Oral surgery is an important cornerstone in orthodontic treatment of malocclusions. Tooth movement is only possible to a limited extent and always depends on the misalignment of the maxilla and mandible in relation to each other, as well as on deformities of the jaw in relation to the other facial bones.
Abnormalities may be congenital or acquired and may affect patients in childhood already. If so, the focus of orthodontic treatment is not primarily in the aesthetic correction, but is guided by functional and prophylactic concerns. Efficient occlusion and restoration of masticatory function are decisive factors for tooth preservation and prevention of secondary disorders (Figs. 1a–c). Without a doubt, aesthetic improvement, as well as the associated self-consciousness, is the main concern of most patients, which can be pursued through surgical correction.
Causes of malocclusion
Generally, patients visit an orthodontic practice only after symptoms or significant abnormalities have already presented. Clinically, this results in late mixed dentition or permanent dentition, which can complicate an accurate mapping of the reasons for this malocclusion. In the literature, the causes of malocclusion and the aetiological structure of the symptoms of malocclusion in orthodontic patients are controversial issues. No explicit information on the percentage of patients with acquired or congenital malocclusions can be found in a study by Schopf (1981) on the exogenous factors that are involved in the development of malocclusion. However, from the assessment of individual patients’ symptoms, all symptoms of malocclusion could be associated with exogenous aetiological factors only in 48% of patients. Brodmann and Saekel (2001) concluded from Schopf’s report that only 20% of the anomalies were hereditary and thus could not be affected by prophylactic interventions. Accordingly, 80% of malocclusions could be resolved through prevention and better oral hygiene. This idea is contrary to the results of the German Oral Health Study. In this study, a decrease in childhood caries was observed. However, clinically these results were not associated with a lower rate of and need for orthodontic treatment. The study at the University of Greifswald, Germany, found that 20.3% of the symptoms were genetically determined, 44.3% were exogenous and 35.3% were not precisely defined. Based on these results, the assumption that 80% of malocclusions can be resolved by prevention and better oral hygiene is very questionable (Hensel, DGKFO opinion, 2001).
embedImagecenter("Imagecenter_1_670",670, "large");
The varying findings and remarks illustrate the difficulty of clear classification of malocclusion. Nonetheless, the demands of the patient have priority and he expects a symptom-based therapy with stable treatment results. This means that in malocclusion cases that cannot be resolved by functional orthodontics solely, orthodontic–surgical planning can be done before any treatment is attempted by pure dentoalveolar compensatory intervention. Compensatory dentoalveolar procedures could prevent a surgical operation. At the same time, patients may run the risk of protracted treatment without any long-lasting benefit. The decision for or against orthopaedic surgery requires interdisciplinary agreement and reliable treatment goals must be defined in advance (Figs. 2a & b).
Target group for orthopaedic surgery
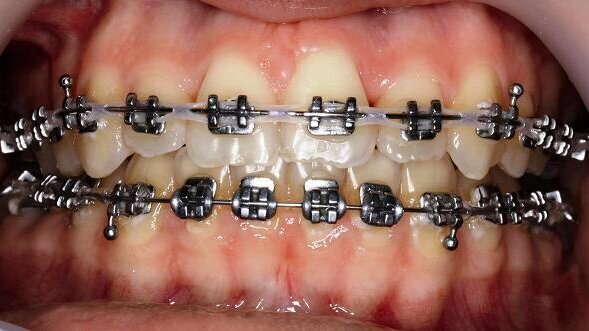
Nowadays, adults make up the majority of patients in the orthodontic practice. They are generally motivated by high socio-cultural demands and the desire for perfect teeth. In adults who have an obvious discrepancy between their maxilla and mandible, it must be clarified whether the deformities are dentoalveolar or skeletal. Owing to the limitations of conventional orthodontic treatment, skeletal discrepancies can rarely be entirely resolved. In those cases, combined orthodontic–surgical treatment is necessary. During growth, it is mostly possible to treat malocclusions successfully without surgery by purely orthodontic treatment using removable appliances or brackets.
