Patients often seek aesthetic dental care to improve their appearance and function and often present with numerous complications and factors that require a comprehensive focus to attain a successful aesthetic result. If all factors present are not treated, a clinician can make improvements, but the case will not be ultimately successful. Identifying all of these factors and involving the patient in these treatment goals is essential.1–3 Besides providing aesthetic solutions for our patients, we should aim to preserve and improve our patients’ systemic health with the treatment options, techniques and materials utilised. A healthy dentition and periodontium, stable temporomandibular joint health, and good airway health should all be taken into account.
The patient in this case presented with obvious aesthetic and functional deficits associated with the effects of severe wear, periodontal disease and tooth loss. This case report demonstrates that, through meticulous treatment planning using digital smile design and a digital workflow for both the surgical and restorative treatment phases, the quality of life and systemic health of our patients can be dramatically improved.
“Without a proper plane of occlusion, the remaining features that establish proper form and function are adversely affected.”
Diagnosis and treatment planning
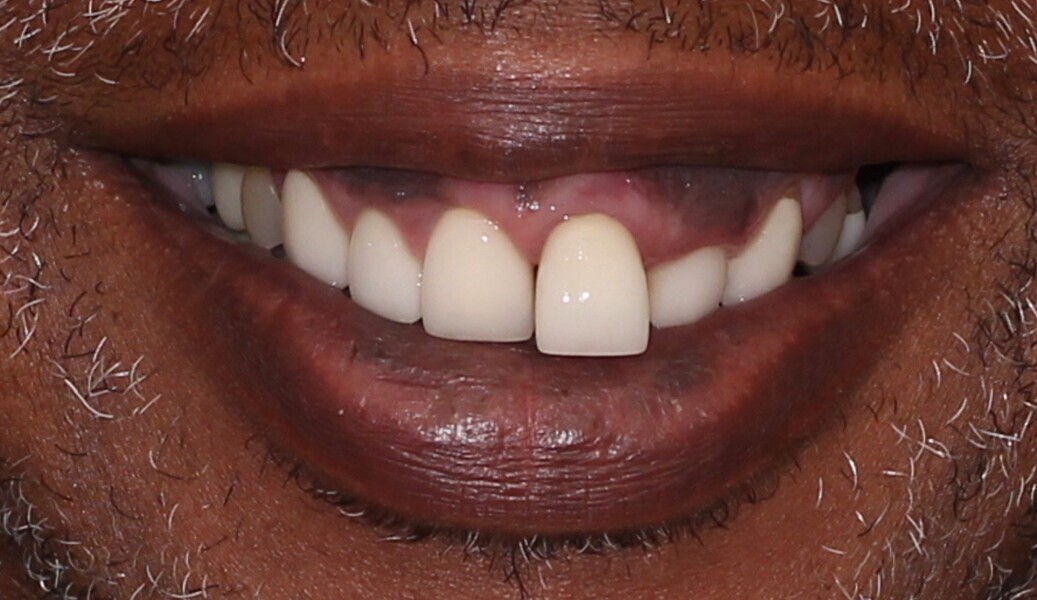
