Dental crowns have been used for decades to restore compromised, heavily restored teeth, and for aesthetic improvements. New Computer Aided Design/Computer Aided Manufacturing (CAD/CAM) materials and systems have been developed and evolved in the last decade for fabrication of all-ceramic restorations. Dental CAD/CAM technology is gaining popularity because of its benefits in terms of time consuming, materials savings, standardisation of the fabrication process, and predictability of the restorations.
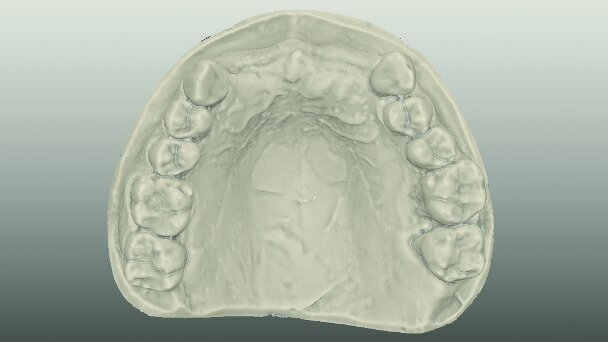
The number of steps required for the fabrication of a restoration is less compared to traditional methods (Fig. 1). Another benefit of CAD/CAM dentistry includes the use of new materials and data acquisition, which represents a non-destructive method of saving impressions, restorations and information that is saved in a computer and constitutes an extraordinary communication tool for evaluation.
The incorporation of dental technology has not only brought a new range of manufacturing methods and material options, but also some concerns about the processes involving restorations’ fit, quality, accuracy, short and long-term prognosis.[1]
The purpose of this document is to provide a review of the literature regarding the different materials and systems available up until 2015 in the USA.
CAD/CAM materials
Glass ceramics
The first in-office ceramic material was Vitablock Mark I (Vident); it was a feldspathic-based ceramic compressed into a block that was milled into a dental restoration. After the invention of the Mark I block, the next generation of materials for CAD/CAM milling fabrication of all-ceramic restorations were Vita Mark II (Vident) and Celay, which replaced the original Mark I in 1987 for fine feldspathic porcelains primarily composed of silica oxide and aluminum oxide.[2,3] Mark II blocks are fabricated from feldspathic porcelain particles embedded in a glass matrix and used for single unit restorations available in polychromatic blanks nowadays. On the other hand, Celay ceramic inlays have been considered clinically acceptable by traditional criteria for marginal fit evaluation.[4]
Dicor-MGC was a glass ceramic material composed of 70 percent tetrasilicic fluormica crystals precipitated in a glass matrix; but this material is no longer available on the market.[5] Studies from Isenberg et al. suggested that inlays of this type of ceramics were judged as clinically successful in a range from 3–5 years of clinical service.[6-8] In 1997, Paradigma MZ100 blocks (3M ESPE) were introduced as a highly filled ultrafine silica ceramic particles embedded in a resin matrix; the main advantage of this material is that it can be use as a milled dense composite that was free of polymerisation shrinkage but cannot be sintered or glazed.[9]
In early 1998, IPS ProCAD (Ivoclar Vivadent) was introduced as a leucite reinforced ceramic, which was similar to IPS Empress but with a finer particle size; this material was designed to be use with the CEREC system (Sirona Dental) and was available in different shades.[2] More recently, the introduction of IPS Empress CAD (Ivoclar Vivadent) and Paradigm C that according to the manufacturer (3M ESPE) is a 30 to 45 percent leucite reinforced glass ceramic with a fine particle size.[10]
To overcome esthetic problems of most CAD/CAM blocks having a monochromatic restoration, a different version was developed as a multicoloured ceramic block, which was called VITA TriLuxe (Vident) and also IPS Empress CAD Multiblock; the base of the block is a dark opaque layer, while the outer layer is more translucent; the CAD software allows the clinician to position or align the restoration into the block for the desired outcome of the restoration.[11,12]
In 2014, the Enamic (VITA) material was released as a ceramic network infi ltrated with a reinforcing polymer network that has the benefi ts of a ceramic and resin in one material, but no clinical data are available.[14]
Alumina-based ceramics
Alumina blocks (Vitablocs In-Ceram Alumina, VITA) are available for milling with the CEREC system (Sirona Dental) and now compatible with other milling machines as well. Due to the opacity of alumina- based ceramic materials, the In-Ceram Spinell (VITA) blocks were developed as an alternative for anterior aesthetic restorations; it is a mixture of alumina and magnesia. Its fl exural strength is less than In-Ceram Alumina, but veneering with feldspathic porcelain for a more esthetic result could follow it after the milling process.[14,15]
Nobel Biocare developed Procera material; for its fabrication high purity aluminum oxide is compacted onto an enlarged die that is fabricated from the scanned data.[16] The enlarged fabricated core shrinks to the dimensions of the working die when sintered at 1,550 °C; this material offers a very high strength core for all-ceramic restorations; the crown is finished with the application of feldspathic porcelain.[17] More recently, In-Coris AL (Sirona Dental) has been introduced as a high-strength aluminum oxide block with similar mechanical properties as Procera.[18]
