Discussion
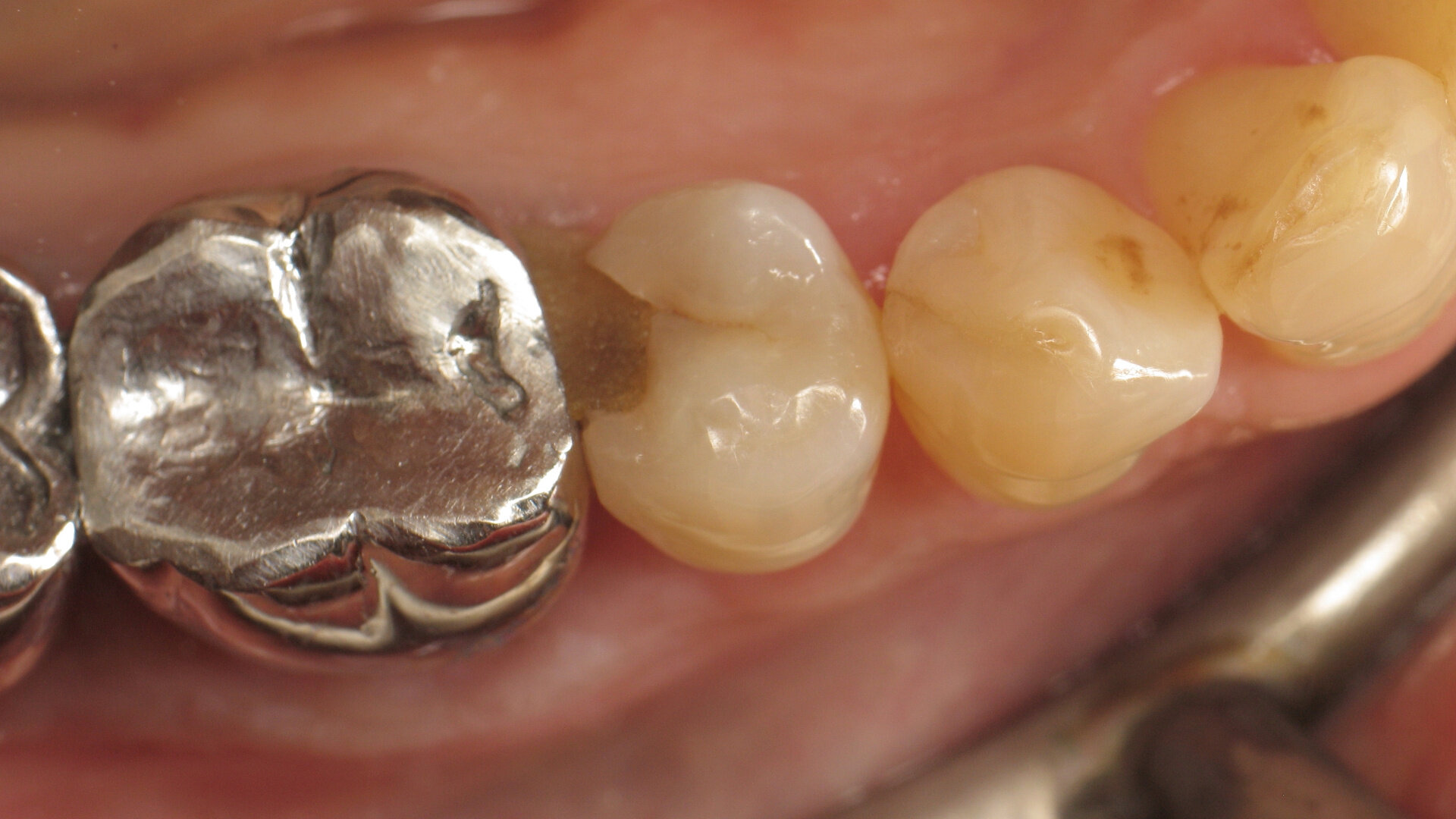
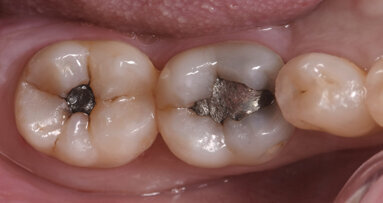
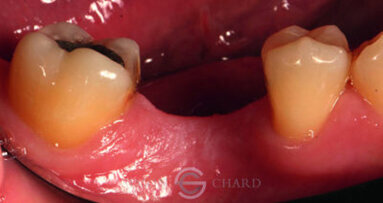
At the end of the nineteenth century, G.V. Black defined cavity Classes I–V for the categorisation of carious lesions. A sixth class, Class VI, was defined by Simon in 1956.2 Class II, the class of the clinical case presented here, refers to caries affecting the proximal surfaces of molars and premolars.
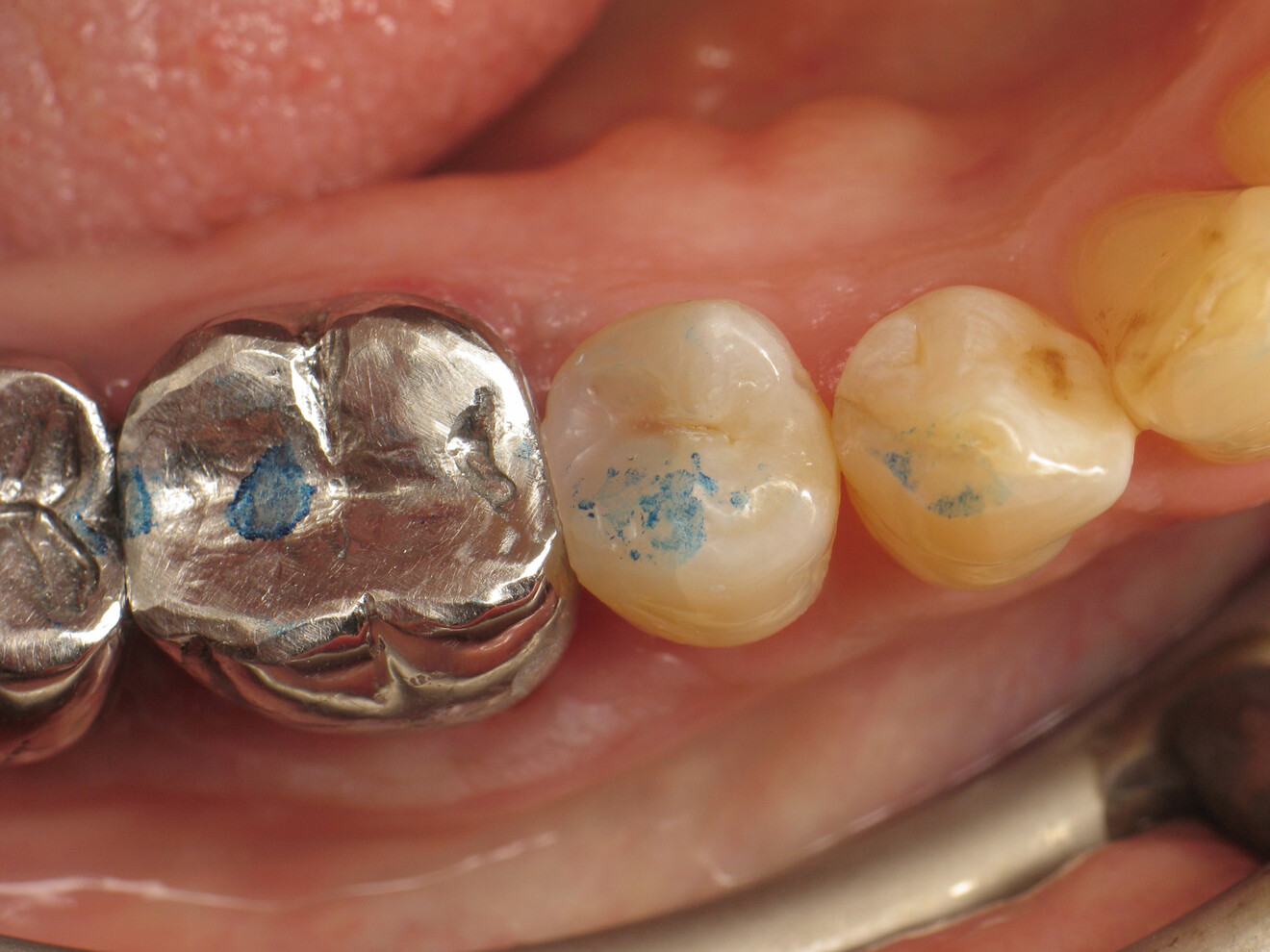
For the practitioner, the challenge lies in respecting the tooth’s natural anatomy and ensuring proper proximal contact points. If anatomical form is lacking, the aesthetics of the restoration will be compromised. Worse still, an inadequate contact point may lead to food impaction, causing discomfort, gingival inflammation and even caries. However, if the dentist succeeds in creating a satisfactory overall anatomical shape, the patient is more likely to retain the tooth in the long term.
