Today’s computer-aided design and manufacture (CAD/CAM) technologies contribute greatly to restorative dentistry and provide clinicians with advanced treatment options for various indications, including inlays, onlays, fixed partial dentures and full dentures, thin veneers and crowns.1,2 These systems also allow use of many restorative materials, including metal, metal-ceramic, composite and all-ceramic, to best meet the needs of the case and patient.1,2 Further, CAD/CAM systems are available for both chairside and laboratory applications, so dentists now have the ability to create highly aesthetic and strong restorations in office.1,2
Unlike earlier generations of in-office systems that presented clinical challenges, today’s technology and materials are cost effective and efficient. Past systems lacked advanced software to control the tool path accurately and design a restoration, and inadequate scanning technology made it difficult to detect the delicate margins created during tooth preparation.1,3 The lack of advanced material sciences also contributed to a number of clinical challenges experienced with early CAD/CAM technology, and dentists struggled to properly seat CAD/CAM-processed restorations. To address the clinical challenges experienced with early CAD/CAM technology, manufacturers have developed systems that offer many advantages, including greater cost effectiveness, simplicity and efficiency.1,4
The CEREC system
Amongst this new generation of CAD/CAM systems is CEREC (Sirona), which was developed to address many concerns dental professionals had regarding the set-up of conventional CAD/CAM software and machines.5,6 The milling chamber is now separated from the image capture and design hardware, allowing dental professionals to simultaneously design one restoration while milling another.5,6 With significantly higher speeds and greater memory, CEREC 3-D design software allows users to view tooth designs as they would if evaluating traditional stone models.5,6
embedImagecenter("Imagecenter_1_471",471, "large");
Today’s CEREC system includes a light-emitting diode (LED) camera (CEREC Bluecam, Sirona) for greater accuracy and higher quality images than previous infrared-emitting camera systems, and the recent addition of CEREC Connect (Sirona) allows impression and restoration information to be digitally acquired and transmitted over the Internet to dental laboratories.5,6 Laboratories can then fabricate restorations using the CEREC inLab System (Sirona).5,6
The CEREC MC XL system (Sirona) is a powerful and accurate low-noise chairside CAD/CAM milling system that offers simplicity and efficiency for processing single-tooth restorations in six minutes and quadrant restorations in three to four minutes in a single appointment.5–7 The CEREC MC XL demonstrates precision and accuracy within the range of +/- 25 µ, and the 7.5 µ milling resolution creates restorations with improved fit and smoother surfaces.5–7 Additional features include automatic software downloads, simple display guides and network connectivity, and the milling chamber design enables easy block clamping without tools.5–7
Material considerations
To address CAD/CAM material concerns, manufacturers have developed new ceramic materials that provide improved strength and aesthetics.5 These newer ceramics withstand CAD/CAM processing without chipping or fracturing and can be brought to full contour during milling to improve fit and function.5 Dentists can choose adhesive bonding or conventional cementation when seating these restorations, which ensures that case requirements are met.5 Improvements to cementation and adhesive systems have also enabled dentists to provide a strong bond between the restoration and underlying tooth substrates.1,4
IPS e.max CAD
Composed of 70 % by volume needle-like crystals in a glassy matrix, lithium disilicate glass-ceramic (IPS e.max, Ivoclar Vivadent) offers many improvements to previous generations of ceramic materials.8 Available in a pressable format (IPS e.max Press) or for CAD processing (IPS e.max CAD), the material demonstrates strength values between 360 (Press) and 400 MPa (CAD).8
IPS e.max also demonstrates lifelike optical qualities that enable dentists to create highly aesthetic and naturally appearing restorations in a variety of cases.8 The versatile material is indicated for anterior and posterior restorations, including thin veneers (0.3 mm), minimally invasive inlays and onlays, partial crowns and crowns, implant superstructures, three-unit anterior/premolar bridges (press only), and three-unit bridges (zirconium-oxide-supported IPS e.max CAD only).8
Case presentation
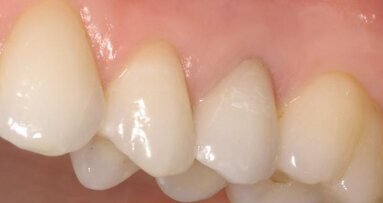
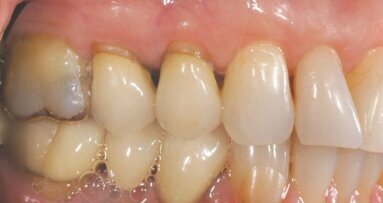
A 53-year-old male patient presented after undergoing recent endodontic treatment on tooth #13 (Fig. 1) and was unhappy with the tooth’s appearance. Along with decay on the adjacent dentition, tobacco stains were also present because the patient was a smoker (Fig. 2). Although the patient requested that treatment be confined to only tooth #13, after a routine head, neck and oral cavity examination, the patient was informed of multiple treatment needs and advised that a comprehensive treatment plan should be started as soon as possible.
