This article describes and demonstrates the use of the Erbium:YAG 2940nm laser system (LiteTouch, Syneron Medical Ltd.) as a central tool in the treatment of osseous crown lengthening, and the advantages this wavelength offers versus the use of conventional methods.
Objectives and methods
Crown lengthening is a surgical procedure employed for the removal of periodontal tissue, in order to increase the clinical crown height. It is the most frequently used and valuable periodontal surgical procedure related to restorative treatment.(1-4)
embedImagecenter("Imagecenter_1_1282",1282, "large");
The objectives of clinical crown lengthening include
- Removal of subgingival caries
- Preservation and maintenance of restorations
- Cosmetic improvement
- Enabling restorative treatment without impinging on biologic width
- Correction of the occlusal plane
- Facilitation of improved oral hygiene
There are two methods of crown lengthening:
- Orthodontic - coronal extension
- Surgical - apical extension
Clinical considerations
- Importance of the tooth
- Subgingival caries
- Clinical crown/root ratio
- Root length and morphology
- Residual amount of bone support
- Furcation involvement
- Tooth mobility
- Aesthetic demands
- Post-op maintenance and plaque control
Biologic width and aesthetic dentistry
The clinician must create a symmetrical and harmonious relationship between lips, gingival architecture and positions of the natural dentate forms. Spear et al.(5) have referred to this diagnostic methodology as facially generated treatment planning, where the maxillary central incisal edges determine where the soft tissue, i.e., gingiva, and bone should be positioned.(6)
To utilize crown lengthening, it is important for the restorative dentist to understand the concept of biologic width, indications, technique and other principles.(7-9) To maintain healthy periodontal tissue, the attached gingival and biologic width must be considered. Biologic width is measured from the bottom of the gingival sulcus to the alveolar crest and is maintained by homeostasis.(10,11) This width consists of the epithelial attachment to the tooth surface and its connective tissue. The average width is 2.04 mm. Impinging biologic width may cause periodontal tissue destruction; therefore, in crown lengthening, the position of the margin is important.
Methods of clinical crown lengthening
As mentioned above, there are two methods to lengthen a crown: coronal extension and apical extension. Apical extension of the crown is achieved by surgery, with or without osseous resection. In apical extension there are two methods:
- Open technique: patients who exhibit asymmetrical gingival levels, those with greater than 3 to 5mm of maxillary gingival display, or both may be candidates for surgical gingival and/or alveolar bone repositioning to improve their aesthetics.
- Closed technique - for minor localized biologic width and/or aesthetic gingival zenith corrections. Can be used in lieu of a flap procedure to make the correction and complete the restorative process without the necessary healing time required for open crown lengthening surgeries.(12)
Case presentation
This clinical report describes a situation in which a crown lengthening procedure was successfully performed with the Er:YAG laser (LiteTouch, Syneron Medical Ltd.) as a principal auxiliary tool, and the advantages of the 2940 nm wavelength versus conventional methods.
Examination
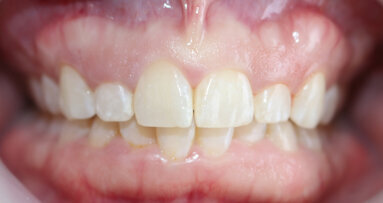
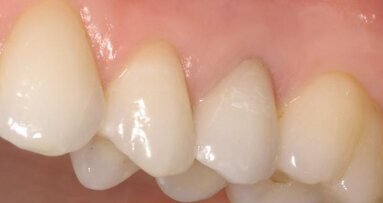
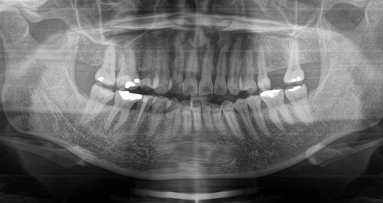
Clinical examination of a 57-year-old male revealed missing teeth at the locations #17, 36, 44, 45 and 46 with overeruption of teeth # 14 and 15 (Fig. 1). Radiographic examination of the area showed overeruption of teeth 14 and 15 with the alveolar bone.
