Case finishing is one of the important clinical steps in dentistry. Aesthetics, functional forces and oral health are the three fundamental components that need to be considered during case finishing. Aesthetic components are clinically visible and guided by the subjective analysis (perception) of the patient and the clinician.
However, the force components are invisible, and their adverse effects are not easily appreciated clinically until the effects become chronic. Moreover, the force components require special tools and clinical techniques to demonstrate and measure them clinically. Therefore, the force is the most neglected component in cosmetic dentistry during case finishing. When the force components are not addressed properly during the treatment, clinicians may encounter various clinical problems, such as damaged restorations (veneers, onlays, crowns and bridges); fractured teeth; tooth mobility; abnormal tooth wear and sensitivity; pain in the teeth, muscles and jaw joints; and increased neck pain, ear pain and headache. In cosmetic dentistry, forces are finished based on articulating paper mark interpretation and the patient’s proprioception feedback. It has been documented in the literature that articulating paper is a poor indicator of occlusal disharmony and cannot measure occlusal load and the timing of tooth contacts. The proper tools and techniques can measure precisely and objectively the necessary occlusal parameters required for finishing the force components in cosmetic dentistry. Minimally invasive cosmetic dentistry customised case finishing integrates the concept of force finishing into the conventional case-finishing protocol of dentistry, in the hope that it will help practitioners to achieve long-term optimum results in terms of health, function and aesthetics, and high patient satisfaction with minimal biological cost.
embedImagecenter("Imagecenter_1_677",677, "large");
Introduction
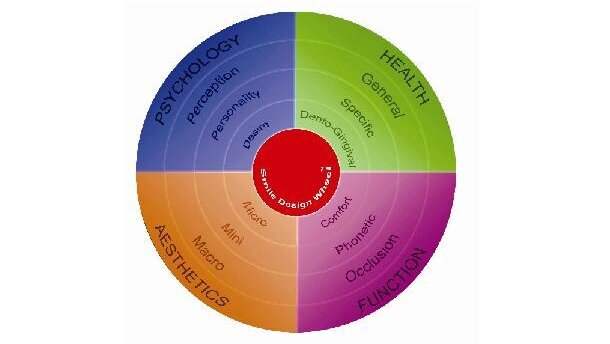
The treatment modalities and protocol of health care should be aimed at the establishment of health and the preservation of the human body with its natural function and aesthetics. The comprehensive concept of minimally invasive cosmetic dentistry (MiCD) and its treatment protocol were introduced in 2009 with the basic aim of a clinician effecting optimum clinical therapeutic improvements in smile enhancement, while performing corrective procedures that require as little clinical intervention as possible.[1] The intervention level of the treatment in MiCD depends on the type of smile defects and the aesthetic needs of the patient.[1] The five core principles (Fig. 1) of the MiCD concept help to guide the clinician in achieving the desired smile enhancement with minimal clinical intervention. However, the core principles must be adapted from case selection to the final case-finishing stages. Proper case finishing is not possible without understanding its two components, namely the micro-aesthetics and the occlusal forces. It is, however, the force component that is often neglected, or improperly considered, in cosmetic dentistry. This article describes an MiCD customised case-finishing (MCCF) concept and protocol that respect both force and aesthetic components.
MiCD customised case-finishing concept
Case finishing is one of the most important steps in any clinical treatment in dentistry. It has three major components that need to be considered: aesthetics, overall health and occlusal function. It is interesting to note that case finishing is viewed differently in different disciplines of dental medicine. In orthodontics, case finishing fundamentally focuses on six keys to occlusion (Fig. 3) described by Andrews,[2] whereas in cosmetic dentistry, it is considered the last step of the clinical procedure and entails refining the micro-aesthetic components of the smile. Cosmetic dentists spend their clinical time and effort rather on the aesthetics of the final result. This is because, aesthetic components are visible to both the clinician and patient, and the outcome can thus be appreciated immediately. However, the force components are invisible, and their negative effects are not easily appreciated clinically until the effects become chronic. Another reason that force finishing may be overlooked is that it requires special tools and clinical techniques to demonstrate and measure the force factors clinically. Therefore, force is the most neglected component in cosmetic dentistry during case finishing.
