Import and adaptation of images: after having acquired the video frames that statistically capture the dynamic phases of the smile and after having imported all the intra- and extra-oral photographs in the manner described in Part I, the smile designer, as if he or she were an architect, undertakes true and accurate mapping of the face and the smile, observing the peculiarities according to focal length. The aesthetic analysis (macro, mini and micro) to which it makes reference is based on values and parameters derived from Powell, Goldstein, Rufenacht, Lombardi, Arnett and Chiche, Pinault, Ricketts, Fradeani and others, and the aesthetic dentist can use these values and parameters with rulers, set squares and goniometers. The full face images of the patient also involve an analytical observation of the portrait and therefore hair and skin colour, make-up, pose, etc. are important. After being imported, these factors will be processed in the manner described below.
Verification of orientation and exposure of the subject photographed (Fig. 18a): the imported images must be verified on the basis of the quality of the shot, exposure, sharpness, etc., technical factors that most software packages can correct and improve, and some of which the Digital Firmware camera cauìn correct itself. Practice to acquire greater familiarity and skill will prove useful to the smile designer.
In addition to the qualitative factors, the correct orientation of the patient’s face is absolutely essential. Some software on Mac operating systems allows rotation of the image with a simple movement of the fingers. In general, however, it is possible to trace a bi-pupillary plane that the software will recognise as the horizontal plane to which to make reference for adapting the image.
embedImagecenter("Imagecenter_1_2115",2115, "large");
Another efficient method, with a dual function, is that of using the cropping grid. This offers the possibility of cropping the photograph to centre the image for use in ADSD. It permits us to align the bipupillary plane horizontally to check the symmetry in relation to the sagittal plane.
There is another simple but efficient way: increasing the zoom on the photograph. The pupils will be more detailed and thus, by rotating the photograph, it will be possible to take as a reference point the upper edge of the software window, on which to verify the pupillary alignment. Later on, it will be possible by scrolling the image towards the top to examine the mouth and the teeth to verify the occlusal plane.
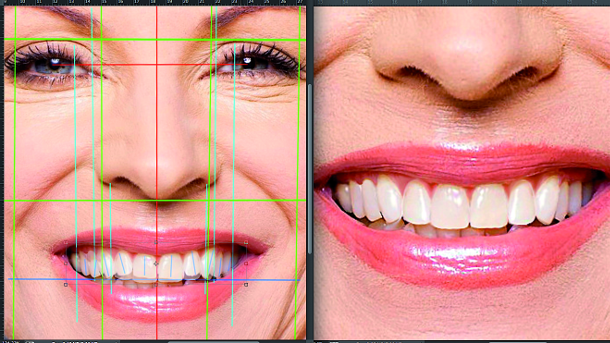
Mapping of the macro-aesthetics (face): having decided on the correct position of the face for a detailed aesthetic analysis and after a digital analysis, it is indispensable to mark the face and the smile with reference lines and areas, verifying symmetries and asymmetries (Fig. 18b). The first thing to do is to mark the reference points and morphological determinants (face marker); these should be saved in the project from the photograph because they are fixed anatomic topographical points in both the extra-oral and intraoral soft tissue, obviously bordering on the teeth and gingivae. From now on, it is essential to save the various ADSD projects. In this manner, we shall have immediately at our disposal the cardinal points of the topographic anatomy on which we shall later base the proportions of the face in terms of vertical and horizontal dimensions and the golden ratio analysis.
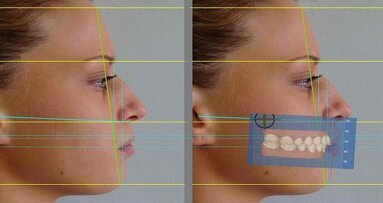
Mapping of the mini-aesthetics (mouth and smile): from the macro-aesthetic focal length, we can come closer to select the perioral and in traoral zone where it is necessary to carry out the virtual simulation after a careful dento-labial analysis (Fig. 18c).
The photographs taken statically with closed lips in relaxation, the lips spontaneously half-closed or the lips in a smile while pronouncing the phonemes “/m/” and “/i/” can be compared to video frames: from the recording of this data, we can evaluate movement, the dynamic curvature of the lower lip in relation to the maxillary anterior teeth, the position of the central incisors, their exposure and the breadth of the smile well delimited by the width of the labial corridors.