Lithium disilicate
Lithium disilicate is composed of quartz, lithium dioxide, phosphor oxide, alumina, potassium oxide and other components. According to Saint-Jean (2014) the crystallization of lithium disilicate is heterogenous and can be achieved through a two or three stage process depending if the glass ceramic is intended to be used as a mill block (e-max CAD) or as a press ingot (e-max press). Lithium disilicate blocks (Fig. 3) are partially sintered and relatively soft; they are easier to mill and form to the desired restoration compared to fully sintered blocks; after this process the material is usually heated to 850 °C for 20 to 30 minutes to precipitate the final phase. This crystallization step is usually associated with a 0.2 percent shrinkage accounted for the designing software.[19] Nowadays, blocks of lithium disilicate are available for both in-office and in-laboratory fabrication of all-ceramic restorations; monolithic blocks require layering or staining to achieve good esthetic results.[8] Different in vitro studies that evaluate the marginal accuracy of milled lithium disilicate reveal that these restorations could be as accurate as 56 to 63 microns.[20]
According to the manufacturer specifications, the designing principles for lithium disilicate are produced by default in the designing software, but in full all-ceramic crowns structures the minimum thickness must be applied in the preparation design (Table I).
During the crystallisation process, the ceramic is converted from a lithium metasilicate crystal phase to lithium disilicate. Some commercial types of ceramics are Empress CAD (Ivoclar Vivadent) and IPS E-max. The first one is a leucite based glass ceramic with a composition similar to Empress ceramic. IPS E-max was introduced in 2006 as a material with a flexural strength of 360 to 400 MPa (two to three times stronger than glass ceramics); the blocks are blue in the partially crystallised state but it achieves the final shade after it is submitted to the firing process in a porcelain oven for 20 to 25 minutes to complete the crystallisation; the final result is a glass-ceramic with a fine grain size of approximately 1.5 μm and 70 percent crystal volume incorporated in a glass matrix.[20]
In 2014, Vident released Suprinity; the first ceramic reinforced with zirconia (10 percent weight); this material is a zirconia reinforced lithium silicate ceramic (ZLS) available in a precrystallized or fully crystallized (Suprinity FC) state indicated for all kind of single all-ceramic restorations.
Zirconia
Zirconia has been used in dentistry as a biomaterial for crown and bridge fabrications since 2004; it has been useful in the most posterior areas of the mouth where high occlusal forces are applied and there is limited interocclusal space.[22]
Zirconia is a polymorphic material that can have three different forms depending on the temperature: monoclinic at room temperature, tetragonal above 1,170 °C, and cubic beyond 2,370°C. According to Piconi (1999) ‘the phase transitions are reversible and free crystals are associated with volume expansion’. Different authors state that when zirconia is heated to a temperature between 1,470 °C and 2,010 °C and cooled, a volume shrinkage of 25 to 35 percent can occur that could affect marginal fit or passiveness of the restorations.[22] This feature limited the use of pure zirconia until 1970 when Rieth and Gupta developed the yttria-tetragonal zirconia polycrystal (Y-TZP) containing 2 to 3 percent mol-yttria in order to minimize this effect.[10]
One of the most interesting properties of zirconia is transformation toughening; Kelly (2008) describes it as: ‘A phenomenon that happens when a fracture takes place by the extension of an already existing defect in the material structure, with the tetragonal grain size and stabilizer, the stress concentration at the tip of the crack constitutes an energy source able to trigger the transformation of tetragonal lattice into the monoclinic phase’. This process dissipates part of the elastic energy that promotes progression of cracks in the restoration; there is a localized expansion of around 3.5 percent that increases the energy that opposes the crack propagation.[4]
Zirconia restorations can be fabricated from fully sintered zirconium oxide or partially sintered zirconium oxide blanks (green-state). Proponent of milling fully sintered zirconia claim that fitness of restorations is better because it avoid volumetric changes during the fabrication process. On the other hand, the partially sintered zirconia (Fig. 4) is easier and faster to mill and proponents of milling partially sintered blanks claim that micro cracks can be induced to the restoration during the milling process and it also requires more time and intensive milling processes; this micro defects or surface flaws can affect the final strength of the final restoration and could potentially chip the marginal areas; however further research is needed about this topic.[10]
