Increased media coverage and the availability of free web-based information has lead to heightened public awareness and thus to a dramatic increase in patients’ aesthetic expectations, desires and demands. Today, a glowing, healthy and vibrant smile is no longer the exclusive domain of the rich and famous and most general practitioners are forced to incorporate various aesthetic treatment modalities in their daily practices to meet this growing demand.
The treatment modalities of any health-care service are aimed at the establishment of health and the conservation of the human body with its natural function and aesthetics. The concept of minimally invasive (MI) treatment was initially introduced in the medical field and was adapted in dentistry in the early 1970s with the application of diamine silver fluoride.1 This was followed by the development of preventive resin restorations (PRR)2 in the 1980s and the atraumatic restorative treatment (ART) approach3 and Carisolv4 in the 1990s. The major components of MI dentistry are the risk assessment of the disease with a focus on early detection and prevention; external and internal re-mineralisation; use of a range of restorations, bio-compatible dental materials and equipment; and surgical intervention only when required and only after any existing disease has been controlled.5–11
Current basic treatment protocols (TPs) and approaches in MI dentistry are the use of air abrasion, laser treatment or sono abrasion to gain cavity access and excavate infected carious tooth tissue through selective caries removal or laser treatment;12,13 cavity restoration by applying ART, PRR, or sandwich restoration; and the use of computer controlled local anaesthesia delivery systems14 with emphasis on the repair of a failed restoration rather than its replacement.15 Thus far, the focus of MI dentistry has been on caries-related topics16 and has not been comprehensively adopted in other fields of dentistry. Dr Miles Markley, one of the great leaders of preventive dentistry, advocated that the loss of even a part of a human tooth should be considered a serious injury and that dentistry’s goal should be to preserve healthy and natural tooth structure. His words are much more relevant in today’s cosmetic dental practice, in which the demand for cosmetic procedures is rapidly increasing. With the treatment approach trend towards the more invasive protocols, millions of healthy teeth are aggressively prepared each year in the name of smile makeovers and instant orthodontics, neglecting the long-term health, function and aesthetics of the oral tissues.
The need for a new concept
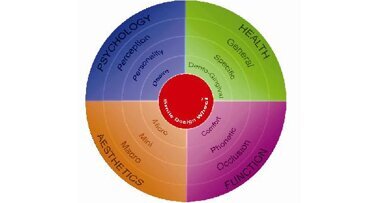
Contemporary aesthetic dentistry demands well-considered concepts and TPs that provide a simple, comprehensive, patient-friendly and MI approach with an emphasis on psychology, health, function and aesthetics (PHFA; Fig. 1). The need for a holistic concept and basic treatment guidelines was expressed by concerned practitioners, aesthetic dentistry associations and academics around the world for the following basic reasons:
- Owing to an increased aesthetic demand, aesthetic dentistry is becoming an integral part of general dentistry. The aesthetic outcome of any dental treatment plays a vital role in the patient’s treatment satisfaction criteria.
- MI dentistry currently focuses on prevention, re-mineralisation and minimal dental intervention in the management of dental carious lesions. It has failed to give the necessary attention to the problems that negatively affect smile aesthetics, for example non-carious dental lesions, or developmental defects and malocclusion.
- The treatment modalities of contemporary cosmetic dentistry are trending towards more invasive procedures with an over-utilisation of crowns, bridges, thick full veneers, and invasive periodontal aesthetic surgeries, while neglecting long-term oral health, actual aesthetic needs and the characteristics of the patient.
- Social trust in dentistry is degrading, owing to the trend of fulfilling the cosmetic demands of patients without ethical consideration and sufficient scientific background (the more you replace, the more you earn; more is more mentality).
In this article, I introduce a concept and TP for minimally invasive cosmetic dentistry (MICD), in order to address these facts properly and integrate the evidence-based MI philosophy and its application into aesthetic dentistry.
Defining MICD
As the perception of aesthetics and beauty is extremely subjective and largely influenced by personal beliefs, trends, fashion, and input from the media, a universally applicable definition is not available. Hence, smile aesthetics is a multifactorial issue that needs to be adequately addressed during aesthetic treatment.17 MICD deals both with subjective and objective issues. Therefore, in this article I define MICD as “a holistic approach that explores the smile defects and aesthetic desires of a patient at an early stage and treats them using the least intervention options in diagnosis and treatment technology by considering the psychology, health, function and aesthetics of the patient.”18
The core MICD principles are:
1. application of the-sooner-the-better approach and exploration of the patient’s smile defects and aesthetics desires at an early stage in order to minimise invasive treatments in the future;
2. smile design in consideration of the psychology, health, function and aesthetics (Smile Design Wheel18) of the patient;
3. adoption of the do-no-harm strategy in the selection of treatment procedures and the maximum possible preservation of healthy oral tissues;
4. selection of dental materials and equipment that support MI treatment options in an evidence-based approach;
5. encouragement of the keep-in-touch relationship with the patient to facilitate regular maintenance, timely repair and strict evaluation of the aesthetic work performed.
