Dental implants to replace missing teeth have become an integral part of current conventional dentistry. Accepted protocols now include two-stage delayed loading, one-stage delayed loading, immediate loading in a healed receptor site, tilted implant placement, immediate loading in fresh extraction sites, partial extraction therapy (PET), socket shield technique and root membrane concept.
Technology has provided clinicians with enhanced tools for diagnosis and treatment planning, instrumentation for surgical intervention, improved implant surface treatments and thread design, improved abutment-to-implant connections, sophisticated dental laboratory software and CAD/CAM applications, a greater selection of transitional and definitive restorative materials, static and dynamic navigation, and changes in drill designs and drilling protocols. Dental implant procedures are predictable, effective and essential to address the needs of patients.
Partial extraction procedures in their various formulations have been demonstrated to be proven methodologies for preserving bone and soft-tissue volume.1–7 Our 2017 article reviewed 3D diagnostic tools for planning and executing root membrane and PET procedures based on the “Triangle of Bone” concept and specific instrumentation to achieve successful outcomes.5
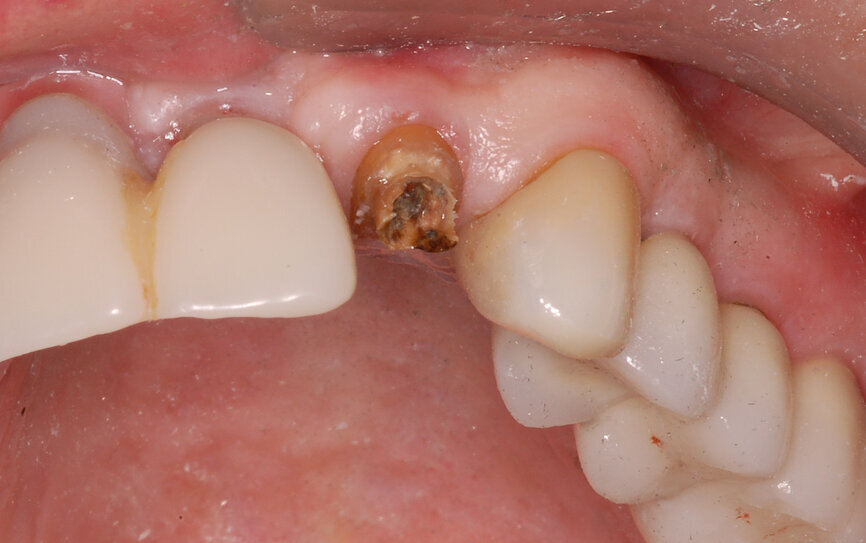
Fig. 1: The patient presented with a horizontally fractured clinical crown, an indication for a partial extraction therapy procedure.
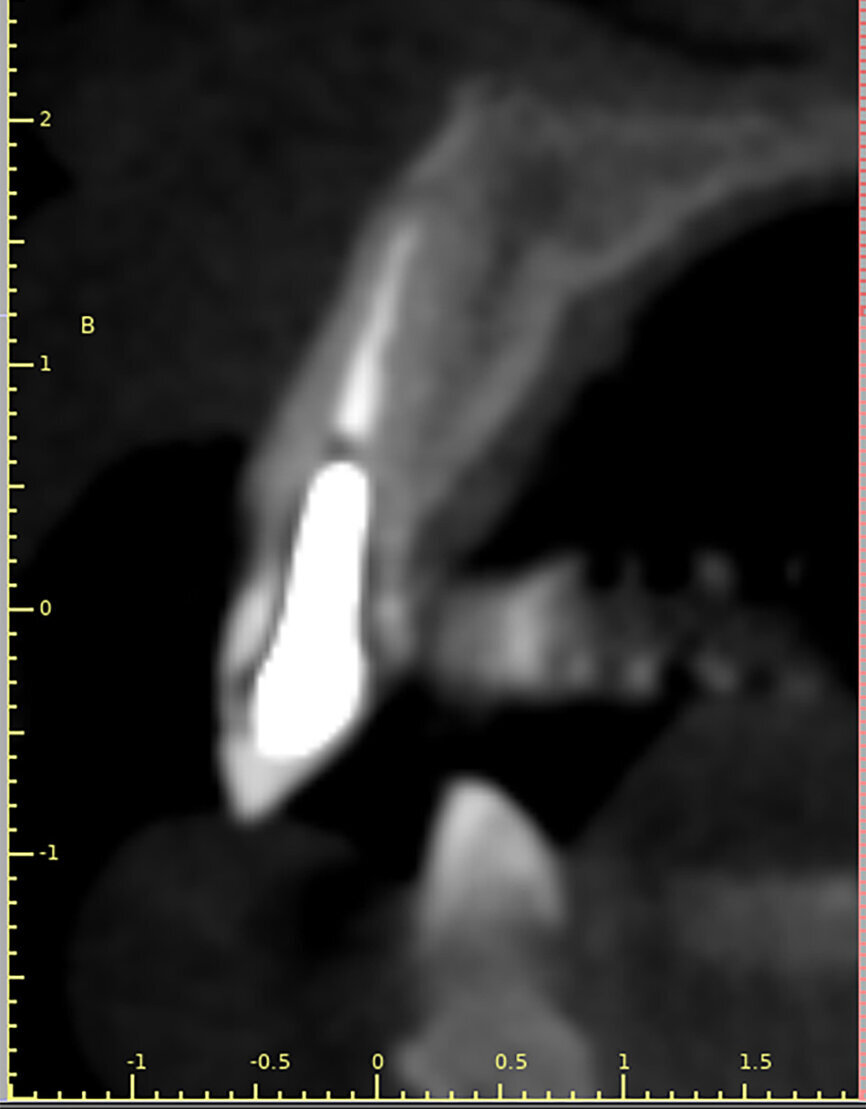
Fig. 2: The trajectory of the root
in relation to the alveolus can be visualised with a cross-sectional image.