In cosmetic dentistry, forces are finished based on articulating paper mark interpretation and the patient’s proprioception feedback. It has been documented in the literature that articulating paper is a poor indicator of occlusal disharmony,[3–5] and studies have shown that mark size varies with the same applied load, with differing thickness of paper, surface texture of tooth and restorations, and that mark interpretation is an operator-based subjective procedure. Moreover, paper cannot measure the timing of occlusal forces.[3–6]
A proper case-finishing protocol must be based on both subjective and objective analysis. In order to measure the occlusal load and timing of occlusal forces, it is necessary to use proper tools, which can measure precisely and objectively the necessary occlusal parameters required in cosmetic case finishing. Computerised instrumentation to analyse occlusal forces was introduced by Tekscan Inc in 1984 as T-Scan I.[7] Over the past 27 years, it has evolved to become a very precise diagnostic and treatment tool that is used to manage the force components in any conventional case-finishing approach to dentistry.
Every clinical case is different, as it is related to the patient’s state of health, his or her functional requirements, and his or her aesthetic needs and desires. Function is directly related to the forces that a patient generates within his or her stomatognathic system. There are four different theories of occlusion. Each of these theories has their value, and treatments that are founded on each have been successful. These theories of occlusion differ in their consideration of the positioning of the jaw or temporomandibular joint during treatment, which are known as jaw-position theories (Fig. 4).
However, all of these theories agree on the following issues:
1. Teeth during mandibular closure: All teeth should occlude simultaneously in mandibular closure movement.[13–16]
2. Occlusal load distribution on arch: An equal percentage of occlusal force should be shared between the right and left arch halves.
3. Occlusal load on tooth: An equal percentage of occlusal force should be distributed on each tooth counterpart.
4. Excursive contacts: The anterior teeth should immediately disclude the posterior teeth during excursive movements.[13–16]
Based on the laterotrusive movements from centric occlusion, various concepts of functional occlusion have been recognised and advocated: balanced occlusion,[17,18] canine-protected occlusion,[19–26] group-function occlusion,[27–31] mixed canine-protected and group function,[32] flat-plane (attrition) occlusion,[33, 34] biological (multi-varied, physiological) occlusion.[35] However, no single type of functional occlusion has been found to predominate in nature and there appears to be no scientific evidence to support one occlusal scheme over other.[36]
Therefore, the literature and research findings, along with individual clinical experiences and accepted parameters of care, should always be considered in selecting the occlusal scheme during cosmetic dental treatment. Case-finishing procedures should not be based on a one-size-fits-all concept, and must be customised and designed according to the patient’s aesthetic desires, functional requirements and physiological limits. MCCF integrates the concept of force finishing into the conventional case-finishing protocol in the hope that it will help practitioners to achieve long-term optimum results in terms of health, function, aesthetics and patient satisfaction with minimal biological cost. MCCF consists of three clinical components:
_force finishing;
_aesthetic finishing; and
_finishing evaluation.
Force finishing
The concept of force finishing is new in cosmetic dentistry and should not be confused with the conventional occlusal equilibration or occlusal adjustment process. The concept of force finishing is based on the universal principles of force balance and force loading timing during dynamic occlusion. In order to achieve precise force finishing in restorative dentistry, clinicians need to plan the occlusal goals. This is required because the force-finishing steps alone cannot refine the major occlusal discrepancies of the patient. Hence, proper jaw positioning, angulation and establishment of tooth form (natural anatomy) must be completed before proceeding to MCCF. There are five areas of the occlusal scheme in which clinicians can affect the force components (Fig. 5).
The force-finishing component of MCCF requires the use of digital occlusal technology that can measure precisely and objectively clinical occlusal force data, while displaying the findings for clinical interpretation and treatment. The objective and precise clinical data helps clinicians to achieve tooth-contact forces and tooth-contact timing sequences that are preservational, rather than destructive, regarding the final case result. However, in cosmetic dentistry, the role of force finishing is generally overlooked, minimised or ignored.