The main MICD benefits include:
1. promotion of health, function and aesthetics of the oral tissues and positive impact on the quality of life of the patient;
2. preservation of sound tooth structures (banking the tooth structure), while achieving the desired aesthetic result;
3. reduction of treatment fear and increased patient confidence;
4. promotion of trust and enhancement of professional image.
The MICD treatment protocol
In my experience, the TPs that are currently in use in aesthetic dentistry are mostly based on more invasive techniques and procedures. With the use of such protocols, cosmetic dentists are knowingly, or unknowingly, heading towards the over-utilisation of invasive technologies in their practices, which is becoming a professional and ethical concern. The basic aim of the MICD TP is to guide practitioners in achieving optimum results with as little intervention as possible. The intervention level of the treatment in MICD depends on the type of smile defects and the aesthetic needs (objective measurement and subjective perception) of the patient.
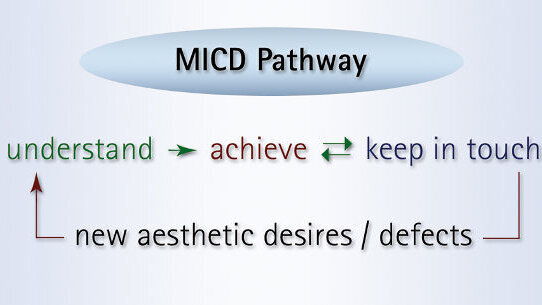
The basic framework and pathway of the MICD TP are illustrated in Figures 2 and 3. It is to be noted that the TP in medical and dental sciences must be dynamic in nature and should be flexible to incorporate evidence-based facts. I have therefore outlined the MICD core principles that are required to achieve the optimum result in terms of health, function and aesthetics with minimum intervention and optimal patient satisfaction. However, it is the practitioner’s duty to incorporate all the necessary guidelines, protocols and regulations of the authority concerned (state or affiliated professional organisations) into the MICD TP.
Phase I: Understand
In the first step of Phase I, the perception, lifestyle, personality, and desires of the patient are explored. The primary goal of this first step is a better patient–dentist understanding. As the aesthetic perceptions of the dentist and the patient may differ, it is imperative to understand the subjective aesthetic perception of the patient. Various types of questions, personal interviews and visual aids can be used as supporting tools. In this step, the practitioner should ask the patient to complete the MICD self smile-evaluation form. The information obtained will help estimate the perceived smile aesthetic score (a-score) and will be used as the base-line data in the evaluation step.
Next, diseases, force elements and aesthetic defects of smile are explored. Information on the medical and dental history, general health and specific health (oral-facial) of the patient is collected and complete dental and periodontal charting is performed. In order to understand the force elements, the existing occlusion, comfort, muscular activity, speech and phonetics are thoroughly examined with the evaluation of para-functional and other oral habits, comfort during mastication and deglutition, and temporo-mandibular joints (TMJ) movements. The necessary diagnostic tests, photographic documentation and the diagnostic study models are prepared during this step for the further exploration of existing diseases, force elements and aesthetic defects.
In the following step, the data collected is analysed in relation to the accepted normal values of a patient’s sex, race and age (SRA) factors. The aesthetic components of the smile are analysed in detail grouped into macro- (facial and dental midline relation, facial profile, symmetry of the facial thirds and hemi-faces), mini- (visibility of upper anterior teeth, smile arc, smile symmetry, buccal corridor, display zone, smile index and lip line) and micro-aesthetics (dental: central dominance, teeth proportion, axial inclination, incisal embrasure, contact-point progression, shade progression, surface texture; gingival: shape, contour, embrasure and zenith height). The practitioner can now grade the smile in terms of the patient’s health, function and aesthetics as follows:
- Grade A: The established parameters of oral health, function and aesthetics are within normal limits and aesthetic enhancement is required only to fulfil the patient’s cosmetic desires.
- Grade B: The established parameters of oral health and function are within normal limits; however, the aesthetic parameters are below the accepted level. Aesthetic enhancement can further improve the aesthetic parameters.
- Grade C: The established parameters of oral health or function or both are below the normal limits. An establishment treatment is mandatory prior to aesthetic enhancement.
From the above, the practitioner will obtain a smile aesthetic grading in terms of the patient’s health, function and aesthetics, as well as a complete overview over the smile aesthetic problems and the macro-, mini- and micro-smile defects.
