With greater public awareness about cosmetic dental reconstructions, the dentist is often challenged with greater demands from the patient. This increased demand for aesthetic restorative treatment challenges the dentist, laboratory technician and dental manufacturers to develop techniques and materials to satisfy the discerning patient. Utilising digital planning, modern materials and effective techniques, the restorative team can succeed in restoring a smile to proper form, function and health. The case presented in this article demonstrates the significance of a systematic approach to planning, preparation and material selection in full-mouth reconstruction of a patient’s dentition.
Case presentation
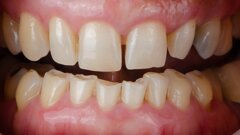
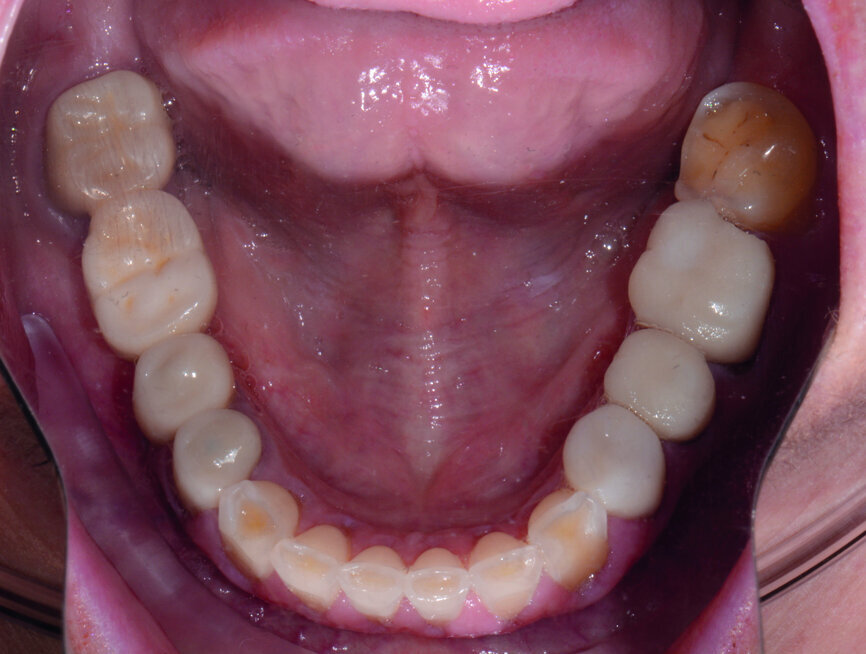
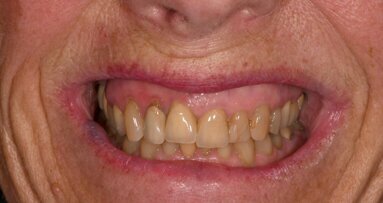
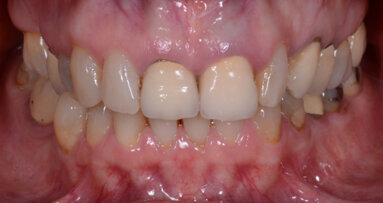
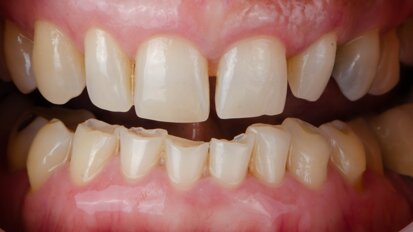
A woman in her early forties was referred to my practice by her dental provider because she was dissatisfied with the appearance of her smile. The patient explained that she felt that her existing teeth and restorations were unattractive because of recurrent caries, wear and colour (Fig. 1). Most importantly, she mentioned that she was suffering from tension headaches, grinding and a limited range of function.