The following are some of the clinical problems that clinicians encounter when they ignore or are unable to harmonise occlusal forces after treatment:
_damaged restorations (veneers, onlays, crowns, bridges);
_fractured teeth;
_tooth mobility;
_abnormal tooth wear and sensitivity;
_pain in the teeth, muscles and jaw joints; and
_increased neck pain, ear pain and headache.
In order to achieve the quality force-finishing results in dentistry, the following clinical conditions must be fulfilled during the force-finishing process:
_even and simultaneous contacts of all teeth during mandibular closure;
_distribution of nearly equal force percentage between the right and left arch halves;
_distribution of more tooth-contact forces on posterior teeth, less on premolar teeth, with only light anterior contacts;
_the centre of force (COF) should be in the middle of the force distribution of all contacting teeth;
_the anterior teeth should immediately disclude the posterior teeth during excursive movements.[13–16]
Optimally, after proper force finishing, all teeth should come into contact with one another at about the same time and with harmonised occlusal forces and measurably short disclusion timing. When this does not occur, the clinical case is considered to be unbalanced and poorly force finished. Force-finishing clinical facts are shown in Figure 6.
Aesthetic finishing
The aesthetic outcome is one of the major concerns of all patients seeking cosmetic dental treatment. The aesthetic-finishing process in cosmetic dentistry involves establishing high surface gloss and creating proper micro-smile aesthetic characteristics. These include proper tooth-size ratio, axial inclination, open incisal embrasures, proper connector location, proper contact-point progression, surface micro-texture, surface gloss or lustre, inciso-gingival shade progression, and special surface effects on the facial surfaces. Additionally, gingival aesthetic characteristics to incorporate during case finishing are the control of tissue contour, embrasure heights, gingival zenith, and the establishment of uniform height (position or level) of the tissue around all the restorations.
In order to improve the practicality of clinical aesthetic case-finishing procedures, the procedures are divided into four clinical steps:
_Aesthetic contouring: The restoration is grossly reduced for the reproduction of the natural size, shape and other details of the tooth form.[53] Re-establishing the contact with
adjacent opposing teeth to a normal and functional form is achieved in this step.[53]
_Finishing: This is a finishing process to establish an even, well-adapted junction between the tooth surface and the restorations.
_Aesthetic touch-up: Necessary minor adjustments to achieve natural surface details through texture, grooves, pits and other special surface effects.
_Polishing: This step entails smoothing restorations to an enamel-like lustre. For clinical convenience, this process can be further divided into three steps:
a) pre-polishing: removing the remaining surface scratches from the aesthetic touch-up process;
b) polishing: achieving blemish-free and smooth surfaces with no visible scratches;
c) super polishing: creating enamel-like lustre or gloss.
Aesthetic-finishing clinical facts are shown in Figure 15.
Finishing evaluation
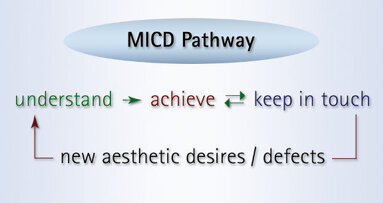
Post-operative clinical evaluation is one of the fundamental requirements of the keep in touch principle of the MiCD treatment protocol.[1] Generally one week after the case finishing, the case should be re-evaluated in terms of health, comfort and aesthetics through clinical examination, digital images and other necessary guiding tools. The end-result of force finishing should be re-confirmed before final case documentation.
MiCD customised case-finishing protocol
Based on the patient’s aesthetic wishes and level of sensitivity towards the occlusal force components (tooth-contact forces and timing sequences), MCCF can be divided into three clinical types:
_Type I: In cases in which forces are not part of creating the aesthetic case changes, as well as cases of non-load-bearing anterior and posterior restorations, tooth-whitening procedures, reductive and additive contouring (both the teeth and gingival tissues) if correction does not alter the existing occlusal scheme, these cases are generally finished according to the type I MCCF protocol (Table I).