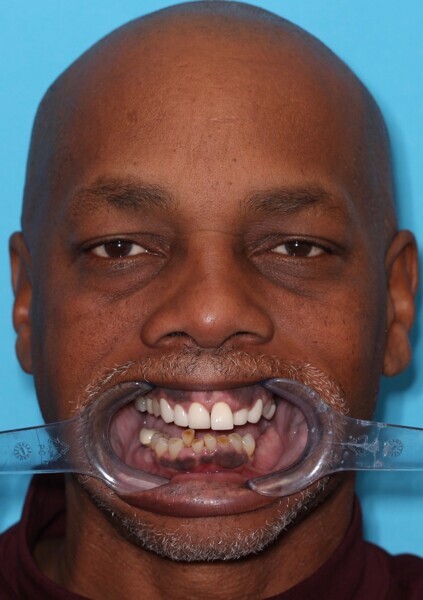
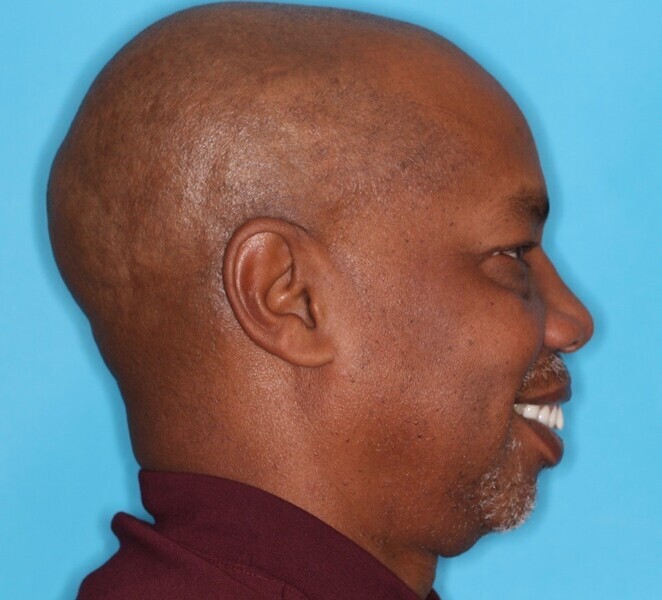
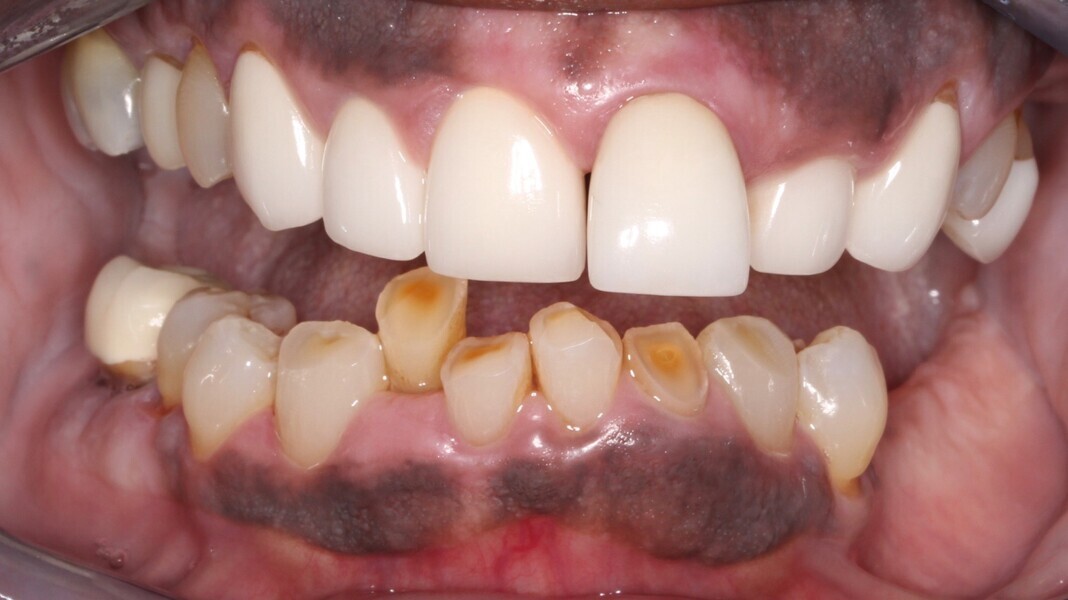
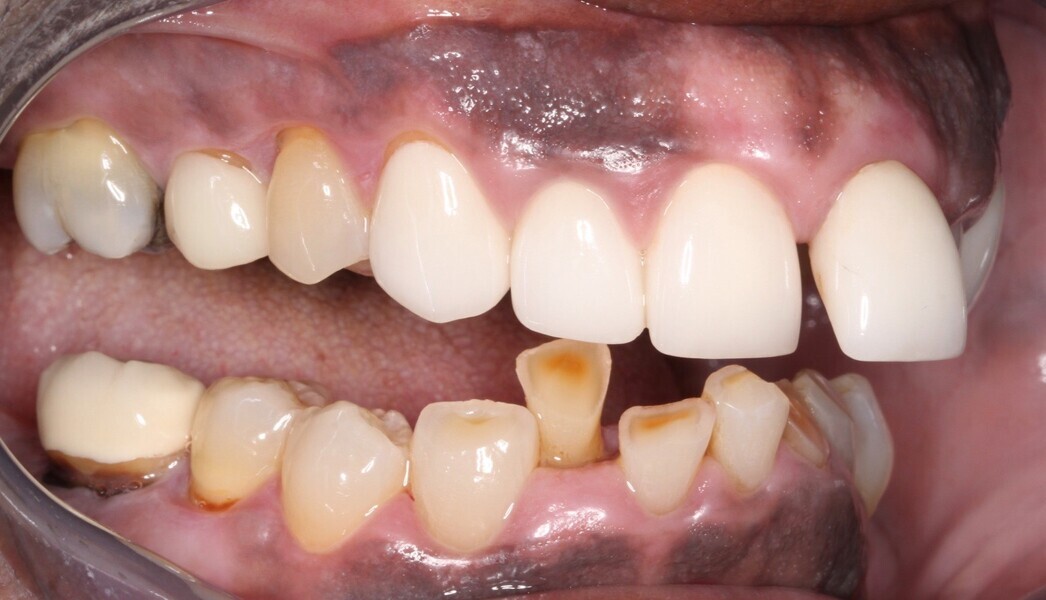
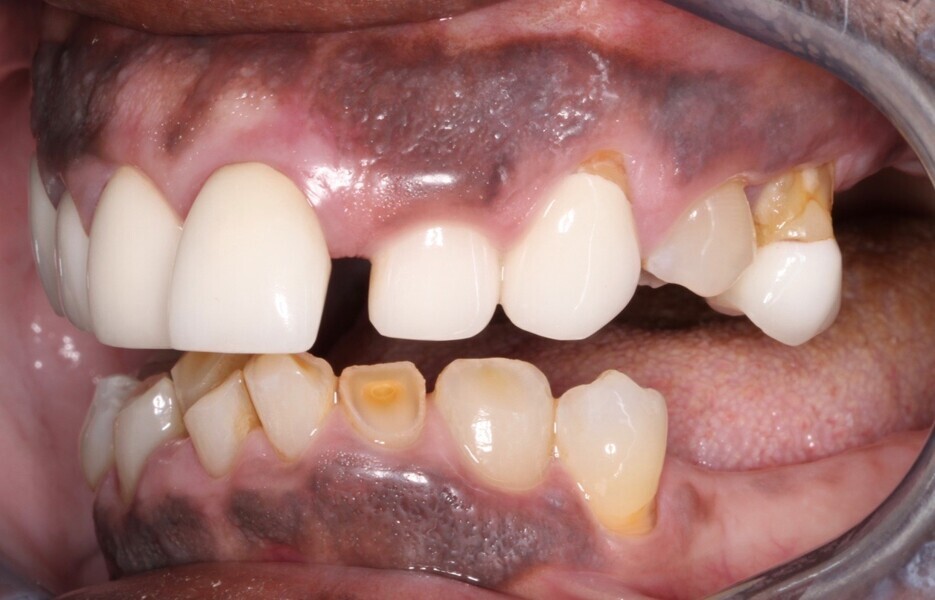
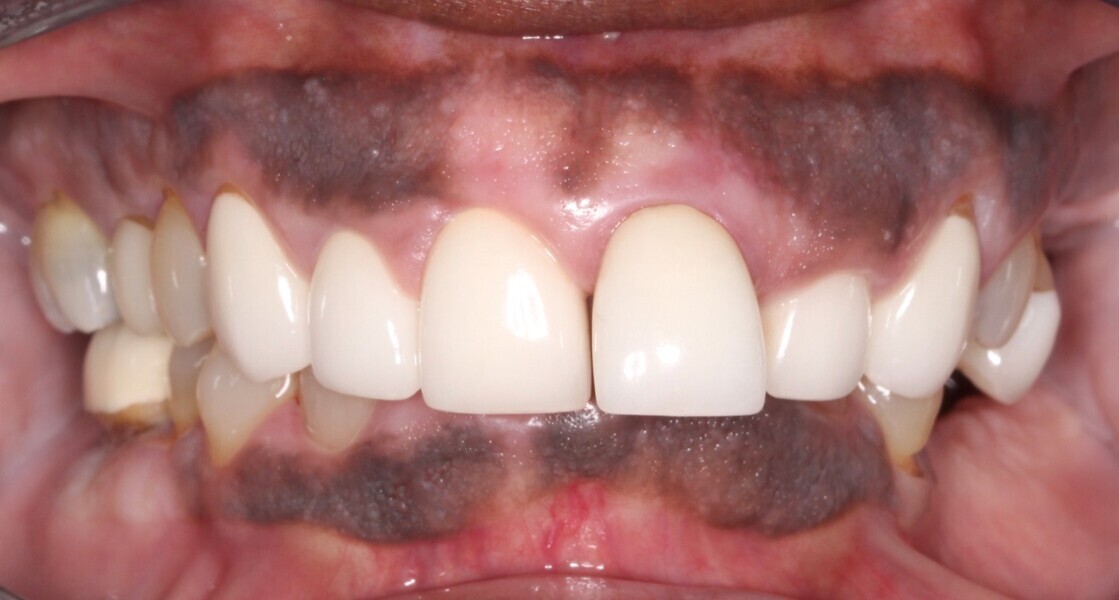
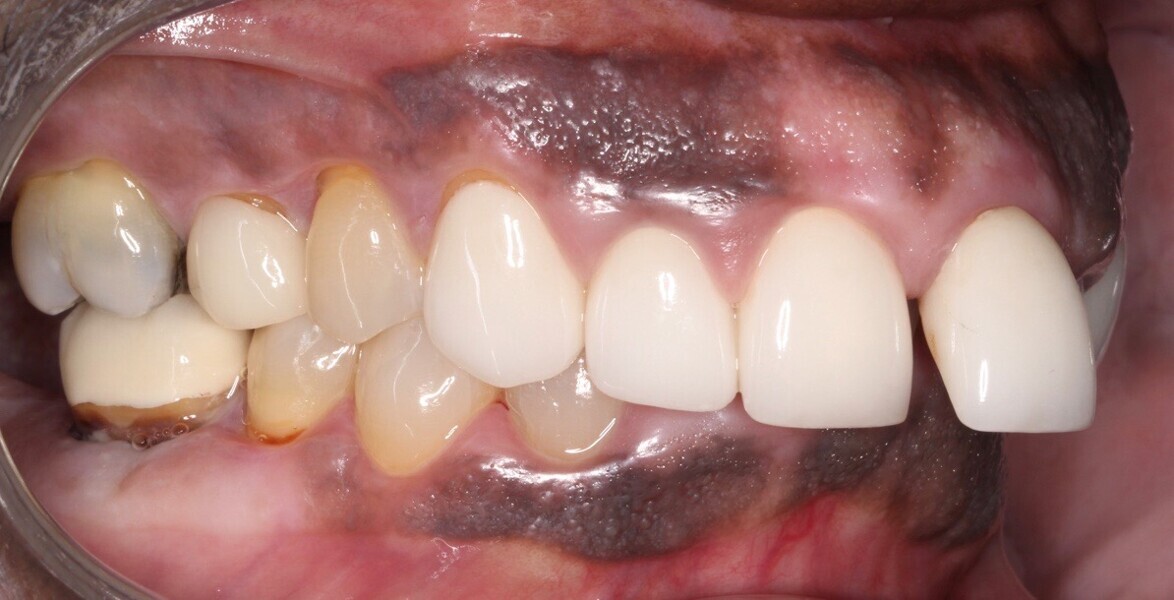
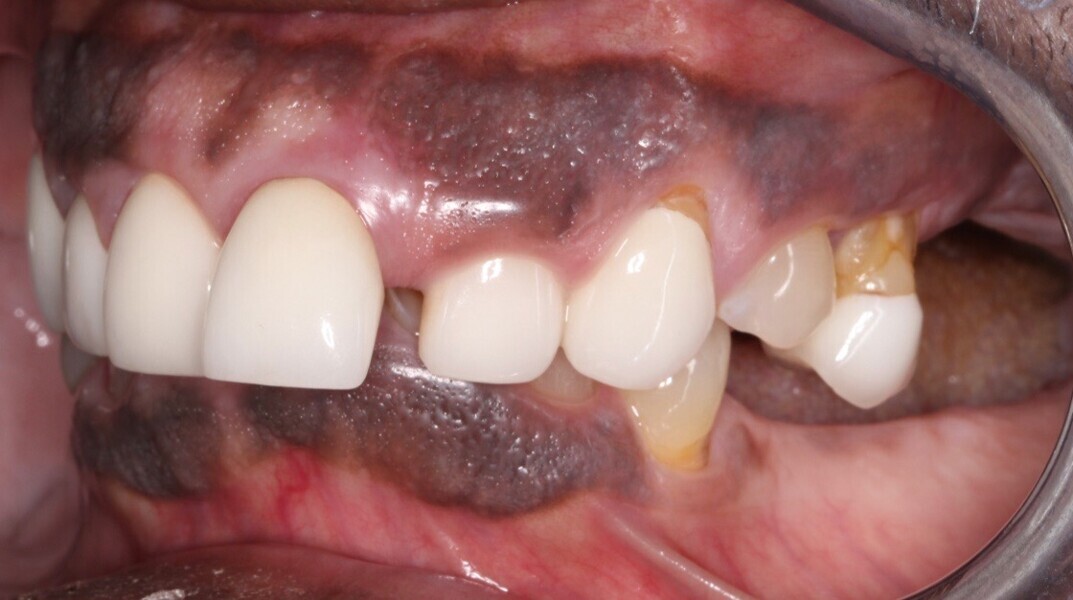
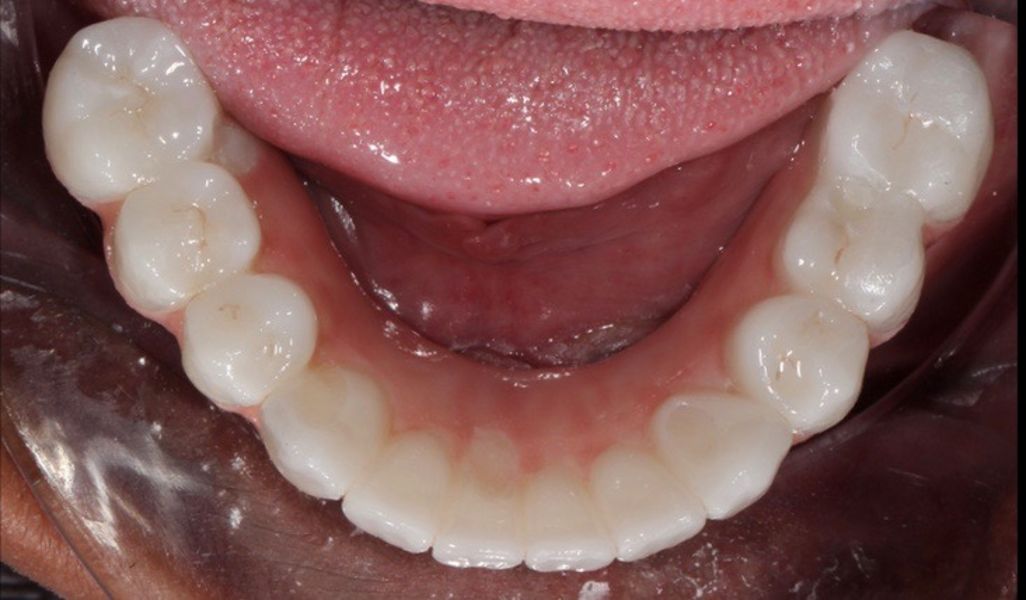
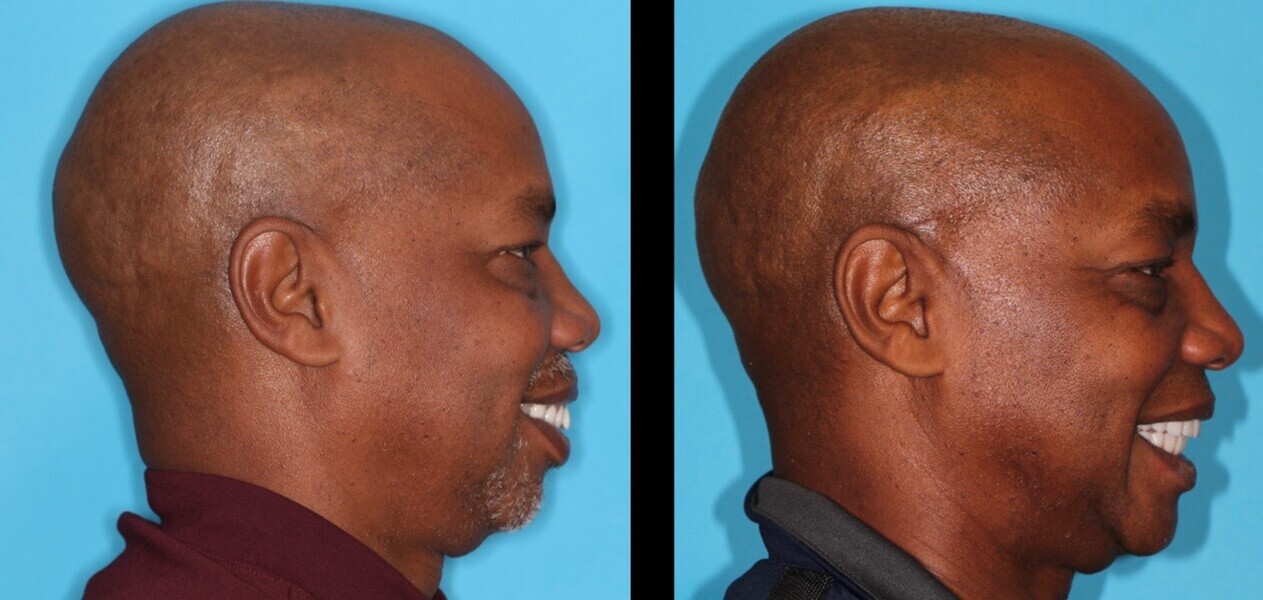
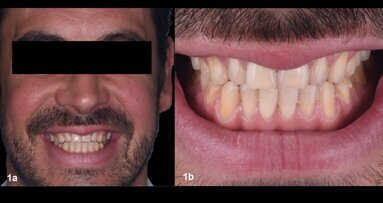
Upon examination, biological, functional and aesthetic deficits were present (Figs. 1–10). Several periodontal defects were located in the maxillary and mandibular anterior sextants and bilateral posterior quadrants. Severe wear due to attrition with compensatory overeruption of the mandibular anterior alveolar crest had contributed to occlusal plane discrepancies. Irregularities in the curve of Wilson and curve of Spee had resulted in occlusal disharmony and no anterior guidance. Excessive overbite and overjet and vertical maxillary anterior excess were noted. Other aesthetic deficiencies included a lip line that did not match the smile line and irregular and asymmetrical gingival zeniths, incisal embrasures and incisal edge positions. The patient’s profile view showed a retruded chin and deficient lower facial third height. Increasing the lower facial third height would allow for improved chin prominence and a more youthful appearance.