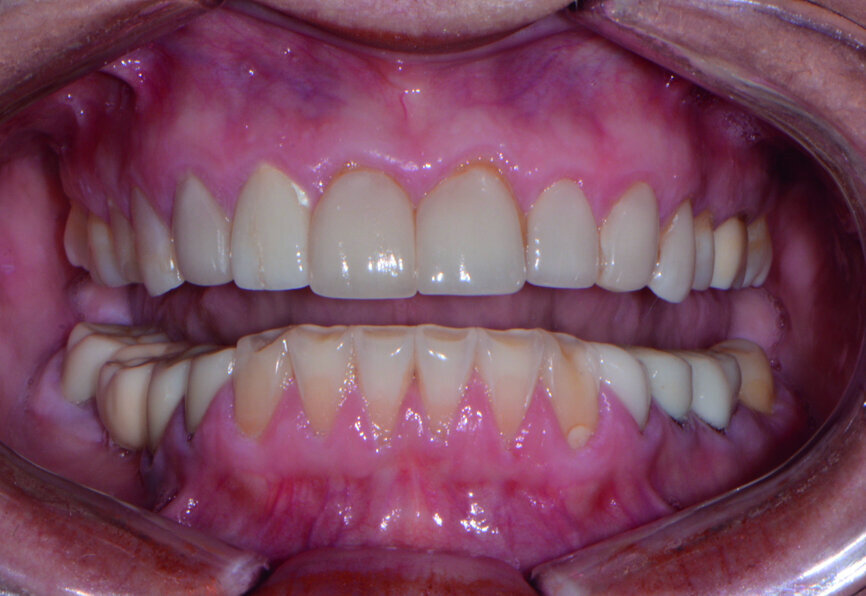
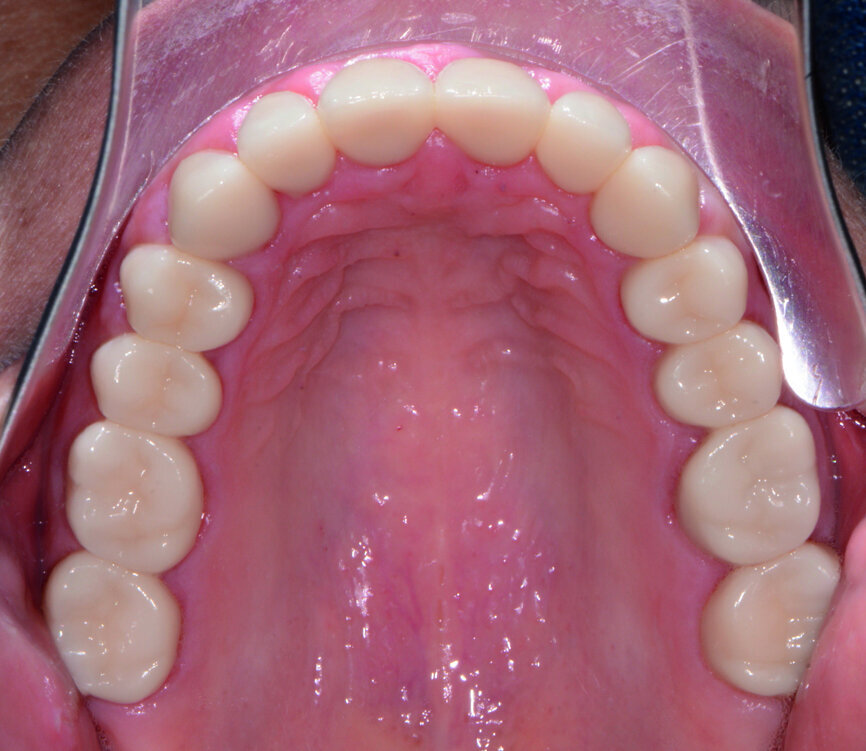
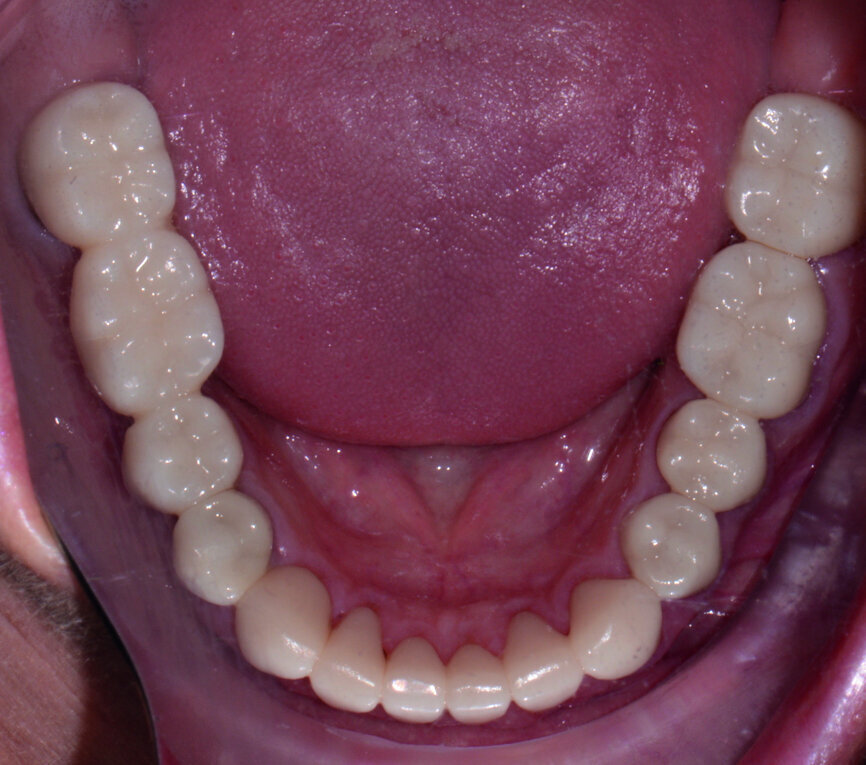
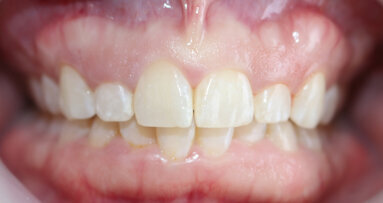
Fig. 10: Post-op retracted view.