Children and young people for whom functional orthodontic treatment has not led to the desired result are treated surgically after the growth period. Early surgery always carries the risk of unexpected growth pattern or unilateral abnormal hyperplasia and can affect the results of the operation.
Selection of patients
Combined orthodontic–surgical treatment requires not only strong and focused interdisciplinary collaboration, but also absolute acceptance of the treatment plan by patients and parents. The treatment is time-consuming and post-operative corrections cannot be excluded. A detailed medical preoperative discussion should inform patients about the risks of combined treatment and the consequences of untreated malocclusions. Malocclusions can cause numerous side-effects, such as back pain and chronic headaches (Figs. 3a & b). In markedly dolichofacial face types, malocclusions can lead to a pharyngeal constriction, which can manifest as obstructive sleep apnoea syndrome (Hochban et al. 1997).
In adult patients, it is normally useful to determine the amount of malocclusion and force bite using a flat-plane bite splint. The splint is worn for six to eight weeks, and guarantees the identification of the physiological condylar position. Pursuing orthodontic correction depends on the intended post-operative situation. Therefore, such correction is only dentoalveolar and does not transfer bite forces (Figs. 4a–c & 5a–e). The most favourable position of the maxilla and mandible is assessed on the basis of simulated cast surgery in which the amount of shift is determined. Using these casts, a splint can be fabricated and placed during surgery to fix the determined physiological condylar position preoperatively (Figs. 6a–c).
Teenagers with mandibular asymmetry that cannot be clearly classified should be treated with special care. Should clinical records be available only from the age of 16—whether as a result of erroneous dental records or simply owing to late initial assessment in a specialised practice—accurate early diagnosis of potential unilateral hyperplasia with further growth tendency is essential. According to the German Society of Oral and Maxillofacial Surgery guidelines, a nuclear medicine diagnostic is necessary—in addition to inspection, palpation and radiography—to determine the risk of an abnormal growth in time. Through increased uptake in the affected region during scintigraphy, it is possible to draw conclusions about the growth’s behaviour. If the jaw continues to change by abnormal bursts of growth, it is advisable to postpone surgical therapy until the cessation of growth.
Surgical technique
The choice of technique for the osteotomy depends on various factors. In displacement osteotomy, surgical access to the bone is created, which is split at fixed points. Correction of the bone and bone healing in the new fixed position is accomplished using simulated cast surgery and a fabricated splint. Following surgical modification of the jaw area, it is important to consider the correct position of the jaw and optimal occlusion. This crucial step has to be performed by the orthodontist as accurately as possible because repositioning and the degree of displacement of the jaw depend on achievable occlusion. Furthermore, teeth have an influence on access to the surgical field and wisdom teeth must be removed before osteotomy in certain cases.
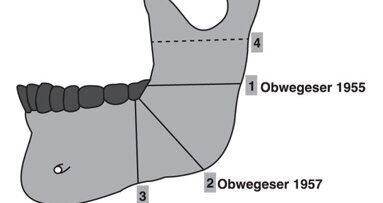
Osteotomy can be done on both jaws or can be limited to the maxilla or mandible. However, in many cases it is functional to perform bimaxillary osteotomy and to shift both jaws. Today, generally the entire tooth-bearing portions of the jaw are shifted. Segmental osteotomy has not been proven to be very successful in the past and corrections of malocclusions are left to the orthodontic treatment partners. In this field of treatment, the Obwegeser–Dal Pont surgical technique is recommended. This procedure describes an intra-oral stepped osteotomy at the mandibular ramus (Figs. 7a & b). Since Bell and Epker described the possibility of bimaxillary surgery as the “down fracture” technique in 1975, it has been popular and today you can find it mostly as a combination of Obwegeser–Dal Pont and Le Fort I osteotomy. The bimaxillary approach seems reasonable, since the maxilla and mandible influence each other during growth. However, it is frequently only possible to obtain a very good and risk-free result by using Obwegeser–Dal Pont surgery. Fixation in split osteotomy of the mandible is usually realised by using minimally invasive plate osteosynthesis. In modified techniques of Obwegeser–Dal Pont surgery, a displaced ramus is fixed using osteosynthesis screws only (Hochban 1997; Figs. 8a & b). This modification avoids the complicated surgical removal of osteosynthesis plates.