This “triangle of youth”, present in people with ideal vertical facial thirds, as described by Gelb, is an inverted triangle from the facial view in which three straight lines connect the most lateral aspects of the right and left cheek bones to the mental protuberance of the chin.4 An aged face is often due to a loss of ideal lower facial third height and a retruded chin, in which from the facial view a triangle can be outlined with a straight line connecting the left and right angles of the mandible to the inferior aspect of the nasal bone.4 The treatment objectives were to restore ideal function and aesthetics by correcting these various deficiencies.
When numerous functional and aesthetic challenges are present, one of the first steps in establishing an aesthetic reconstruction is to define the proper plane of occlusion.5 According to Dawson, “the form of the occlusal plane is directly related to specific functional requirements, alignment of teeth in relationship to the arc of closure for best resistance to loading and ease of access for positioning of the food on the occlusal surface”.6 Without a proper plane of occlusion, the remaining features that establish proper form and function are adversely affected. Tooth dimensions and embrasures will not be balanced and oriented properly, and an aesthetic outcome will be compromised.7 To restore proper form and function and correct the identified deficiencies, our treatment plan involved full-arch implant-retained prostheses following a predictable and streamlined digital workflow.
Clinical protocol
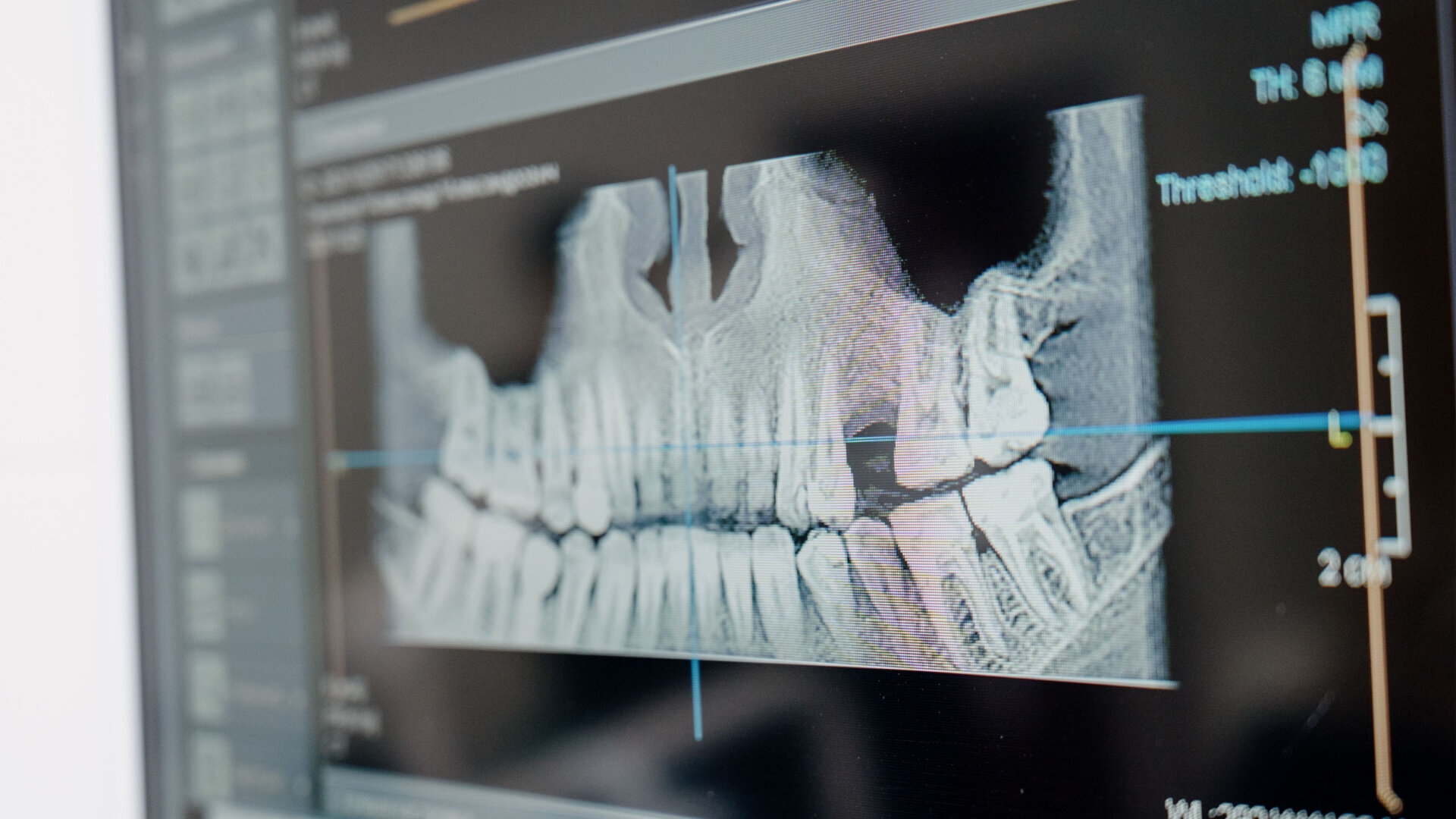
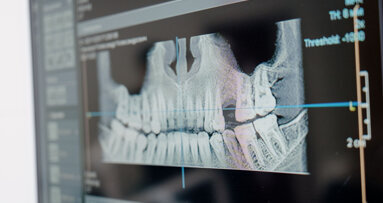
Using the NavaGation Synergy Guided Workflow (Absolute Dental Services), the restorative and surgical planning phase began with collaboration between the guided surgery specialist (Matt Vrhovac from Absolute Dental Services), surgeon (Dr Teresa Biggerstaff) and restorative dentist (me). To correct the patient’s aesthetic and functional deficiencies, the planning began by obtaining an accurate CBCT scan taken at the patient’s current vertical dimension of occlusion in centric relation position (Fig. 11). Several digital photographs were taken, including full-face smile photographs to identify the lip position and high smile line, profile photographs and retracted views (Canon Rebel T5i with a 100 mm L macro lens with both a Canon EL-100 flash system and a Canon MR-14EX II macro flash). Digital photographs are essential for the digital treatment planning workflow, as they are needed to assess aesthetics, tooth position and smile design and to guide the treatment planning process.
