Minimally invasive treatments restore form, function and aesthetics with minimal removal of sound tooth structure. Understandably, the restorations age with the patient. Eventually, teeth that have been restored will break down and patients will need to have those restorations replaced.
Fortunately, restorative materials and procedures evolve constantly. If an initial restoration was created using minimally invasive procedures, there should be more tooth structure to work with when a second restoration is needed. The following case report demonstrates such a conservative approach.
Case report
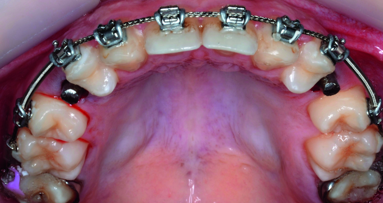
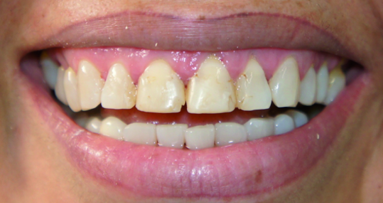
After orthodontic treatment, a 19-year-old female patient was dissatisfied with the unpleasant, disproportional appearance of her conoid maxillary lateral incisors. A direct composite technique was selected for smile enhancement at the initial appointment (Figs. 1–4).
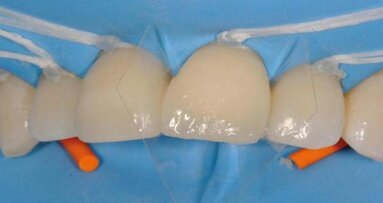
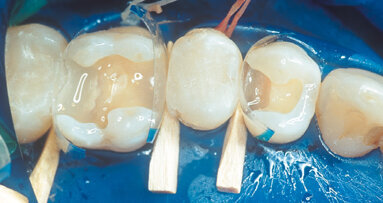
Following enamel-preserving preparation using a tapered, round-ended fine diamond bur and sand-blasting, a celluloid strip was placed subgingivally and fixed using flowable composite. This helped to create the desired emergence profile and contact points. Next, a retraction cord was inserted into the labial part of the gingival sulcus (Fig. 5).
embedImagecenter("Imagecenter_1_762",762, "large");
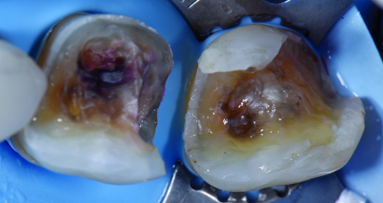
After isolation of the operative field, the preparation was etched with 37% phosphoric acid for 30 seconds, then thoroughly rinsed and dried. Subsequently, a fifth-generation bonding agent was applied and light cured (Fig. 6).
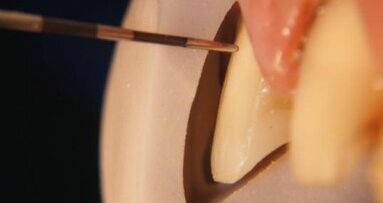
The next step entailed creating palatal and two lateral enamel walls that were completed using increments of enamel-shade resin. Creating a lingual shelf in this manner left room for the subsequent dentine layering (Fig. 7).
The appropriate dentine-shade resin was then applied in order to create distal and mesial lobes. These were light cured for ten seconds (Fig. 8). Dentine in a darker shade was placed onto the cervical third. Prior to light curing, the white strip was painted horizontally along the incisal edge of the enamel shelf using a white tint and smooth brush (Fig. 9). Finally, an enamel resin layer was placed, contoured, smoothed with a brush and light cured (Fig. 10).
After completion of composite applications and polymerisation, fine flame-tipped finishing diamond burs and Sof-Lex discs (3M ESPE) were used for gross contouring and creating texture. The final polish was achieved using rubber finishers, a brush, a felt wheel and a paste kit (Fig. 11).
