Four thousand years ago, a number of Babylonian legal decisions were compiled in what came to be known as the Code of Hammurabi. The one referencing the construction of dwellings and the responsibility for their safety begins: If a builder engineers a house for a man and does not make it firm, and the structure collapses and causes the death of the owner, the builder shall be put to death.
We are all builders or engineers of sorts; we calculate the path of our arms and legs with the computer of our brain, and we catch baseballs and footballs with greater dependability than the most advanced weapons system intercepts missiles. In our professional lives, however, in contradistinction to the paradigm of evidence-based dentistry, our efforts as builders often rely solely upon personal experience, intuitive cognition and anecdotal accounts of successful strategies.
The challenges posed by implant-driven treatment planning mandate vigilance of the interaction between those involved in research and development, manufacturing and distribution and the leaders of ideologically diverse disciplines. Temporal shifts and trends in the service mix are part of the evolution of the art and science of dentistry; to some degree, the implant-driven vector has captured the heart and minds of those who seek to nullify preservation of natural tooth structure in the oral ecosystem and deify orthobiologic replacement. The corporate entities from which we derive our tools too often fail to distinguish the point where science ends and policy begins.
By positioning advocates and acolytes at the vanguard of their marketing campaigns, they effect change; however, their support for education is directed toward dissemination of product, not the fundamentals and rudiments of biologic imperatives. Prospective large cohort clinical trials with clearly defined criteria for survival, with and without intervention, quality of life information and economic outcomes, are essential to compare alternative foundational treatments. These studies will require expertise, time and financial support from the various stakeholders, professional and corporate alike1.
“The authority of those who teach is often an obstacle to those who want to learn.” — Cicero
The prosthodontic pundits maintain that the spiraling costs of saving endodontically retreated teeth, where extraction may well prove to be the common endpoint, begs the question of whether such teeth should be sacrificed early. Ruskin et al concluded that implants have greater success than endodontic therapy, are more predictable and cost less when you consider the “inevitable” failure of initial root canal treatment, retreatment and periapical surgery.2
Is it responsible therapeutics or irresponsible expediency that justifies the removal and restoration of such teeth from the outset with an implant-supported restoration? Can one ethically argue that extraction is warranted as the financial cost of orthodontic extrusion/soft tissue surgery, endodontic retreatment and post/core/crown fabrication is greater than extraction with an implant-buttressed restoration, and in all likelihood, more predictable3?
Jokstad et al4 identified more than 220 implant brands in the dental marketplace. With variability in surface, shape, length, width and form, there are potentially more than 2,000 implants for any given treatment situation. A systematic review by Berglundh et al5 assessed the reporting of biologic and technical complications in prospective implant studies. Their findings indicated that while implant survival and loss were reported in all studies, biologic difficulties such as sensory disturbance, soft-tissue complications, peri-implantitis/mucositis and crestal bone loss were considered in only 40 to 60 per cent of studies.
Technical complications such as component/connection and superstructure failure were addressed in only 60 to 80 per cent of the studies. Are we as a profession standing idly by and watching marketing pressures force treatment decisions to be made empirically, with untested materials and techniques? There is an unsettling similarity between these events and the early days of implant development6.
The endodontic pundits argue major studies published to date suggest there is no difference in long-term prognosis between single-tooth implants and restored root canal-treated teeth. In fact, regardless of the similarity of treatment outcomes, the preponderance of post-treatment complications favors endodontic therapy.
Therefore, the decision to treat a tooth endodontically or to place a single-tooth implant should be based on criteria such as restorability of the tooth, quality and quantity of bone, esthetic demands, cost-benefit ratio, systemic factors, potential for adverse effects and patient preferences.7-11
A review of endodontic treatment outcomes by Friedman and Mor12 used radiographic absence of disease and clinical absence of signs and symptoms as the defining parameters for success. They suggested the chance of having a tooth extracted after failure from initial endodontic treatment, retreatment and apical surgery collectively would be roughly one in 500 cases.