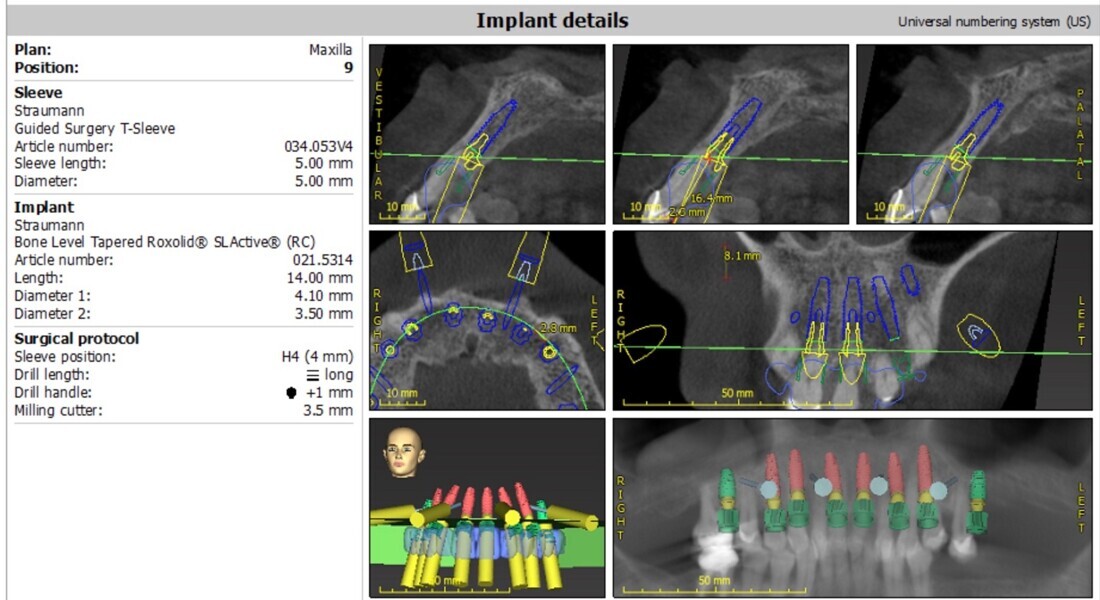
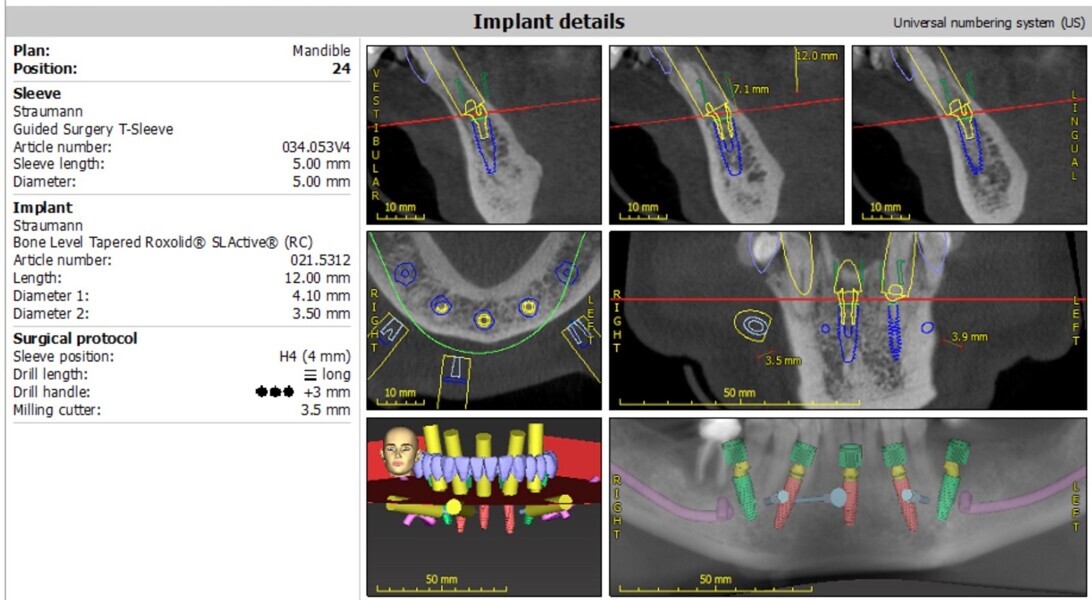
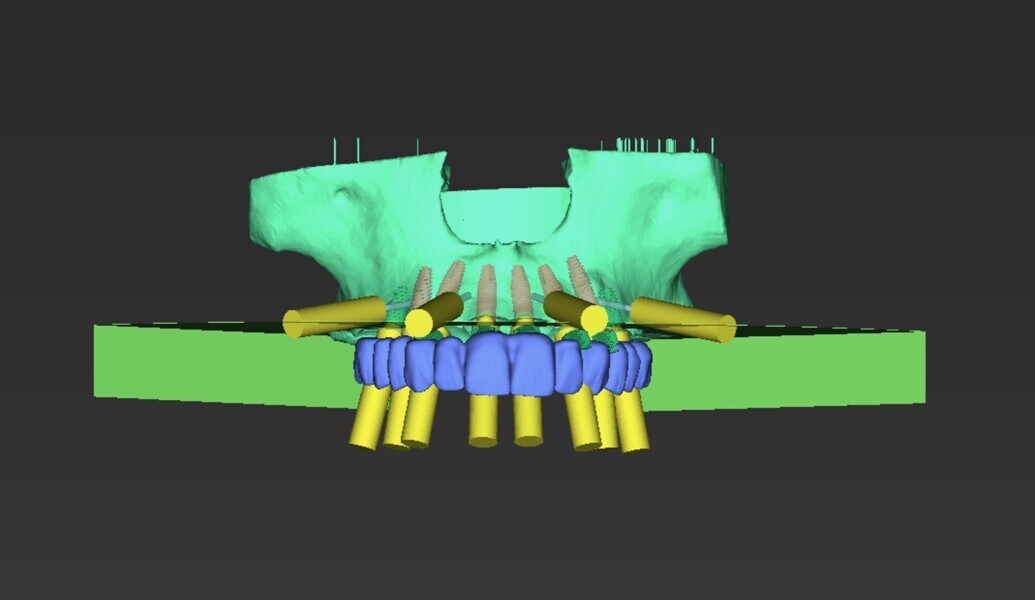
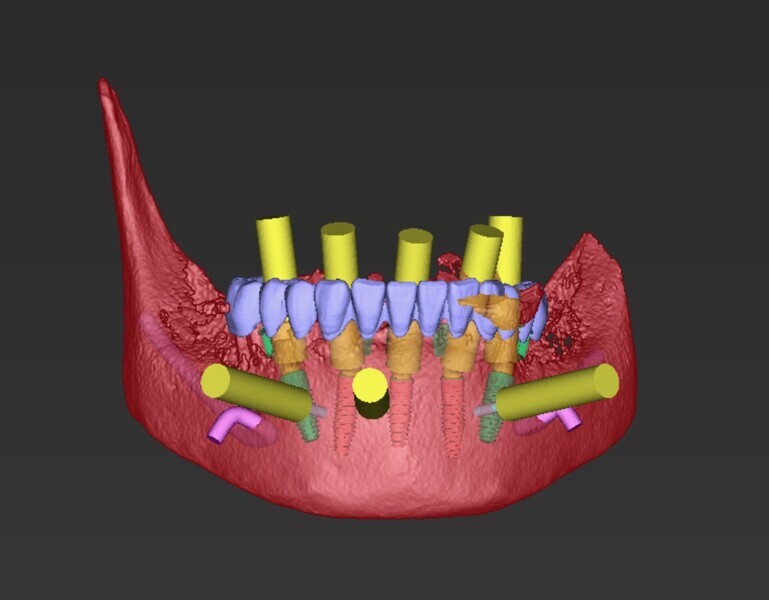
A digital wax-up was designed using 3Shape software to idealise the occlusal plane and correct the aesthetic and functional deficiencies. PreVu cosmetic simulation and smile design software (PreVu Dental) was used to superimpose the digital wax-up on to the patient’s digital photographs, enabling the guided surgery specialist, surgeon and restorative dentist to evaluate the smile plan for implant placement based upon the final prostheses. During the treatment planning meeting, the surgeon and guided surgery specialist planned for implant position, model matching and bone reduction using Absolute Dental Services’ in-house surgical planning software and coDiagnostiX software (Dental Wings; Figs. 12–15). The plan was to place eight maxillary implants and five mandibular implants for full-arch implant-retained zirconia prostheses.
To streamline an accurate and precise surgical protocol, the NavaGation Synergy Guided Workflow was utilised. A unilateral key fixation foundation guide was placed and the position verified with a 3D-printed PMMA (Flexcera, Desktop Health) tooth stabilisation guide aligner. After extraction of the failed dentition, a 3D-printed Flexcera scalloped maxillary bone reduction guide was used to idealise the maxillary alveolar ridge contours, and a mandibular bone reduction guide was used to reduce the overerupted mandibular anterior osseous segment. Buccal fixation pins were used to secure the foundation and bone reduction guides accurately and securely to the maxillary and mandibular bone. Implant placement guides were subsequently utilised to guide precise implant placement. Eight Straumann Bone Level Tapered Roxolid SLActive Regular CrossFit implants were placed in the maxillary arch (4.8 × 8.0 mm implants in sites #16 and 26, 4.1 × 12.0 mm implant in site #14 and 4.1 × 14.0 mm implants in sites #13, 11, 21, 23 and 24). Five Straumann Bone Level Tapered Roxolid SLActive Regular CrossFit implants were placed in the mandibular arch (4.8 × 12.0 mm implants in sites #36 and 46, 4.1×14.0 mm implants in sites #33 and 43, and 4.1 × 12.0 mm implant in site #31).
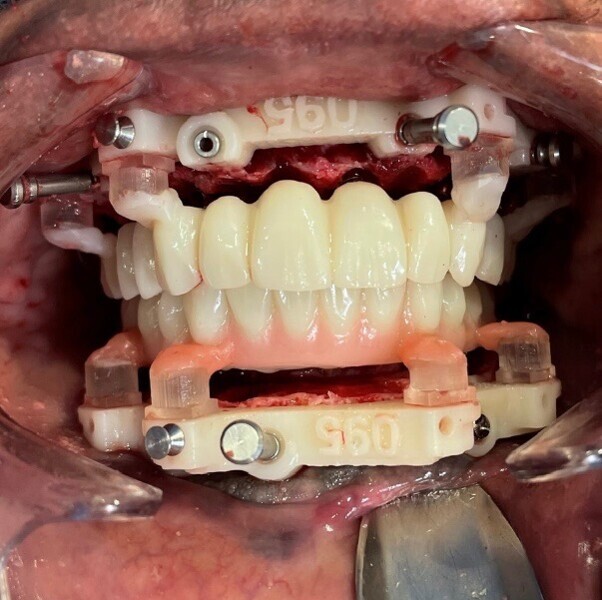
Once the implants had been placed, the implant placement guide was removed and Regular CrossFit screwretained 17° multi-unit abutments were placed using a 3D-printed Flexcera multi-unit abutment aligner guide. The transitional prostheses made from Flexcera Smile were then picked up with a dual-polymerising polymer (Triad, Dentsply Sirona), after placing the temporary titanium cylinders, each blocked out with silicone blockout tubes, on to the multi-unit abutments (Figs. 16 & 17). PTFE tape and flowable Filtek Supreme Ultra (3M ESPE) composite were used to seal each access hole prior to assessing the occlusion (Figs. 18 & 19). At this time, Flexcera Smile duplicates of the transitional prostheses were picked up with the same protocol to use when the time came for the final impressions, capturing the desired vertical dimension, tooth position and healed soft tissue. Bilateral masseter Botox injections were administered to manage excessive occlusal forces during the osseointegration phase.
