The terminology and classification of incomplete tooth fractures have received significant attention in the scientific literature for many decades. Numerous terms and definitions have been proposed through the years, arising from the difficulties related to diagnosis, prognosis assessment and treatment planning.
Cuspal fracture (Gibbs 1954), fissure fracture (Thoma 1954), fissural fracture (Down 1957), crack lines and greenstick fracture (Sutton 1961; 1962), cracked tooth syndrome (Cameron 1964), hairline fracture (Wiebusch 1972), split-root syndrome (Silvestri 1976), enamel infraction (Andreasen 1981), crack lines and craze lines (Abou-Rass 1983), and incomplete tooth fracture (Luebke 1984) are some of the terms used through the years. Many of these terms were used by different authors to describe the same clinical entity.
Recently, the American Association of Endodontists categorised longitudinal tooth fractures into five major classes:
- craze line;
- fractured cusp;
- cracked tooth;
- split tooth; and
- vertical root fracture (VRF).
Craze lines affect only the enamel, originate on the occlusal surface, are typically from occlusal forces or thermo-cycling, and are asymptomatic.
A fractured cusp is defined as a complete or incomplete fracture initiated from the crown of the tooth and extending sub-gingivally, usually directed both mesiodistally and buccolingually.
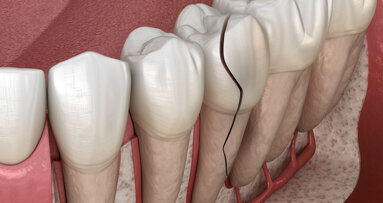
A cracked tooth is defined as an incomplete fracture initiated from the crown and extending sub-gingivally, usually directed mesiodistally.
A split tooth is defined as a complete fracture initiated from the crown and extending sub-gingivally, usually directed mesiodistally through both of the marginal ridges and the proximal surfaces.
A true VRF is defined as a complete or incomplete fracture from the root at any level, usually directed buccolingually.
Cracked teeth are thought to occur as a result of para-functional habits or weakened tooth structure. The fractures are incomplete, tend to present in a mesial-to-distal orientation, and are generally centred on the occlusal table. The symptoms that develop subsequent to these cracks have been termed “cracked tooth syndrome”. This has been described as acute pain that results during the mastication (or release) of small, hard food substances and is exacerbated by cold. However, the signs and symptoms of a cracked tooth may also be consistent with an irreversible pulpitis or necrosis.
Based on the available literature and investigations on root cracks and fractures, it has been suggested that the endodontic prognosis for teeth with these types of cracks is poor, with a high potential for unfavourable post-treatment sequelae.
In their paper, Berman and Kuttler (2010) conclude that pulp necrosis, in the absence of extensive restorations, caries or luxation injuries, is likely caused by a longitudinal fracture extending from the occlusal surface and into the pulp. They suggest, based on the available literature, that these types of teeth may have a poor prognosis after endodontic treatment, with the potential ramification of extensive periodontal and/or periapical bone loss. They therefore suggest extraction as the primary treatment option.
Although this conclusion appears reasonable enough, it should be noted that the detection of the incomplete fracture line limits before proceeding to the extraction of a longitudinally fractured tooth is of outmost importance.
The detection of incomplete longitudinal fractures is a challenging task that is very often neglected. Generally, a combination of simple inspection, transillumination, staining with dyes, diagnostic surgery, microscopy and a cone-beam computerised tomography scan is necessary to identify and confirm the presence of cracks. The extraction of cracked teeth without identifying and documenting the fracture line limits is unjustifiable according to the author.
The aim of the present case report is to demonstrate the importance of the diagnostic procedures in the prognosis and treatment planning of incompletely longitudinally fractured teeth.
embedImagecenter("Imagecenter_1_676",676, "large");
Case report
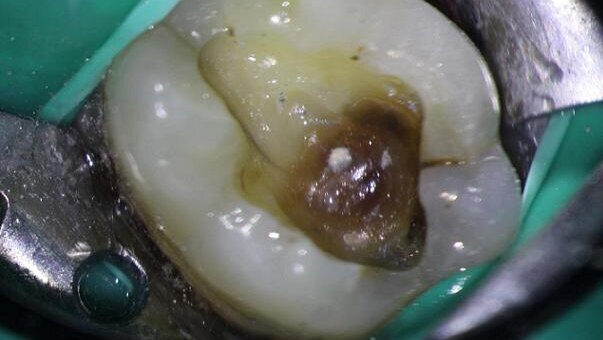
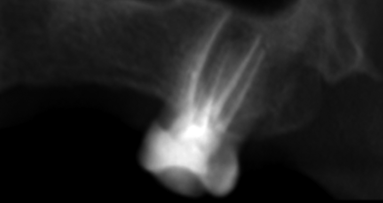
A 30-year-old male patient was referred to our endodontics practice for the evaluation and possible treatment of his mandibular left first molar. The referral note mentioned a possible diagnosis of VRF and suggested the extraction of the tooth, followed by grafting and implant placement. The patient’s medical history was non-contributory. There was no history of trauma and no para-functional habits were identified. There was a buccal swelling in the furcation area and the tooth was percussion sensitive. The referring dentist had removed the amalgam restoration and placed a temporary filling material. Cold and electric vitality tests were negative. There was a deep buccal periodontal probing defect. The clinical view of the mandibular left first molar can be seen in Figure 1a. The radiographic examination revealed an extensive periapical lesion extending through the furcation area (Fig. 2a).
