The aim of this article is to highlight the possibility of the successful outcome of non-surgical retreatment involving disassembly of a cast restoration then orthograde MTA obturation, following failed surgical retreatment of a maxillary central incisor.
Introduction
Several studies have documented that bacterial infection of the root canal is the primary cause of apical periodontitis;[1–4] therefore, eradication of micro-organisms from the infected tooth is essential for healing.[5–7] Schilder outlined the principles of 3-D cleaning, shaping and obturation of the root-canal system, which are the foundations for predictable endodontic success.[8, 9] Some of the reasons for failure of primary endodontic therapy are persistent intra-radicular infection owing to incomplete debridement and obturation of the root-canal system, which can occur as a result of missed anatomy,[10] ledges, blockage,[11] canal transportation,[12] fractured instruments,[13] strip perforation[14] and damage to the apical foramen.[15] Other causes of apical periodontitis following root-canal therapy are a lack of coronal seal, secondary caries, vertical root fractures and coronal cracks, trauma, and periodontal disease, which can allow the ingress of bacteria into the root-canal system.[16] Other extra-radicular causes of periapical infection include cellulose-containing materials from paper points or cotton pellets, which are known to cause a chronic inflammatory reaction if present in the periapical tissue,[17] periapical actinomycosis,[18] an unresolved cystic lesion[19] or the accumulation of cholesterol crystals in the periapical area.[20]
The treatment modalities for teeth that have symptoms of apical periodontitis after endodontic treatment are endodontic surgery or non-surgical retreatment if the tooth is to be saved. Non-surgical retreatment is an attempt to remove the micro-organisms from within the canal system and isolate micro-organisms from extra-radicular areas, whereas endodontic surgery is an attempt to confine the micro-organisms within the root-canal system and remove micro-organisms from the extra-radicular areas.[21] Endodontic surgery shows a more favourable initial success but non-surgical retreatment shows a better long-term success.[22] Extraction of teeth with failed root-canal treatment and replacement with implants has increasingly become more popular than surgical and non-surgical endodontic retreatment.[23, 24] Technological advances, such as the use of magnification and ultrasonics, and the development of new materials promise greater efficiency and improved treatment outcomes. The decision of whether to extract or retain a tooth should be based on its suitability for further restoration after retreatment, as long as it is periodontally sound.[16, 25] It is important that in patients with high aesthetic expectations and a thin mucosal biotype that greater efforts be made to save a questionable anterior tooth in order to ensure preservation of the soft-tissue architecture.[26, 27]
In non-surgical retreatment, the presence of cast restorations and posts may pose technical difficulty in accessing the root-canal space. Cast and prefabricated metal posts can be removed with ultrasonics and post-pulling devices; fibre posts can be drilled out.[28] The simplest means of removing a screw post is to use the corresponding wrench—if the head of the post has been damaged, a piece of cotton wool can be placed in the wrench to provide a tighter fit.[28] Ultrasonic vibration applied to posts reduces the force needed to remove the post. It is important to use a water spray to prevent overheating the tooth during ultrasonic vibration of the post. The risk of root fracture during post removal has been reported to be less than 1%.[29] Traditionally, teeth with failed apicoectomies without retrograde fillings were retreated surgically or a combination of non-surgical and surgical procedures was employed.[30] Retreatment of teeth with previously apically resected roots was first reported by Stewart in 1975.[31] In these cases, the existing root filling should be removed carefully in order to avoid extruding the filling into the periapical area when a retrograde filling is absent. Pannkuk [32] demonstrated a method for removal of amalgam root-end fillings during retreatment. Once the previous filling material has been removed, further treatment proceeds as in the treatment of immature teeth with open apices. MTA has been proposed as the material of choice for apical barrier formation in teeth with open apices and necrotic pulps.[33] It is biocompatible, osteoinductive, cementogenic and has antifungal and antibacterial properties.[34]
embedImagecenter("Imagecenter_1_756",756, "large");
Case report
A 61-year-old female patient was referred for treatment of a symptomatic maxillary right incisor. Her chief complaint was that she had had an apicoectomy done by a maxillofacial surgeon on her anterior tooth (#11) one year previously and three months after the procedure she kept getting a swelling in the gum above the tooth and recently the swelling had become painful and the tooth was painful when biting. She had seen her dentist two days previously and he had prescribed clindamycin 150 mg. Her other concern was the dark cervical margin exposed above her crown on the tooth owing to the receding gum line.