Fig. 11: Post-op retracted view.
Fig. 12: Post-op retracted view.
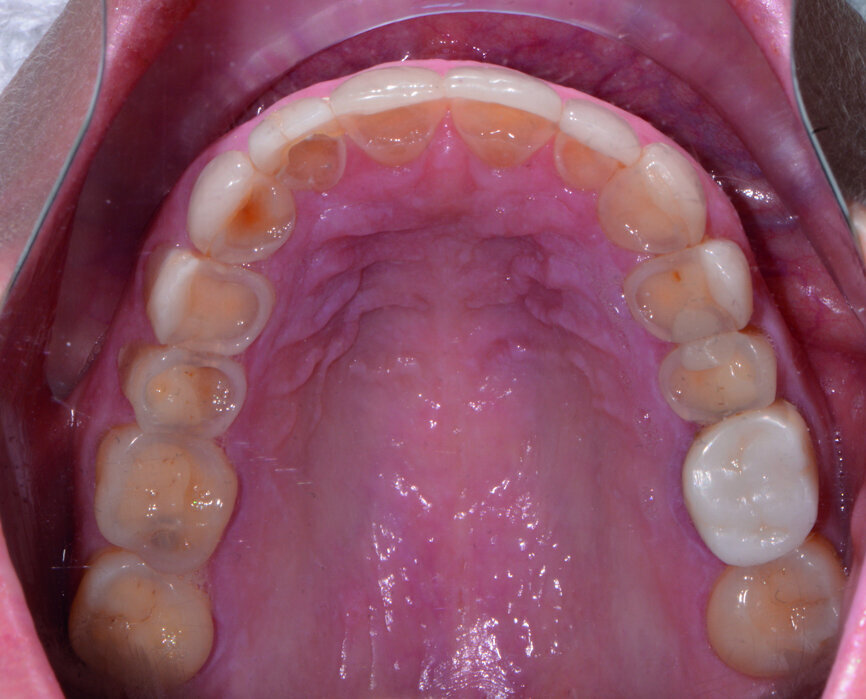
Initial diagnostic evaluation at the first appointment consisted of a series of digital images with study casts, a centric relation bite record, a facebow transfer and a full-mouth set of radiographs. In the maxillary arch, the patient had several teeth with worn composite and veneer restorations, as well as abfractions with cervical caries. In the lower arch, several existing composite restorations had worn and exhibited caries on the facial cervical areas. Although there were no restorations present in the mandibular anterior teeth, there was severe wear of the incisal edges, possibly due to grinding and other parafunction.
Planning
After reviewing the clinical findings and the mounted models, the patient was diagnosed with a restricted envelope of function and decreased vertical dimension from continuous wear. In order to develop a treatment plan and determine whether the vertical dimension could be increased, a diagnostic 3-D White Wax-Up (Arrowhead Dental Laboratory) was fabricated (Fig. 4).
In the wax-up, the vertical dimension was increased by 1.5 mm. Also, based on information gathered from the initial consultation and digital images, it was determined that the maxillary central incisors could be lengthened by 1.3 mm to improve the aesthetics. The canines would also be lengthened to restore canine guidance in lateral excursions. Regarding the mandibular anterior teeth, the goal was to correct the length-to-width ratio and createa less worn appearance.
As a result of the information gathered from the diagnostic wax-up, it was determined that aesthetics and function could be enhanced by restoring the entire dentition. The final treatment plan would consist of crown restorations, placing composite cores where needed from teeth #17–27 in the upper arch and teeth #37–46 in the lower arch.