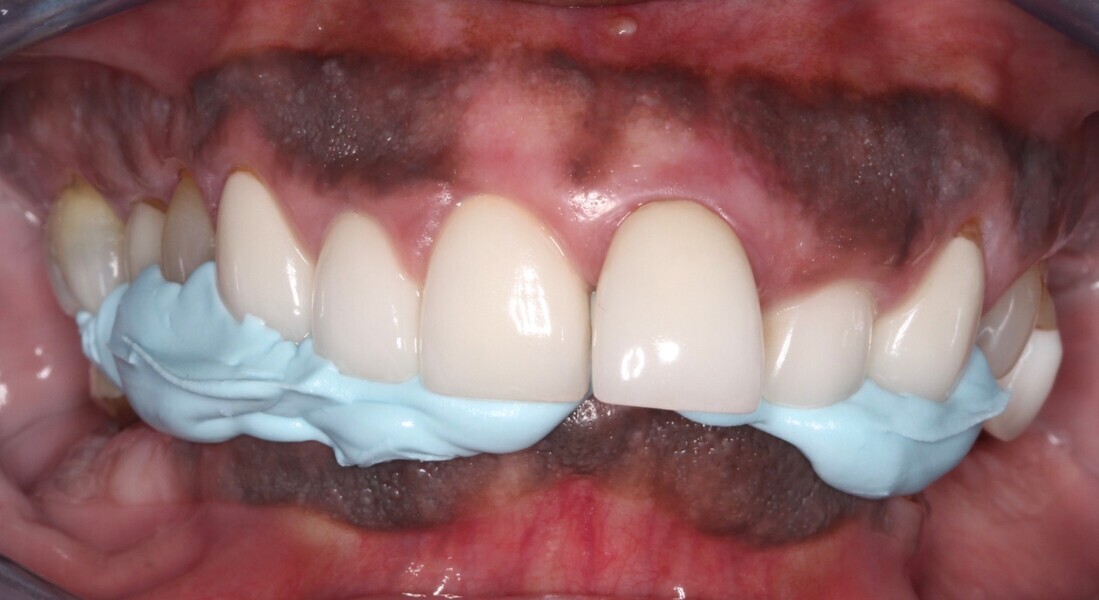
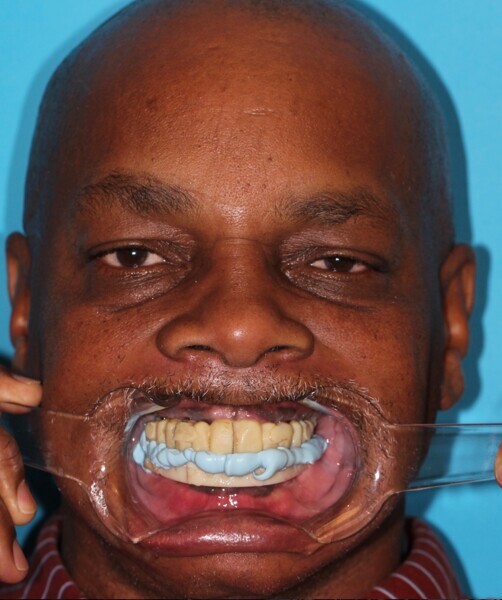
Forty-eight hours after surgery, the occlusion was assessed and minor adjustments were made to the Flexcera Smile transitional protheses. After five months of osseointegration, Flexcera Smile final impression duplicates of the transitional prostheses were seated and hand tightened to the multi-unit abutments, and a minor adjustment to the midline was marked on the impression duplicate for communication with the laboratory. A light-bodied polyvinylsiloxane (VPS) impression material was used to capture the intaglio space between the tissue and the impression duplicate of both prostheses. During the osseointegration phase, soft-tissue shrinkage is a normal sequela of the healing process; therefore, the light-bodied VPS helps to ensure seamless intaglio adaptation of the final prostheses to the soft tissue. A centric relation bite registration was taken using Blu-Mousse VPS bite registration material (Parkell; Fig. 20).
