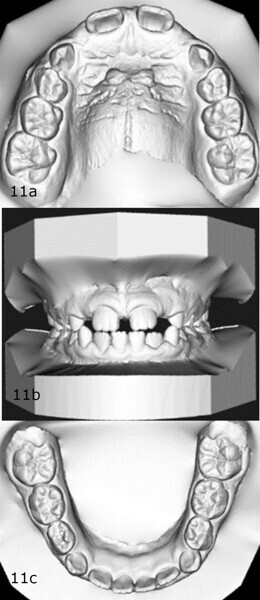
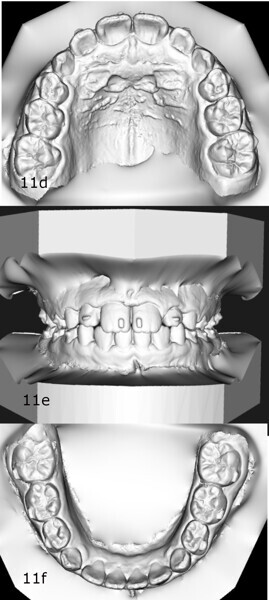
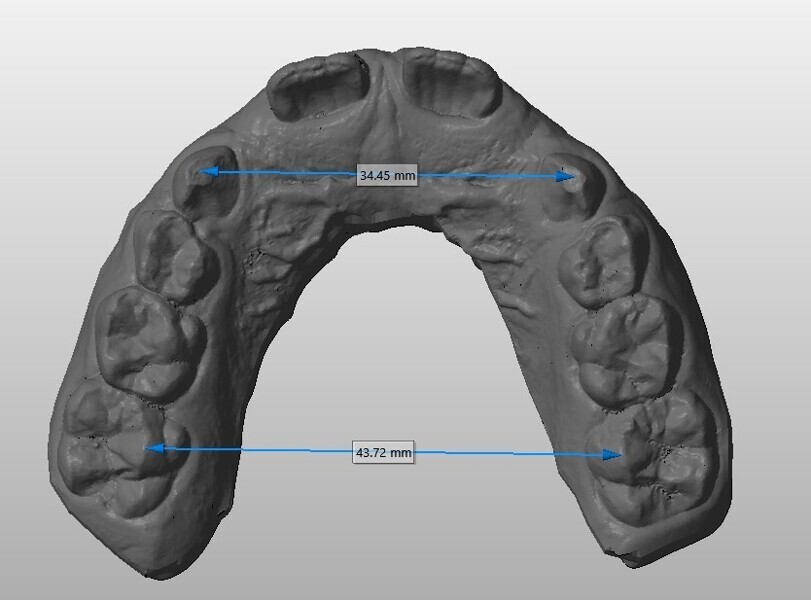
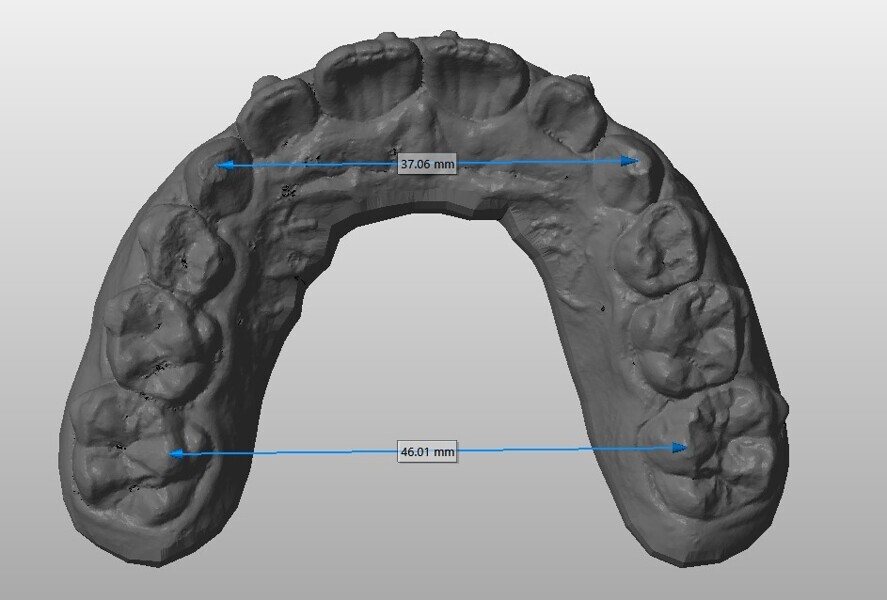
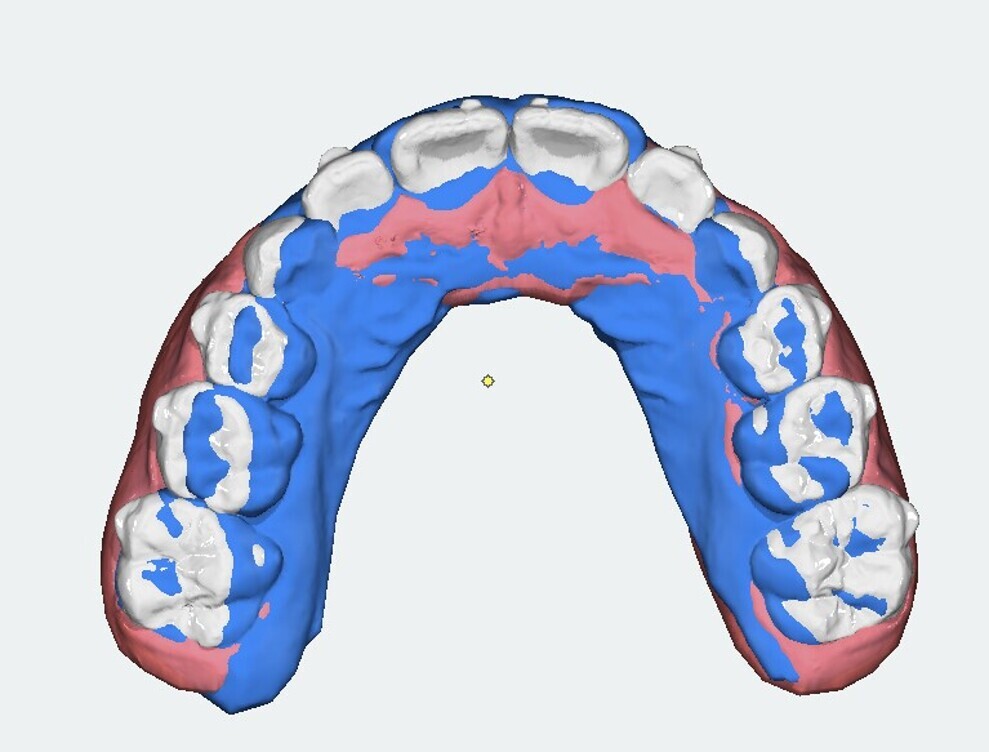
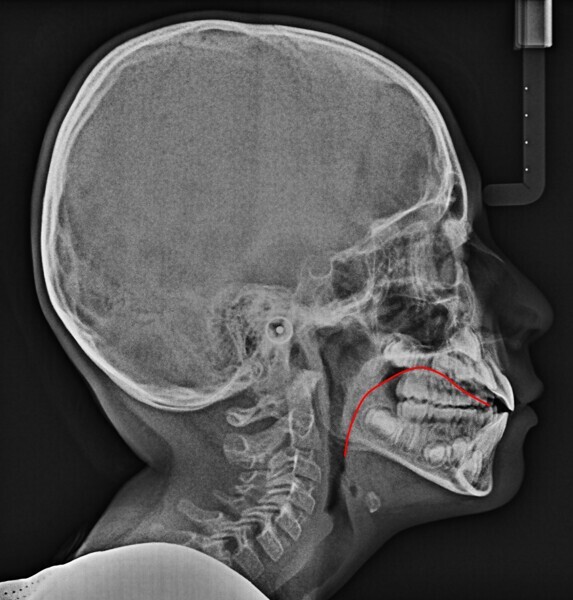
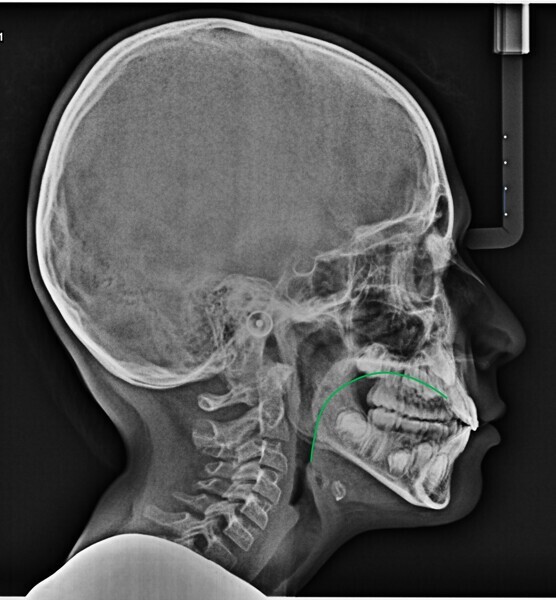
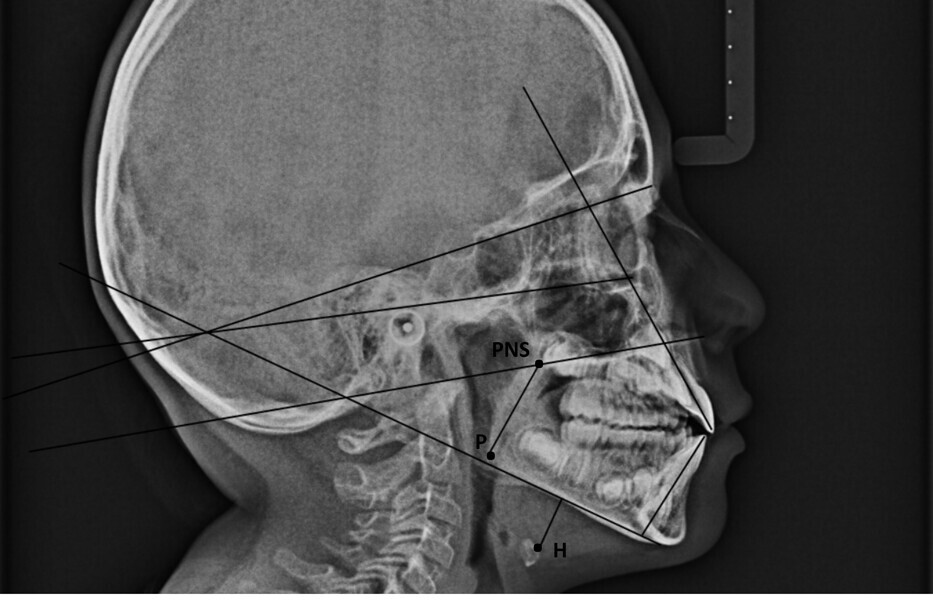
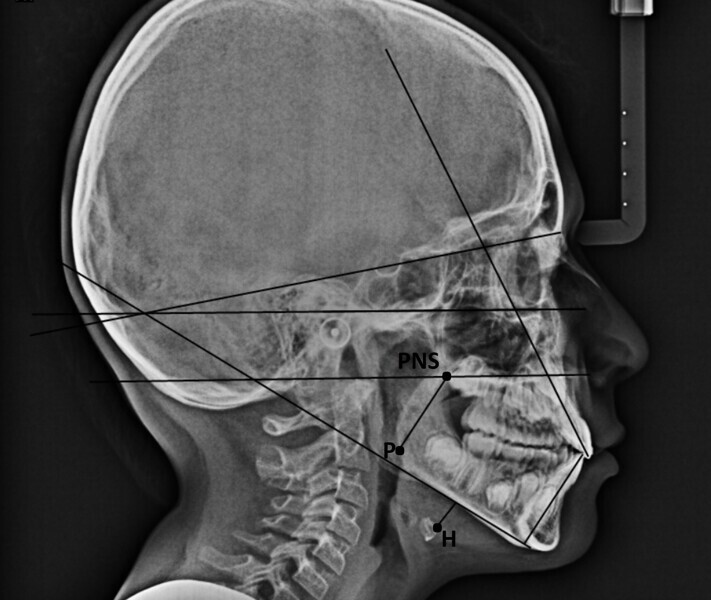
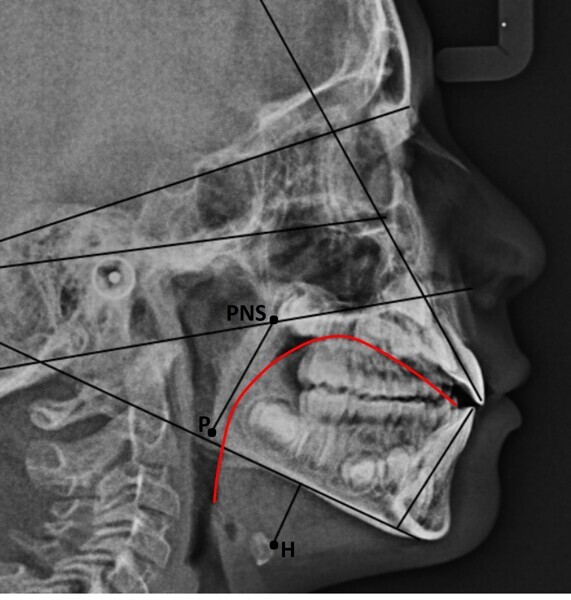
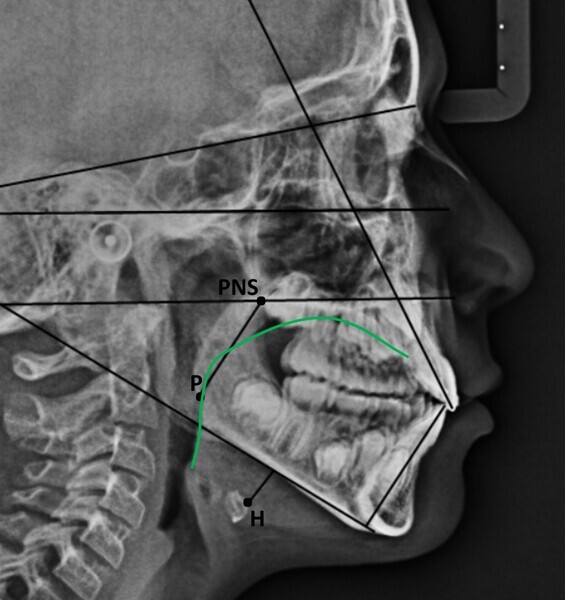
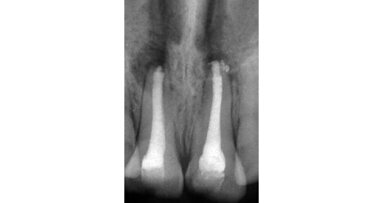