All of these factors are relevant to the smile design. It is also fundamental to verify the relationship with closed lips between the labial ver milion (analysed both frontally and in profile) and the labial dimensions useful for defining and comparing the vertical dimensions of the face, eventual losses or excesses of substance, bruxism, atrophic jaws, dental alignment, micro- or macrodontia, malocclusion or even simple loss of lip fullness, which is currently of great aesthetic interest not only clinically, but also and above all in the media.
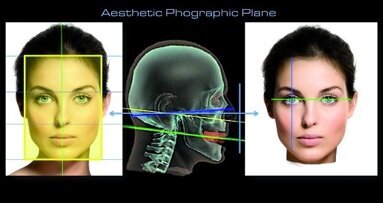
Often the multidisciplinary approach to a clinical case entails a preliminary examination by the plastic surgeon to establish the aesthetics of the labial profile. The plastic surgeon, who has to speak in favour of possible plastic surgery to the profile or the like, sends the patient to the dentist for a clinical evaluation of the dental–skeletal ratios, which is comparable with the aesthetic analysis of the entire profile of the face (Powell’s aesthetic triangle, Ricketts’ aesthetic plane, etc.). A dento-facial aesthetic analysis thus becomes a fundamental pillar for the co-operation between the specialists in the facial aesthetics medical team (Fig. 1 in Part I) to allow a predictable diagnosis and a treatment plan based on a multidisciplinary vision, considering the fact that the soft tissue of the lower third of the face is supported by and moves by sliding on the hard structures (bones and teeth).
In this regard, ADSD can be of help for analyzing the lateral thickness of the hard tissue, particularly the position of the anterior teeth, their inclination and their emergence profile. Indeed, it is possible to perform digital image editing analytically on a millimetre grid based on the reference points from the mapping of the facial profile. The simple superimposition of the images and the implementation of protocols or complementary examinations (virtual 3-D orthodontic simulations; vto; cephalometric analysis; dental design related to the thickness of veneers, overlays, prosthetic crowns, recontouring, etc.) can process virtual plans, in which it is possible to pre- dict the future position of the lips and vestibules (Fig. 19).
Mapping of the micro-aesthetics (intra-oral): the iconography of the analysed face includes the study of photographs taken with lip retractors in place (micro-aesthetics). The focus of this type of image is the close-up of the mouth, the details of which are relative to and parameterised according to the horizontal and vertical lines traced on the patient’s face. Our virtual project will centre on the occlusal plane ideally parallel to the bi-pupillary plane, and the main vertical lines (i.e. the median of the face, inter-incisal of the teeth, subnasal area, etc.).
The intra-oral mapping is thus a simple magnification of what has already been traced on the face. In practice, on our computer desktop, we will have a map in which there are very distinct regions, including outlines, ridges and depressions characteristic of the dento-facial morphology.
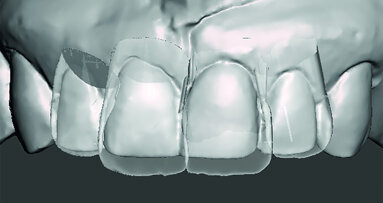
At this point, all we have to do is to start tracing lines (outlines; Figs. 11a & b in Part I) on the intraoral photographs, passing over the gingival margins, papillae, and interproximal margins of the central incisors, lateral incisors and canines (Digital Dental Design). In order to achieve a symmetrical drawing, the lines and contours of the teeth can be duplicated to create a mirror image. In this way, it is possible to obtain the positioning of the forms on the contralateral teeth. Among the lines used, it is very important to insert a line corresponding to the ideal aesthetic curve, which will have a value directly proportional to the position of the occlusal plane.
Paste or overlay the images taken from the Dental Digital Photo Database or model a filling of the outlines. In many cases, it is not strictly necessary to draw the teeth, since often the images of the teeth are copied, shaped, moved and positioned on the dental arch (Digital Dental Calibrated Transposition).
Position the teeth by reducing the opacity to place them with greater visibility in the desired positions. Opacity enables one to better visualise the underlying images when using tools for the superimposition of images, is an option in all photograph- editing software and can easily be adjusted in percentage.
Adapt and proportion the teeth in space (dimension and alignment) by using the images rendered semi-transparent by adjusting opacity comparable to the previous opacity (Fig. 18d).