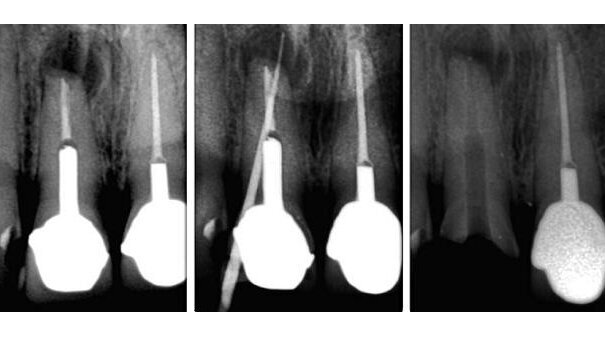
On clinical examination, the gingiva above tooth #11 was inflamed and a draining sinus was noted in the gingiva 10 mm above the cervical margin of the incisor. There was recession of the gingiva above the cervical margin of the crown of tooth #11 and a PFM crown on tooth #21 (Fig. 1). Thermal tests were negative. Tooth #11 was tender to percussion and palpation. Periodontal probing showed 2 mm pockets around teeth #11, 12 and 21. No pathological mobility of tooth #11 was detected. Radiographic examination demonstrated that there was a post crown on tooth #11, periapical radiolucency and no retrograde filling placed at the apex (Fig. 2). The crown–root ratio was approximately 50:50. The draining sinus was at the apical level of the post, and a root fracture was suspected. A gutta-percha point was inserted into the draining sinus and a periapical radiograph showed the gutta-percha point tracking the sinus to the periapical radiolucency (Fig. 3).
Treatment options were discussed with the patient. The following options were suggested: non-surgical retreatment, surgical retreatment, extraction followed by implant placement, denture or bridge. She was motivated to keep her tooth, refused another apicoectomy procedure and could not afford an implant and bone augmentation and the possible replacement of the neighbouring crown because of gingival recession following extraction. A decision was made to attempt non-surgical retreatment and the patient was warned that there was a possibility of fracture.
The patient was scheduled for a two-hour appointment. Following anaesthesia, a polyvinyl siloxane impression (PRESIDENT, Coltène/Whaledent) was taken of the maxillary arch. The crown was sectioned off using a tapered crown preparation diamond bur (Komet) and a tungsten carbide bur (Tri Hawk). A minimum 2 mm ferrule was observed around the cast post core. A rubber dam was placed and secured with wedges placed between teeth #12 and 13, and between #21 and 22.
Post-core removal was initiated using the Start-X #4 ultrasonic tip (DENTSPLY Maillefer) in a piezoelectric scaler handpiece (NSK), moving the tip anti-clockwise along the longitudinal axis of the post core. The Start-X tip has a lumen for water spray, which prevents overheating of the post and surrounding periodontal ligament. After 15 minutes of ultrasonic vibration, the post core had not completely loosened. A hole was drilled through the core bucco-palatally using a Great White #2 tungsten carbide bur (SS White). A double-layered dental floss ligature (Satin Tape, Oral-B) was looped into the hole in the core. The cable attachment of the Safe Relax automatic crown and bridge remover (Anthogyr) was looped through the dental floss ligature. The purpose of this is that the dental floss ligature acts as a stress breaker, thereby preventing excessive force on the root and minimising the risk of root fracture or inadvertent extraction of the tooth. The post core was removed without any damage to the root following 30 seconds of low intensity force application with the Safe Relax. The Safe Relax was used because the post was not serrated .
The residual cement in the canal was removed with a #3 Start-X ultrasonic tip (DENTSPLY Maillefer). The gutta-percha was removed using a few drops of chloroform (Allied Drug Company) and a #40 Hedstrom file (DENTSPLY Maillefer). A radiograph was taken to confirm removal of the gutta-percha (Fig. 4). Working length was determined using the iPex digital apex locator (NSK) and the apex was gauged to a size #100 using a K-file (DENTSPLY Maillefer).