One of the first systems that used zirconia was In-Ceram Zirconia (Vident), which is a modification of the In-Ceram Alumina but with the addition of partially stabilised zirconia oxide to the composition. Recently many companies have integrated zirconia into their CAD/CAM workflow due to its mechanical properties, which are attractive for restorative dentistry; some of these properties are: high mechanical strength, fracture toughness, radiopacity for marginal integrity evaluation, and relatively high esthetics.[13,14]
Different manufacturers are using zirconia as one of their main materials such as: Ceramill Zolid (Amann Girbach), Prettau (Zirkonzahn), Cercon (DENTSPLY), BruxZir (Glidewell Laboratories), IPS ZirCAD (Ivoclar Vivadent), Zenostar (Ivoclar Vivadent), inCoris ZI (Sirona Dental), VITA In-Ceram YZ (Vident), among others. Companies have introduced materials that are in combination with zirconia to improve its properties in different clinical situations. Lava Plus, for example, is a combination of zirconia and a nano-ceramic.
CAD/CAM systems
A number of different manufacturers are providing CAD/CAM systems that generally consist of a scanner, design computer and a milling machine or 3-D printer. Laboratories are able to receive digital impression files from dentists or use a scanner to create digital models that are used for restorations designing or CAD. Dental scanners vary in speed and accuracy. Milling machines vary in size, speed, axes, and also in which restorative materials can be milled; in this category milling machines could be classified as wet or dry depending if the materials require irrigation.
The development of dental CAD/CAM systems occurred around 1980 with the introduction of the Sopha system developed by Dr. Francois Duret. A few years after that event, Dr. Werner Mörmann and the electrical engineer Marco Brandestini developed the CEREC-1 system in 1983, the first full digital dental system created to allow dentists to design and fabricate in-office restorations. Since then, the continuous evolution of systems dedicated to this field has continued and has exponentially increased in the last decade.[14]
CEREC systems has evolved into CEREC Bluecam scanner;accuracies as close as 17 microns for a single tooth have been reported by authors using this system. Recently CEREC Omnicam was introduced offering true colour digital impressions without the need of a contrast medium. In a recent study by Neves et al. (2013) on the marginal fit of CAD/CAM restorations fabricated with CEREC Bluecam, they compared lithium disilicate single unit restorations to heat-pressed restorations and 83.8 percent of the specimens had a vertical gap measurement with less or at least 75 microns.[15]
The CEREC InLab CAD software (Sirona Dental) was designed for dental laboratories for a wide range of dental capabilities that can be combined with third party systems. With this software, the dental technician is able to scan their own models using Sirona inEos X5 (Sirona Dental) scanner and design the restoration; once this process is completed, the file can be sent to a remote milling machine or a milling centre for fabrication in a wide range of materials.
The Procera system, introduced in 1994, was the first system to provide fabrication of a restoration using a network connection. According to research data the average ranges of marginal fit of this restorations are from 54 to 64 microns.[20] A computer integrated crown reconstruction system (CICERO) introduced by Denison et al. in 1999 included a rapid custom fabrication of high-strength alumina coping and semifinished crowns to be delivered to dental laboratories for porcelain layering and finishing.[15]
Another system that was developed years ago was the Celay system, which fabricated feldpathic restorations through a copy-milling process. The system duplicated an acrylic resin pattern replica of a restoration. Zirkonzahn developed a similar system called the Zirkograph in 2003, which was able to copy-mill zirconia prosthesis and restorations out of a replica of the restoration. Some years after, the Cercon system (DENTSPLY Ceramco) was able to design and mill zirconia restorations out of a wax pattern.[1]
Almost at the same time that these companies developed the first copy mill prototypes, Lava (3M ESPE) introduced in 2002 the fabrication of yttria-tetragonal zirconia polycrystal (Y-TZP) cores and frameworks for all ceramic restorations. With the Lava system, the die is scanned by an optical process, the CAD software designs and enlarge the restoration or framework that is milled from a pre-sintered blank. Studies on marginal adaptation suggest that Lava restorations have a marginal fit that can be as low as 21 microns.[27] Some other systems that were able to mill zirconia were DCS Zirkon(DCS Dental) and Denzir.[16]
In the last decade, companies have decided to differentiate their products by having a full CAD/CAM platform or by focusing on specific areas of expertise like CAD software and intraoral scanners; these companies claim to be open platform because their systems allow to export universal files such as STL or OBJ (Fig. 5) to be used with the majority of nesting softwares and milling machines that are able to import them.
