The patient reported on in this article was referred to my dental office by his general dental practitioner. There was a large cavity and symptoms of irreversible pulpitis in tooth #26. The 38-year-old male patient had reported to his general dental practitioner with the complaint of toothache in the left upper jaw. The maxillary left first molar was diagnosed as the cause of his complaint. The cavity had been partially prepared, and the mesial wall temporarily restored.
The patient had an interesting history of the area extending from tooth #24 to tooth #26. Tooth #24 had been extracted many years before owing to vertical root fracture. About four years before, a titanium implant replaced it, but there was no osseointegration and the implant was removed. The patient decided on a partial metal–ceramic bridge for several years before attempting another implantation.
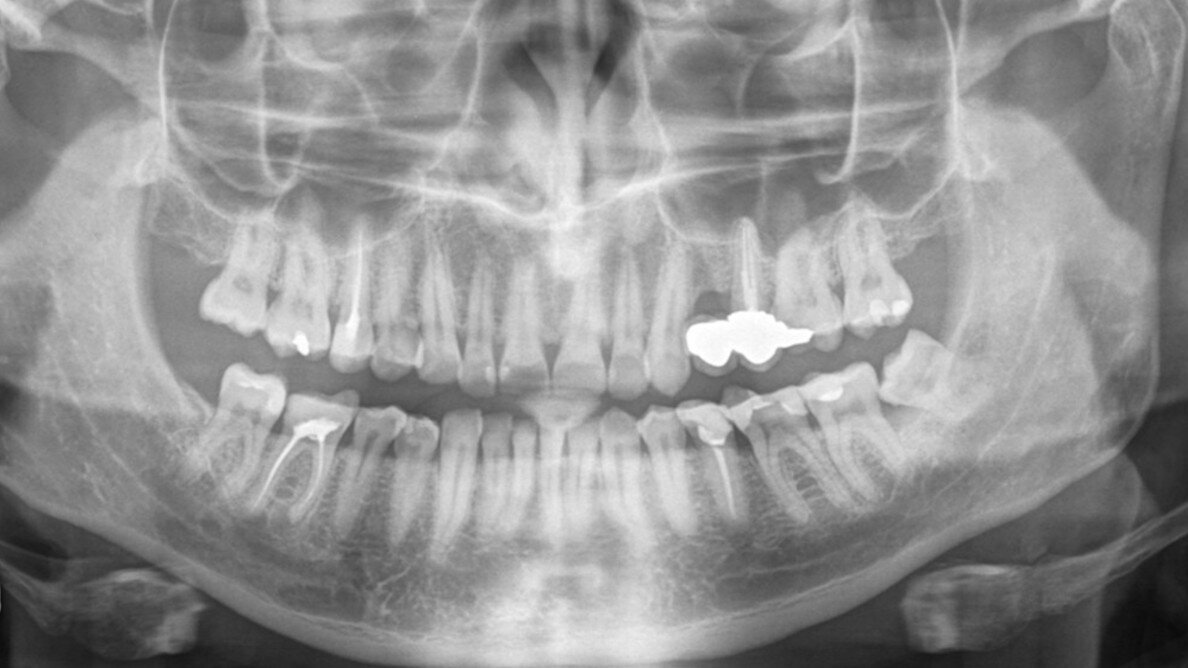
On examination, it was noticed that tooth #26 was tender to cold and sweet. A panoramic radiograph revealed the presence of dental caries penetrating to the pulp chamber (Fig. 1).
Fig. 1: Panoramic radiograph.
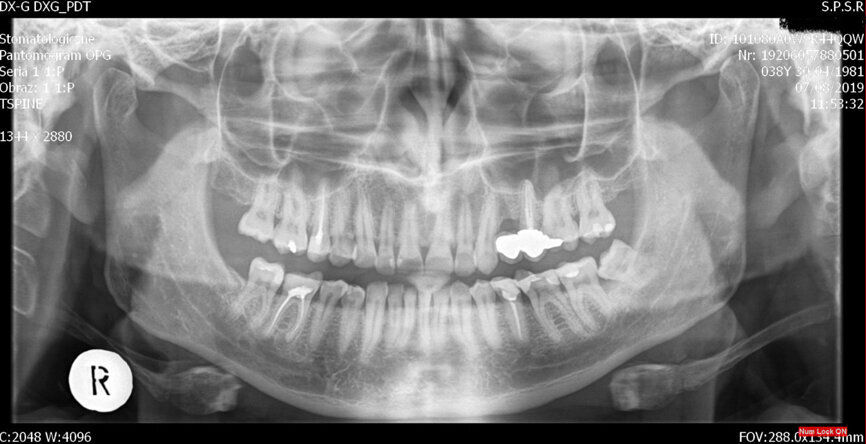
Fig. 2: Initial radiograph.