The dialogue comparing “endodontic treatment vs. implant therapy” jarringly overlooks the crucial fact that it is often the caliber of the restoration and its prognosis and not the endodontic prognosis per se, that is the determinant of the treatment outcome. The primary biologic mandate of any dental procedure is the retention of the orofacial ecosystem in a disease-free state. Surgical and nonsurgical endodontic therapies have historically been key modalities in the attainment of this foundational goal. Friedman noted “the patient weighing one ‘success’ rate against the other may erroneously assume their definitions to be comparable and select the treatment alternative that appears to be offering the better chance of ‘success.’ ”13 The conundrum researchers and clinicians alike wrestle with increasingly includes the non-science of emotion as well.
This publication will address non-surgical and/or surgical resolution of failing primary endodontic treatment outcomes and the historic and ongoing efforts of the dental industry to successfully engineer the biomimetic replacement of natural teeth and replicate the structural predicates that comprise the substitution algorithm of bone, soft tissue and tooth. There are many levels to the accrual of “best evidence dentistry.” The purpose of this paper is to ensure all variables in the treatment-planning equation of foundational dentistry are understood and given equal weight in the comprehensive care decision-making process.
Whenever possible, the treatment choice should be an attempt to salvage a tooth using a multidisciplinary team approach, putting aside preconceived notions and biases. Finances should not dictate the advice proffered. Furthermore, it is advisable to forego being clinically “conservative.” Treatment should not be initiated in the absence of a critical evaluation of the potential for all contributing factors to equate with a positive outcome. When needed, care must be taken to carry out every diagnostic procedure available, even those of a more invasive nature. (See Fig. 1: The term ‘tipping point’ refers to the moment of critical mass, the threshold, the boiling point. The color sequence highlights the diagnostic steps to be followed in each tipping point algorithm for the listed pathologic states.) Before arriving at a definitive diagnosis and treatment plan, the clinician should obtain consent from the patient to remove any restoration in order to analyze the residual tooth structure and assess the potential to carry out reliably predictable treatment. The patient must understand in detail the feasibility of and margin for success of each treatment option presented.14
embedImagecenter("Imagecenter128",128);
There are few studies in the endodontic literature analyzing the reasons for extraction of endodontically treated teeth. Root-filled teeth are invariably prone to extraction due to non-restorable carious destruction and fracture of unprotected cusps. Tamse et al found that mandibular first molars were extracted with greater frequency than maxillary first molars; the most significant causal difference was the incidence of vertical root fracture (VRF — 1.8 per cent maxillary molar, 9.8 per cent mandibular molar).15 Teeth not crowned after obturation are lost with six times the frequency of those restored with full coverage restorations.16
Procedural failure, iatrogenic perforation or stripping, idiopathic resorption, trauma and periodontal disease all contribute to a lesser degree. The major biologic factor influencing endodontic treatment outcome failure with the possibility of extraction appears to be the extent of microbiological insult to the pulp and periapical tissue, as reflected by the periapical diagnosis and the magnitude of periapical pathosis.17 (See Table I; Fig. 2a: The use of dyes, coloring agents and micro-etching is invaluable in visualizing a suspected crack in tooth structure. Cohen et al found when premolars were used as bridge abutments, a surprising number of these abutments sustained a VRF. [J Am Dent Assoc 2003; 134(4)434-441]; and Fig. 2b: The dental literature reports a statistically higher level of accuracy using cbCT [cone beam volumetric tomography] scans for detecting vertical root fractures than with the use of periapical radiography alone; Fig. 2c: The multivariate nature of the endodontic implant algorithm mandates the use of cbCT to detect and evaluate the degree of periapical pathosis. Analysis of the size, extent, nature and position of periapical and resorptive lesions in three dimensions is essential for the optimal level of standard of care in diagnosis.)