The patient’s PHFA factors are the four fundamental components of aesthetic dentistry18 and must be respected to achieve healthy, harmonious and beautiful smiles. The design step depends on the information obtained from exploration and analysis. The information on psychology is subjective in nature; however, health, function and aesthetic analysis provides the objective information that will guide the design with the various established and basic principles of smile aesthetics and also the feasible and practical extent of the aesthetic desires of the patient. The aesthetic mock-up, manual tracing, digital makeover and smile catalogues are some of the popular tools used in this step. A new smile, alternative designs, types of treatments involved, complexity, possible risk factors and complications, treatment limitation, and tentative costs should be established during this step.
For easy application, the aesthetic treatments in MICD are categorised as follows:
- Type I: Micro-aesthetic components;
- Type II: Mini-aesthetic components; and
- Type III: Macro-aesthetic components: facial and dental midline relation, facial profile, symmetry of facial thirds and hemi-faces.
As the treatment modality depends on the professional capability and experience of the practitioner, simple and practical methods are used to categorise the MICD treatment complexity:
- Grade I: Treatment that may require consultation with a specialist (preventive, simple oral surgery/endodontics/periodontics/implants, short orthodontics);
- Grade II: Treatment that requires the procedural involvement of other dental specialists (complex endodontics/periodontics/orthodontics) but not oral and maxillofacial surgery or plastic surgery; and
- Grade III: Treatment that requires the procedural involvement of oral and maxillofacial surgery or plastic surgery.
With the aid of this simple grading system, any practitioner can determine the complexity of the treatment involved for the accomplishment of a new smile design for an individual patient and can plan for the necessary multidisciplinary support.
The last step of this phase is the most important in MICD TP because in this step the patient is presented with an image of his or her future smile. Visual aids, such as a smile catalogue, aesthetic mock-ups, manual sketches, modified digital pictures, computer-designed makeovers or animations can be used as presentation tools. The results of the design step are systematically presented to the patient with professional honesty and ethics. All pertinent queries of the patient related to the proposed smile need to be addressed during presentation. The treatment complexity, its limitations, the risks involved, possible complications, treatment cost estimation and maintenance responsibility must properly be explained to the patient. The patient is thus involved in finalising the treatment plan and will sign the written informed consent form before proceeding to Phase II.
Phase II: Achieve
As per the TP, which is finalised during the presentation step, all necessary preventive interceptive and restorative (curative) dental treatments are conducted in order to establish the proper health and function of the oral tissues. Owing to the complexity of the treatment, a multidisciplinary approach may be necessary for a good result. Once the case is stable in terms of health (controlled disease) and function (balanced force elements) with good oral habits, the patient is requested to re-evaluate his or her smile in terms of aesthetics with the help of the MICD self smile re-evaluation form. This is important, because in some cases the patient is fully satisfied with the results of the establishment step alone and may modify his or her idea of further aesthetic enhancement. In MICD TP it is considered unethical should the practitioner not collect self smile re-evaluation information from the patient.
The enhancement step of MICD is focused on the fulfilment of the patient’s aesthetic desires, which can be grouped into two categories based on the patient’s needs and wants. Even though it is sometimes difficult to draw a clear line between the two and their related treatment, in MICD they are categorised as follows:
- needs: objective restorative needs of the patient in harmony with the SRA factors and due emphasis on health and function of oral tissues (naturo-mimetic smile enhancement)
- wants: subjective desires of the patient, which may not be in harmony with the SRA factors (cosmetic smile enhancement)
During any want-based aesthetic treatment, where healthy oral tissue is treated with no direct benefit to health or function, the treatment modalities should be within the scope of non-invasive (NI) or MI procedures.19 The patient’s cosmetic desires alone should not be the rational for the treatment.20 Do no harm! should always be the credo pertinent to all dental treatment procedures.
Phase III: Keep in touch
Regular maintenance, compliance and timely repair play a crucial role in the long-term success of aesthetic enhancement procedures. Hence, MICD emphasises the keep-in-touch concept and encourages patients to go for regular follow-up visits. Responsibility for maintenance is grouped into two categories:
- Self-care: Patients are advised to continue their normal oral hygiene procedures. If necessary, special care and precautionary methods are given, as well as protective devices. Self-care should focus on regular tooth brushing, flossing, the use of prescribed protective devices and other pertinent professional advice for maintaining general health.
- Professional care: The oral habits, health of the oral tissues, and the functional and aesthetic status of the work preformed are well documented during each follow-up visit, and necessary maintenance repair jobs are carried out.
Evaluation is the final step of MICD TP. Any ‘completed’ treatment without a proper evaluation is considered incomplete in MICD protocol. The following components need to be evaluated:
- Global patient satisfaction: After receiving aesthetic dental treatment, the patient is requested to complete the MICD exit form, in which the patient evaluates his or her new smile, gives a second perceived smile aesthetic score (b-score), and indicates his or her global satisfaction score. The b-score is compared with the previous a-score. This process helps determine the patient’s actual satisfaction status. In MICD, this is the main parameter for evaluating a patient’s aesthetic satisfaction.