Treatment options
The treatment options available in this case were:
- Insertion of implants and metal-ceramic crowns at the locations of teeth #17, 36, 44, 45 and 46.
- In addition to option one above: crown lengthening for teeth #14 and 15 and covering them with metal-ceramic crowns.
Following discussion with the patient and evaluation of the possibilities for success, it was decided to perform crown lengthening. Treatment would involve the use of the Er:YAG laser to perform the following steps, based upon accepted research:
- Flap incision(13-15)
- Ablation of soft tissue around the teeth after raising a flap(16-18)
- Remodelling, shaping and ablating of the bone(13,15,19,20)
Treatment
All five implants were placed in one sitting (Fig. 2). Crown lengthening was performed three weeks postop (Fig. 3). Laser operating parameters employed for the various surgical stages were as follows:
- Flap Access: Wavelength: 2940nm (Er:YAG), 600-micron sapphire tip, contact mode; 200 mJ per pulse at 35 Hz. Total power: 7 Watts.
- Soft Tissue Removal: Wavelength: 2940nm (Er:YAG), 1300-micron sapphire tip, non-contact mode; 400 mJ per pulse at 20Hz. Total power: 8 Watts.
- Bone Surgery: Wavelength: 2940nm (Er:YAG), 1300-micron sapphire tip, non-contact mode; 300 mJ per pulse at 20 Hz. Total power: 6 Watts.
With the assistance of a diode laser operating at a power setting of 2.4 W in contact mode, the location of the incision was marked (Figs. 4 and 5). An incision was made with the laser (after anaesthesia) at the buccal and palatal side of teeth #14 and 15 (Fig. 6) and a vertical incision was not required. The buccal and palatal flaps were lifted and the area was explored (Fig. 7); there was soft tissue around the neck of the teeth. The soft tissue was ablated using the laser. Vaporization of soft/granulation tissue (if any exists) after raising a flap is efficient with the Er:YAG laser, offering a lower risk of overheating the bone than that posed by the diode or CO2 lasers23 and often obviates the need for hand instruments. Results from both controlled clinical and basic studies have pointed to the high potential of the Er:YAG laser and its excellent ability to effectively ablate soft tissue without producing major thermal side effects to adjacent tissue have been demonstrated in numerous studies.(16-18)
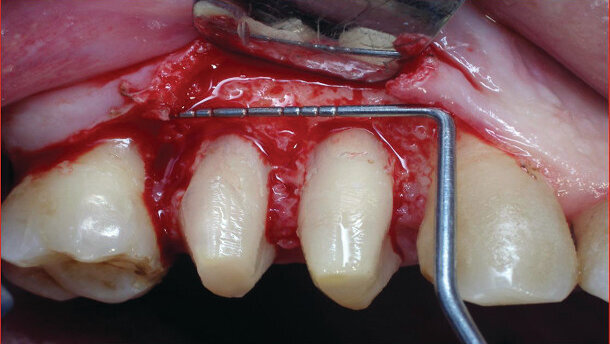
The Er:YAG laser was aimed at the surface of the exposed bone which was ablated in non-contact mode (Fig. 8). Studies have shown that Er:YAG laser energy effects on bone include bacterial reduction.(22) Following this, all accessible bone surfaces were exposed to laser energy to ablate necrotic bone and to shape and remodel the surface in accordance with established clinical protocols.(13,15,20) The bone level around teeth #14 and 15 fits to the bone level of teeth #13 and 16 (Fig. 9). The mucoperiosteal flap was re-positioned and sutured with silk 3-0, paying particular attention to primary closure of the flap (Fig. 10).
Postoperative instructions
The patient was prescribed antibiotics to avoid infection and painkillers for pain. Instructions were given to rinse with Chlorhexidine 0.2 %, starting the next day for two weeks, three times per day.