The material of choice for these crown restorations would be Zenostar (Wieland/Ivoclar Vivadent). According to the manufacturer, this translucent zirconia material combines excellent flexural strength with the aesthetics of natural tooth shades.
With full-contour Zenostar restorations, there are two methods of achieving the desired shade: the Zenostar brush infiltration technique or the Zenostar staining technique. Six pre-shaded zirconia blanks—pure, light, medium, intense, sun and sun chroma—form the basis for reproducing the patient’s natural dentition. Owing to their warm, reddish nuance, Zenostar Zr Translucent sun and sun chroma are suitable for restorations with individual colour characterisation and can therefore be used for patients whose own natural dentition deviates from the classical tooth shades.
Preparation
Once informed consent had been obtained from the patient, treatment was initiated.
After anaesthetic had been administered, the existing veneer and crown restorations were removed and the teeth cored with composite if there was any indication of recurrent caries remaining in the respective tooth.
Adhese Universal bonding agent (Ivoclar Vivadent) was applied following the manufacturer’s protocol and cured using the Bluephase LED curing light (Ivoclar Vivadent). Using MultiCore Flow Light (Ivoclar Vivadent), build-ups were accomplished on the teeth that required cores. A Clear Reduction Guide (Arrowhead Dental Laboratory) provided with the White Wax-Up was used to ensure adequate reduction for the definitive restorations. Using a coarse-grit chamfer diamond bur (Komet), the entire dentition was prepared for Zenostar crowns, starting from teeth #17–27 and then teeth #37–46.
A full-arch impression was taken using Instant Custom Trays (Good Fit). Made of a proprietary material (PMMA) that becomes mouldable when heated in boiling water, these trays provide a quick, efficient way of capturing a dimensionally accurate impression with uniform thickness of the impression material.
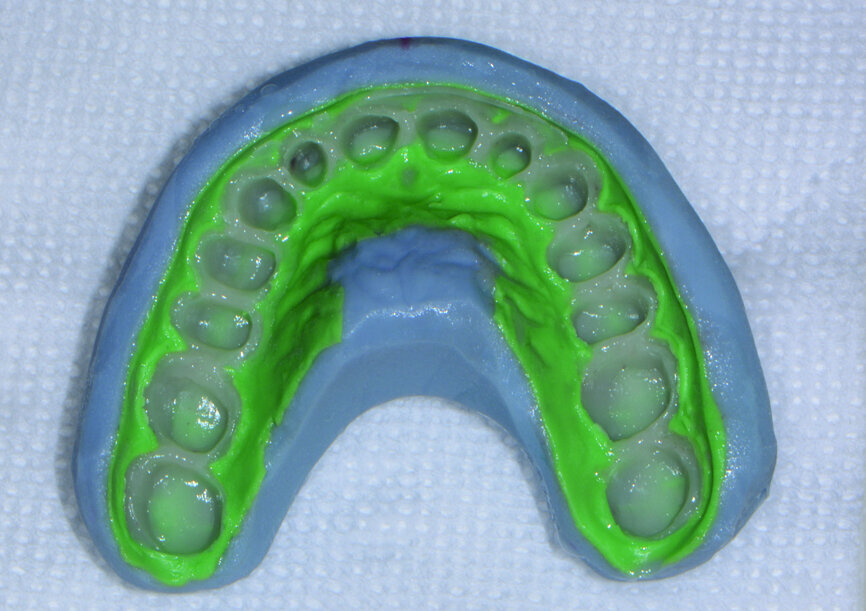
Once moulded and customised to the patient’s maxilla and mandible, full-arch impressions were taken using a heavy and light polyvinylsiloxane impression material (Panasil, Kettenbach).
