Professional paradigm shift
If prevention is to be successfully integrated into everyday practice, a new systematic prevention protocol based on the state of the art in science and technological progress is required.
Scientific progress: Biofilm is a biological challenge
Today, the ecological plaque hypothesis according to Marsh is accepted worldwide as explaining the aetiology of the major oral diseases.5 According to this hypothesis, dysbiotic sub- and supragingival biofilm is the main cause of these diseases, which are caries, gingivitis, periodontitis, peri-implant mucositis and peri-implantitis.
A change in the environmental conditions from symbiosis to dysbiosis takes place in the biofilm. This ecological shift leads to a disturbance of homeostasis. Dental diseases are the result of the inflammatory host response to microbial biofilm. Because we know the cause of most oral diseases, there can only be one objective for dentistry: to preserve oral health lifelong. This objective can be achieved by combining individualised home and professional oral hygiene measures.6
Technological progress: Aids for biofilm management
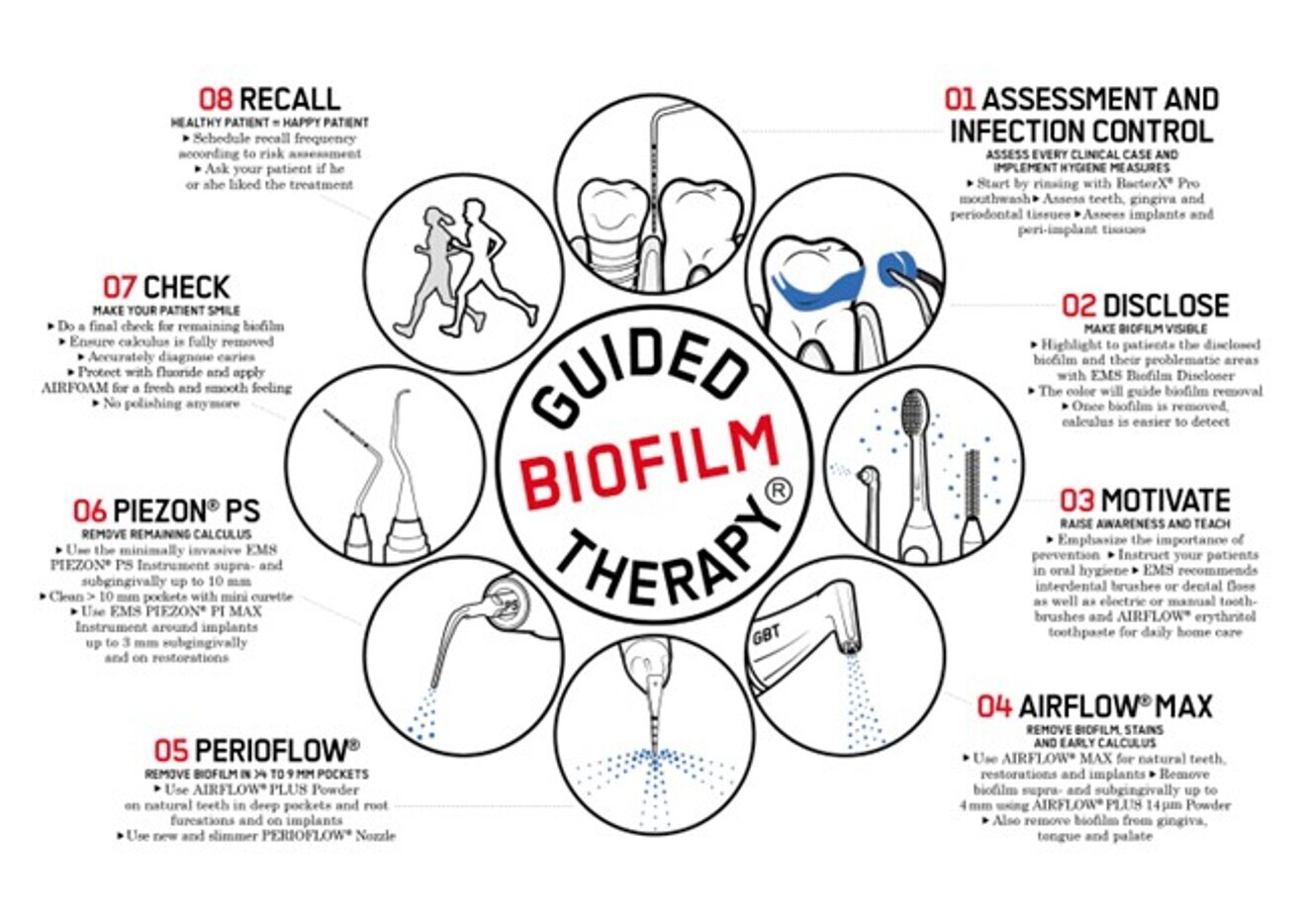
In general, we distinguish between home and professional biofilm management, and chemical and mechanical aids are available for both. Professional tooth cleaning or more precisely, professional mechanical plaque removal, is a central component of systematic prevention. Mechanical professional biofilm management can be performed with hand instruments such as scalers and curettes, with mechanical aids such as sonic scalers and ultrasonic scalers, with air–powder–water jet devices (air polishing and AIR-FLOWING; Fig. 1) and with rubber cup polishing. The terms “air polishing” and “AIR-FLOWING” are often used synonymously, but they differ considerably and must be distinguished from each other: both work according to the same principle of powder–water jet technology. AIR-FLOWING is a technically, physically and chemically coordinated system (AIRFLOW Prophylaxis Master device, AIRFLOW MAX handpiece, PERIOFLOW handpiece, minimally invasive erythritol-based AIRFLOW PLUS powder) and is the only system that operates with a constant and regulated powder flow rate and laminar flow.
For all aids, the same objectives apply: effective and targeted removal of biofilm, modification of biofilm, effective and targeted removal of dental calculus, preservation of the tooth substance, and patient and practitioner comfort. Comparison of the aids according to these objectives shows that AIR-FLOWING is superior to all other aids in effective targeted removal of supra- and subgingival biofilm.7–12 Recent work has shown that it is possible to modify biofilm and restore symbiosis with AIR-FLOWING and piezoceramic ultrasound (PIEZON NO PAIN technology and PS instrument).13, 14 Calculus can be removed more specifically and more effectively with piezoceramic ultrasound than with hand instruments.15–17 AIR-FLOWING and modern ultrasonic systems are also superior to hand instruments in terms of tooth substance preservation18–21 and practitioner22 and patient comfort.23–28



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East














































To post a reply please login or register