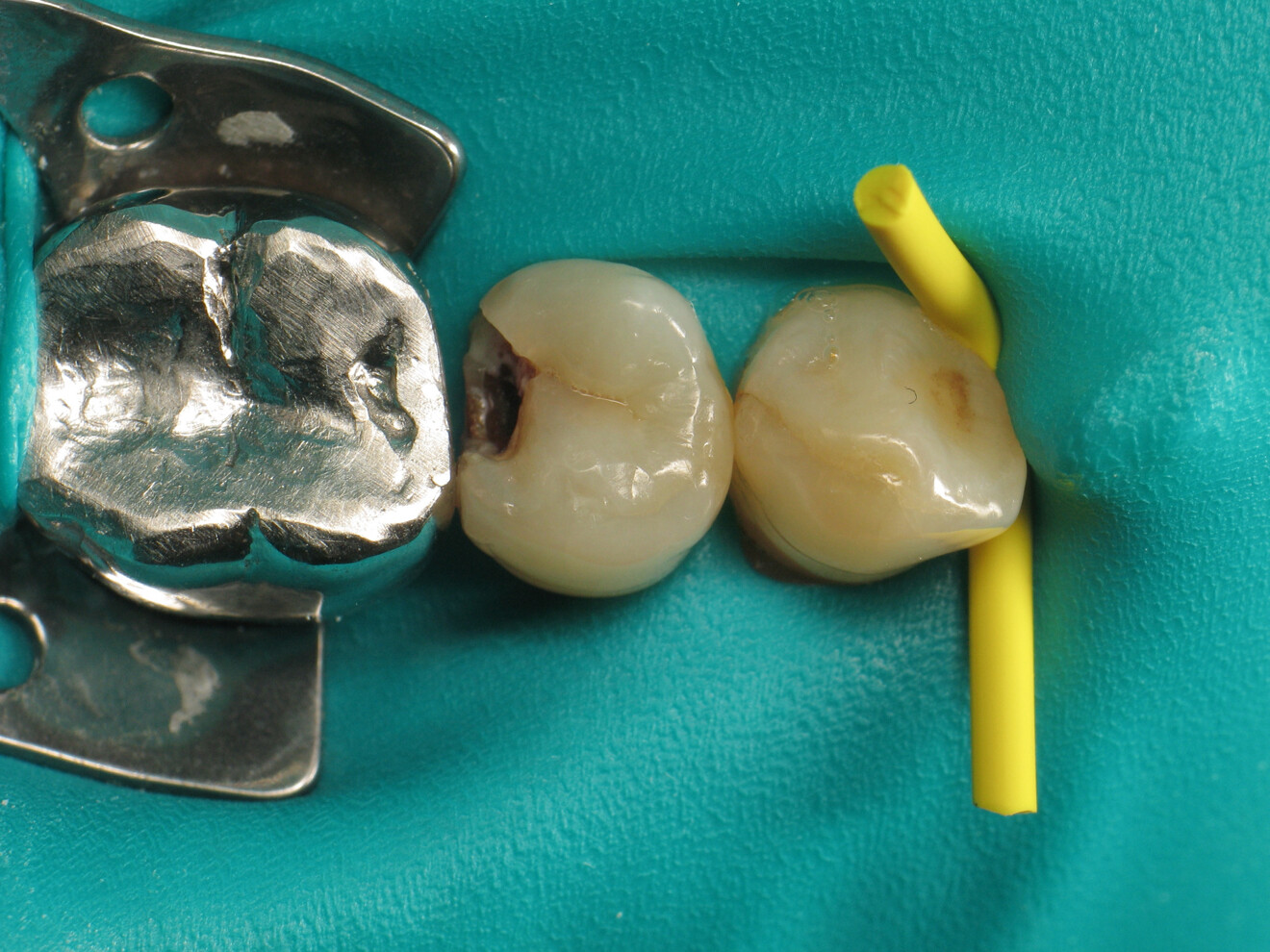
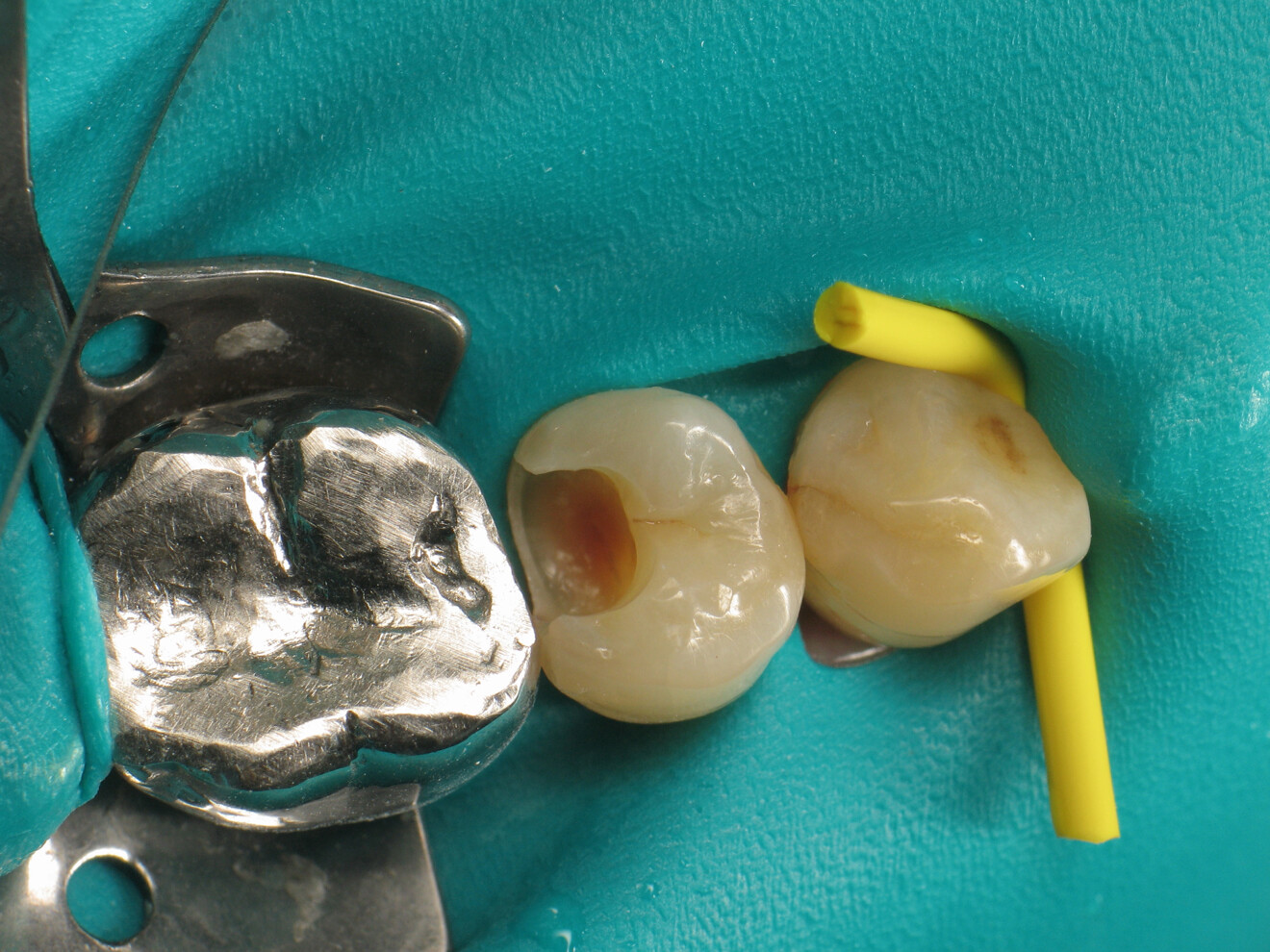
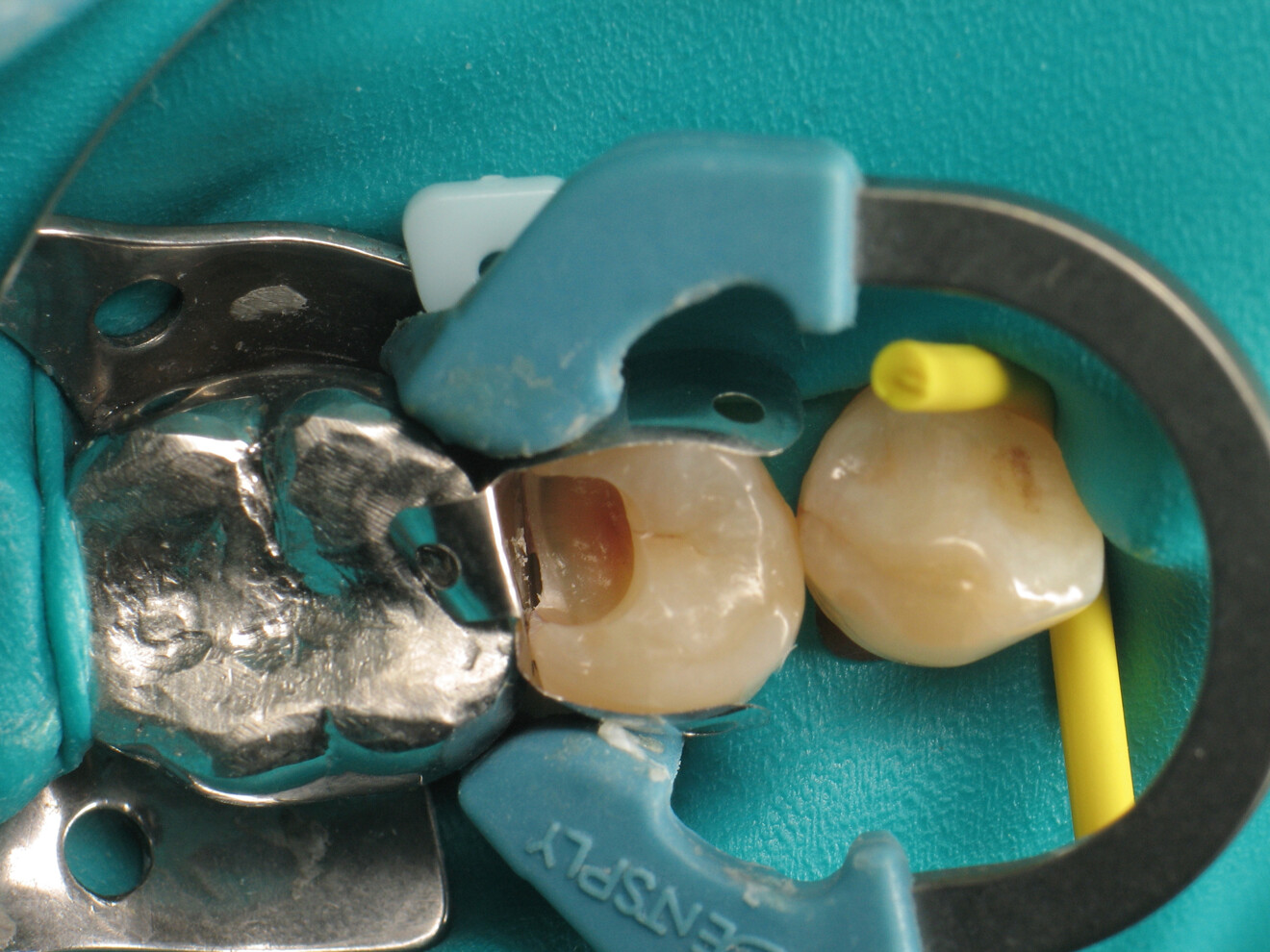
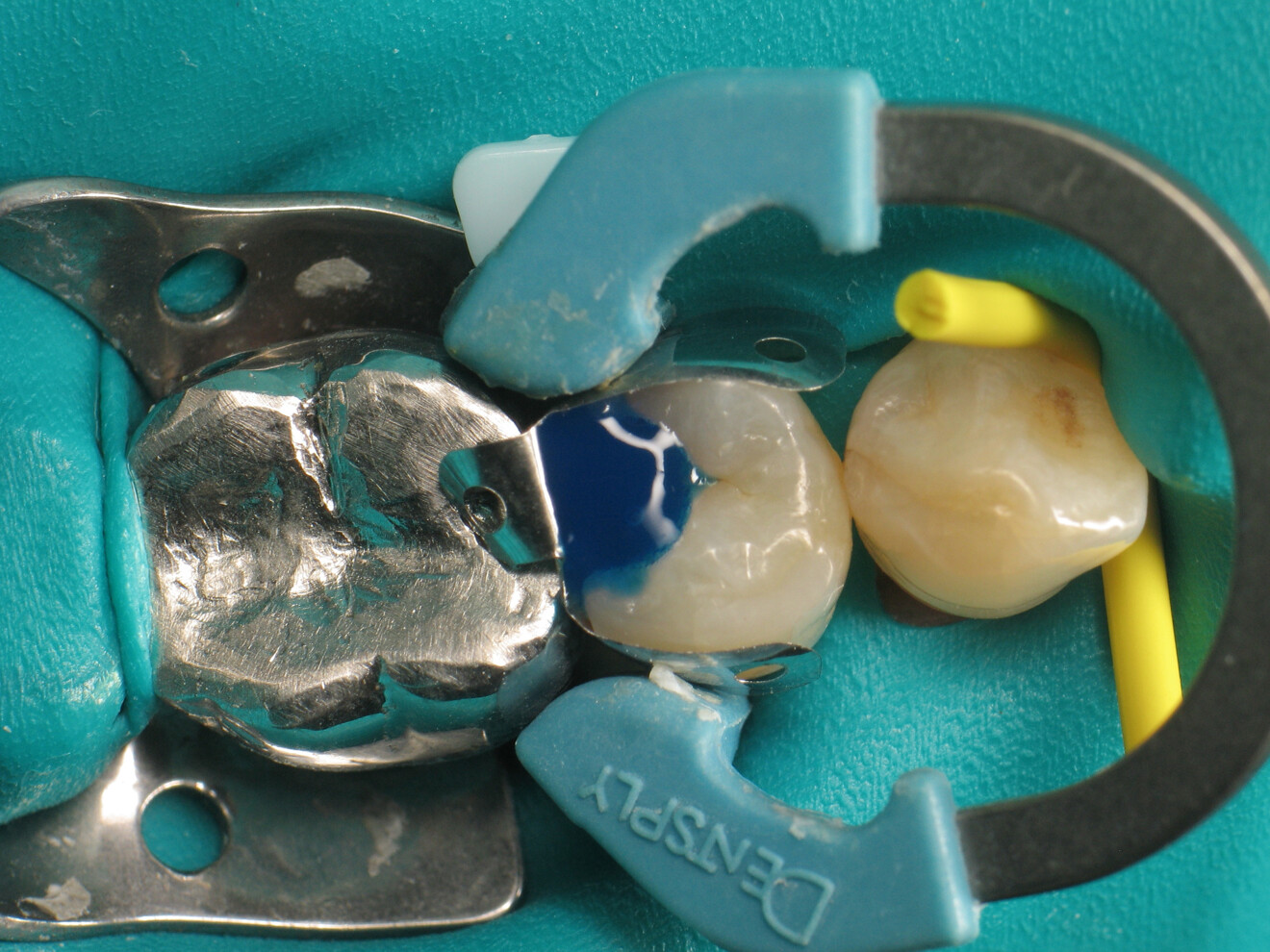
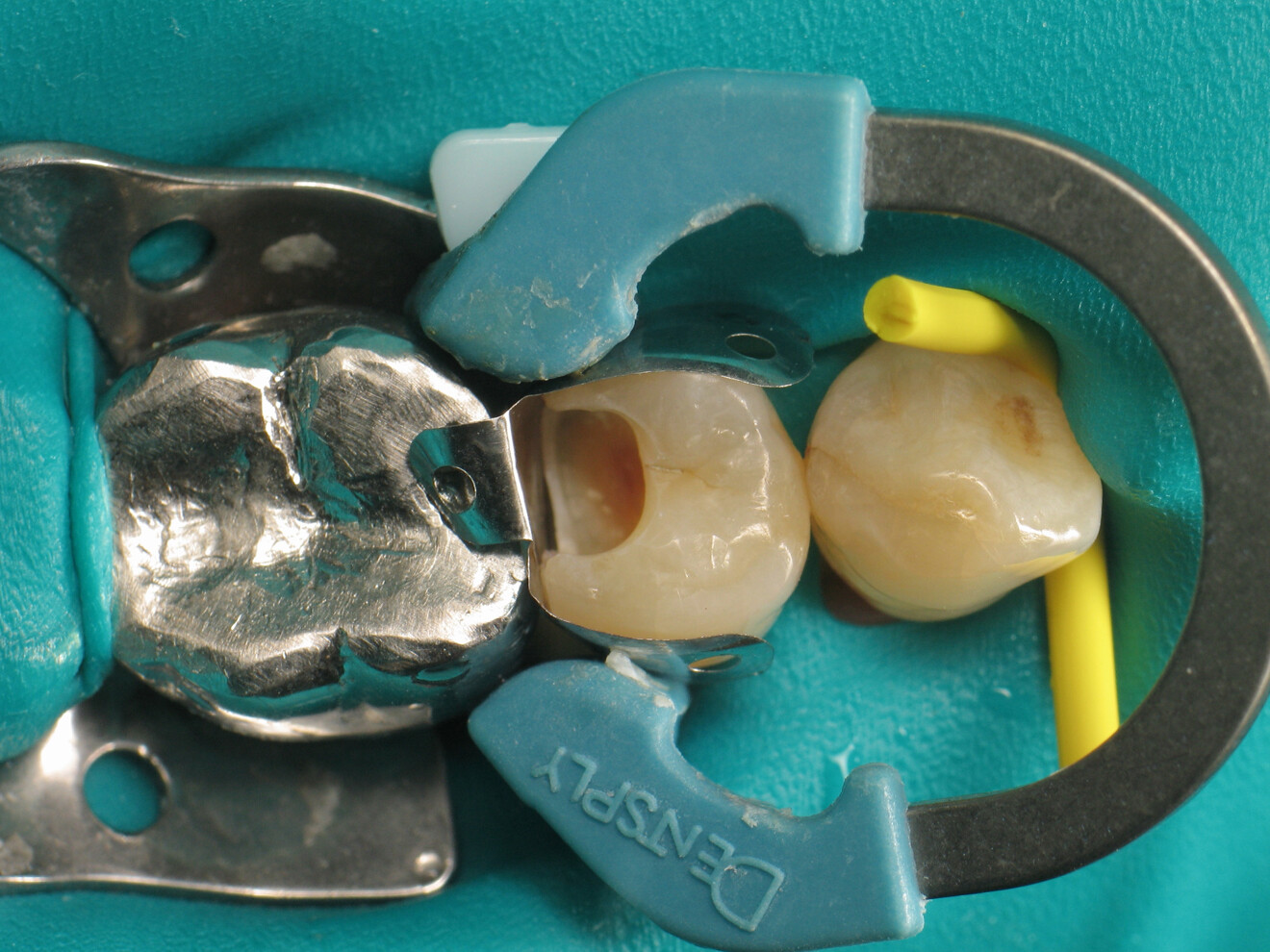
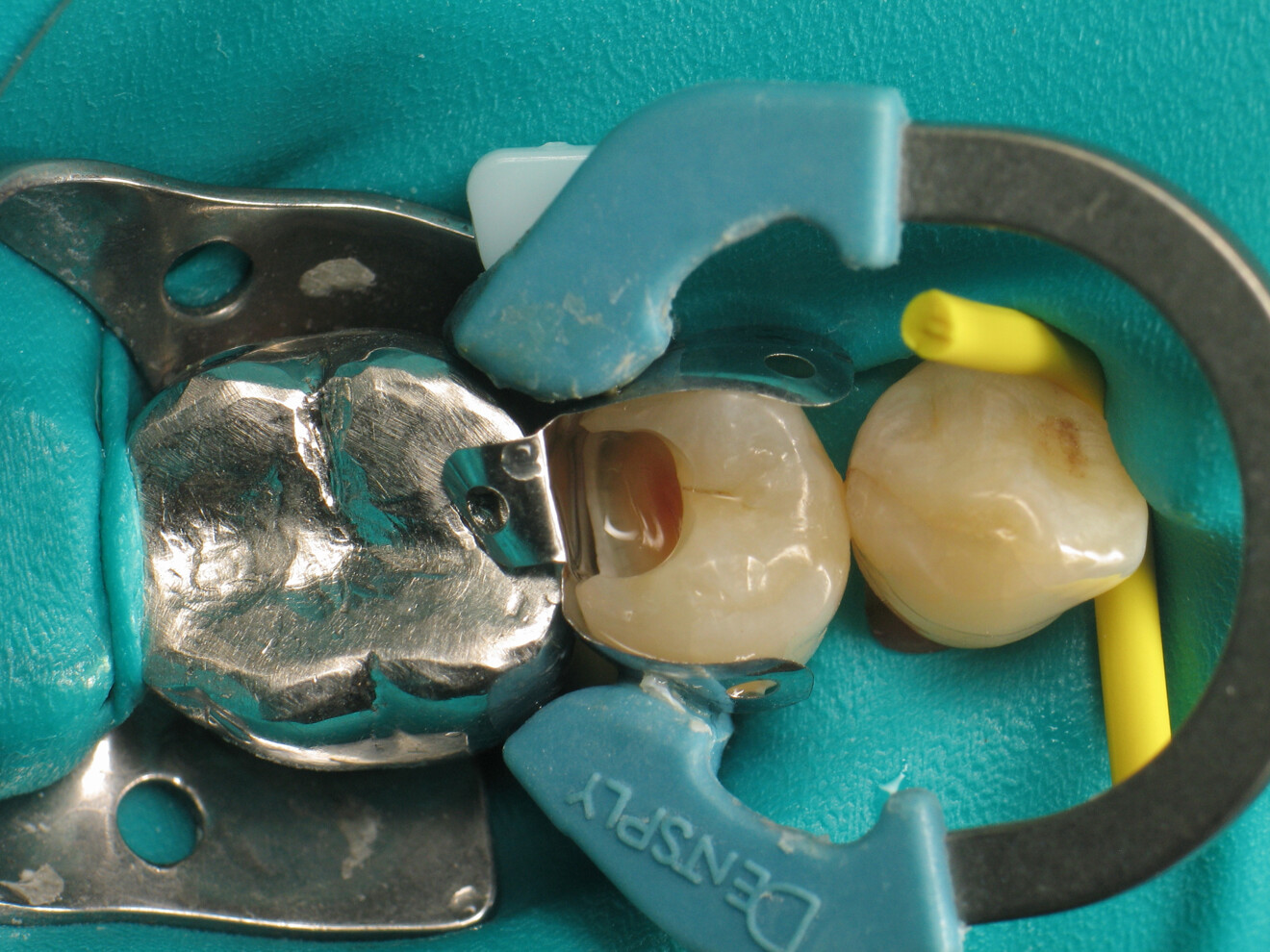
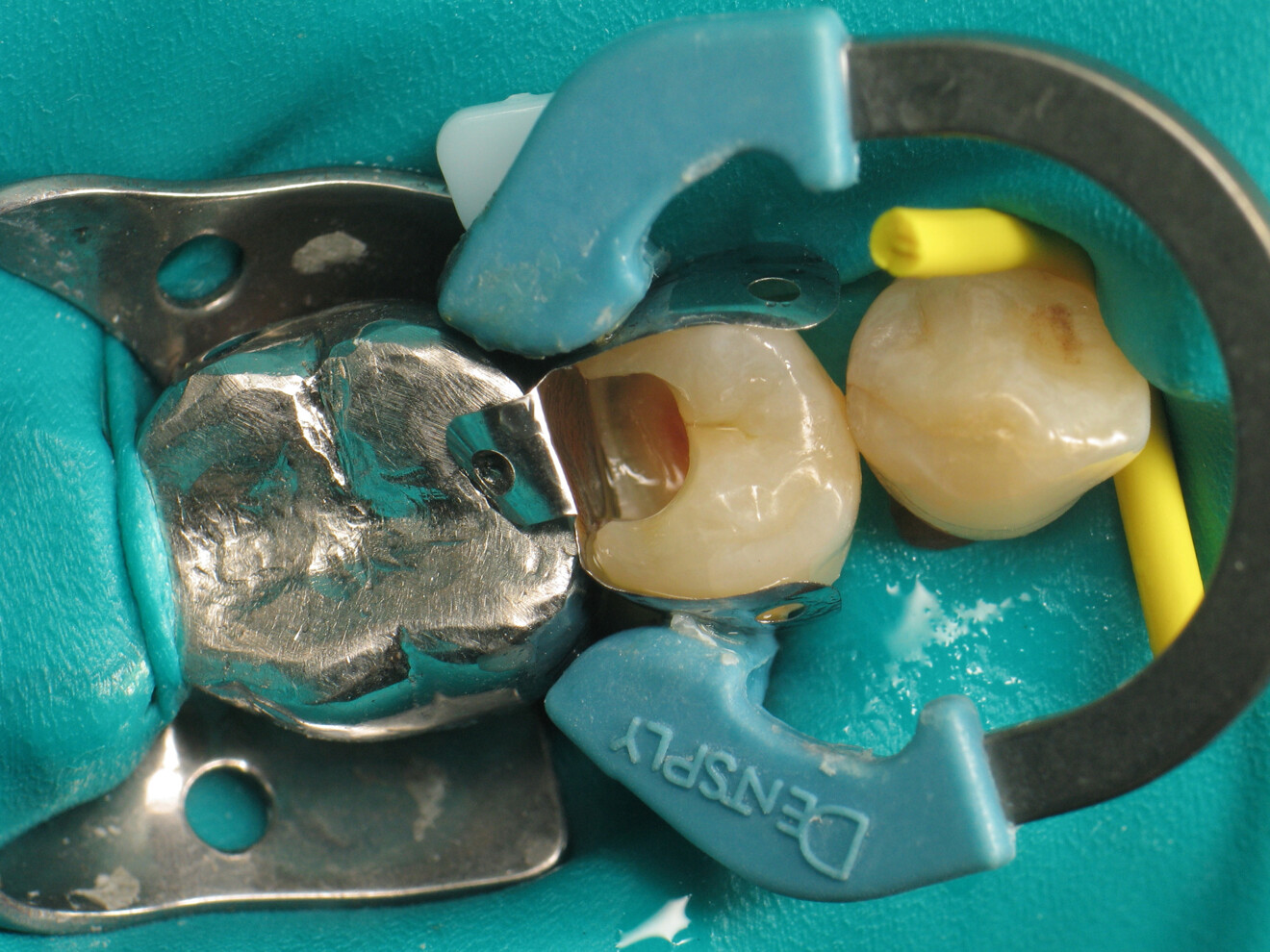
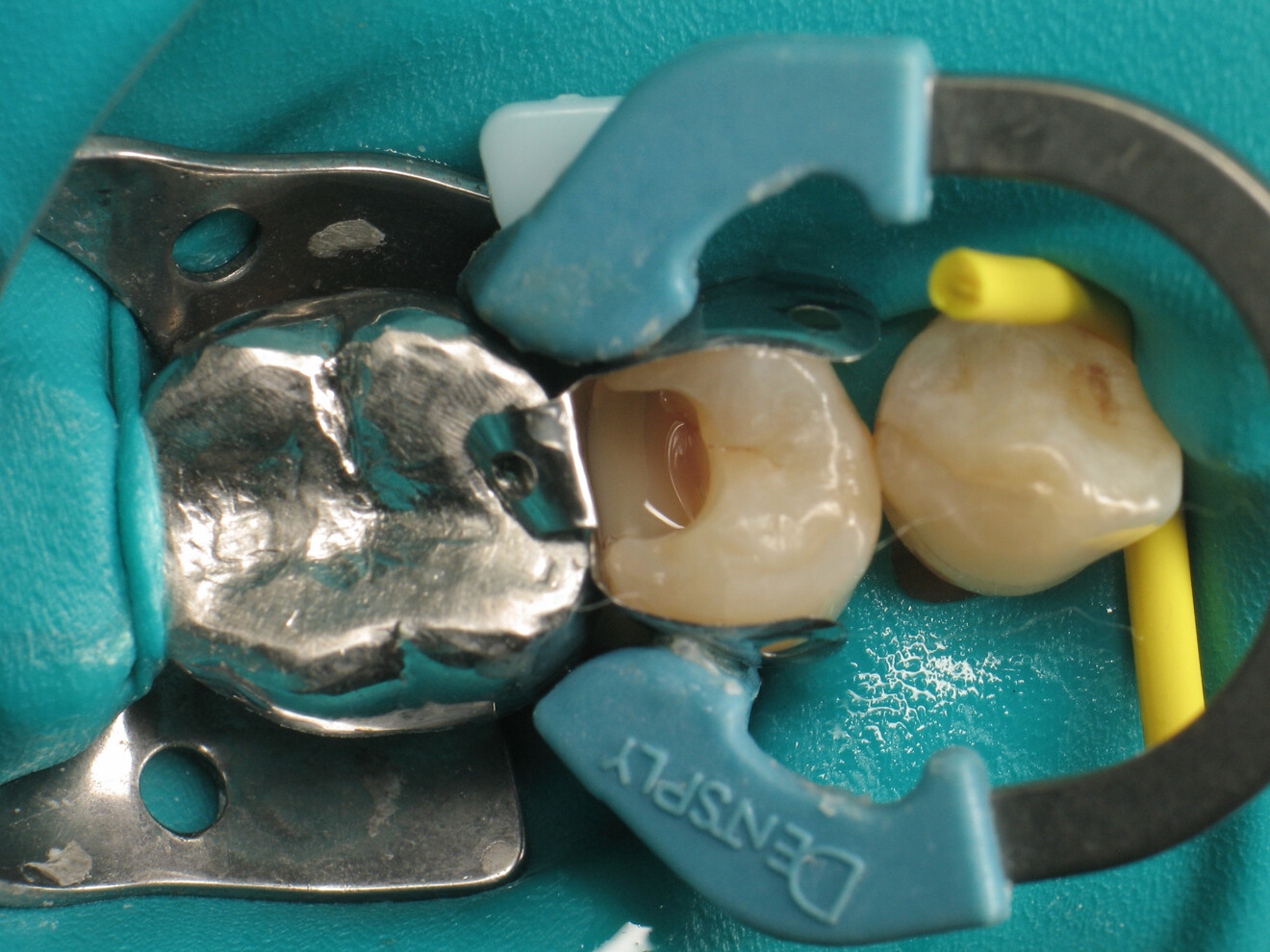
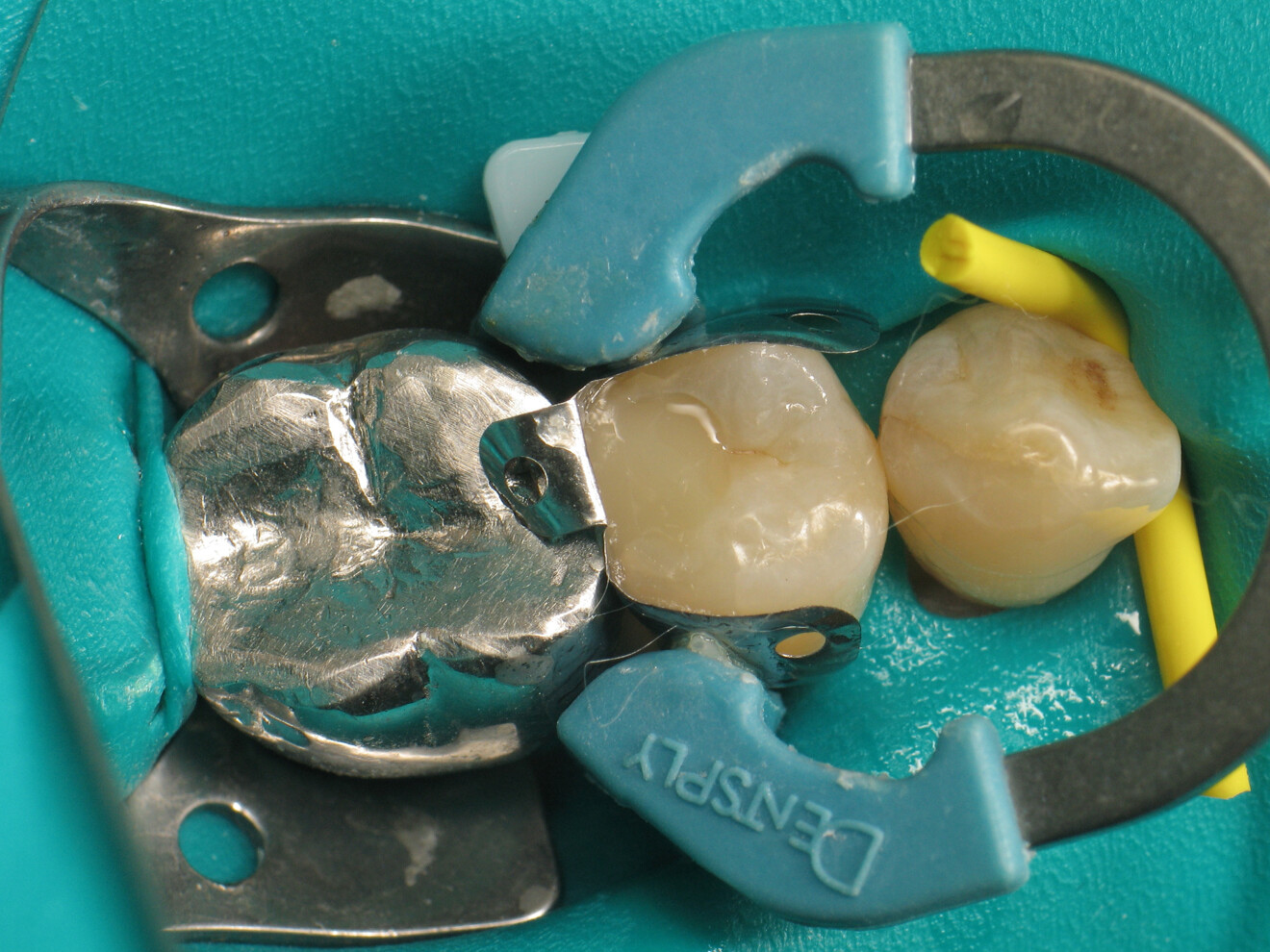
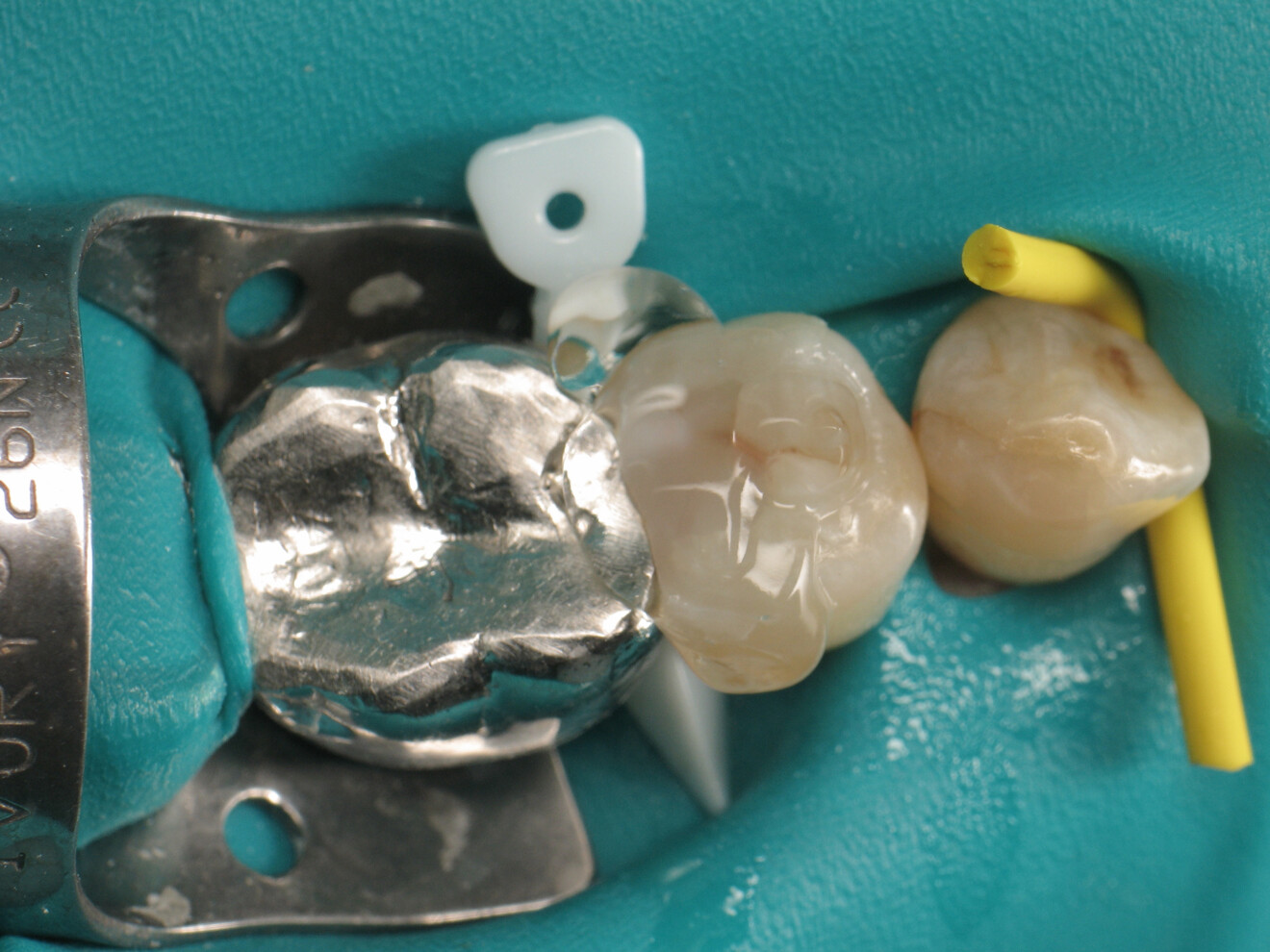