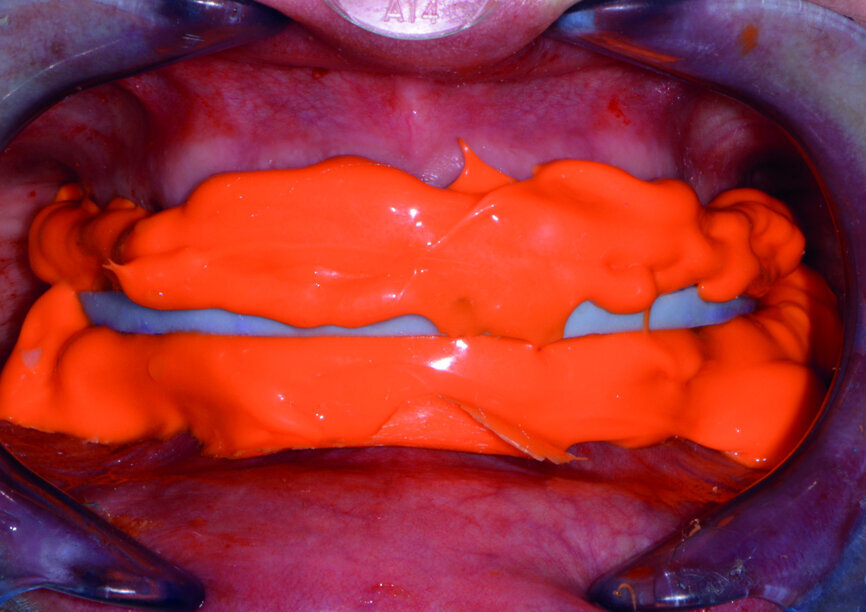
After the impressions had been completed, a bite relation jig fabricated on the White Wax-Up models was tried in the mouth. Medium-body impression material (Panasil) was placed into the relation jig and seated in the patient’s mouth on to the prepared teeth (Figs. 5 & 6).
The patient was asked to bite into the relation jig until she reached the vertical stops and the material set. Instruc tions for the size shape and colour of the final restorations was forwarded to the dental laboratory (Arrowhead Dental Laboratory), as were the White Wax-Up models. Also, a stump shade (Ivoclar Vivadent) was selected for shade matching of the preparations to assist the laboratory technician in creating natural-looking restorations.
Provisionalisation
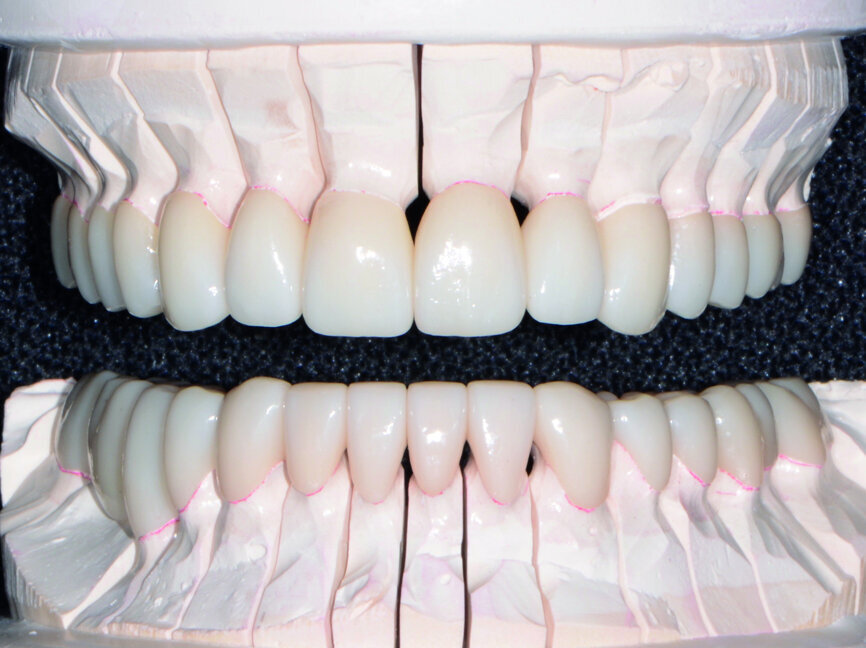
Provisional restorations, which would aid in determining the best size, shape, colour and position for the definitive restorations, were made from Sil-Tech (Ivoclar Vivadent) impressions of the White Wax-Ups provided by the dental laboratory.
Using the B1 shade of Visalys Temp (Kettenbach), the Sil-Tech mould was quickly filled and placed on the patient’s prepared dentition. Within minutes, the provisional restorations were fabricated and effortlessly trimmed with trimming burs (Komet). Once the teeth had been desensitised with Systemp.desensitizer (Ivoclar Vivadent) and dried, the provisional restorations were temporarily cemented using Temp-Bond Clear (Kerr). The patient was instructed about their care and use in eating, speaking and biting.
A few weeks later, the patient returned for evaluation of aesthetics, phonetics and bite. Already, she exhibited excitement about and confidence with her provisional restorations, commenting that all her co-workers had remarked that she looked younger and happier.
Most importantly, the patient said that she no longer experienced discomfort in her temporomandibular joint and that her bite had never felt better. Since no adjustment or modification of the temporary was needed, the dental laboratory was instructed to replicate the White Wax-Up when fabricating the definitive restorations.
