We report the case of a 17-year-old patient who came into the clinic because she had noticed a colour change to the maxillary left central incisor (tooth #21) of 48-hour duration. During clinical examination, tooth #21 appeared darker than the rest of the teeth. After performing a complete exploration and obtaining no response to vitality tests, a pulp necrosis of tooth #21 was diagnosed.
Differential diagnosis began with the completion of the medical record. The patient had received orthodontic treatment and a supernumerary tooth in the anterior region of the maxilla had been extracted. The patient did not recall having suffered injuries or trauma in the incisal region.
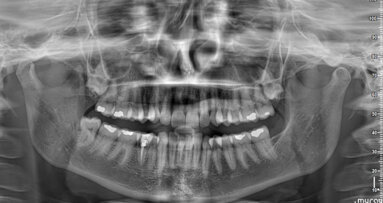
A dental panoramic tomogram was obtained, and a high-density area was observed at the apical level in the area of tooth #21. A 3-D computed tomography (CT) scan was then obtained, and it showed the presence of a supernumerary tooth in the periapical region of tooth #21, palatally located and oriented upwards. Necrosis by compression of the neurovascular pedicle of tooth #21 due to the expansion of the erupting follicle of the supernumerary tooth was diagnosed.
Pulpectomy and surgical removal of the supernumerary tooth were performed. During surgical removal of the supernumerary tooth, the neurovascular pedicle appeared oedematous and congested and was the cause of the tooth pulp necrosis.
Case report
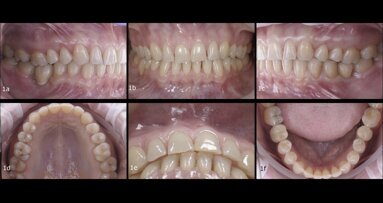
A 17-year-old patient who had undergone orthodontic treatment four years before came into the clinic because she had noticed a colour change to her maxillary left central incisor lasting for 48 hours. The patient presented with a tooth discoloration (Fig. 1) with slight pain that ceased with a non-steroidal anti-inflammatory drug. During the initial visit to her general dentist, vitality tests were performed and a slight response to the tests was detected. After that, the patient was referred to a specialist.
embedImagecenter("Imagecenter_1_1797",1797, "large");
When she presented to the endodontist, the tooth had darkened to a grey-brown colour. In addition to that, the tooth no longer responded to pulp vitality tests. During the visit, the endodontist performed periapical radiographs of the area (Fig. 2), and based on this the existence of a supernumerary tooth at the apical level of the incisor growing towards the floor of the nasal cavity was confirmed. The endodontist requested a CT scan to study the position and assess the possibility of surgical extraction.
The CT scan showed the position of the supernumerary tooth relative to the roots of the adjacent teeth, confirming growth towards the periapical region of tooth #21, that is, a 180-degree deviation from the correct orientation for eruption in the dental arch. Reconstruction in 3-D showed this phenomenon clearly (Figs. 3–6).
Endodontic treatment of tooth #21 was performed, during which the congested pulp was removed and some bleeding was observed. The length of the gutta-percha obturation was deliberately longer than required in order to facilitate surgery (Figs. 7–9).
Surgical treatment was planned and consisted of raising a semilunar flap on the periapical region of tooth #21 and performing a minimum root resection of 2 mm approximately without a bevel, using a size 0.23 round bur with a straight handpiece, to expose the supernumerary tooth’s crown. The crown was sectioned at the coronal middle third and the incisal portion was removed (Fig. 11). A hole was made in what would be the middle and cervical thirds of the supernumerary tooth to force it up (Fig. 12) and make the extraction through the osteotomy created for apicectomy, thereby achieving a complete extraction (Fig. 13) with minimal trauma to bone and the roots of the incisors.