Operation risk
Any surgical procedure can lead to unexpected complications, which must always be considered according to the risk–benefit principle. Today, the need for osteotomy remains controversial because a jaw deformity is not a serious illness like a tumour, abscess or bone fracture, which is necessarily treated by surgery. Since deformities are often aesthetic corrections and can be classified as elective procedures, operation safety is a chief concern. Isolated osteotomies of the mandible, which present a significantly lower surgery risk, should be the first choice for orthodontic–surgical interventions.
The most significant risk of osteotomy of the mandible is a probability of about 5% of damaging the sensory nerve, called the inferior alveolar nerve. This can cause sensibility problems of the lower lip and chin area (Figs. 9a–c). Additional serious risks are not expected using Obwegeser–Dal Pont surgery and post-operative bleeding can be controlled very safely.
Interdisciplinary collaboration
The literature review of work done in the 1970s makes clear that today’s conscientious collaboration between surgeons and orthodontists is not a matter of course. Over the years, orthognathic surgery was considered to be the last option for treating orthodontic cases that could not be resolved using standard treatment techniques. Therefore, operations were carried out based on tolerance of dentoalveolar compensation and likely made further corrective surgery more probable.
Today, in almost all cases of malocclusion, orthodontic treatment is preceded by surgical treatment. Nowadays, the planning of the operation based on simulated cast surgery and the creation of a splint is a very safe method by which to achieve predictable and stable long-term results (Figs. 10a & b). Individual dentoalveolar discrepancies in occlusion can be corrected preoperatively or post-operatively by orthodontic treatment. Therefore, interdisciplinary collaboration is always a benefit for the patient and treatment team.
Editorial note: This article was published in the 02/2012 issue of the cosmetic dentistry international magazine.
Orthodontic treatment generally follows aesthetic, functional, and prophylactic objectives, where individual aspects of isolated cases are accorded varying ...
While growing up, I always enjoyed brain teasers. When my career in orthodontics began, I was intrigued because everything seemed like a puzzle. While ...
BEIJING, China: When the largest Chinese clear aligner manufacturer floated shares on the Hong Kong stock exchange in June, it was obliged to make available...
AMMAN, Jordan: Dental and facial aesthetics do more than shape a smile; they can influence how individuals perform socially and academically, according to ...
Faced by a missing lateral incisor, practitioners often consider a wide range of issues and are also faced by numerous treatment options:
1. in a young ...
CHIA, Italy: “Focus on New Visions in Dentistry” is the theme at the 10th International Dental Congress and will take place in Chia in Sardinia on ...
With greater public awareness about cosmetic dental reconstructions, the dentist is often challenged with greater demands from the patient. This increased ...
MALSCH, Germany: A concern regarding digitalisation is that it is linked to the risk of important professional disciplines losing significance in the public...
Dentists today are living during exciting times when advancements in materials, techniques and diagnostics allow us to predictably improve the quality of ...
LONDON, UK: Align Technology launched its 2021 Digital Excellence Series on 19 May with a live step-by-step demonstration of an end-to-end restorative ...
Live webinar
Tue. 26 May 2026
12:00 pm EST (New York)
Live webinar
Tue. 26 May 2026
2:00 pm EST (New York)
Live webinar
Wed. 27 May 2026
8:00 am EST (New York)
Live webinar
Thu. 28 May 2026
12:00 pm EST (New York)
Dr. Anthony Viazis DDS, MS. Inventor & Founder of Fastbraces®
Live webinar
Mon. 1 June 2026
1:00 pm EST (New York)
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East

































To post a reply please login or register