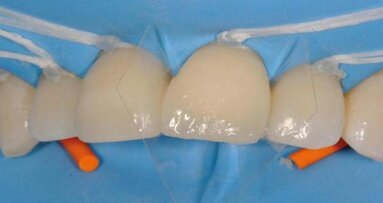
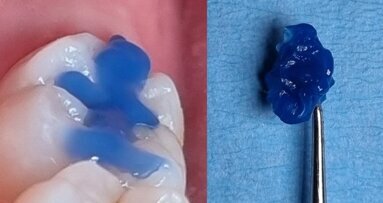
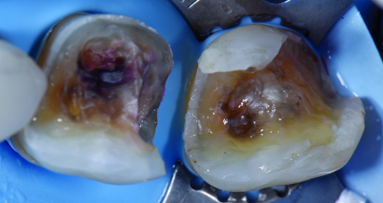
To achieve satisfactory anatomy and function, several elements must be considered: preparation, interdental separation and contouring. A matrix should be used to replicate the proximal wall destroyed by the carious lesion. Typically, a metallic matrix is used because it is malleable and does not adhere to the restorative material. The height of the matrix is crucial because, if it is too short, the seal will be compromised, and if it is too long, manipulation will be hampered by the gingival papilla. Interdental separation involves widening the interdental space using a wedge. Usually, the wedge is made of wood or plastic of various sizes. The size