The canal was irrigated with 3% sodium hypochlorite (Vista Dental) and agitated with the EndoActivator (DENTSPLY Tulsa) for one minute and this was repeated ten times with fresh irrigant each time. The canal was dried with paper points and then flooded with 17% EDTA and agitated with the EndoActivator for one minute and then dried and rinsed with distilled water. A 2% chlorhexidine solution was left to soak in the canal while the post core was being prepared for temporary recementation.
The post core was air abraded using the RONDOflex (KaVo) with 27 µ aluminium oxide powder. The post core was then soaked in 2% chlorhexidine (Vista Dental) for two minutes. The hole in the core was etched with 37% phosphoric acid (Ultradent), rinsed and air-dried. Then Monobond Plus primer (Ivoclar Vivadent) was applied to the surface and air-dried after 60 seconds. The Xeno V (DENTSPLY) bonding agent was applied to the core and light cured for 20 seconds using the SmartLite (DENTSPLY) ultraviolet curing light. The QuiXfil (DENTSPLY) resin composite was used to fill the hole in the core and light cured for ten seconds.
The buccal margin of the crown preparation was extended to the gingival margin using a #018 tapered diamond bur (Komet). The canal was air-dried and UltraCal XS (Ultradent), a radiopaque calcium hydroxide paste, was syringed into the canal using a NaviTip needle (Ultradent). The post core was recemented with NexTemp temporary cement (Premier Dental) and the rubber dam removed. A temporary crown was fabricated by placing Protemp 4 (3M ESPE) in the polyvinyl siloxane impression and reseating it. The temporary crown was polished and cemented using Meron glass ionomer luting cement (VOCO). A post -operative periapical radiograph was taken (Fig. 5). The patient was scheduled to return for evaluation and further treatment after six weeks.
Second visit
The patient reported that her symptoms had disappeared within the first week after the first visit. On clinical examination, it was noted that the inflammation and draining sinus in the gingiva above tooth #11 had healed. A periapical radiograph showed some dissolution of the calcium hydroxide dressing apically (Fig. 6).
Following anaesthesia and isolation, a horizontal slot was cut on the buccal cervical aspect of the temporary crown and it was levered off along with the post core using a flat plastic instrument. The canal was irrigated with 17% EDTA, which was agitated using the EndoActivator for one minute to help remove the remaining calcium hydroxide dressing. Then distilled water was used to flush the canal and 2% chlorhexidine was left in the canal for two minutes. Thereafter, the canal was irrigated with distilled water and dried with paper points. A periapical radiograph was taken to determine the placement of the MTA Gun System (DENTSPLY Maillefer) and confirm removal of residual calcium hydroxide (Fig. 7).
White MTA-Angelus (Angelus) was mixed according to the manufacturer’s instructions and placed into the canal using the MTA carrier gun. After the placement of three aliquots of MTA, a #5 Dr Machtou Plugger (DENTSPLY Maillefer) was used to condense the MTA, with ultrasonic vibration applied to the plugger for 20 seconds to aid in condensing the MTA mass apically. A further three aliquots of MTA were placed and the condensation procedure repeated. The post was used to condense the final two aliquots of MTA. A periapical radiograph was taken to assess the MTA placement (Fig. 8). A post brush (DiaDent) was used to remove excess MTA in the post space, and a cotton pellet soaked in distilled water was placed in the canal for 15 minutes.
The RONDOflex was used to lightly air abrade the post surface to remove the remnant of the temporary cement, and the post was soaked in 2% chlorhexidine for two minutes. The post was then etched with 37% phosphoric acid for 20 seconds, rinsed and air-dried, and then Monobond Plus was applied and air-dried after 30 seconds. After 30 minutes the initial set of the MTA was confirmed by inserting a #60 K-file (DENTSPLY Maillefer) into the canal against the MTA mass. The post space was dried using paper points. The post-core crown was recemented using the RelyX Unicem resin-modified glass ionomer cement (3M ESPE) and a periapical radiograph was taken (Fig. 9).