Save the images where the transparency level enables us to calculate it as a superimposition (Figs. 20a & b), where the points of departure and arrival can be seen and where the sublabial dental composition can be seen (i.e. superimposing the micro-aesthetic images with the mini- and macroaesthetic ones, and being able to observe above and below the labial and perilabial soft tissue). Indicate and record on the photograph the unit of measurement chosen for the conversion scale of the software so that the data approximates clinical reality. If the measurements were previously according to an analogue or digital scale, you will be able to obtain optimal indications as regards reference points. For example, the position of the maxillary central incisors can provide information about the distance between the incisal edge or cervical margin and the subnasal or bi-pupillary line. Therefore, remember to indicate and record on the photograph the unit of measurement chosen for the software conversion scale so that the data approximates the clinical reality of the subject photographed.
Verify and modify the gingival architecture concerning the aesthetic component and tissue ratios. The positioning of the zenith, papillae and cervical parabolas represents an absolute value in aesthetic analysis for planning. It is particularly sensitive data useful for deciding on therapy with the periodontist.
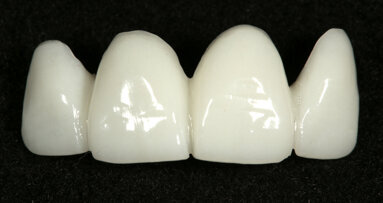
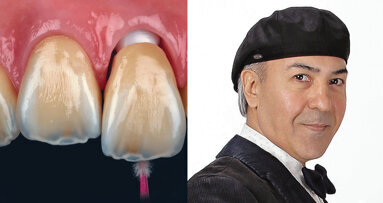
After finishing the positioning of the teeth and gingivae, shape them morphologically according to the customised aesthetic “plan”, bordering on the aesthetic dental composition (Fig. 18e).
Every image editing step relating to the simulation must be saved in the software format so that no data is lost to allow modification at a later date. The same must be done for JPG and similar formats in the patient’s file, re-naming them in a sequential manner, which permits a more reliable and revisable back-up for the smile designer and the aesthetic dental team, and permits a better method of communicating the various therapeutic possibilities to the patient. It also provides essential information for checking the positioning of the prototypes (Figs. 20c & 21a–c).
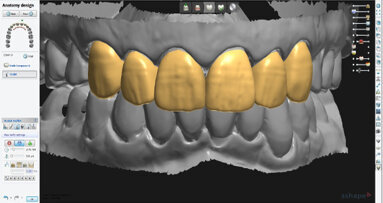
At this point, we have at our disposal the digital wax-up, which we can transfer to the dental technician so that he or she can create an actual diagnostic wax-up, which once photographed can be inserted into the oral cavity. Note that, where it is already possible to transfer the ADSD file into CAD, the CAM phase will produce a model that is useful for reducing the time and synchronizing the methods implementing the protocols. By decreasing the opacity of the image and working on the transparency, we can check whether the virtual records and indications conform to the analogue model.
If everything corresponds, it is possible to make modifications then to continue with the direct or indirect mock-up, which necessitates the preparation of a silicone key to accommodate provisional material to be adapted to the teeth or a workpiece produced by the dental technician without it being necessary to adapt the material to the teeth, such as composite veneer, resin and PMMA.
Having positioned the aesthetic model in the oral cavity, it is inspected and approved with the patient, correcting any individual or functional details from the point of view of occlusion, facial expressions and the dento-labial relationship, which can easily be tested using phonetic tests. In this phase, as well as giving the patient the opportunity to look at himself or herself in a mirror, it is very useful to use the camera again, since the recording of the physiology of the smile in relation to the phonetics and facial expressions may become the subject of further live 3-D analysis of the patient. The more information we send to the dental technician, the more it will be possible for him to observe the patient and update himself or herself on the analysis being carried out. While the dentist is in his or her surgery, the technician in the laboratory can watch the video clips, analyse the photographs and communicate via the telephone or video-conferencing on Skype. All this offers many advantages to this protocol. Being able to dispel any doubts will give greater satisfaction to the dental team and result in clinical success, clearly demonstrated by the aesthetic harmony in the smiles of our patients.
Once the mock-up has been approved with the consent of the patient, who will have been the first critical spectator of and commentator on the video clip, one can take another traditional dental impression or take an impression using an interoral scanner (optical impression). During the video playback, the patient is able to observe peculiarities about himself or herself that he or she would not be able to see using only a mirror, the first being seeing himself or herself in profile through images that are not static and precisely because of their dynamic nature correspond to spontaneity and naturalness.