Management of complications and follow-up
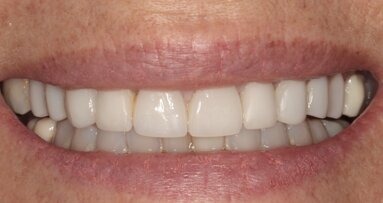
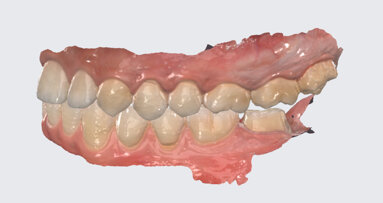
The following day the patient reported moderate pain and moderate swelling. There was no tissue bleeding and the site was closed. The flap was showing signs of attachment and was healing nicely. At seven days post-op, the patient returned for inspection and removal of sutures. The swelling had resolved and healing was progressing well (Fig. 11). After five months, the soft tissue was healed completely without complications (Fig. 12). The soft issue had healed over the bone and there were no bony projections observed under the soft tissue. The prognosis is excellent. An impression for two metal-ceramic crowns was taken five months post-op (Fig. 10). An aesthetic result was achieved (Figs. 13 and 14).
Conclusion
The Er:YAG laser system (LiteTouch, Syneron Medical, 2940nm) can be employed as an auxiliary tool for the purpose of crown lengthening and has been shown to be effective and safe. The use of the LiteTouch wavelength for these procedures presents many advantages as opposed to conventional methods, including enhancement of the surgical site and less bleeding during the operation, providing the surgeon with a better field of visibility and reducing patient discomfort during use. In addition, anecdotal claims have been made that post-operative effects such as pain and swelling are less pronounced. Finally, the laser offers the dental surgeon enhanced ease of use with the hand piece's 360° swivel capability.
This article was published in laser international magazine of laser dentistry No. 01/2013.
Veneer removal using rotary instruments can be time-consuming and risks damaging the underlying tooth structure. The Er:YAG laser offers a conservative and ...
A 31-year-old female patient presented to our care with esthetic concerns regarding the appearance of her gummy smile and bony protuberances above her ...
Enamel hypoplasia is the most common abnormality of development and mineralisation of human teeth. The lesion is characterised by a quantitative defect in ...
KIEL, Germany: In November last year, researchers at Kiel University reported a technological advance in additive manufacturing. They reported the first ...
According to the Classification System for Periodontal Diseases and Conditions (1999)(1), drug-induced gingival enlargement belongs to the group of gingival...
A 72-year-old patient presented to our clinic for whom crown treatment of tooth #37 was planned owing to the patient complaining of recent pain on biting ...
CAD/CAM technology allows dental professionals to manufacture solid all-ceramic crowns chairside. A digital image of the preparation is captured with an ...
A 48-year-old female patient was referred to our clinic owing to a defective amalgam restoration on tooth #46. She had spontaneous acute pain in the area of...
Broken file management is one of the most challenging parts of endodontic treatment. Regardless of whether the clinician is faced with a retreatment ...
Over the past decade, digital dentistry has significantly transformed prosthetic treatment workflows. Advances in intra-oral scanning and CAD/CAM ...
Live webinar
Tue. 19 May 2026
11:00 am EST (New York)
Live webinar
Tue. 19 May 2026
1:00 pm EST (New York)
Prof. Dr. med. dent. Ivo Krejci
Live webinar
Wed. 20 May 2026
7:00 am EST (New York)
Dr. Graham Carmichael BDSc (Hons), DClinDent (Pros), FRACDS, Dr. Robert Gottlander DDS
Live webinar
Wed. 20 May 2026
9:00 am EST (New York)
Live webinar
Wed. 20 May 2026
11:00 am EST (New York)
Live webinar
Wed. 20 May 2026
1:00 pm EST (New York)
Prof. Dr. med. dent. Tim Joda PhD, MSc, eMBA
Live webinar
Thu. 21 May 2026
12:00 pm EST (New York)
Dr. Leonardo Muniz DDS, MSC



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



































To post a reply please login or register