Dentin is the most abundant mineralized tissue in the human tooth. In spite of this importance, over half a century of research has failed to provide consistent values of dentin’s mechanical properties. In clinical dentistry, knowledge of these properties is pivotal to any number of variables ranging from innovations in preparation design to the choice of bonding materials and methods. The Young’s modulus (the measure of the stiffness of an isotropic elastic material) and the shear modulus (modulus of rigidity) are diminished by visco-elastic behaviour (time-dependent stress relaxation) at strain rates of physiologic (functional) relevance. The reported tensile strength data suggests that failure initiates at flaws. These flaws may be intrinsic, perhaps regions of altered mineralization, or extrinsic, caused by cavity or post channel preparation, wear or damage. There have been few studies of fracture toughness or fatigue.18 Finally, little is known about the biomechanical properties of altered forms of dentin subsequent to decay, the influence of irrigants, chemicals and the choice of curing techniques used for bonded restorations.19
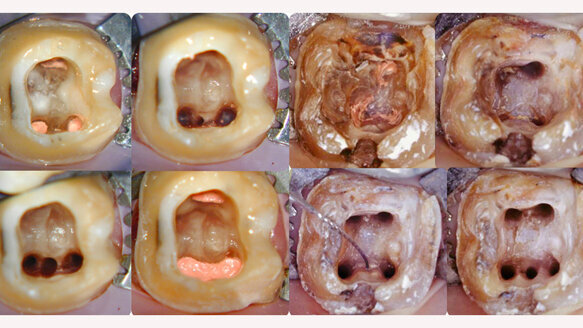
Studies suggest there are at least two forms of transparent or sclerotic dentin; a form associated with caries and a form associated with age-related changes in the root. The impact upon tooth strength as a function of these altered forms of dentin is not well understood. The long-term predictability of residual coronal tooth structure to function in a manner commensurate with the demands of the orofacial ecosystem, may need to be reassessed in light of observations that sclerotic dentin, unlike normal dentin, exhibits no yielding before failure and that the fatigue lifetime is deleteriously affected at high stress levels.20 Mechanisms for energy dissipation and crack growth resistance present in young dentin are not present in old dentin. Restorative methods and techniques, particularly as it relates to ferrule creation for endodontically treated teeth, may need to be amplified to address the fact that fatigue crack growth resistance of dentin decreases with age.21 (See Fig. 3: Two different retreated teeth; two different potential treatment outcomes. The root-canal system of both teeth has been reengineered in its anatomic entirety; however, the treatment outcome after restoration for both is unlikely to be the same. Regenerative technologies incorporating mesenchymal stem cells derived from dental tissues may one day obviate the concern.)
Understanding the mechanical properties of teeth is essential in order to address the most common clinical problem affecting all endodontically treated teeth; fracturing, which in spite of even minimal loss of tooth structure, may be severe enough to necessitate removal.22-24 The hypothesis that dentin brittleness increases with diminished moisture content has been debunked; conserving bulk dentin is the sine qua non of fracture prevention.
Kuttler et al reported that dentin thickness correlates inversely to post space diameter in the distal roots of mandibular molars.25 A #4 Gates-Glidden drill caused strip perforations in 7.3 per cent of canals studied. The authors recommend Gates-Glidden drills no larger than a size #3 be used. After endodontic treatment, the furcation side dentin thickness was less than 1 mm in 82 per cent of the distal roots studied. (See Fig. 4: A) Less porous, less hydrated and highly mineralized outer dentine. B) Pulp canal space. C) More porous, more hydrated and less mineralized inner dentin. D) Water in the dentinal tubules and pulp space is held in a confined environment under hydrostatic pressure.)
There are primary causes that predispose teeth to fracture and secondary causes that predispose fracture after a period of time. (See Fig. 5: Primary causes of fracture include excessive structure loss, loss of free unbound water from the root canal lumen and dentinal tubuli, age-induced changes in the dentin and restorations and restorative procedures. Secondary causes of fracture include the effects of endodontic irrigants and medicaments on dentin, the effects of bacterial interaction with dentin substrate and bio-corrosion of metallic post-cores.)
Endodontics is a component of an interdisciplinary process and a chain is only as strong as its weakest link. Subsequent to any endodontic procedure, intensity of stress concentration and tensile stresses within an endodontically treated tooth will depend upon 1) the material properties of the crown, post and core material chosen, 2) the shape of the post, 3) the adhesive strength at the crown–tooth, core–tooth and core– post, post–tooth interfaces, 4) the magnitude and direction of occlusal loads, 5) the amount of available tooth structure and 6) the anatomy of the tooth. Any combination of vectored stress concentration and high tensile stresses will predispose these teeth to fracture without an adequately engineered restorative design.