Carry out digital smile morphing of the images step by step to demonstrate and transmit the actual simulation corresponding to virtual planning. This phase is of great interest and effect for the patientbecause morphing, being shown sequentially, appears to be like a film. This procedure is carried out as far as the superimposition of the images processed during the first analytical aesthetic phase up to the related functional models inserted into the oral cavity before the definitive restoration.
From the analogue phase of the model, we move on to the digital phase to produce the prosthesis with CAD/CAM procedures (these images can be further analysed in the virtual planning phase; Figs. 22a & b).
In the case of particular work procedures in which software-assisted implantology techniques are used, one may also have at one’s disposal a second model in PMMA, diagnostic or surgical guides especially for implant structures, etc.
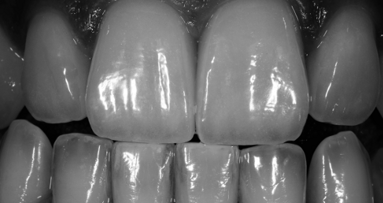
The final step in the implementation of ADSD in the CAD/CAM protocol is the placement of the definitive restoration in the oral cavity (Figs. 23a & b). The outcome of the multidisciplinary approach should confirm the predictability concerning the aesthetic and bio-cosmetic integration of the prosthesis.
Conclusion
The detailed analysis of the smile and its project, indispensable for the formulation of an aesthetic clinical diagnosis, is a fundamental part of the delicate approach to the patient, the true protagonist of aesthetic dentistry. Today, the operator has at his or her disposal new non-invasive means of formulating the treatment plan; digital dentistry and image-editing software are now part of a dentist’s armamentarium. Furthermore, the entire treating team being advanced in the use of instruments and technologies for diagnosis and communication makes an excellent marketing tool for dental services. ADSD is a simple and economical way of offering the patient a predictable plan that can be visualised immediately or at least at the second appointment to demonstrate the aesthetic and functional changes possible with treatment with the aid of corresponding models. It is also a tool for transmitting all the information necessary to the entire treating team in the multidisciplinary approach. Let us hope that a new professional figure may soon establish himself or herself in the world of dentistry, the smile designer, a new way to communicate.
Note: Figures 18a–e are demo simulation of ADSD method, they are not a case report.
Editorial note: This second part of a two-part article was published in cosmetic dentistry No. 2/2015. Part I of the article appeared in cosmetic dentistry No. 1/2015.
The concept of aesthetics has been explored by various authors and discussed by eminent philosophers. While their definitions are subjective, they all agree...
MANGALORE, India: Digital smile design has begun employing artificial intelligence (AI), raising questions about the quality and acceptability of ...
The communication between dentist and patient is important, especially in cases of partial or complete aesthetic restoration in the anterior (smile ...
Achieving a successful outcome in aesthetic dentistry can be a formidable challenge for all dental practitioners, regardless of their experience level. The ...
Dentofacial abnormalities are alterations in facial proportion and dental relationships, and such abnormalities in dental and facial appearance often lead ...
There are times when we copy the natural teeth of patients and fabricate an identical yet improved version of them. This means that we apply improvements on...
The fabrication of restorations has entered a new technological age, moving from 2-D to 3-D. Restoration design—whether it is a framework, full-mouth ...
Aesthetic medicine is increasingly taking on a global connotation of harmony and balance, defined certainly by historically evolved and shared canons, but ...
Success in aesthetic dentistry depends on biology, function and mechanics; aesthetic dentistry cannot exist independently. Cosmetic dentistry had the ...
SCHAAN, Liechtenstein/ROME, Italy: Digital and aesthetic dentistry will be in the spotlight at Ivoclar Vivadent’s fourth International Expert Symposium, ...
Live webinar
Thu. 14 May 2026
12:00 pm EST (New York)
Live webinar
Thu. 14 May 2026
2:00 pm EST (New York)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Tue. 19 May 2026
11:00 am EST (New York)
Live webinar
Tue. 19 May 2026
1:00 pm EST (New York)
Prof. Dr. med. dent. Ivo Krejci
Live webinar
Wed. 20 May 2026
7:00 am EST (New York)
Dr. Graham Carmichael BDSc (Hons), DClinDent (Pros), FRACDS, Dr. Robert Gottlander DDS
Live webinar
Wed. 20 May 2026
9:00 am EST (New York)
Live webinar
Wed. 20 May 2026
1:00 pm EST (New York)
Prof. Dr. med. dent. Tim Joda PhD, MSc, eMBA



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





































To post a reply please login or register