Laboratory considerations
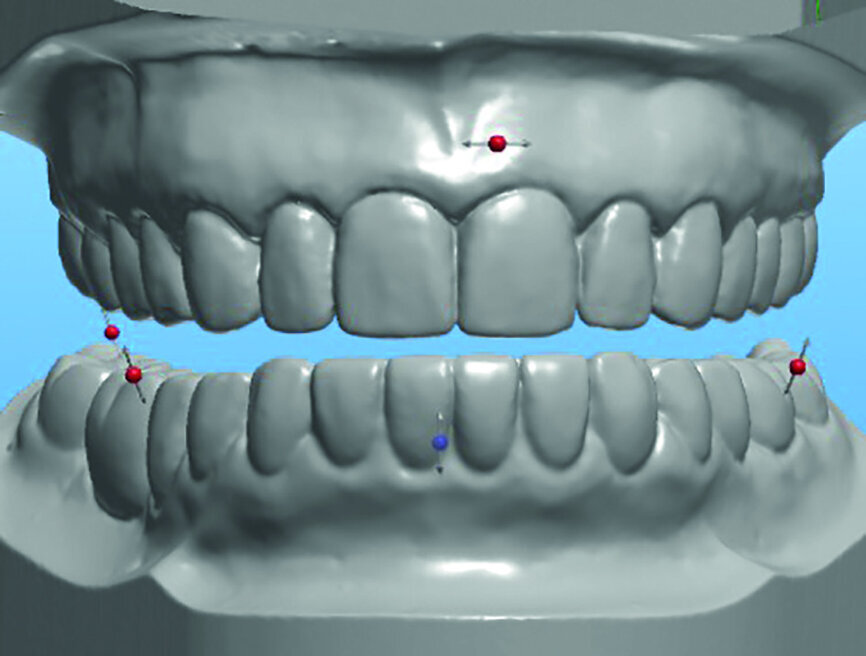
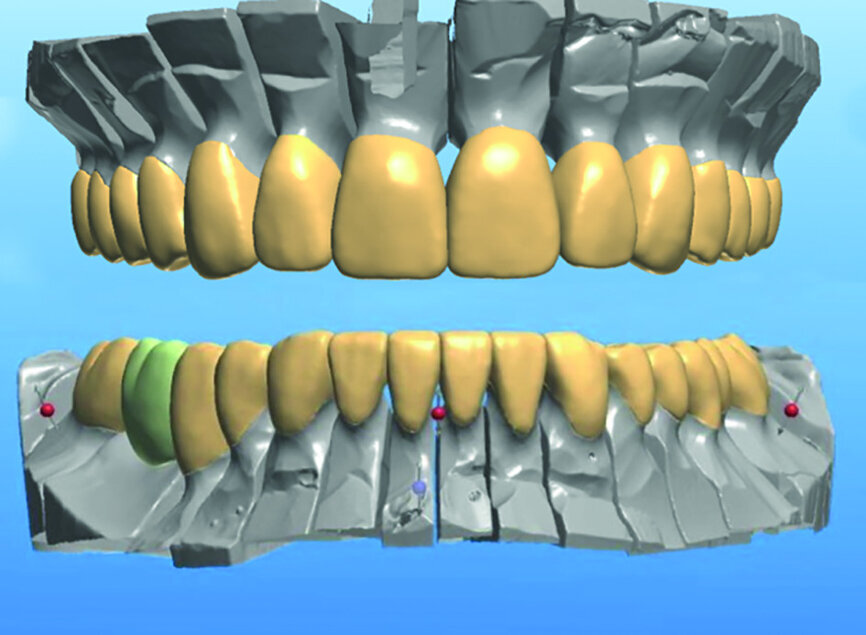
The White Wax-Ups, colour photographs, impressions and bite relations were forwarded to the dental laboratory (Arrowhead Dental Laboratory). A scan of the White Wax-Ups was used to select an appropriate arch form, tooth size and occlusion from the library of teeth available in the 3Shape software (Fig. 7).