Re-engineering
Reengineering negative treatment outcomes is a significant part of the contemporary endodontic oeuvre. The presence of apical periodontitis may or may not affect the outcome of initial endodontic treatment26; however, there is a general consensus that apical periodontitis is the most important variable influencing a positive outcome with non-surgical and surgical retreatment.27-29 Positive treatment outcomes may be more likely in certain teeth with a combination of both procedures rather than with one or the other alone. (See Fig. 6: The image on the left is a flat field periapical radiograph; the one on the right, a small focal field cone beam volumetric tomograph [Kodak 90003D, Kodak Dental Systems, Woodbridge Conn.]. The differential in visualization of periapical pathology from a 3-D to a 2-D image is as much as 2:1 [Estrela et al, 2009]).
The premise that non-surgical retreatment improves the outcome of periapical surgery has been supported by both historical and current studies.30-32 Apical surgical “correction” of intracanal infections may isolate, but not eliminate, the residual microflora of the root canal space. It should therefore be limited to situations where non-surgical retreatment is judged impractical. With the range of sophisticated equipment and material in the conventional endodontic armamentarium, this is a remote consideration at best. When the etiology is independent of the root-canal system, surgery is the most beneficial treatment.33 Non-surgical retreatment may still be indicated in these cases, especially when intracanal infection cannot be ruled out. Time constraints or financial pressures should never be a factor in making surgery the first treatment choice. (See Fig. 7: The initial endodontic treatment procedure was inadequate and failing. Reengineering [inclusive of interim calcium hydroxide therapy] ensured optimal eradication of microflora from the root canal space, and the obturation produced definitive closure of the apical termini. Surgery was performed to redress persistent symptoms.)
The variables associated with non-surgical retreatment are myriad and treatment outcome studies in endodontics have been egregiously abused by those wishing to diminish the value of reengineering natural teeth. Many studies have categorized teeth with caries, fractures, periodontal involvement and poor coronal restorations as negative endodontic outcomes.34,35
Prior procedural errors36, occlusal considerations37, material choice for the restoration38 and design of the full coverage component all suggest that success is a function of comprehensive treatment planning as much as technical expertise. Evidence-based or controlled best evidence studies should conclude these are non-endodontic causes of failure and the success of endodontic treatment itself is high and predictable.
Kvist and Reit39 have shown that while surgical cases may demonstrate higher healing rates than non-surgical retreatment cases initially, four years out there was no difference between the two modalities due to “late” surgical failure. The failure rate for surgical therapy appears to be analogous to the failure rate for retreatment as a function of the size of the lesion treated.40 Levels of apical resection41 and the type of root end filling material make a difference in surgical treatment outcome success42; however, the dentin bonded composite technique and the use of compomer materials has not been widely reported. As these techniques dome the resected root face, sealing off the cut tubuli, they may prove to be the most effective retrograde surgical protocols of all. In regard to periapical re-surgery, the literature is unclear.
Gagliani et al43 compared periapical surgery and re-surgery over a five-year follow-up period. Using magnification and microsurgical root-end preparations, the positive outcome for primary surgery was 86 per cent and 59 per cent for re-surgery. While others have shown positive outcomes for re-surgery, the decision remains highly case specific. In spite of our best efforts, negative endodontic treatment outcomes occur and orthobiologic replacement of teeth and their surrounding anchoring structures is an integral part of contemporary foundational treatment planning.
A recent article by Assuncao et al44 describes engineering methods used in dentistry to evaluate the biomechanical behaviour of osseo-integrated implants. Photo-elasticity is used for determining stress concentration factors in irregular geometries. The application of strain-gauge methodology on dental implants provides both in vitro and vivo measurement strains under static and dynamic loads. Finite element analysis can simulate stress using a computer-created model to calculate stress, strain and displacement.
An analysis of the impact of mechanical/technical risk factors on implant-supported reconstructions is beyond the scope of this publication; however, the replacement of lost teeth by implants should, without exemption, provide a feeling of restitutio ad integrum. The means by which the restoration of the original condition at the “crown/root” interface is idealized will be detailed.