The 8-year-old male patient presented with a diastema between teeth #11 and 21 and non-eruption of teeth #12 and 22 (Fig. 1). The patient underwent a thorough orthodontic examination, including intra-oral photographs, extra-oral photographs, cephalometric radiography of the skull with cephalometric tracing, dental panoramic tomograms, impressions by intra-oral scanning, and functional and phonetic tests. Intra-oral examination (Fig. 2) and pattern analysis showed a Class I molar and canine relationship and contraction of the maxillary arch, displaced pre-contact between teeth #63 and 73, a 3.7 mm diastema between teeth #11 and 21, a mandibular midline deviation to the left, a maxillary midline to the right, and an open bite (−1.5 mm).
During the examination, the Payne test for fluorescein analysis of the lingual support on the palate was not performed because the large spacing between teeth would have affected it. However, the lingual frenulum18 was evaluated by calculating the tongue range of motion ratio for the tip of the tongue19 and with the tongue held in suction against the palate,20 obtaining a Grade 1 for both indices and thus excluding that the low tongue position was caused by a short frenulum. This evaluation is essential in all orthodontic patients, particularly paediatric patients.
Functional analysis showed oronasal breathing, a low tongue posture according to Artese et al. with anterior thrust,21 and consistently leftward-deviating mandibular movements, even in phonetic tests. In these tests, anterior lisp and gliding were present, in addition to lateralisation to the left for articulation.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





























To post a reply please login or register