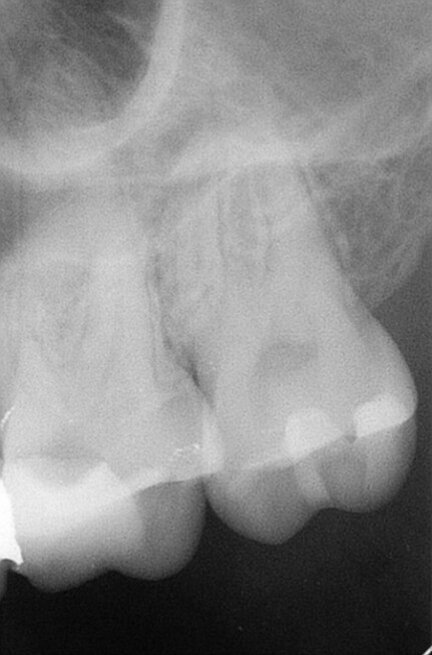
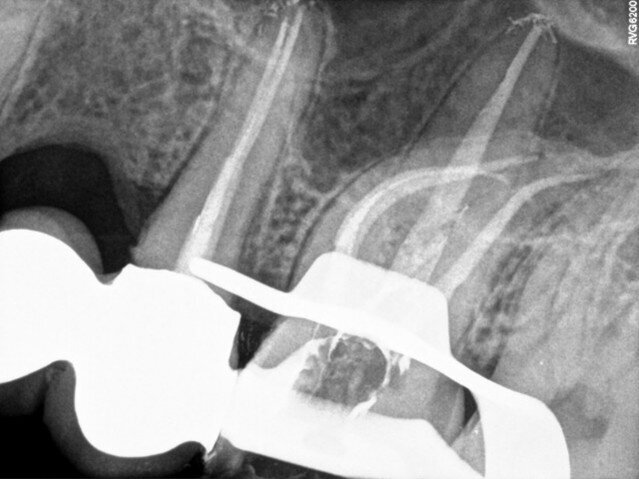
Fig. 3: Post-op radiograph.
I decided on single-visit endodontic treatment. The treatment began with administration of local anaesthetic and dental dam isolation. Crown access was performed with a diamond bur and ultrasonic tip (CAVI 2-D, VDW), which was also used to perform the removal of the coronal portion of the pulp and canal localisation. On access, four canals were identified by inspection with an endodontic probe. The working length of the palatal canal was 21.5 mm (C-PILOT, ISO size 10, VDW), of the mesiobuccal and distobuccal canal was 21.0 mm (C-PILOT, ISO size 10), and of the second mesiobuccal canal was 20.0 mm (C-PILOT, ISO size 8). An electronic apex locator was used for working length confirmation. As can be seen in the panoramic radiograph and dental radiograph (Fig. 2), the canals were quite narrow and curved, so I decided to use rotary files (VDW.ROTATE, VDW).
To achieve a successful treatment, all canals have to be cleaned and shaped to the working length. In this case, it was very important to respect the natural curvature of the canals. For this reason, a single-length technique was performed. VDW.ROTATE files were used in the following sequences: 15/.04, 20/.05 and 25/.06 for the mesiobuccal and distobuccal canal; and 30/.04, 35/.04 and 40/.04 for the palatal canal. To prevent canal transportation in the second mesiobuccal canal, the master apical file was 25/.04. A dental operating microscope (Leica M320, Leica Microsystems) was a helpful tool during endodontic treatment.
Copious irrigation with 5% sodium hypochlorite was performed during the shaping and cleaning procedures. Copious irrigation with 5% sodium hypochlorite was performed during the shaping and cleaning procedures. An ultra sonic tip (Endo Chuck, EMS) and sonic powered irrigation tip (EDDY, VDW) were used to activate the irrigants. At the end, the canals were irrigated with 17% EDTA, and this solution was kept in the canals for 2 minutes. The canals were dried with paper points. An epoxy-amine root canal sealer and a master gutta-percha cone were placed in the canals and the canals were obturated using the continuous wave obturation technique. Glass ionomer cement was used as a temporary filling material (Fig. 3). The patient was referred for final restoration to his general dental practitioner.
Editorial note: This article was published in roots—international magazine of endodontics No. 01/2021.
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East





























To post a reply please login or register