“The structure and composition of teeth is perfectly adapted to the functional demands of the mouth, and are superior in comparison to any artificial material. So first of all, do no harm ...” – Anonymous
Back to the egg
An increased uniform amount of coronal dentin significantly amplifies the fracture resistance of endodontically treated teeth regardless of the post system used or the choice of material for the full coverage restoration.45 A recent article by Coppede et al demonstrated that friction-locking mechanics and the solid design of internal conical abutments provided greater resistance to deformation and fracture under oblique compressive loading when compared to internal hex abutments.46 These two “seemingly” disparate observations define the inherent continuum between natural tooth engineering and the principles of engineering necessary to orthobiologically replicate the native state.
The use of a ferrule or collet and a bonded or intimately fit post-core to restore function and form to an endodontically treated tooth is analogous to the use of a long, tapered friction fit interface with a retaining screw (Morse taper) to secure an abutment to a fixture. In both cases, the role of contact pressure between mating surfaces to generate frictional resistance provides a locked connection. This has been shown to affect long-term stability of crestal bone support for the overlying gingival tissues and maintains a healthy protective and esthetic periodontal attachment apparatus47.
The Roman architect Vitruvius’ (Marcus Vitruvius Pollio) description of the perfect human form in geometrical terms was a source of inspiration for Leonardo da Vinci who successfully illustrated the proportions outlined in Vitruvius’ work “De Architectura.” The result, the Vitruvian man, is one of the most recognized drawings in the world and is accepted as the standard of human physical beauty. Vitruvius theorized that the essential symmetry of the human body with arms and legs extended should fit into the perfect geometric forms; the circle and the square. It took Leonardo Da Vinci to recognize that the circle and the square are only tangent at one place, the base. Observe the insert. (See Fig 8: The strength of the ‘egg like’ coronal structure of a tooth can support substantial occlusal stress and force; however, disrupting the integrity of the ‘dome’ or roof of the pulp chamber with an access preparation will invariably lead to a statistically significant degree of fracturing after endodontic therapy.16) The stabilizing platform for the human form outlined begins at that tangent; the intersection is graphically analogous to the structural configuration of platform switching.
The relative simplicity of this construct reinforces the obvious. When we compare design in living things to the artificial designs they inspire, a striking parallel emerges. Almost all the products of man’s technology are no more than imitations of those in nature and usually, they fail to match the superior design in living things.
Consider the engineering perfection that is the egg. Its strength lies in its oblate spheroid shape. A blow to the side of an egg from a sharp object puts pressure across the thin shell and breaks it easily. However; if the egg is squeezed directly on its poles, the vectored pressure is compressed along the surface structure, not across the shell; the egg cannot be broken without extraordinary force. However, if a pin hole is created in one of the poles disrupting the integrity of the structure, the pressure will readily break the egg, commensurate with a sharp blow to the side.
In geometry, an oval is a curve resembling an egg or an ellipse. Architects and engineers have used smooth ovate curves to support the weight of structures over an open space literally since the second millennium BC. These arches, vaults and domes can be seen in buildings and bridges all over the world; the most pervasive example being the keystone arches used by the Romans for aqueducts and mills.
An arch directs pressure along its form so that it compresses the building material from which it is constructed. Even a concrete block is readily broken if you hit it on the side with a sledgehammer. But under compression forces from above, the block is incredibly strong and unyielding. Many will remember the weight-bearing tripod experiments from grade school where an egg acts as one of three supporting legs of a square section of wood bearing books as the load. The structure could support more than 60 books, almost 20 pounds, before breaking the supporting egg. One need only look at the root trunk and coronal tooth structure of a multi-rooted teeth and it becomes apparent that strength of the tooth form is dependent upon an arch form for its integrity (Fig. 8 [see above] and Fig. 9: An arch eliminates tensile stresses in spanning an open space as all forces are resolved into compressive stresses. It requires all of its elements to hold it together, thus making it self-supporting. The incorporation of platform switching into the design of an implant abutment simulates three oblate spheroid shapes; one vertical, two horizontal. The objective is to ensure axially vectored compressive stresses are contained within an idealized shape that is structurally enhanced by the use of a precise friction fit connection.)