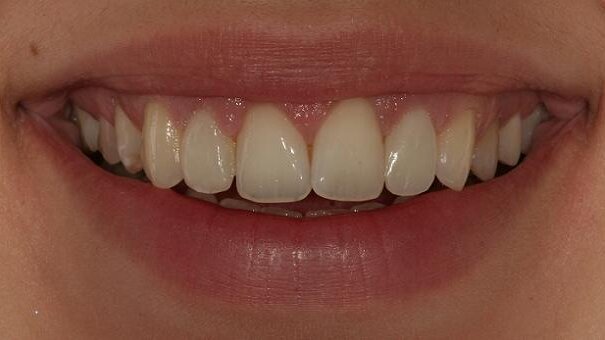
The same procedures were followed during reconstruction of the left lateral incisor (Figs. 12 & 13). Figures 14 to 16 show the situation 30 days post-operatively. The lateral incisors show favourable integration of form and colour as achieved through the direct composite resin restoration procedure. Adequate contours and proportions create a smile with harmonious symmetry and a natural appearance.
Some cases present with conoid lateral incisors displaying a lack of gingival harmony, as was the case with this patient (Figs. 17 & 20). This usually manifests as the translocation of the gingival contour coronal to the zenith of the canine and the central incisor. Such a clinical situation requires gingival recontouring before direct restoration.
In the case presented, the recontouring procedure was carried out using a Soft Tissue Trimmer bur (Edenta). Modifications were limited by the patient’s biologic width. As observed at four-week follow-up visits, there was a very good gingival response to the polished restorations (Figs. 19 & 21).
Conclusion
Conoid lateral incisors are not uncommon. They may be found unilaterally or bilaterally. Their poor appearance can spoil an otherwise attractive smile. The case presented describes a minimally invasive way of addressing this problem using direct composite bonding. The step-by-step images illustrate how dentists can solve this cosmetic issue without using aggressive techniques and with the advantage of being in full control of shade matching and characterisation.
This article was published in Cosmetic Dentistry_beauty & science No. 1/2013.
The purpose of this article is to show the diferent modalities of treatment for upper lateral incisors agenesis. In daily practice, orthodontists often meet...
For many years, the trend in restorative dentistry has been to place only one- or two-shade composite restorations in daily practice. However, with this ...
The restorative dental treatment possibilities available to practicing dentists have grown immensely over the past few decades. Considerable progress has ...
It is widely accepted that in order to obtain highly aesthetic results, detailed treatment planning is mandatory in order to schedule the various stages of ...
It is widely accepted that in order to obtain highly aesthetic results, a detailed treatment planning is mandatory, to let us schedule the different stages ...
For reasons of cost, patients and dentists today often find themselves obliged to use restorative materials for the treatment of large structural, ...
Aesthetic dentistry is featured widely in the media as the field of dentistry that can change or enhance the appearance of the face, leading to an improved ...
The second most common dental agenesis is that of the maxillary lateral incisors, after agenesis of the mandibular third molars.1 This common agenesis has ...
In an earlier article on this topic,1 I demonstrated the workability of thermo-viscous composites. After warming, the composite can be easily handled for ...
Faced by a missing lateral incisor, practitioners often consider a wide range of issues and are also faced by numerous treatment options:
1. in a young ...
Live webinar
Fri. 22 May 2026
10:00 am EST (New York)
Dr. Paweł Aleksandrowicz PhD
Live webinar
Fri. 22 May 2026
11:00 am EST (New York)
Live webinar
Fri. 22 May 2026
12:00 pm EST (New York)
Prof. Dr. Ali Murat Kökat
Live webinar
Fri. 22 May 2026
1:00 pm EST (New York)
Live webinar
Fri. 22 May 2026
2:00 pm EST (New York)
Live webinar
Tue. 26 May 2026
12:00 pm EST (New York)
Live webinar
Tue. 26 May 2026
2:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East























To post a reply please login or register