Treatment plan
The patient brought to the office the endodontic report from his other clinician, advising that a good prognosis was expected from his endodontic treatment. Although the report did not detail the possible need for crown lengthening or gingivectomy procedures, these were areas of diagnostic concern in this case. However, biological width encroachment did not appear to be an issue during cleaning and probing.
To address the patient’s concern with the aesthetic appearance of tooth #13, high-translucency and high-strength, lithium disilicate glass-ceramic would be CAD/CAM processed into a crown. Milled to as thin as 300 µm axially, the lithium disilicate crown would instil a contact lens effect on the gingival–facial margin of tooth #13.
The crown would then be bonded in place with an adhesive that demonstrates high radiopacity to ensure that excess cement was not inadvertently left behind, specifically in the deep distal margin in this case. The adhesive bonding agent also ensured that cementation was predictable. When complete, the tooth would appear natural and indistinguishable from the surrounding dentition.
Clinical protocol
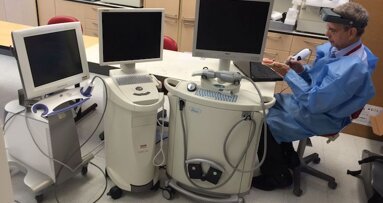
After thorough examination and prophylaxis, tooth #13 was prepared for restoration with a CAD/CAM (CEREC MC XL) processed lithium disilicate crown (IPS e.max CAD) and the temporary material removed. A specialised mouthpiece (Isolite, Isolite Systems) was placed intra-orally to ensure total isolation was achieved (Figs. 3 & 4).
Prior to scanning, the tooth #13 preparation, the surrounding dentition and the soft tissues were sprayed with a CAD/CAM powder (Fig. 5). The anatomical form of the dentition and soft tissues was then captured using an LED scanning unit (CEREC Bluecam). After scanning, 3-D software (CEREC 3D) was used to design the desired crown contours and occlusal relationships. A prefabricated high translucency lithium disilicate block (IPS e.max CAD) was then milled chairside (CEREC MC XL) into a crown for tooth #13 (Fig. 6). Lithium disilicate was the material of choice in this case because it demonstrates high strength and lifelike optical properties.
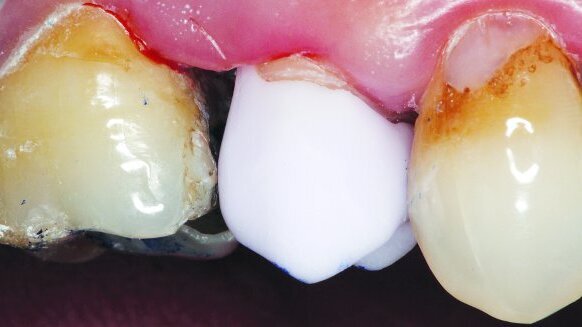
The crown was tried in the patient’s mouth over the tooth #13 preparation to evaluate fit, contour and anatomical harmony (Figs. 7 & 8). Upon confirmation of proper fit and function, the crown was removed, cleaned and dried. Stains were then placed on the crown surface to mimic the tobacco stains on the surrounding dentition. However, it was decided that cervical stains to mimic the decay on the natural dentition would not be placed. After staining, the lithium disilicate crown was crystallised and ready for immediate seating (Fig. 9). The specialised mouthpiece (Isolite) was repositioned in the mouth to isolate the tooth during cementation.
Dual-curing luting composite (Multilink Automix, Ivoclar Vivadent) was used to seat the crown. Indicated for use with metal, all-ceramic, metal-ceramic and composite restorations, the luting composite offers a strong hold on all surfaces and is available in transparent, yellow or opaque shades to ensure proper aesthetics are achieved. Additionally, the cement does not need to be protected from ambient light during mixing and placement.