Is it possible for this natural feat of engineering wonder to be biomimetically replicated to the design parameters of osseo-integrated implants? There are a number of paradigms that continue to fuel debate in the dental clinical and scientific communities pertaining to the optimal engineering predicates for implant design. These include smooth vs. rough surfaces, submerged vs. non-submerged installation techniques, mixed tooth-implant vs. solely implant-supported reconstructions, Morse taper abutment fixation vs. a butt-joint interface and titanium abutments vs. esthetic abutments in clinical situations where esthetics is of primary concern.
The cone-screw abutment has been shown to diminish micromovement by reducing the burden of component loosening and fracture. This enables the identification of the effects of the parameters such as friction, geometric properties of the screw, the taper angle and the elastic properties of the materials on the mechanics of the system. In particular, a relation between the tightening torque and the screw pretension is identified. It was shown that the loosening torque is smaller than the tightening torque for typical values of the parameters. Most of the tightening load is carried by the tapered section of the abutment, and in certain combinations of the parameters the pretension in the screw may become zero.
This enables the identification of the effects of the parameters such as friction, geometric properties of the screw, the taper angle and the elastic properties of the materials on the mechanics of the system. In particular, a relation between the tightening torque and the screw pretension is identified. It was shown that the loosening torque is smaller than the tightening torque for typical values of the parameters. Most of the tightening load is carried by the tapered section of the abutment, and in certain combinations of the parameters the pretension in the screw may become zero. This tapered abutment connection provides high resistance to bending and rotational torque during clinical function, which significantly reduces the possibilities of screw fracture or loosening.
Biomechanics
“The seed of a tree has the nature of a branch or twig or bud. It is a part of the tree, but if separated and set in the earth to be better nourished, the embryo or young tree contained in it takes root and grows into a new tree.” — Newton
Pressure on the cervical cortical plate, micro-movement of the fixture-abutment interface (FAI) as well as microflora leakage and colonization at and within the FAI are some of the pathologic vectors associated with osseous remodeling, both crestal and peripheral to dental implants.48 Occlusal considerations engineered into fixture design should enable optimum load distribution for permanent load stability during functional loading, reduce functional stress transfer to the interfacial tissues and enhance the biologic reaction of interfacial tissues to occlusally generated stress transfer conditions.49 Future modifications to implant biomechanics should focus on designs wherein the osseous trabecular framework retaining the fixture will adapt to the amount and the direction of applied mechanical forces, cope with off-axis loading, compensate for occlusal plane to implant height ratios differences as well as adjusting to mandibular flexion and torsion.50
In this new era of implant-driven treatment planning, fixtures should be engineered to support single crowns with cantilevers instead of implant/implant or implant/teeth connections for a span of any degree. These engineering design iterations will minimize high-stress torque load at the implant abutment interface and obviate areas with degrees of bone insufficiency. The goal should be to biomimetically replicate the natural state to the greatest degree in regard to load bearing capacity. (See Fig. 10a: Foundational dentistry mandates that the impact of an orthobiologic replacement unit be commensurate with the biologic objectives and functional requirements of the natural tooth; and Fig. 10b: As the number of implant-supported single tooth replacements increases, implant-abutment connection design should ensure that occlusal table replication displays equivalency in both dimension and cuspal inclination with the surrounding natural dentition.)
Stable crestal bone levels are the yardstick by which treatment success and health are measured in the orofacial ecosystem whether it relates to natural tooth retention or restorative and/or replacement rehabilitation. It is therefore surprising the treatment outcome standards for osseo-integration accept crestal bone remodeling and resorption of up to 1.5–2 mm during the first year following fixture placement and prosthetic insertion.51
The concept of “biological width” outlines the minimum soft-tissue dimension physiologically necessary to protect and separate the osseous crest from a healthy gingival margin surrounding teeth and the peri-implant environment.