of the wedge is crucial because, if the wedge is too small, the contact point will be too loose, but if the wedge is too large, postoperative discomfort may occur. Contouring involves defining the general shape of the proximal surface of the tooth. A ring is typically used to press the matrix against the tooth and give the restoration a natural shape.
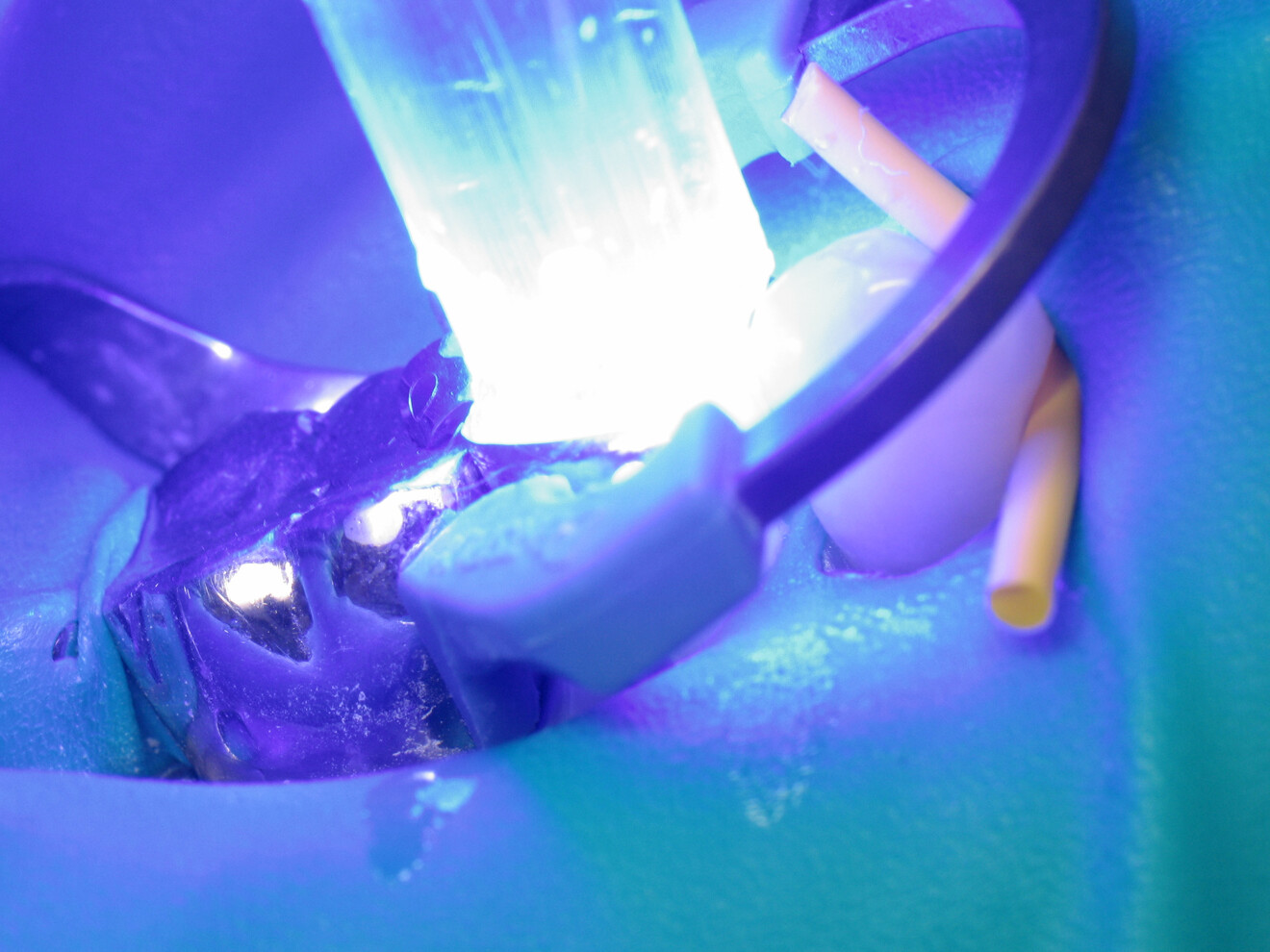
While all these steps are technical and time-consuming, they are essential for achieving a satisfactory Class II restoration. Fortunately for practitioners, the actual cavity filling can be quick and convenient. The use of a bulk-fill composite allows for single-step filling if the cavity depth does not exceed 4 mm. In addition, an initial layer may be applied to raise the cavity floor if needed.