“Digital treatment planning for improved aesthetics and function can be both rewarding for the clinicians and fulfilling for the patient.”
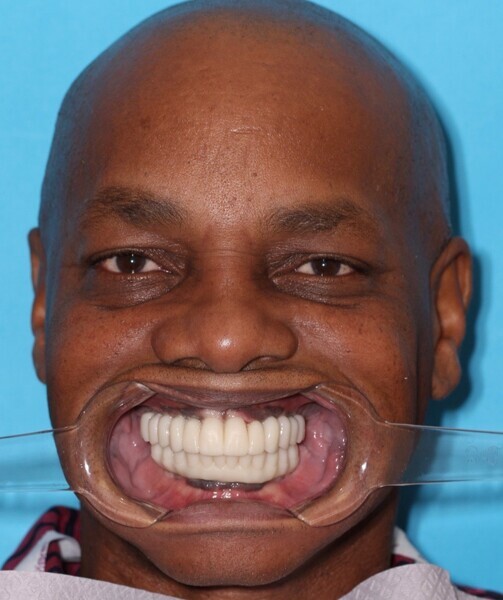
This NavaGation Synergy guided surgery and prosthetic protocol eliminates the need for guesswork, verification jigs, occlusal rims and wax set-ups. The final impression duplicates of the transitional prostheses served as both final impression trays and correct vertical dimension and tooth position guides. At the subsequent visit, prototypes made from Flexcera Smile were tried in and aesthetics, function, phonetics and occlusion were assessed (Figs. 21–25).
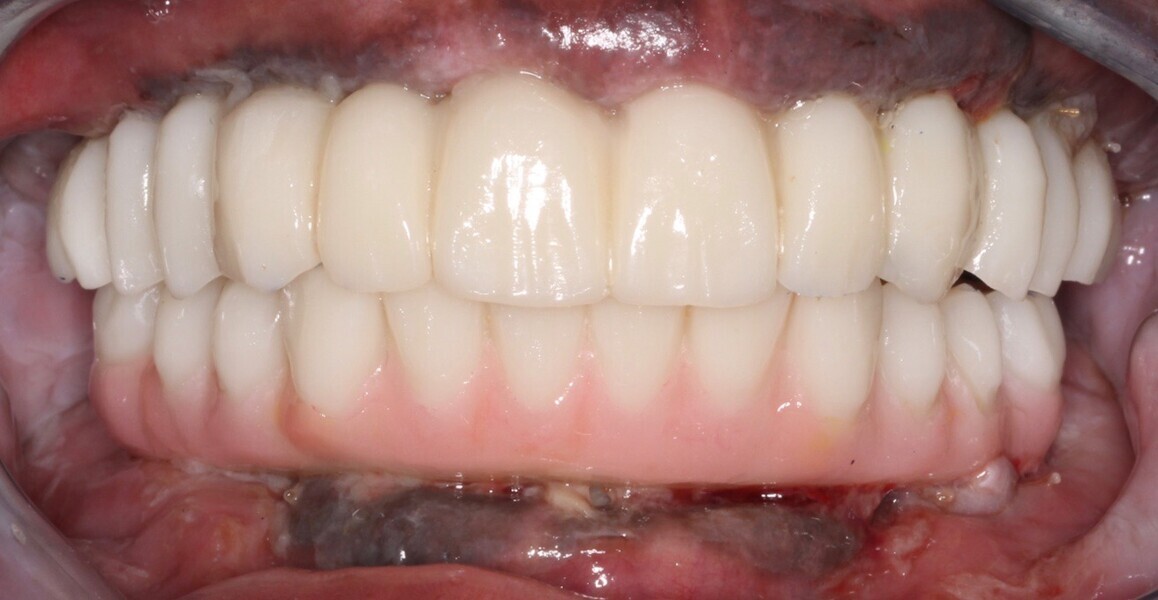
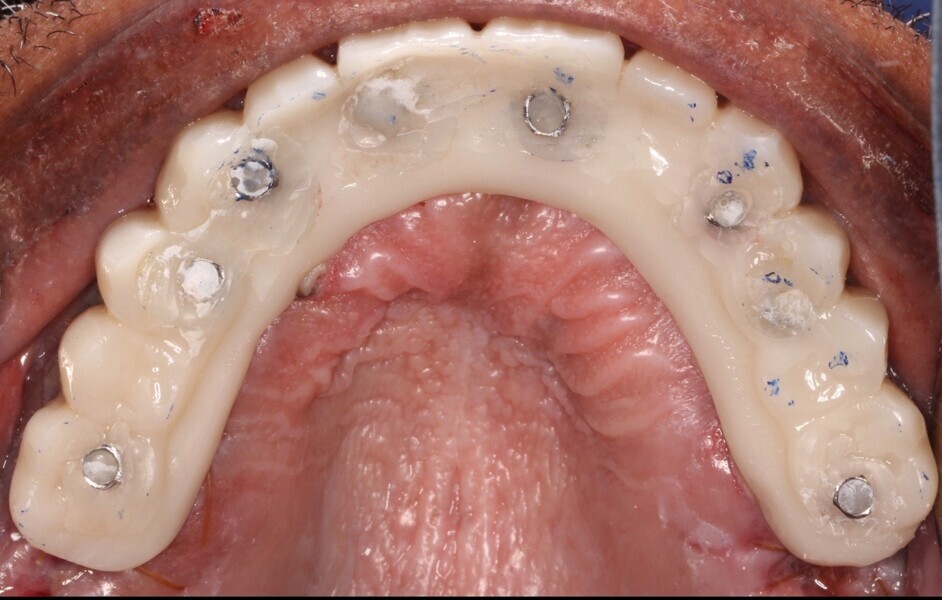
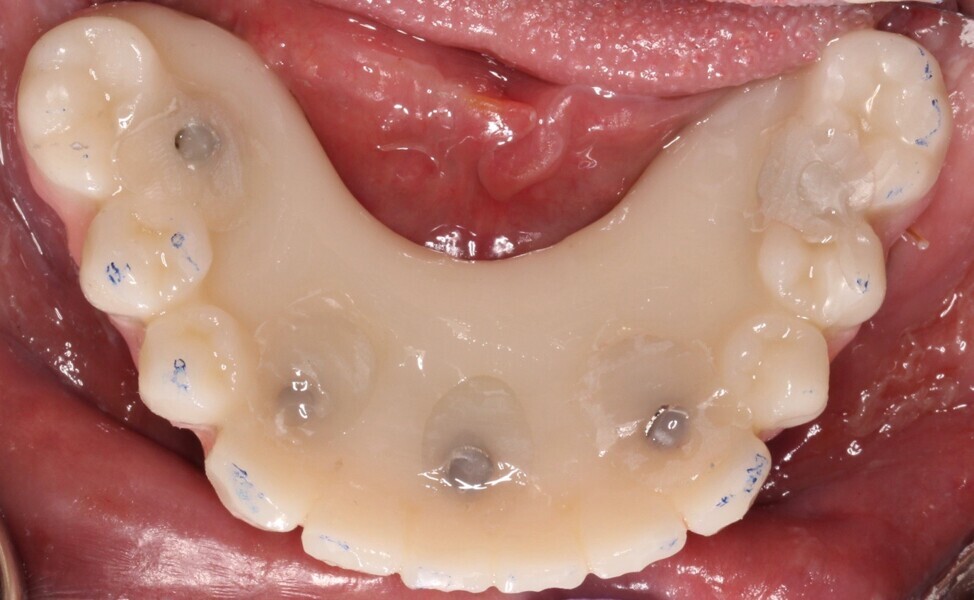
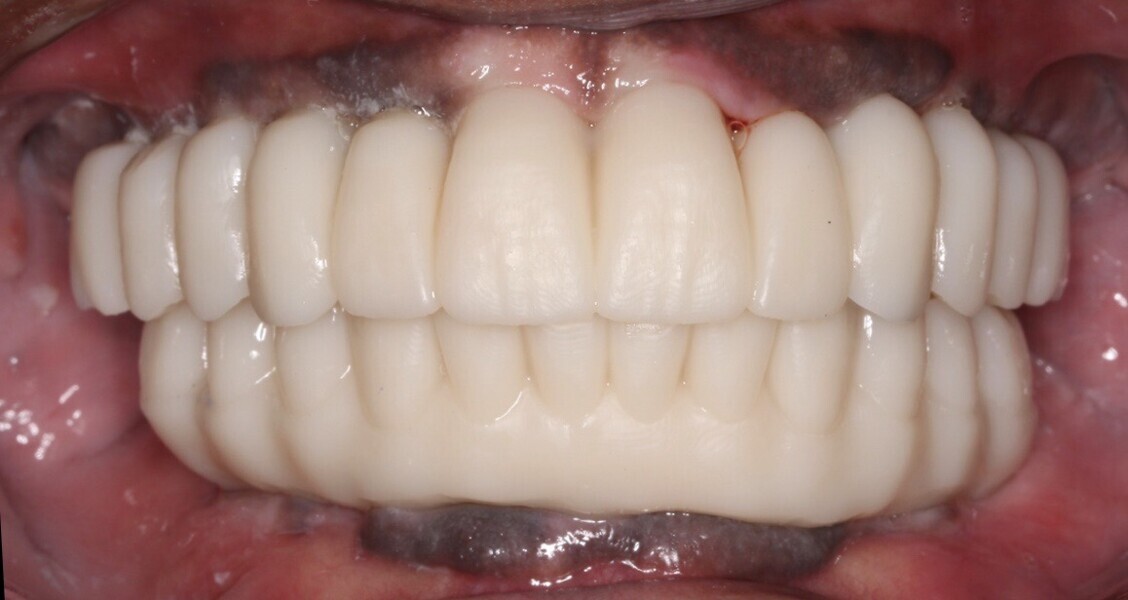
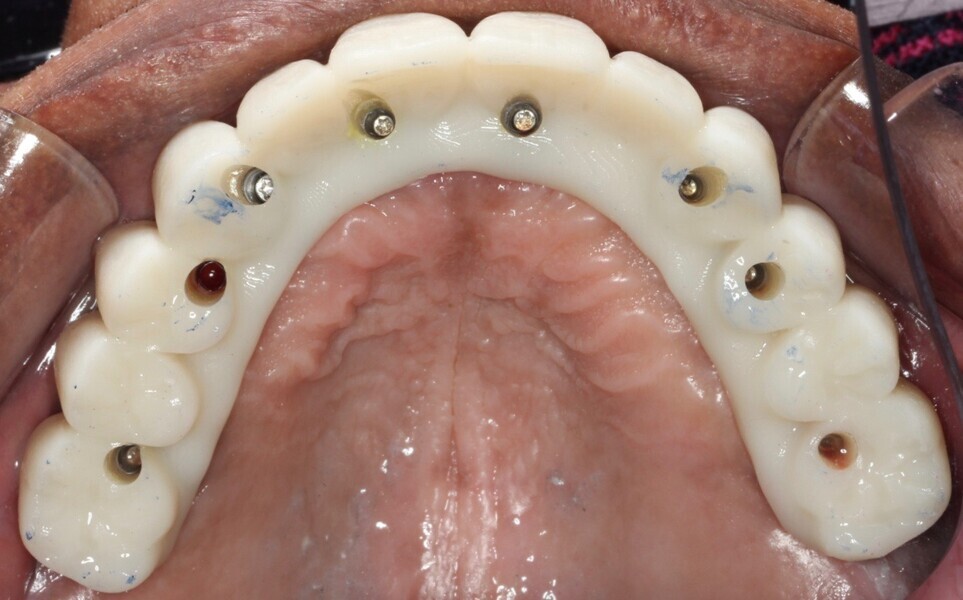
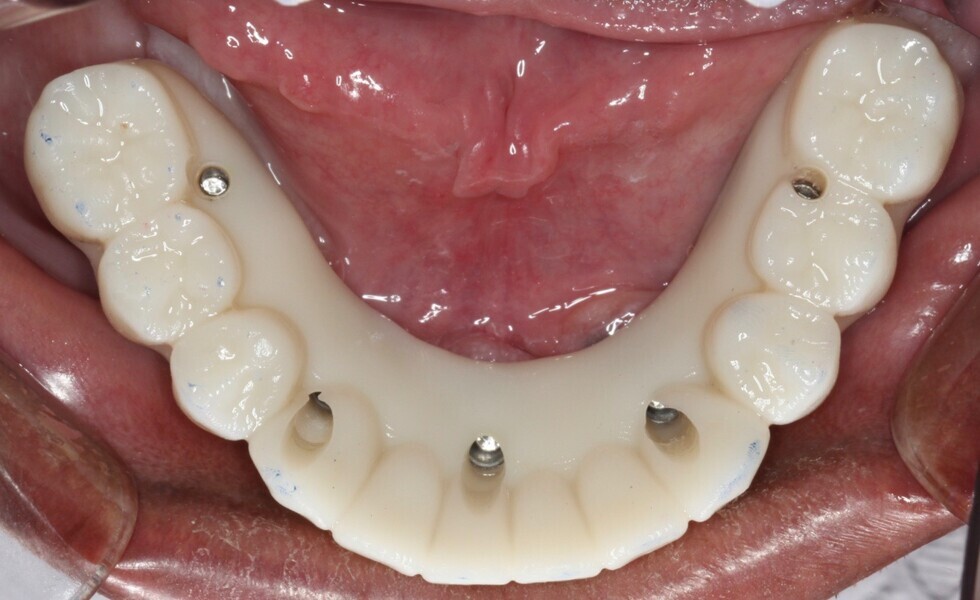
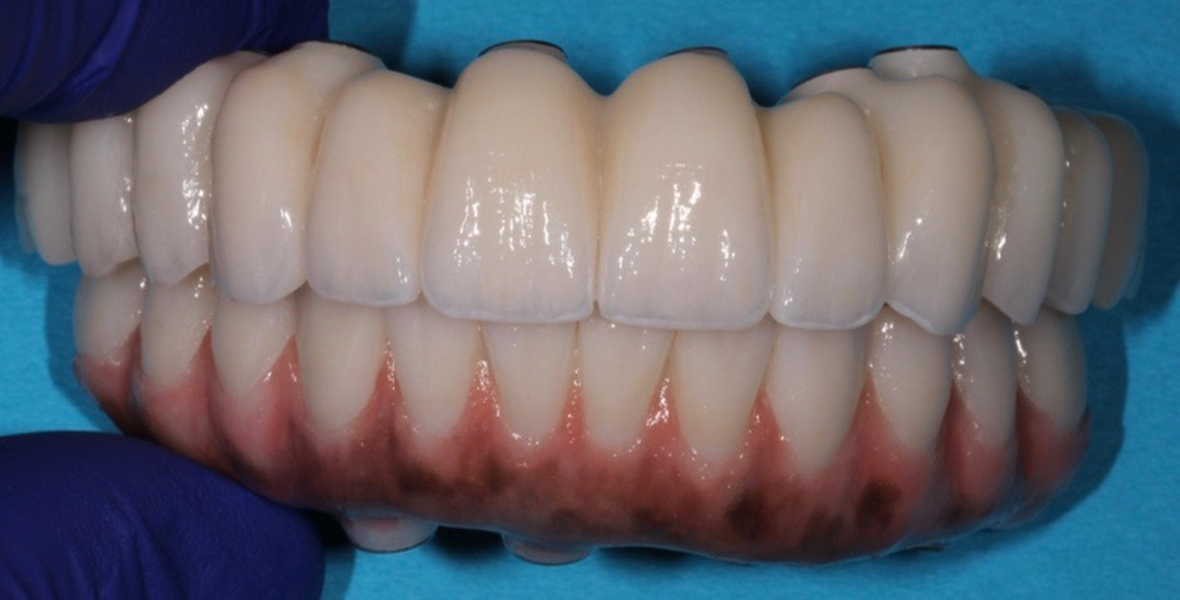