A bacteria-proof seal, the lack of micro-movement associated with a friction grip interface and a minimally invasive second-stage surgery (where indicated) without any major trauma to the periosteal tissues are also important factors in preventing cervical bone loss. The literature suggests the stability of the implant/abutment interface may have an important role in determining crestal bone levels.52 Tarnow’s seminal study on crestal bone height support for the interdental papilla clearly showed the influence of the bony crest on the presence or absence of papillae between implants and adjacent teeth.53 Twenty years later, logic dictates anticipated early crestal bone loss and diminished, albeit continual loss, during successive years of function, should have been engineered out of the substitution algorithm for peri-implant tissues.54
Platform switching: by default or by design
“There is no logical way to the discovery of elemental laws. There is only the way of intuition, which is helped by a feeling for the order lying behind the appearance.” — Einstein
Platform switching theorizes that by using an abutment diameter of a lesser dimension than the periphery of the implant fixture, horizontal relocation of the implant-abutment connection will reduce remodeling and resorption of crestal bone after insertion and loading. The concept implies peri-implant hard-tissue stability will engender soft-tissue and papilla preservation.
Maeda et al reported stress levels in the cervical bone area peripheral to a fixture were greatly reduced when a narrow diameter abutment was connected in comparison to a size commensurate with the fixture diameter.55 The authors concluded the biomechanical advantage of shifting stress concentrations away from the cervical area diminishes the impact on the biologic dimension of hard and soft tissue extending apically from the FAI. (See Fig. 11a: The composition of biologic width around implants. Sulcus depth (SD) — distance from peri-implant mucosal margin PM to the most coronal point of junctional epithelium (cJE). Junctional epithelium (JE) — distance from cJE to the most apical point of the junctional epithelium (JE) — distance from cJE to most apical point of the junctional epithelium (aJE). Connective tissue zone (CT) — distance from aJE to the first bone-to-implant contact (BC). [Source: The influence of mucosal tissue thickness on crestal bone stability around dental implants. Tomas Linkevicus, Riga Stradins University]; Fig. 11b: When a matching implant–abutment diameter is used, the inflammatory cell infiltrate is located at the outer edge of the implant-abutment junction close to crestal bone; this close proximity may explain, in part, the biologic and radiographic observations of crestal bone loss or saucerization around restored implants. This is not peri-implantitis or mucositis; however, any area of bacterial accumulation and stasis, inaccessible to normal hygiene protocols, is a risk factor for exacerbation; and Fig. 11c: The Morse taper connection of the Ankylos C/X (internal index) fixture distributes oblique and horizontally applied forces over a large area of the matrix joining surface inside the implant. The connection is therefore only loaded in the vertical direction. The cross section shows no gap between the abutment taper and the implant, which avoids micro-loosening. This is in contrast to systems with internal hex connections (clearance fit), which demonstrate micro-motion and ‘rotational slop,’ making them prone to inflammatory reactions at the implant-abutment connection due to micro-leakage.) The inherent disadvantage is it shifts stress to the abutment screw with the potential for loosening or fracture.
Ericsson et al56 detected neutrophilic infiltrate in the connective tissue zone contacting the implant-abutment interface. The facility by which platform switching/shifting reduces bone loss around implants has been investigated by Lazzara et al.57
The authors hypothesized if the abutment diameter matches the implant, the inflammatory cell infiltrate is formed in the connective tissue contacting the microgap created at the FAI. If an abutment of narrower diameter is connected to a wider neck implant, the FAI is shifted away from the outer edge of the implant, thus distancing inflammatory cell infiltrate away from bone. Hypothetically, less crestal bone loss is expected and an increased implant/abutment disparity allows more stable peri-implant soft-tissue integration.
Baggi et al conducted a finite element analysis experiment to define stress distribution and magnitude in the crestal area around three commercially available implants: ITI Straumann (Institut Straumann AG, Basel CH), Nobel Biocare (Nobel Biocare AB, Goteborg SE) and Ankylos C/X (Dentsply-Friadent, Manheim, DE).58
Numerical models of maxillary and mandibular molar bone segments were generated from computed-tomography images and local stress vectors were introduced to allow for the assessment of bone overload risk. Different crestal bone geometries were also modeled. Type II bone quality was approximated and complete osseous integration was assumed. It was concluded the Ankylos C/X implant based on its platform switched and subcrestally positioned design demonstrated better stress-based performance and lower risk of bone overload than the other implant systems evaluated.