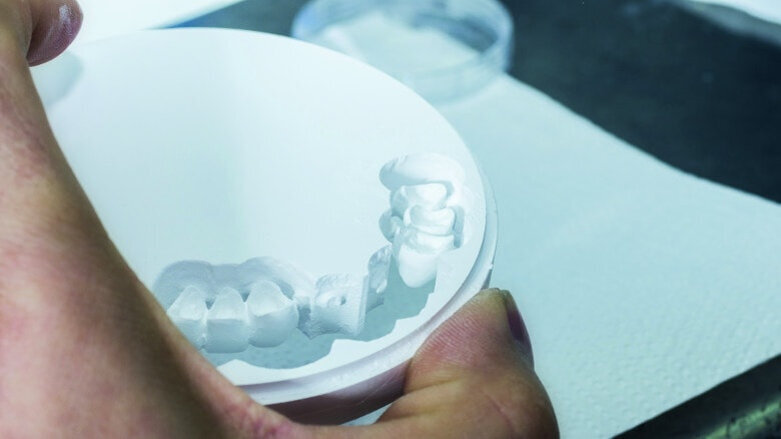
Using 3Shape Communicate, images of the proposed reconstruction were forwarded to my office by e-mail. Any minor adjustments in tooth shape and contour were communicated with the technical adviser to achieve the most ideal aesthetics. Once approved, the milling process was begun (Fig. 8).
Cementation
Before try-in of the definitive restorations, the provision al restorations were removed using the Easy Pneumatic Crown and Bridge Remover (Dent Corp) and any remaining provisional cement was cleaned off the prepared teeth. The maxillary and mandibular zirconia restorations were tried to verify fit, form and shade. After the patient had been shown the retracted view for acceptance, the cementation process was initiated.
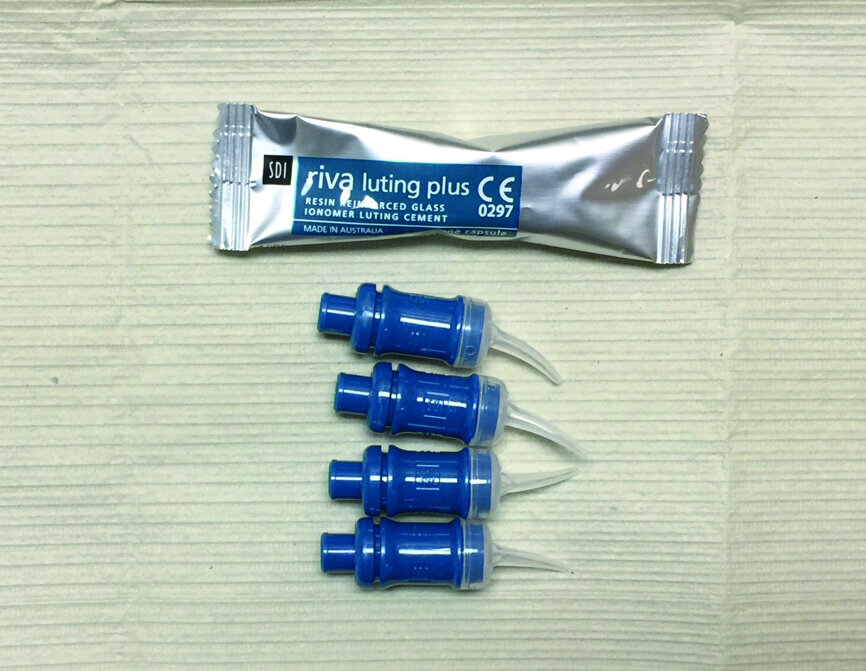
Riva luting plus (SDI), a resin-modified, self-curing glass ionomer luting cement, was used for the cementation of these zirconia restorations because it can be used without special preparation using cleaning agents, nor does it require any bonding agent (Fig. 9).
According to the manufacturer, Riva luting plus utilises SDI’s proprietary ionglass filler. longlass is a radiopaque, high-ion-releasing reactive glass used in SDI’s range of dental cements. Riva luting plus releases substantially higher levels of fluoride to assist with remineralisation of the natural dentition. This higher level of fluoride has a proven antimicrobial activity against three cariogenic bacteria: Streptococcus mutans, Streptococcus sobrinus and Lactobacillus.[1] In addition, Riva luting plus has low solubility in the oral environment, increasing the material’s ability to resist degradation and wear at the margins caused by oral acidity.
The preparations were washed and dried to the extent that they were still slightly moist. At this time, the cement capsules were depressed consecutively to activate and placed in the ultramat 2 (SDI) amalgamator for only ten seconds for trituration.
Using the applicator dispenser (SDI), the cement was loaded into the restorations (Fig. 8), starting from the midline and working distally. With a very low film thickness and creamy consistency, Riva luting plus cement was dispensed into the restorations with easy insertion and seating.
