EDMONTON, Alberta, Canada/NEW YORK, U.S.: As more and more countries ease their lockdown restrictions, an increasing number of workers are returning to their jobs. A significant proportion of COVID-19 cases are related to occupational exposure. While the risk of infection is fairly high for most workers, it is particularly high for people working in certain occupations. Various analyses have shown that health care workers in general and dental professionals in particular are exposed to a high risk of contracting the virus.
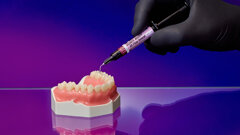
Protection of dental patients and staff during the pandemic is challenging owing to the existence of patients who are infectious and yet asymptomatic. SARS-CoV-2 is most frequently transmitted from human to human through direct contact and respiratory droplets and through indirect contacts with fomites. Therefore, there is a great risk of infection for dentists and dental staff because they have to be in very close proximity to their patients in order to treat them.
Albertan dental workers exposed to highest risk
The Alberta Federation of Labour (AFL) analyzed employment in Alberta using data from the 2016 census of population, cross-referenced with workplace health and safety data from O*NET OnLine, a database that describes various physical aspects of different occupations. The analysis was based on two variables: firstly, the level of physical proximity to the public experienced by workers in their jobs and, secondly, the overall frequency of exposure to contagious diseases and infections at work. The AFL identified the potential risk of SARS-CoV-2 exposure in hundreds of different occupations and created a list of the 100 jobs in Alberta for which the infection risk was the highest.
“The government has an obligation to protect the health of all Albertans; but, as people return to work, the premier and his officials have a particular duty to workers in high-risk jobs”
– Gil McGowan, AFL president
Based on the analysis, the Albertan workers who ranked highest for infection risk were dental hygienists and dental therapists, having an index of 100.0, closely followed by dental assistants (97.5), and dentists and denturists (97.0). The next occupational groups with just a slightly lower risk than dental workers were general practitioners and family physicians (95.5).
In a press release by the AFL, Gil McGowan, president of the association, said: “We’ve flattened the curve, but the virus is still circulating. There’s still no vaccine and no treatment. And the virus is still potentially deadly.”
“The government has an obligation to protect the health of all Albertans; but, as people return to work, the premier and his officials have a particular duty to workers in high-risk jobs. Extra efforts need to be made to protect these workers. If we fail in that regard, a second wave of infection—and another spike in deaths—will be the result. Let’s use this list to help target and strengthen our efforts to stop that from happening,” he continued.
Similar results in US
A chart in an article in the New York Times graphically illustrated the risk levels of different occupational groups in the U.S., based on data from O*NET. Each occupation was represented by a bubble and its position indicated the risk level of contracting SARS-CoV-2. The vertical position of each bubble measured how often workers are exposed to disease and infection; the horizontal position evaluated how close people are to others during their working hours.
Dental hygienists were situated in the very top right corner of the graph and were thus at the highest risk of infection. The score for each of the two categories of frequency of exposure and physical proximity to others was 100. Other occupational groups in dentistry that had nearly the same chance of exposure were oral and maxillofacial surgeons (score of 99 and 99, respectively), dental assistants (96 and 99) and general dentists (95 and 99).
Guidance for dental care and oral health during the pandemic
Researchers from the Eastman Institute for Oral Health at the University of Rochester in the U.S. have published an article in the JDR Clinical and Translational Research on dental care during the SARS-CoV-2 pandemic with the aim of providing guidance on the risk of virus transmission in dental settings, on protection against nosocomial infections and on COVID-19–related oral health research. Topics covered in the paper include transmission from asymptomatic and pre-symptomatic patients, oral health implications of SARS-CoV-2 and COVID-19, and provision of dental care during the pandemic. The ultimate goal is to guarantee dental provision while protecting patients and staff.
“The COVID-19 pandemic has exposed significant gaps in the collective response of global healthcare systems to a public health emergency,” said JDR Clinical and Translational Research Editor-in-Chief Prof. Jocelyne Feine in a press release of the International Association for Dental Research. “Though dentistry is a relatively small part in the COVID-19 response, dental professionals and organizations should take this opportunity to assess the role of dental care professionals in a global public health emergency.”
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East































Can you please provide any data that identifies covid incidence rates for dental professionals? I can not find any reports for the US or my state of North Carolina.
I am a dental hygienist.
Do you have data on covid incidence rate in dental professions? How was risk assessment evaluated? I am a dentist and I can’t find information about incidence.
Dear Leslie,
thank you for your comment. We are aware that the situation is critical for all dental health care workers and this is why we used “dental professionals” in the introduction instead of “dentists”. Also, dental assistants are specifically mentioned in the Albertan analyses with a a very high index of 97.5 (even more than dentists). Kind regards, Franziska from DTI
When will the dental community recognize and identify the Dental Assistant as a dental professional and a vital DHCP? The dental team that is subjected to the dangers are not only the dentist and hygienist. Please identify all DHCP.