_Type II: When aesthetic cases are sensitive to tooth-contact forces because a major restoration is being fabricated on the load-bearing areas of the anterior or posterior teeth (as when utilising inlays, onlays, overlays, crowns and bridges, veneers, dentures, or performing a re-restoration of frequently fractured restorations), force-finishing procedures should precede aesthetic case finishing. This will improve the long-term clinical success of the restoration and create effective functional health. Force finishing in type II cases requires the use of digital technology (T-Scan III) that can measure and display the underlying tooth-contact forces precisely and objectively. The type II MCCF finishing protocol is shown in Table II.
_Type III: Complex aesthetic cases (full-mouth restoration, orthodontic treatment, implant restoration, cases with para-functional habits, restorations that alter the anterior guidance, cases with a known history of TMD symptoms) require significant tooth-contact force and timing management. In these complex restorative cases, force finishing is performed before aesthetic finishing is accomplished in order to achieve enhanced occlusal function and ideal aesthetics, combined with teeth, muscle and joint harmony. The type III MCCF protocol is shown in Table III.
All three types of force finishing should always be in harmony with the aesthetic results. After force finishing, the micro-aesthetic elements should be re-examined, and cases should be completed with the necessary aesthetic touch-ups, and super polishing of all restorations. It should be remembered that the force-finishing process should be followed by aesthetic finishing to complete the case successfully.
Conclusion
In the performance of cosmetic dentistry, the force components are frequently neglected or misunderstood. Therefore, the physical strength of the tooth-coloured restorative materials is still an important topic in cosmetic dentistry. The restorative materials chosen are often much stronger than the natural teeth because the clinician hopes the materials selected will overcome potential fracture of the restorations. However, it is necessary to understand that the highly concentrated occlusal force locations within the occlusal scheme may not always fracture the restorations, but will create other problems with the teeth, muscles and/or joints in some patients. Therefore, if the clinician overcomes fracture of the restorations through material choice, he or she may actually be ignoring the underling force factors.[68]
It is to be noted that whatever the theory or concept of occlusal scheme selected during the treatment procedure, the role of MCCF is paramount to achieving long-term optimum results in terms of health, function, aesthetics and high patient satisfaction with minimal biological cost.
Editorial note: A complete list of references is available from the publisher.
The author does not have any conflict of interest regarding the products mentioned in this article.
This article originally appeared in the MiCD Clinical Journal, 2011 Dec-Mar; 01(1):32-42. Reprinted with permission from Vedic Institute of smile Aesthetics (VISA)
Minimally invasive cosmetic dentistry (MiCD), also known as “do no harm” dentistry, focuses on preserving the natural tooth structure while achieving ...
In the field of dental prosthetics, digital communication has undergone a major revolution in recent years, transforming how dental technicians interact ...
Increased media coverage and the availability of free web-based information has lead to heightened public awareness and thus to a dramatic increase in ...
Petersilka et al. said: “If a new form of therapy is to be considered worth integrating into standard periodontal therapy, it either has to be superior in...
Artificial intelligence (AI) has moved from theory into daily prosthodontic practice, reshaping diagnosis, treatment planning and design workflows. My ...
Endodontic treatment of teeth with significant coronal destruction is a very common clinical procedure in the restorative clinical practice. When we are ...
Artificial intelligence (AI) continues to significantly transform digital dentistry. In aligner therapy, AI-driven systems now assist with tooth ...
DUBAI, UAE: Augmentation of an insufficient bone volume is indicated before or in conjunction with implant placement to gain long-term functioning and an ...
In this clinical case, Irfan Abas, an expert in the field of oral implantology and restorative dentistry, shows how excellent, lasting aesthetic results can...
In recent years, manufacturers have developed increasingly advanced composite materials, offering improvements in aesthetics, handling and mechanical ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East

































To post a reply please login or register