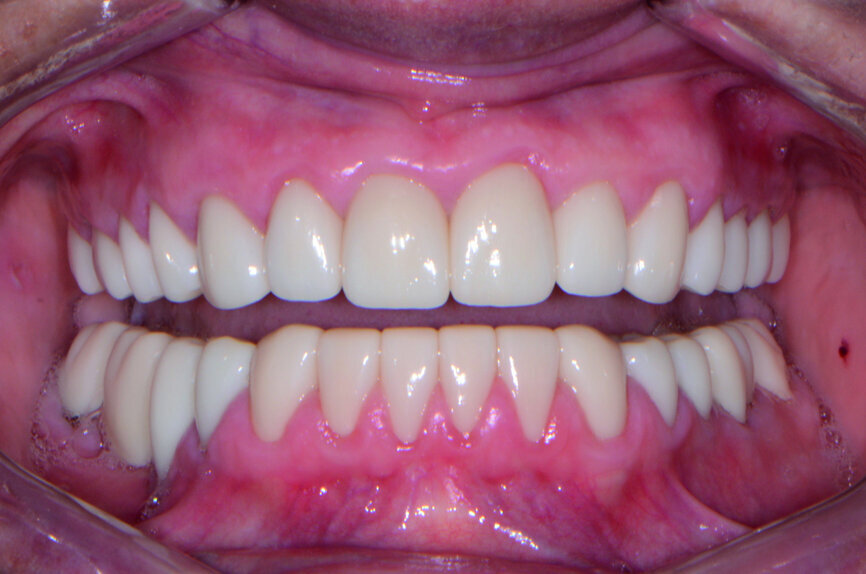
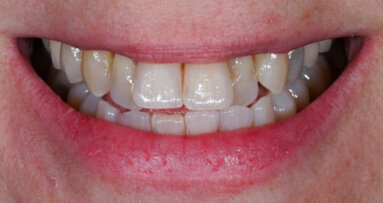
Removal of excess cement was cleaned up in about two minutes at the gel phase. After the cement was fully set at five minutes, the occlusion was verified and adjusted. The overall health and structure of the soft tissue and restorations were very good. The patient was extremely satisfied with the definitive results (Figs. 10–12).
The occlusion was checked and verified with T-Scan (Tekscan) to make sure that all of the proper points of contact were in their ideal positions to ensure longevity of the reconstruction. The patient no longer experienced pain and was very pleased with her new enhanced smile (Fig. 10).
Conclusion
In conclusion, having a systematic method for treatment planning, material selection, tooth preparation and cementation, the dental provider will be able to address the needs of the patient more effectively and efficiently. Because of this and more, the final outcome will be much more predictable aesthetically and functionally.
Acknowledgement
Special thanks to Chris Barnes and his staff at Arrowhead Dental Laboratory for the fabrication of the restorations depicted in this case.
Editorial note: A list of references is available from the publisher. This article was published in CAD/CAM—international magazine of digital dentistry No. 02/2018.
Tags:
HILDEN, Germany: By providing a natural colour gradient and high translucency, the modern multilayered zirconia KATANA Zirconia STML (Kuraray Noritake ...
During the last decade, zirconia has increasingly become established as the material of choice in prosthodontics. Its excellent mechanical and inert ...
When dental zirconia evolved into a highly aesthetic material suitable for the production of restorations with a monolithic design or minimal labial ...
Maxillary lateral incisor agenesis (MLIA) is a congenital condition in which at least one of the maxillary lateral incisors is missing in the primary or ...
The restorative dental treatment possibilities available to practicing dentists have grown immensely over the past few decades. Considerable progress has ...
CHIA, Italy: “Focus on New Visions in Dentistry” is the theme at the 10th International Dental Congress and will take place in Chia in Sardinia on ...
The aesthetics are always a significant challenge during implant restoration, especially in the aesthetic zone, in addition to the full consideration ...
A 31-year-old female patient presented to our care with esthetic concerns regarding the appearance of her gummy smile and bony protuberances above her ...
Oral surgery is an important cornerstone in orthodontic treatment of malocclusions. Tooth movement is only possible to a limited extent and always depends ...
Today’s consumers are always searching for the ultimate bargain, even when it comes to their dental care. They want high-quality results and minimally...
Live webinar
Tue. 26 May 2026
12:00 pm EST (New York)
Live webinar
Tue. 26 May 2026
2:00 pm EST (New York)
Live webinar
Wed. 27 May 2026
8:00 am EST (New York)
Live webinar
Thu. 28 May 2026
12:00 pm EST (New York)
Dr. Anthony Viazis DDS, MS. Inventor & Founder of Fastbraces®
Live webinar
Mon. 1 June 2026
1:00 pm EST (New York)
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





























To post a reply please login or register