The preparation of the permanent crown was postponed to monitor healing and symptoms, to assess the gingival response to the new crown margin and to spread the cost. A five-month post-operative radiograph (Fig. 10) showed some dissolution of the extruded MTA, and the tooth was asymptomatic and the gingiva above tooth #11 showed no further recession (Fig. 11). An 18-month follow-up radiograph showed a decrease in periapical radiolucency (Fig. 12a) and the patient was happy with the new crown (Fig. 12b).
Discussion
It is important to discuss treatment alternatives, risk factors and costs with patients before proceeding with treatment.[21] The approach to cleaning and shaping in teeth with open apices requires an adaption of strategies and the biological objectives described by Schilder [9] take precedence. Particular attention should be given to working length control to reduce the possibility of extrusion of irrigants. Subsonic agitation was used for the irrigants to minimise extrusion35 and improve the efficacy of chemical debridement.[36] The combined use of EDTA and sodium hypochlorite has been shown to have better antibacterial efficacy than sodium hypochlorite alone.[37] Chlorhexidine exhibits substantivity and dentine medicated with a 2% solution for ten minutes can exhibit substantivity for up to 12 weeks. Furthermore, chlorhexidine is antifungal, which is beneficial because fungi may be involved in cases with persistent or secondary endodontic infection.[38] Premedication with calcium hydroxide improves the marginal adaptation of the apical MTA plug [39] and it appears to be the only medicament that is effective against endotoxin.[40] White MTA-Angelus was used because of its short setting time. (MTA-Angelus is available in both grey and white forms.) It is composed of 80% Portland cement and 20% bismuth oxide. The absence of calcium sulphate allows a quicker initial setting time of approximately 15 minutes.[41] In teeth with open apices, apical control is difficult during obturation, but MTA extrusion is well tolerated.[32]
In the present case, the cast post core was reused because there was no unnecessary mechanical enlargement of the post space, the well-fitting post core was removed largely intact, its reuse minimised the cost to the patient and there was an adequate ferrule around on sound tooth structure.
A second surgery in teeth that have undergone apicoectomy results in further scarring, shortening of the root and decreased localised blood supply.[32] The present case report shows healing in progress and the absence of symptoms 18 months after non-surgical retreatment. Further follow-up is necessary to assess the long-term outcome.
Non-surgical retreatment with an MTA apical barrier after root resection is considered an empirical treatment modality, as no data exists on success rates.[31] This warrants further research of this approach, as it may provide comparable healing and less morbidity compared with conventional retreatment combined with apical surgery.
Editorial note: A complete list of references is available from the publisher.
Acknowledgement: I would like to thank Prof. J. L. Gutmann for his encouragement and help in writing this case report and Dr K. Serota and the roots community.
This article was published in ROOTS international magazine of endodontology No. 3/2012.
LONDON, UK: Despite improvements in treatments, intra-bony defects are associated with progression of periodontal disease and tooth loss unless they are ...
Taking into consideration the active lifestyle of most of our working patients with maxillary odontogenic radicular cysts, such patients require more ...
Treating bone insufficiency is a familiar challenge for all implant practitioners. Such insufficiency can compromise the placement of an implant, its ...
In symptomatic periapical periodontitis, sufficient preparation and disinfection of the root canal is usually the only way to eliminate pain. Particularly ...
As a researcher at the University of Brescia in Italy and the operator of a private practice, Prof. Magda Mensi has a special interest in the non-surgical ...
CHICAGO, US: The American Dental Association (ADA) has issued updated recommendations on dental imaging, reinforcing that radiographs and CBCT scans should ...
In an earlier article on this topic,1 I demonstrated the workability of thermo-viscous composites. After warming, the composite can be easily handled for ...
Dental implants are a fantastic addition to the repertoire of any restorative dentist and allow us to provide a tooth replacement in a way that minimises ...
LONDON, England: The UK’s General Dental Council has emphasised its commitment to understanding and monitoring the evolving impact of artificial ...
The use of 3D printers is rapidly gaining interest across the world. 3D printing is threatening to replace traditional subtractive CAD/CAM methods in ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East
































To post a reply please login or register