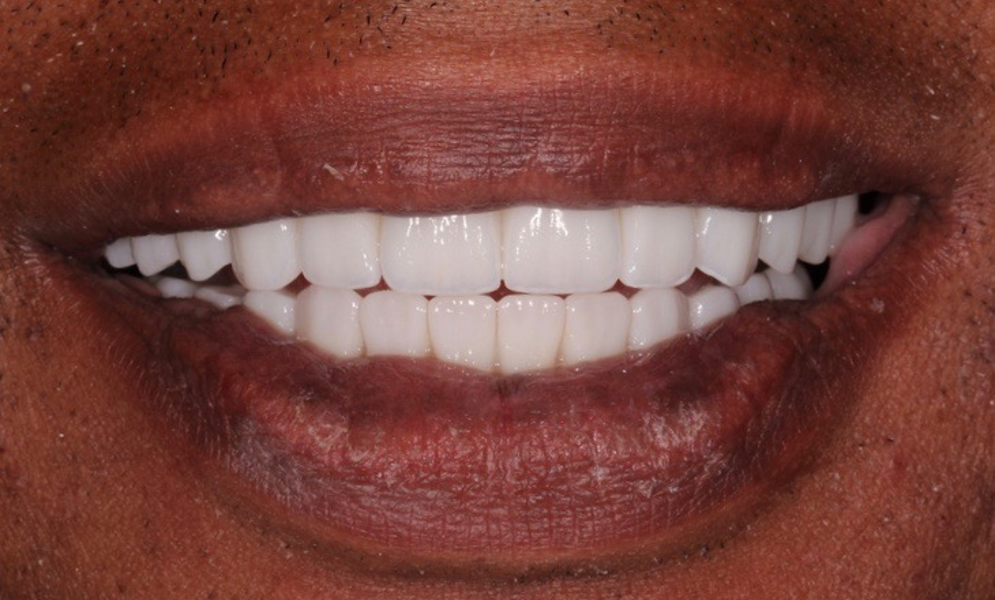
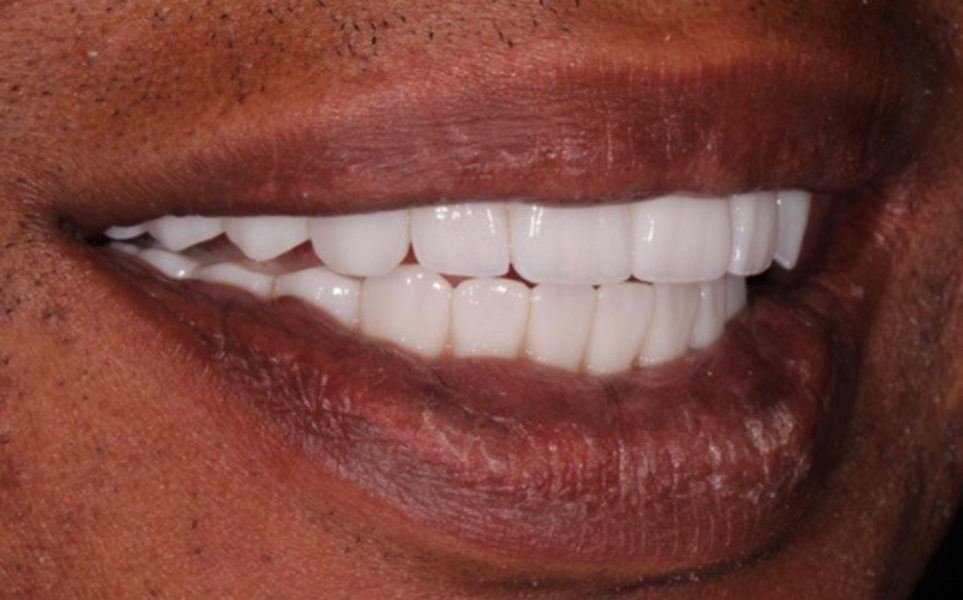
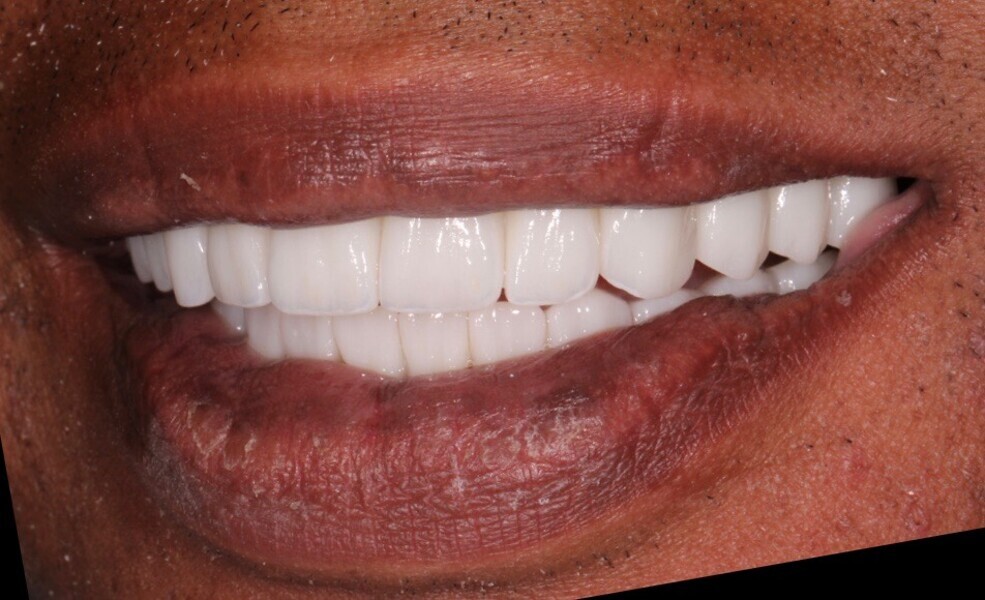
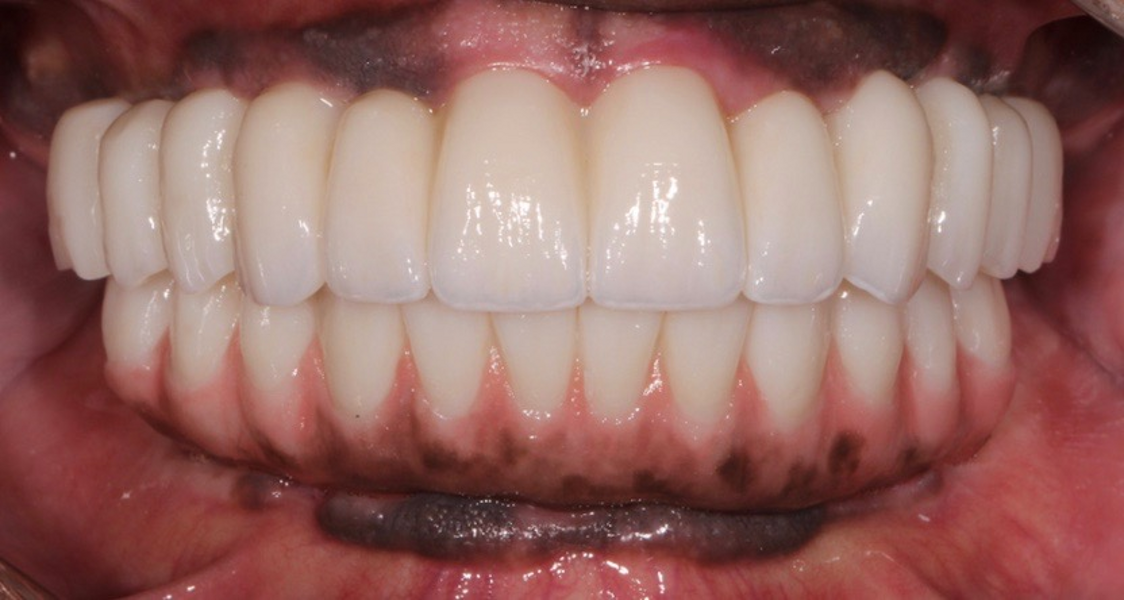
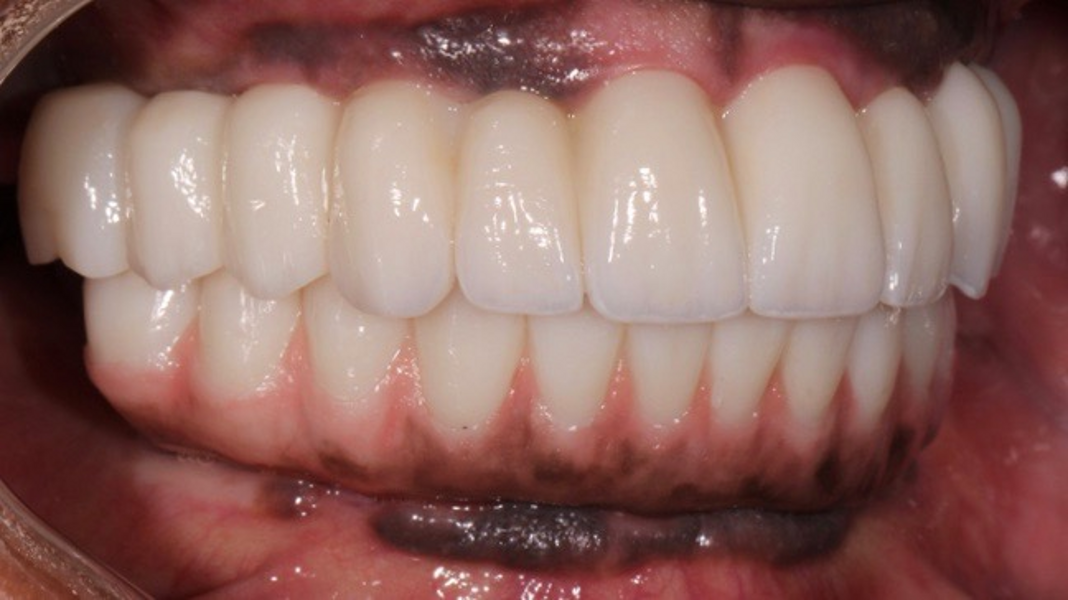
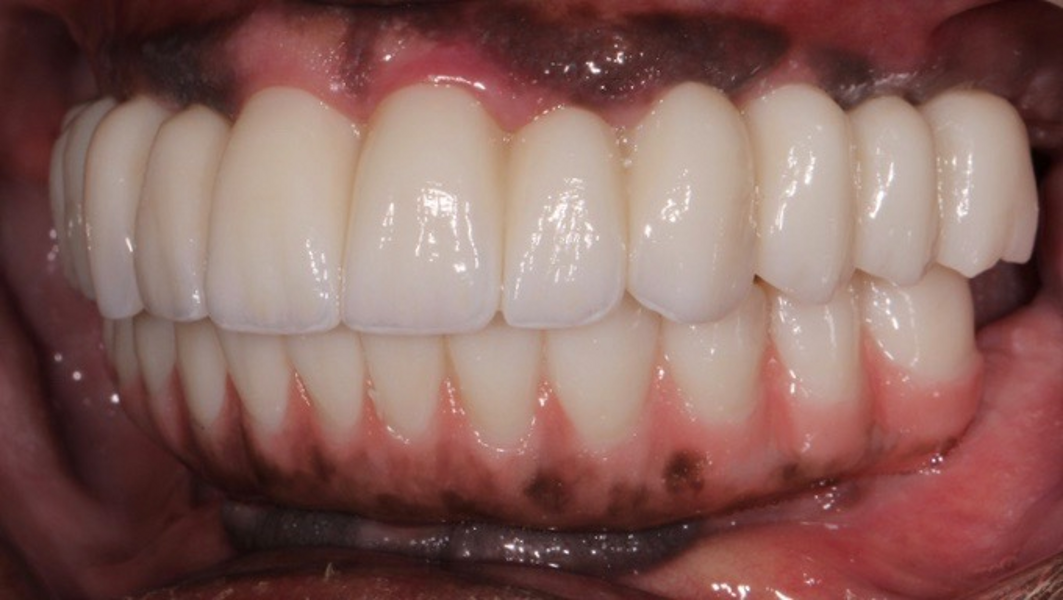
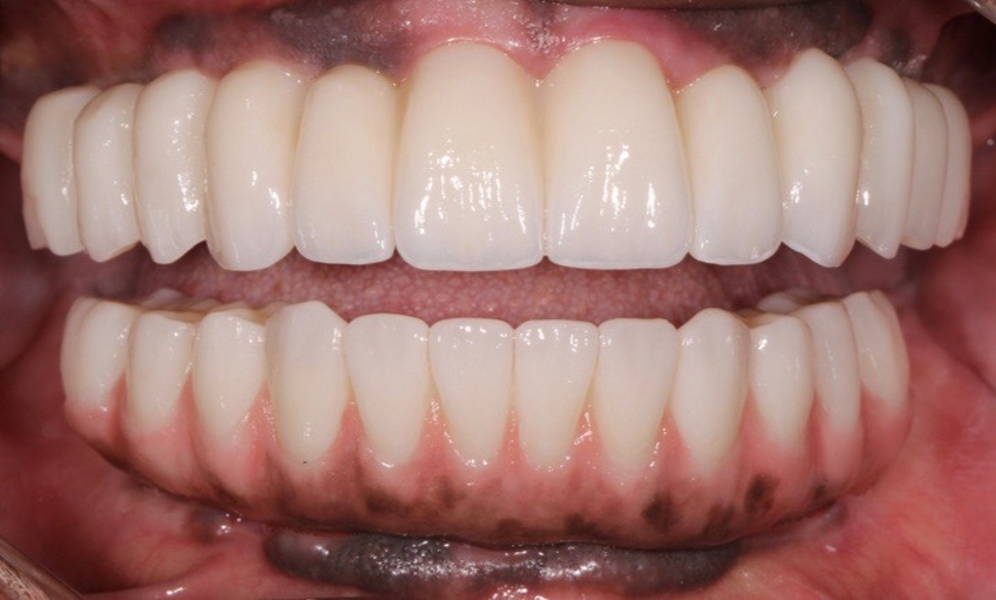
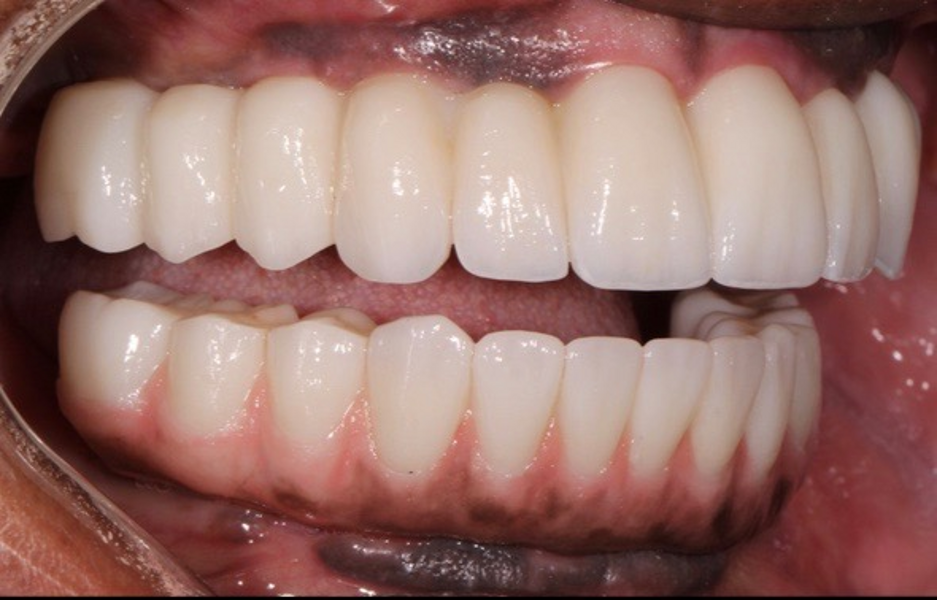
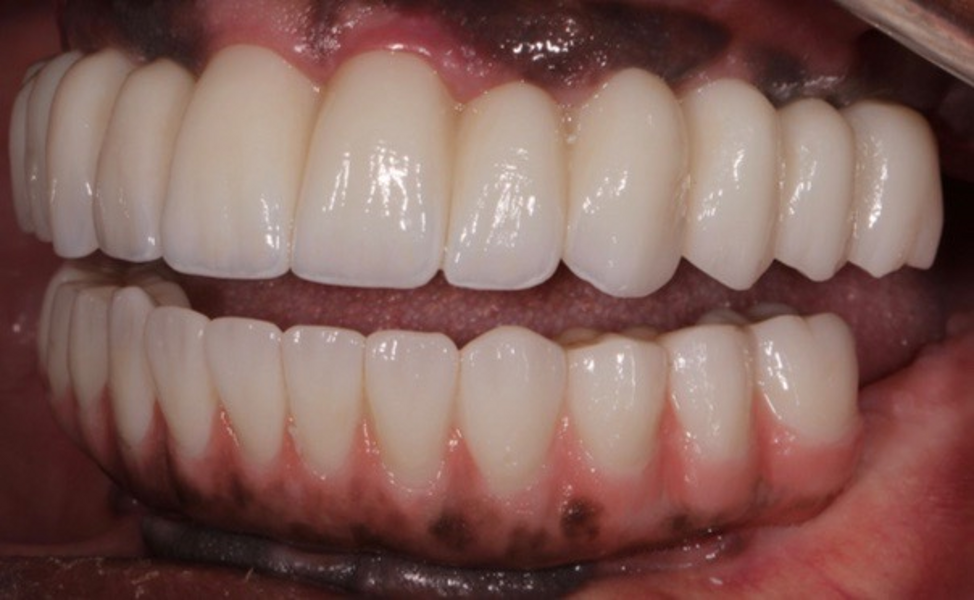
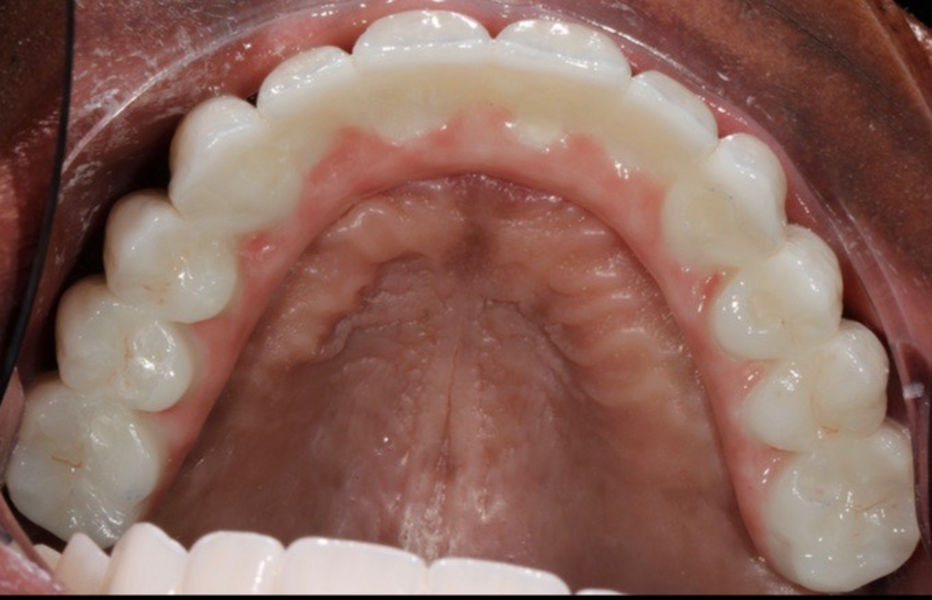
Adjustments to the gingival embrasures were made to idealise the gingival scalloping and guide papillae fill-in, and a final bite registration was obtained using Blu-Mousse. The final prostheses were fabricated from full-contour solid zirconia (ArgenZ HT+ Multilayer, 1,250MPa; Argen) and were custom stained and glazed to transition naturally with the gingival characterisation (Figs. 26–40). The multi-unit prosthetic screws were torqued to the manufacturer’s recommendations and the access holes sealed with PTFE tape and Filtek Supreme Ultra. A full-coverage maxillary flat plane occlusal night guard was fabricated to be worn indefinitely to reduce and manage occlusal parafunctional forces on the prostheses and implants.
Conclusion
Digital treatment planning for improved aesthetics and function can be both rewarding for the clinicians and fulfilling for the patient.7 Predictable surgical and prosthetic results are possible with a streamlined digitally guided workflow that eliminates guesswork. The collaboration of the surgeon, restorative dentist and guided surgery specialist in treatment planning enables visualisation of the desired outcome prior to surgery. Numerous aesthetic and functional deficiencies were addressed and resolved in this patient’s case, resulting in much improved dental health, function and appearance. The patient and all involved with the case were pleased with the outcome.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





























To post a reply please login or register