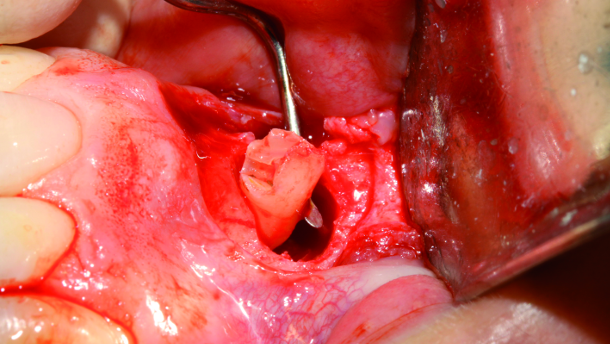
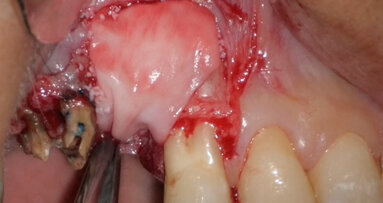
The oedematous pedicle that was compressed by the erupting follicle of the supernumerary tooth and caused a lack of blood supply to the pulp of the left central incisor can be observed in the image, held by a haemostat (Fig. 14).
Afterwards, preparation for retrograde root filling was performed using a Satelec ultrasonic system and the appropriate handpiece for this surgery. Retrograde root filling was performed with SuperEBA (Bosworth), thereby achieving sealing of the canal at apical level (Figs. 15 &16). The flap was closed with three silk sutures (Fig. 17), which were removed after seven days.
Supernumerary tooth after extraction can be observed in the picture (Fig. 18).
Two months after the intervention, internal whitening was performed to improve the colour of the incisor. The last two images show the clinical appearance (Fig. 19) and a radiograph (Fig. 20) three years posttreatment.
Discussion
CT scans, which have been widely used in endodontic diagnostics for fractures and fissures, for example, and in implantology, are not yet commonly used in surgical planning to obtain diagnostic and anatomical data. The relevant and detailed information that this imaging technique provides, especially regarding the position of supernumerary teeth, is proof that it should form part of the protocol during surgical planning.
The second point of discussion is the pathway used to approach the supernumerary tooth. We could have used a palatal pathway, but the CT scan revealed that the vestibular pathway was less risky, provided greater visibility and better respected the important anatomical structures, such as the adjacent teeth, without injuring them by accident and risking an iatrogenic injury.
Another important point to be observed is the pathophysiological mechanism that resulted in pulp necrosis. We suspected an apical or periapical resorption of tooth #21 because of the expansion of the erupting follicle and secondary osteolysis, which cannot be excluded. In order to eliminate the greatest number of cells involved in the resorptive-destructive process, an apicectomy was performed. Nevertheless, pulp congestion suggested that the most probable pathophysiological mechanism involved was venous stasis of the vascular plexus that enters the incisor, just before apex.
The last point of discussion is when these supernumerary teeth should be removed. If possible, the best time for removal is before any pathology signs appear. This requires consideration of the individual case of each patient, and performing clinical and radiographic follow-up of the case in order to determine the right time.
Conclusion
The presence of supernumerary teeth in the permanent dentition has a frequency of between 0.1% and 3.8%. Necrosis of the adjacent teeth is one of the possible complications of this phenomenon; therefore, clinicians must consider the possibility of a supernumerary tooth during diagnosis, especially in patients with pulp necrosis without previous traumatic dental pathology.
Editorial note: This article was published in cone beam – international magazine of cone beam dentistry No. 01/2015.
The SynCone Over Denture System is one restorative implant-supported removable option within the Ankylos Dental Implant System. The SynCone Over Denture ...
INDIANAPOLIS, US: Despite advances in periodontal disease research and treatments, it remains a growing health issue in the US. To address this topic, ...
In recent years, the technology associated with endodontic therapy has undergone a veritable revolution. For years, intraoral radiographs were used as the ...
The aetiology of external cervical root resorption remains unclear, and it is probably a multifactorial problem, causing dentine exposure to the oral cavity...
The unceasing innovations and iterations in dental technologies and materials have taken the sophistication of treatment modalities to a historic level. ...
The process of decision making is nowadays influenced by the continuous flux of information, the advancement of technology and the development of new ...
Dental technicians have so many different restorative materials and design and finishing concepts available to them that it can seem difficult to select the...
RIYADH, Saudi Arabia: While many artificial intelligence (AI) systems for dental diagnosis demonstrate high accuracy, their real clinical value depends on ...
Ectopic canines are a complex condition to treat with aligners only, since it is not easy to create a reliable and stable anchorage unit for forced ...
The terminology and classification of incomplete tooth fractures have received significant attention in the scientific literature for many decades. Numerous...
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 pm EST (New York)
Live webinar
Thu. 11 June 2026
1:00 pm EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






























To post a reply please login or register