Prior to application, the primer liquids (Multilink A/B) were mixed in a 1:1 ratio. A micro-brush was used to apply and lightly scrub the primer mix on the preparation enamel and dentine for 15 seconds. The priming agent was allowed to set on the enamel and dentine for 30 seconds, after which time air was used to evaporate the primer solvents. Because the primer is self-curing, light-curing was unnecessary.
The luting composite (Multilink Automix) was extruded from the mixing tip and placed directly on the inner surfaces of the lithium disilicate crown (Fig. 10). The luting composite was placed carefully to ensure that all internal surfaces were fully covered. The lithium disilicate crown was then seated on tooth #13 and slight pressure applied (Fig. 11).
A micro-brush was utilised initially to remove excess cement from the interproximal spaces and cervical areas of the crown (Fig. 12). Further pressure was applied with dental forceps to ensure the crown remained seated in the proper position during initial clean-up (Fig. 13). While still applying pressure to the seated crown, excess cement between the interproximal areas of the crown and surrounding dentition was removed with dental floss (Fig. 14). After flossing, the crown was cured with an LED curing light (bluephase G2, Ivoclar Vivadent) on the buccal, mesial, lingual and distal surfaces (Fig. 15). The interproximal spaces were then flossed to ensure that all excess cement had been removed (Fig. 16).
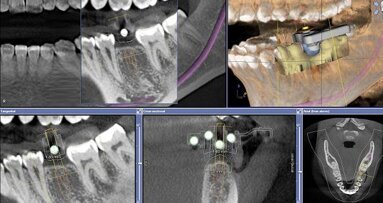
Upon completion of the case, the CAD/CAM-processed lithium disilicate glass-ceramic crown cemented with the dual-curing luting composite demonstrated excellent fit, function and strength (Figs. 17–20). Additionally, a post-operative radiograph confirmed that all excess cement had been removed and excellent internal/marginal adaptation achieved (Fig. 21).
The patient was very pleased with the aesthetics of the crown, which appeared natural and indistinguishable from the surrounding dentition. Further, the patient was pleased that he did not have to return for another appointment because the chairside CAD/CAM system allowed the restoration to be scanned, designed, milled and seated in a single appointment.
Conclusion
I use the CEREC CAD/CAM system almost exclusively in my practice because patients appreciate the quality, immediacy and not having to return for additional appointments. Restorations milled with CEREC demonstrate the form and fit required for restoring even the most challenging cases. Patients also enjoy the high aesthetics and strength of lithium disilicate glass-ceramic IPS e.max that has been milled with CEREC.
This article was originally published in CAD/CAM Vol. 2 No. 3, 2011. A complete list of references is available from the publisher.
CAD/CAM technology allows dental professionals to manufacture solid all-ceramic crowns chairside. A digital image of the preparation is captured with an ...
Dr. Gary Hack is an associate professor at the University of Maryland School of Dentistry, where he teaches in the Department of Advanced Oral Sciences and ...
Guided surgery has been around for a long time. However, very few dentists in the UK place implants using surgical guides. The reasons for this are ...
Dental crowns have been used for decades to restore compromised, heavily restored teeth, and for aesthetic improvements. New Computer Aided Design/Computer ...
In today’s fast-paced world, instant gratification is expected to be synonymous with worthwhile results. This also applies to dental treatments. While...
CAD/CAM technology continues to influence how dental practices and laboratories plan, design and deliver restorative treatment, and dental teams need to ...
At this year’s International Dental Show (IDS), Dr Marco Tudts, a renowned aesthetic and prosthetic dentist from Lier in Belgium, shares his insights on ...
The E4D in-office CAD/CAM unit (Editorial note: Planmeca E4D Technologies) has been employed in an investigative laboratory study to design and mill an ...
The prevalence of edentulous patients in Germany has been steadily declining for many years. According to the Sixth German Oral Health Study, the prevalence...
The aesthetics are always a significant challenge during implant restoration, especially in the aesthetic zone, in addition to the full consideration ...
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 pm EST (New York)
Live webinar
Thu. 11 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 11 June 2026
2:00 pm EST (New York)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Fri. 12 June 2026
8:00 am EST (New York)
Dipl.-Hdl. Joachim Brandes
Live webinar
Mon. 15 June 2026
11:00 am EST (New York)
Dr. Cristian Scognamiglio, Dr. Alessandro Perucchi



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





































To post a reply please login or register