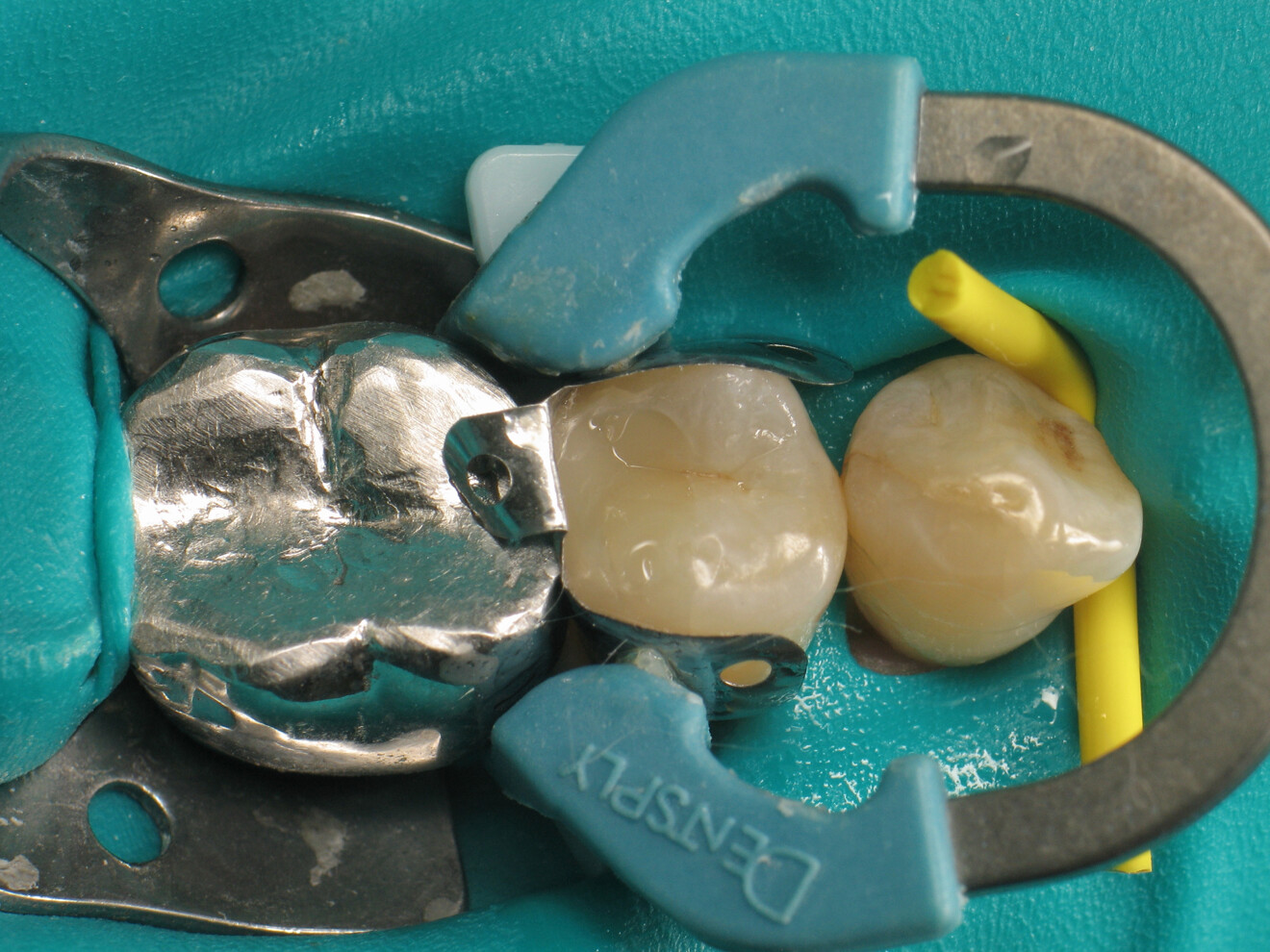
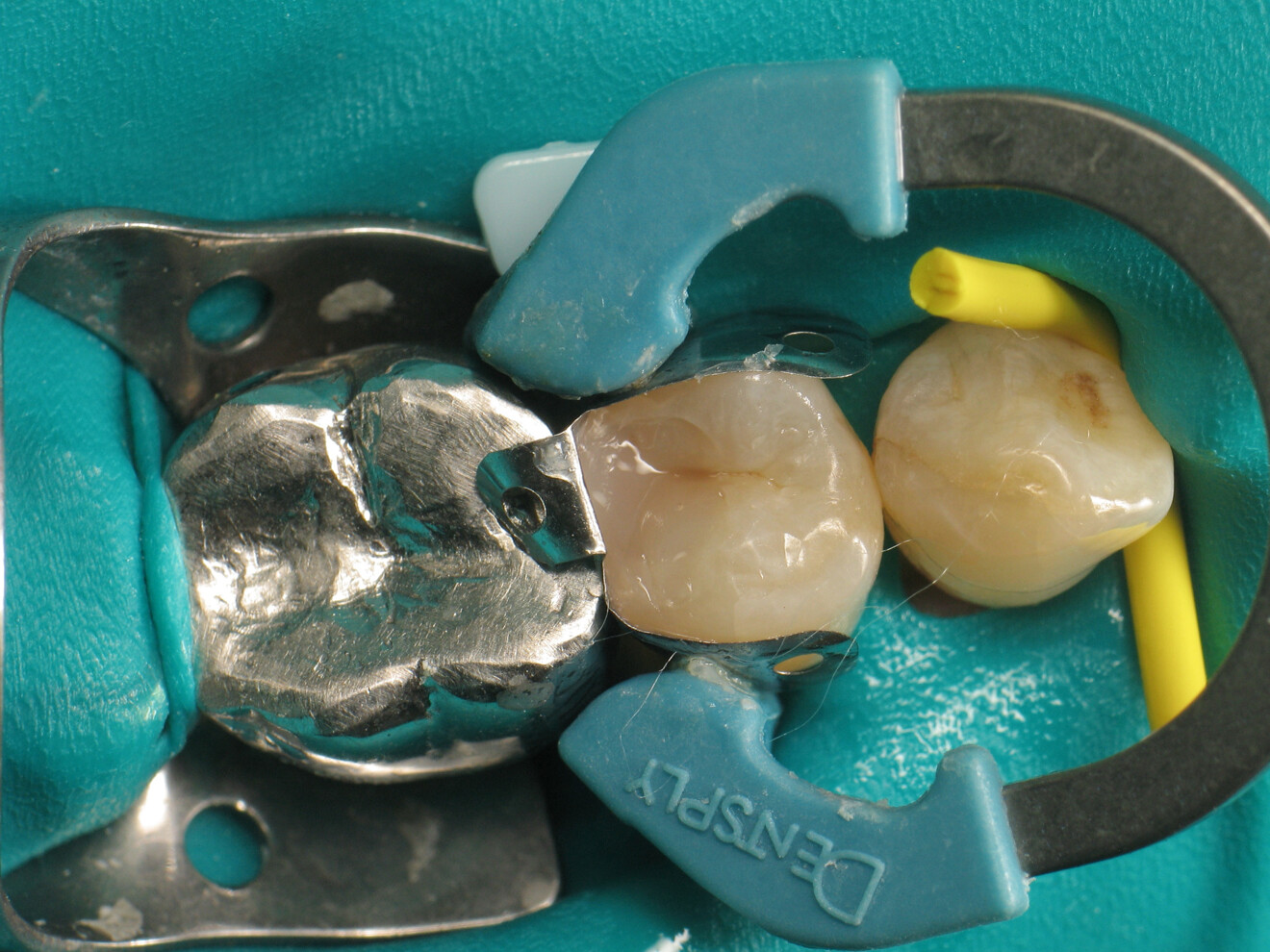
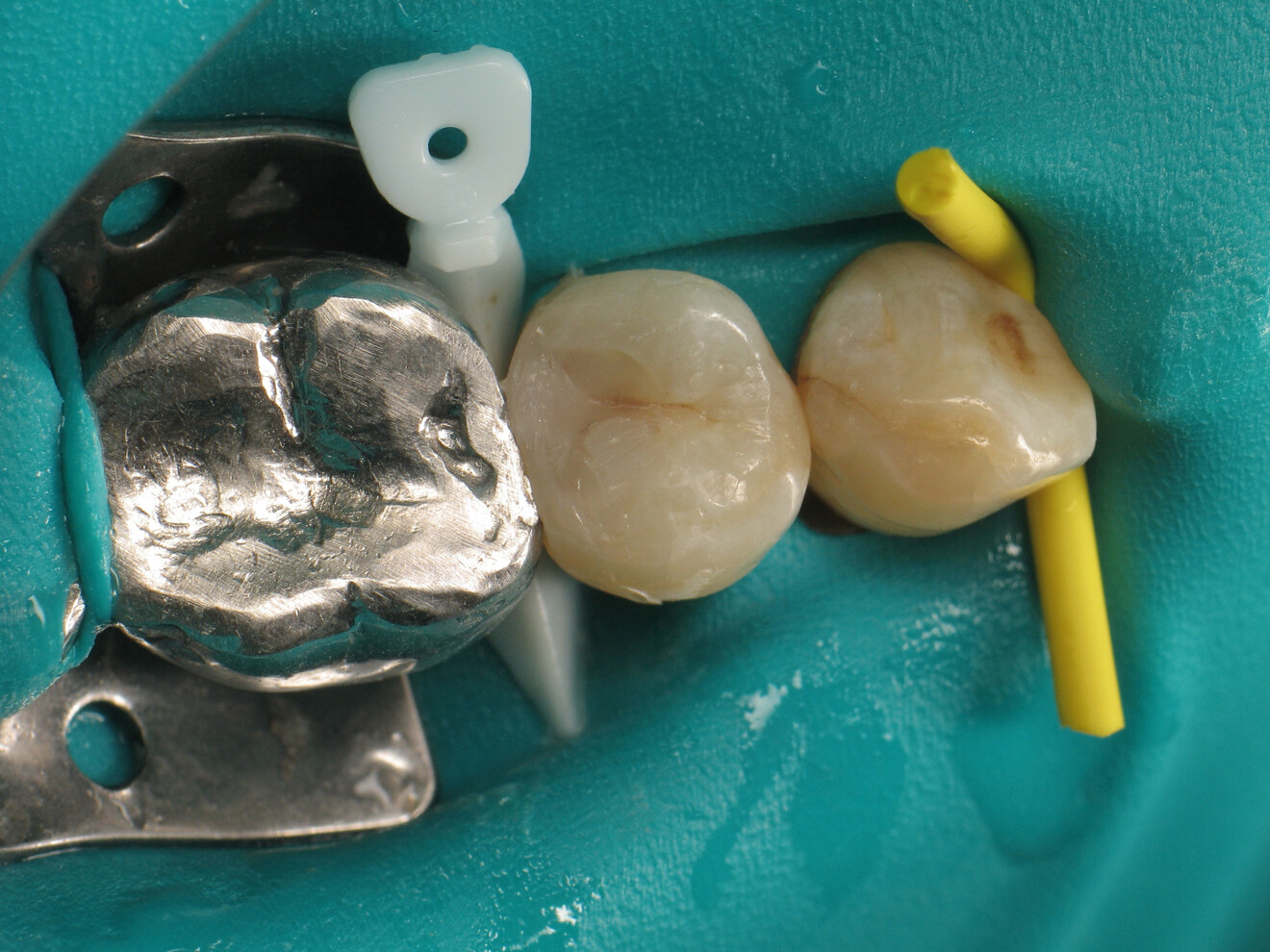
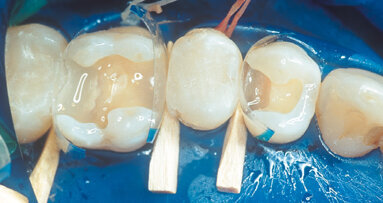
By using a thermo-viscous composite, the dentist can fully express the material’s aesthetic potential. It allows for an impressive level of anatomical detail using simple and readily available instruments. First, a probe can be used to carefully remove excess material and shape the general contours of the cusps. It is then possible to create pronounced intercuspal grooves and even define the cusp lobes using an endodontic file. These steps are straightforward and quick and result in a natural-looking restoration.