- Clinical success: Clinical success is a multifactorial issue. Selection of proper cases (the patient), restorative materials, TPs and their correct and skilful application are the key factors for clinical success. Therefore, MICD TP suggests self-evaluation of the following four factors (4Ps) using the MICD clinical evaluation form:
Patient factors: regular maintenance status, compliance issues and attitude of the patient towards aesthetic treatment;
Product factors: bio-compatibility, mechanical and aesthetic quality of the products used for the treatment;
Protocol factors: TP used in terms of its simplicity, predictability and its evidence-based nature;
Professional factors: existing knowledge and skills, and attitude towards developing these.
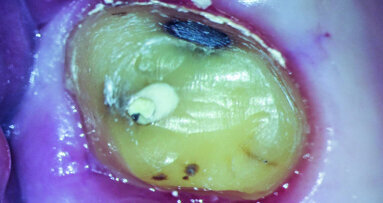
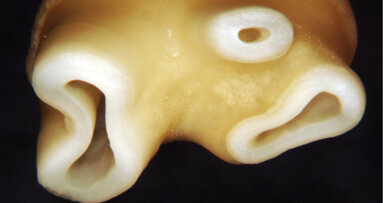
Detailed clinical documentation of the case during maintenance and evaluation can provide various cues to the practitioner in the evaluation of his or her clinical success in terms of case planning, material and protocol selection, as well as his or her existing restorative skills. I believe that a thorough evaluation can support any practitioner in initiating practice-based research and keeping up-to-date with the recent trend of evidence-based dentistry (Figs. 4a–5b).
MICD treatment modalities
Various types of treatment modalities are available in MICD. Their effective use depends on the level of smile defects, type of smile design, proposed treatment type and the treatment complexity grade. There is only one principle in selecting treatment modalities in MICD: always select the least invasive procedure as the choice of the treatment.
The two categories of MICD treatment are NI and MI treatment (Table 1). However, conventional invasive treatment modalities may also be required, depending on the complexity of the case.
Conclusion
MI dentistry was developed over a decade ago by restorative experts and founded on sound evidence-based principles.21–30 In dentistry, it has focused mainly on prevention, re-mineralisation and minimal dental intervention in caries management and not given sufficient attention to other oral health problems. I believe that the MI philosophy should be the mantra adopted comprehensively in every field of the dentistry. For this reason, I have explained the MICD concept and its TP, which integrates the evidence-based MI philosophy into aesthetic dentistry, in the hope that it will help practitioners achieve optimum results in terms of health, function and aesthetics with minimum treatment intervention and optimum patient satisfaction.
Acknowledgements
In formulating the MICD TP, I discussed the concept with several national and international colleagues in order to ensure that it is simple, practical and comprehensive. I would like to extend my gratitude to Dr Akira Senda (Japan), Dr Didier Dietschi (Switzerland), Dr Hisashi Hisamitsu (Japan), Dr Oliver Hennedige (Singapore), Dr Dinos Kountouras (Greece), Dr Mabi L. Singh (USA), Dr Ryuichi Kondo (Japan), Dr So-Ran Kwon (Korea), Dr Prafulla Thumati (India), Dr Vijayaratnam Vijayakumaran (Sri Lanka), as well as Dr Suhit R. Adhikari, Dr Rabindra Man Shrestha, Dr Binod Acharya and Dr Dinesh Bhusal of Nepal, for their valuable comments, advice and feedback
Editorial note: A complete list of references and the MICD forms are available from the publisher.
HELSINKI, Finland: Aligners offer a straightforward and efficient orthodontic treatment option that can be used to achieve aesthetic and functional ...
Minimally invasive—the most well-known oxymoron in dentistry—is probably nowadays considered the new standard of care in almost every field of dental ...
On 20 June, GC Europe will be holding its first international congress on minimum intervention (MI) dentistry. As an introduction, German-based dentist Dr ...
Traditional endodontics has been based on feel, not sight. Tactile proprioreception was the only guide as burs and files were blindly inserted into pulp ...
In the field of dental prosthetics, digital communication has undergone a major revolution in recent years, transforming how dental technicians interact ...
COLOGNE, Germany: Exocad, an Align Technology company, is showcasing its latest developments, including new AI-enabled services, the upcoming Chemnitz ...
Case finishing is one of the important clinical steps in dentistry. Aesthetics, functional forces and oral health are the three fundamental components that ...
LONDON, UK: Despite improvements in treatments, intra-bony defects are associated with progression of periodontal disease and tooth loss unless they are ...
A free webinar on 19 June will offer participants an opportunity to learn about how to implement orthodontic treatment as a fundamental tool in the context...
Resin composites are wonderful restorative materials. Besides allowing for minimally invasive, defect-oriented tooth preparation, they can be modelled as ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



































To post a reply please login or register