Defenders of closed platforms claim that the integration of different CAD/CAM systems does not allow for a good integration between parts and probably leads to the incorporation of fabrication errors; at this point no research about systems integration is available. Table II shows some of the systems used for dental CAD with their file output; Table III shows some of the most used CAM systems with their material recommendations and capabilities.
Some of the main concerns from clinicians about all-ceramic CAD/CAM restorations accuracy of fit are: scanning resolution, software designing limitations, and milling hardware limitations of accuracy. Clinicians’ and technicians’ experience with the CAM/CAM system integration is also a key factor for fabricating good restoration; the computer software per se will not allow an inexperienced operator to create an excellent dental restoration from scratch.[18]
Discussion
Several advantages can be drawn from including CAD/CAM dental technology, 3-D scanning and the use of mill materials for all-ceramic restorations. Even though clinical studies have shown that marginal fit of CAD/CAM restorations is compared to conventional restorations the fabrication of dental restorations is still a complex task that requires experience, knowledge and skills.
The incorporation of new systems and materials bring a lot of concerns regarding system implementation, capabilities and mechanical properties of the different materials. One of the biggest problems that still remain in CAD/CAM dental systems is the accuracy of each step in the CAD/CAM chain, from digital impression to the milling step. Using computer aided manufacturing is dependent on the calibration of hardware with software in the workflow. Furthermore, the virtual configuration of the die spacer between the tooth and the restorations is essential for the accuracy of the marginal adaptation and has to be calibrated for each one of the systems. Weittstein et al. demonstrated that the difference of fit between CAD/ CAM restorations is directly related to the gap parameters from the computer design and also related to the intrinsic properties of the CAD/CAM system.[16]
Conclusion
This review of current and past literature regarding the evolution, characteristics, and marginal fit of milled CAD/CAM all-ceramic restorations materials and systems show that it is possible to fabricate restorations with the same marginal fit expected from conventional methods and within the range of clinically accepted restorations. When comparing both methods the advantage of using CAD/CAM technology is not to obtain the most precise level of fit, but rather to obtain a high level of reliability in a large number of restorations; especially when high production levels are expected. However, there are a limited number of clinical studies and the diversity of the results between systems and protocols does not allow us to give a definitive conclusion.
Editorial note: A full list of references can be requested from the publisher. This article was published in CAD/CAM international magazine of digital dentistry No. 03/2016.
Dr Alexandra Papanikolaou owns a private dental clinic in Athens in Greece, focused mainly on restorative and aesthetic dentistry. In an upcoming webinar, ...
SCHAAN, Liechtenstein: The Ivoclar Group, a leading manufacturer of integrated solutions for high-quality dental applications, and MALO ...
AMMERBUCH, Germany: The Ivoclar Group, a global provider of integrated solutions for high-quality dental care, and vhf camfacture, a leading manufacturer of...
SCHAAN, Liechtenstein: Ivoclar revolutionised the fabrication of complete dentures two years ago with the introduction of the Ivotion Denture System, which ...
COPENHAGEN, Denmark: 3Shape and Ivoclar Vivadent have announced a new collaboration that enables orthodontists, dentists, and laboratory professionals to ...
SCHAAN, Liechtenstein: Adhese 2 is the latest addition to Ivoclar’s portfolio of adhesives and is designed to improve flexibility and efficiency in ...
SCHAAN, Liechtenstein: Ivoclar has introduced IPS e.max Ceram Art, a ready-to-use line of stain, glaze and structure pastes for the customisation of ceramic...
SCHAAN, Liechtensein: Adequate moisture control and unobstructed access to the treatment area are essential requirements for successful dental treatments. ...
SCHAAN, Liechtenstein: Digital technologies and processes are constantly driving changes in the dental industry and have a major impact on the way dental ...
In a rapidly evolving dental landscape shaped by digitalisation, artificial intelligence and rising patient expectations, Ivoclar continues to focus on ...
Dr. Maximilian Dobbertin M.Sc
Dr. med. dent. Simona-Georgiana Schick



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East









































where are the refernces plz