Conclusion
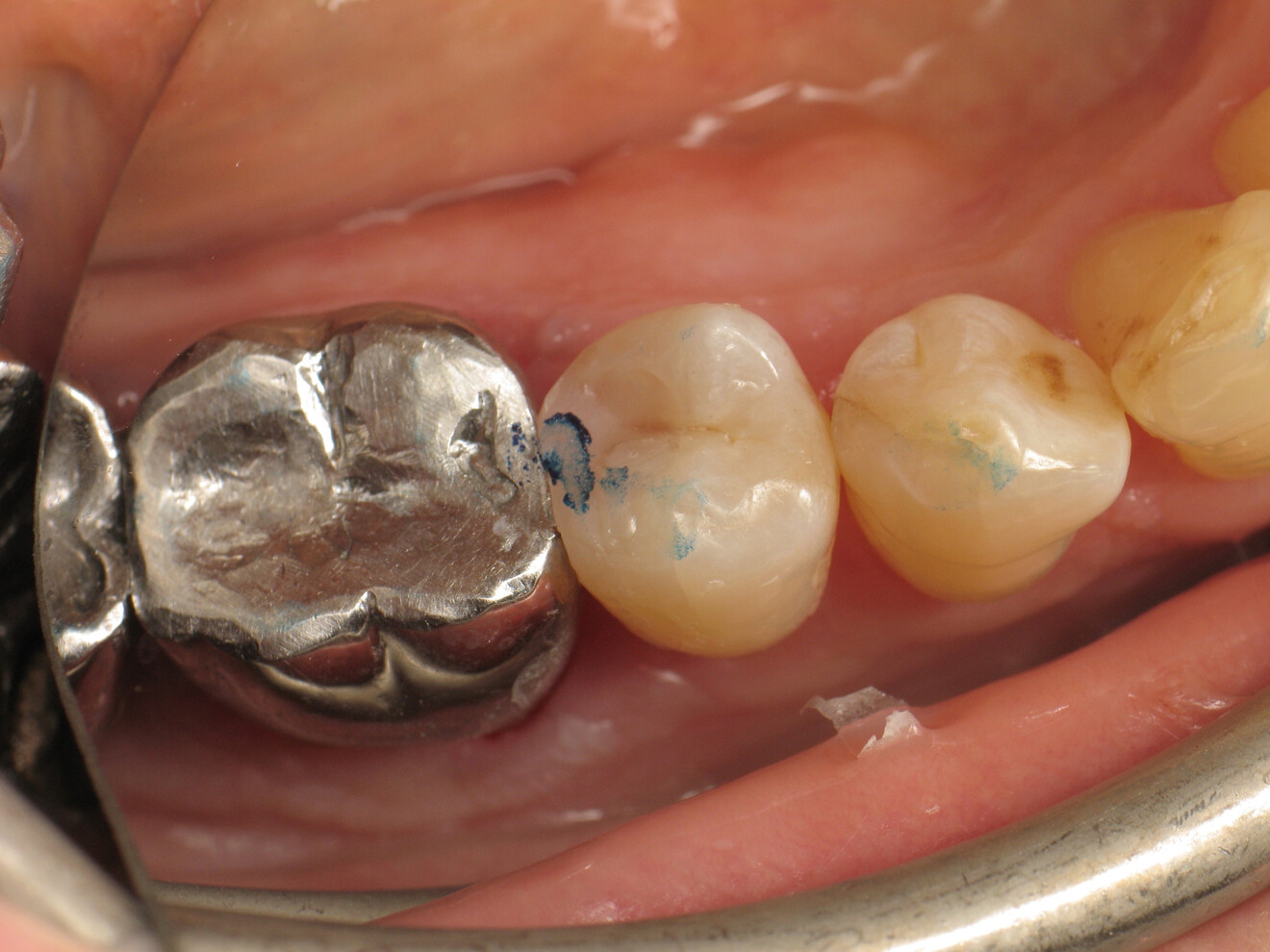
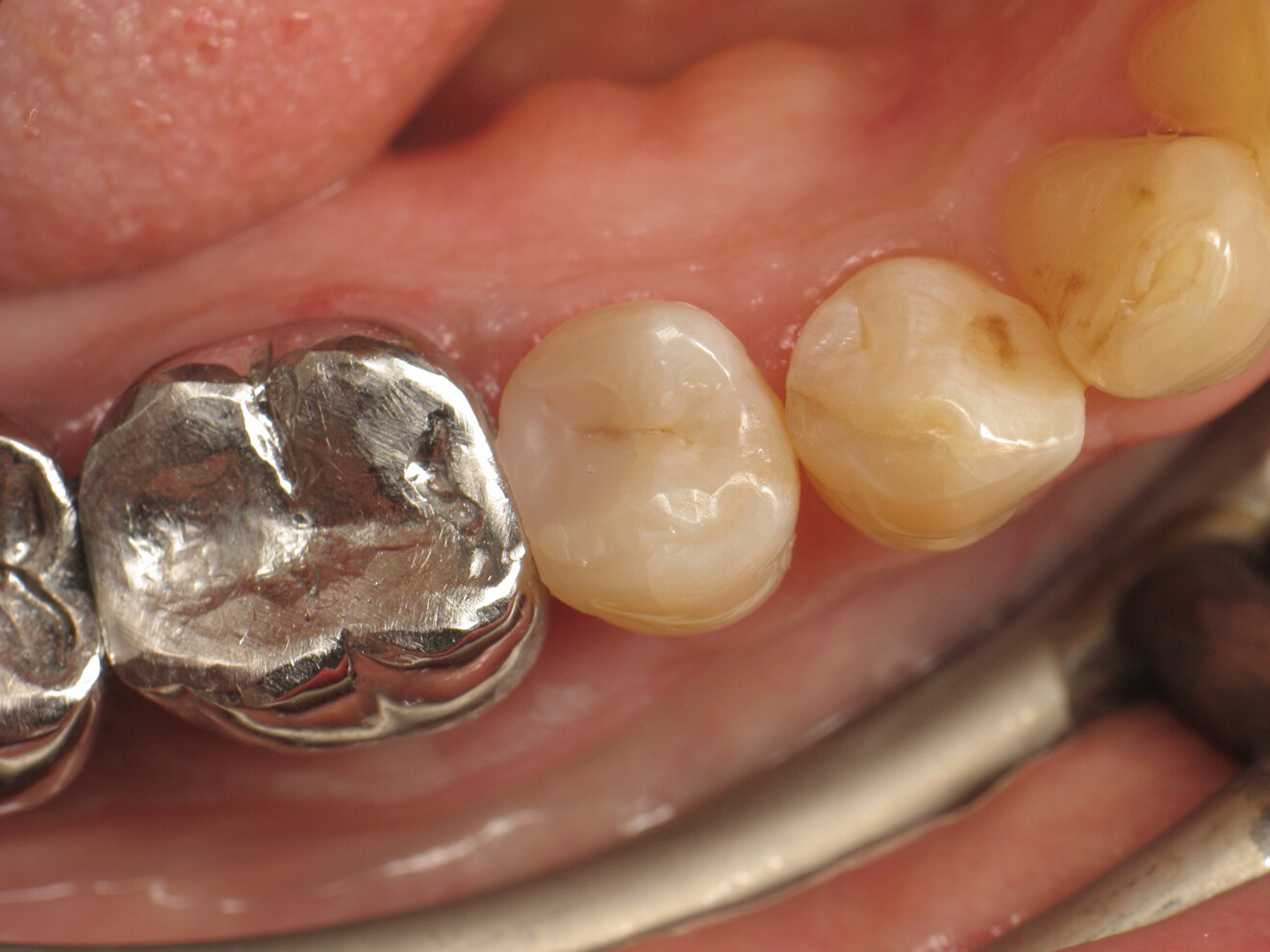
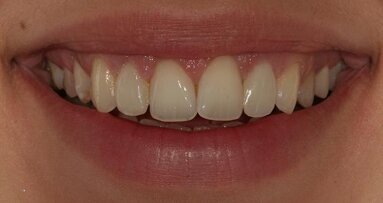
Proper Class II restoration requires restoration of the aesthetics and, above all, the function of the tooth affected by the carious lesion. The use of a thermo-viscous composite allows for establishing of a satisfactory contact point for the patient within a reasonable working time.
The patient was very satisfied with the treatment results and impressed by the aesthetics of the restoration, which was barely distinguishable from the natural tooth. Furthermore, she was able to floss without any difficulty.
Acknowledgements
I would like to thank Dr Matthias Mehring, VOCO’s knowledge manager, for the contribution of materials.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





























To post a reply please login or register