Platform switching, together with a stable implant-abutment connection, are increasingly accepted essential implant design features required to reduce or eliminate early crestal bone loss. A bacteria-proof seal, a lack of micro-movement due to a long friction grip tapered channel and minimally invasive second-stage surgery without any major trauma for the periosteal tissues are also important factors in preventing cervical bone loss. A preconfigured platform switched design has a significant impact on the implant treatment in esthetic areas as not only is the tissue biotype preserved, but it has been shown to be enhanced by osseous generation over the collar of the fixture. (See Fig. 12a: The platform ‘switched’ design negates micro-motion and resultant crestal bone resorption. The goal of orthobiologic replacement is idealized replication of the natural state; and Fig. 12b: The expectation of a precise cone fixture-abutment connection is that the crestal bone will overgrow the fixture platform and remain in that position regardless of whether the implant was placed in a grafted site or immediately placed in an extraction site. Die-back or saucerization is not a consideration.)59,60
The endodontic implant algorithm parallels the question, “Which came first, the chicken or the egg?” as an example of circular cause and consequence.
It could be reformulated as follows: “Which came first, X that can’t come without Y, or Y that can’t come without X?” An equivalent situation arises in engineering and science known as circular reference in which a parameter is required to calculate that parameter itself. This is the essence of foundational dentistry.
If nature creates the ideal, are we as clinicians not responsible for replicating the ideal should adverse conditions irrevocably alter nature and necessitate its elimination?
Nature wisely created a structure that could harmoniously interpolate hard and soft tissue, act as the portal of nutrition and communication for the body and be the gatekeeper on guard and in function throughout our lifetime. As such, our role is to ensure that however we reengineer nature, we must adhere to its rules, its logic and fundamentals.
This is not an easy task as filtering out the best range of evidence from a wide range of sources, presenting clear, comprehensive analyses and incorporating patient experience is a Herculean task. In many ways this is analogous to “Alice’s Adventures in Wonderland” as so much of what we do grows curiouser and curiouser as each new innovation demands we go through the looking glass and determine what Alice found there.
“There’s no use trying,” said Alice. “One can’t believe impossible things.” “I daresay you haven’t had much practice,” said the Queen. “When I was your age, I always did it for half an hour a day. Why, sometimes I’ve believed as many as six impossible things before breakfast.” — Lewis Carroll
Kenneth S. Serota, DDS, MMSc (kendo@endosolns.com) is an endodontist in Mississauga, Ontario, Canada. He wishes to thank the members of the ROOTS and IMPLANTS forums (ls.rxdentistry.com, www.rxroots.com and www.rximplants.com) for contributions to the material herein.
A complete list of references is available from the publisher.
Over the years, endodontics has diminished itself by enabling the presumption that it is comprised of a narrowly defined service mix; root canal therapy ...
CHARLOTTE, N.C., US: With a heritage of more than 150 years in dentistry, Dentsply Sirona is highlighting trust as a central theme in its endodontic ...
Technologies are producing a paradigm shift in all areas of healthcare. Dentistry has seen significant changes in this context. Alongside new patient ...
How to achieve greater efficiency, safety and job satisfaction in endodontics—endodontist and trainer Dr Sabine Remensberger has been sharing her ...
The Class II restoration remains one of the most common—and technically demanding—procedures in dentistry. Every day, clinicians must deliver durable, ...
BRISBANE, Australia: From 15 to 17 August, dental professionals from all around the world came together for the 21st International Symposium on Dental ...
MILAN, Italy: The annual meeting of the European Association for Osseointegration (EAO) was held in Milan last week, and one of the highlights of the event ...
SEOUL, South Korea: Osstem Implant, a leading company in global implant sales, has announced that it has taken the initiative to help to develop regional ...
Root canal decontamination and adequate sealing play an important role in endodontic success. However, the obturation process represents a challenge to the ...
Modern endodontics is no longer an isolated discipline. It marks the start of a restorative process that extends all the way to the final composite layer. ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





































To post a reply please login or register