The clinical and radiographic image indicated an incomplete longitudinal fracture necrosis with an associated extensive endodontic-periodontal defect. A decision was made to seek to identify the fracture line in order to assess the restorability of the tooth.
After administrating infiltration anaesthetic, a rubber dam was placed. The temporary filling material was removed and the underlying dentine was stained with methylene blue dye (Figs. 1b & c). A fracture line was detected, extending from the mesial marginal ridge across the dentinal structure to the distal marginal ridge (Figs. 1c & d). The pulp chamber was accessed in order to determine the extent of the fracture line. Upon accessing the pulp chamber, the pulp floor calcifications were removed with ultrasonics under the microscope (Fig. 1e). The pulp floor and the axial dentinal walls were stained again with methylene blue dye and inspected under the microscope (Fig. 1f). No fracture lines or cracks were detected across the pulp floor, while the mesial and the distal fracture line appeared to end before entering the mesiobuccal and the distal root-canal orifices.
The fractured tooth was judged as treatable and restorable. Standard non-surgical root-canal treatment was accomplished under the microscope and the tooth was restored using a dual-cured composite resin build-up.
Shaping of the canals was accomplished using the HyFlex CM rotary files (Coltène/Whaledent) and cleaning of the canals was achieved according to a strict irrigation protocol. The irrigation protocol followed entailed syringe irrigation with a 6% NaOCl solution with surface modifiers (CanalPro, Coltène/Whaledent). The irrigation solution was activated with a #15 ultrasonic K-file (SATELEC) after the completion of the shaping procedures (3 x 20 seconds per canal). The canals were dried with paper points and flooded for five minutes with a 17% EDTA solution (CanalPro). The final rinse was achieved using sterile water.
The canals were dried again and were flooded for another five minutes with a 2% chlorhexidine solution (Vista Dental). The canals were rinsed again with sterile water and were dried with sterile paper points (Roeko Cellpack, Coltène/Whaledent).
The obturation of the canals was achieved using the continuous wave of condensation technique plus injectable thermo-plasticised gutta-percha backfilling.
The pulp floor chamber was cleaned through sodium bicarbonate sand-blasting (Fig. 1g) and the orifices were covered with flowable dual-cured composite resin under the microscope. The build-up was accomplished using dual-cured composite resin and the occlusion was adjusted. The radiographic image of the tooth after the completion of the root-canal treatment and the build-up can be seen in Figures 2b and c.
The tooth was monitored for one year. The one-year follow-up radiograph revealed uneventful healing (Fig. 2d). The periodontal probing was within normal limits all around the tooth and the clinical view was favourable (Figs. 1h & i).
The patient was referred back to his prosthodontist for full-coverage crown protection. The prognosis of this case was judged as excellent.
Discussion
The diagnosis, prognosis assessment and treatment planning of cases with incomplete longitudinal fractures can be really challenging. These fractures are very difficult, if not impossible, to identify in the 2-D periapical radiograph. The 3-D small field of view CBCT scan provides far more information. However, even with the CBCT scan, the incomplete fractures might remain undetectable.
The clinical identification of the fracture lines and their extent throughout the tooth structure is generally a difficult task.
According to the author, the operating microscope is an indispensable aid for the detailed assessment and documentation of incomplete fractures.
A combination of microscopic inspection, trans illumination, staining with dyes and diagnostic surgery is what it takes to identify incomplete fractures properly.
The treatment planning of cases with incomplete fractures should not rely on hypothesis, but should always rely on microscopic diagnosis and documentation. Not every single case of a cracked tooth needs extraction. The extraction of incompletely fractured teeth without assessing and documenting the extent of the fracture line is unjustifiable.
Besides adequate knowledge of root canal morphology in general, it is of utmost importance to evaluate each individual case for aberrant anatomy and to ...
LONDON, England: Balanced nutrition is known to lower the risk of major non-communicable diseases, including cardiovascular disease, neurodegenerative ...
KUOPIO, Finland: A study by researchers in Finland and the UK has found that self-reported daily smokers had a higher incidence of deepened periodontal ...
INDIANAPOLIS, US: Despite advances in periodontal disease research and treatments, it remains a growing health issue in the US. To address this topic, ...
Objective: The patient’s awareness and knowledge of periodontal disease is a key factor for successful periodontal treatment. The objective of this ...
This was a challenging case with the combined issues of a failed root canal therapy and an iatrogenic perforation of the floor of the pulp chamber. Though ...
A vertical root fracture (VRF) is a longitudinally oriented fracture of the root that, depending on its cause, can originate from the apex and propagate to ...
Dr Elizabeth Himel’s path in dentistry is shaped by heritage and guided by a strong sense of purpose. From taking over her father’s private practice to ...
Hypertrophy of the masseter muscle is defined as the excessive growth of muscle mass in the transverse direction and is more common between the second and ...
Implant treatment has evolved into a reliable modality for the replacement of missing teeth. Although rare, complications may occur, and some uncertainty ...
Live webinar
Fri. 22 May 2026
10:00 am EST (New York)
Dr. Paweł Aleksandrowicz PhD
Live webinar
Fri. 22 May 2026
11:00 am EST (New York)
Live webinar
Fri. 22 May 2026
12:00 pm EST (New York)
Prof. Dr. Ali Murat Kökat
Live webinar
Fri. 22 May 2026
1:00 pm EST (New York)
Live webinar
Fri. 22 May 2026
2:00 pm EST (New York)
Live webinar
Tue. 26 May 2026
12:00 pm EST (New York)
Live webinar
Tue. 26 May 2026
2:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






























To post a reply please login or register