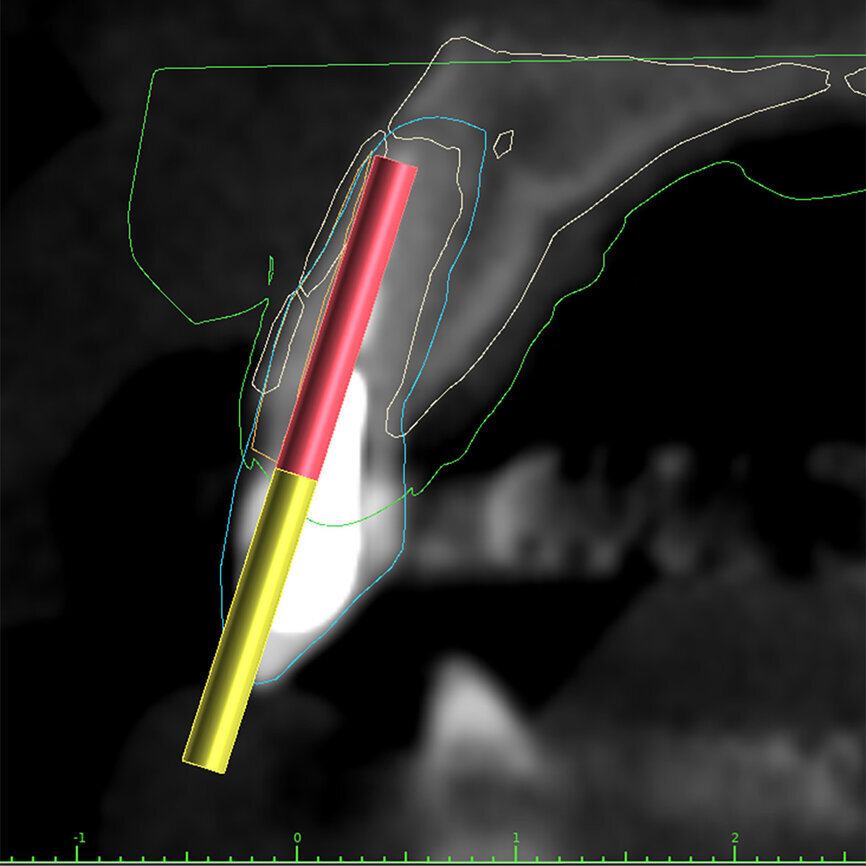
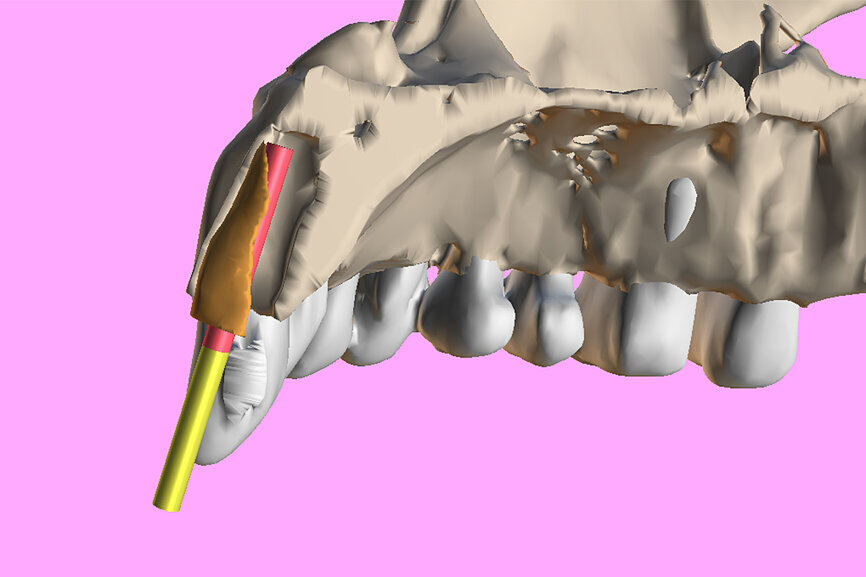
Fig. 3a: Planning the initial drill path using a custom implant design (red) to match the
diameter of the initial drill to reach the tooth apex. The abutment projection is shown in yellow.
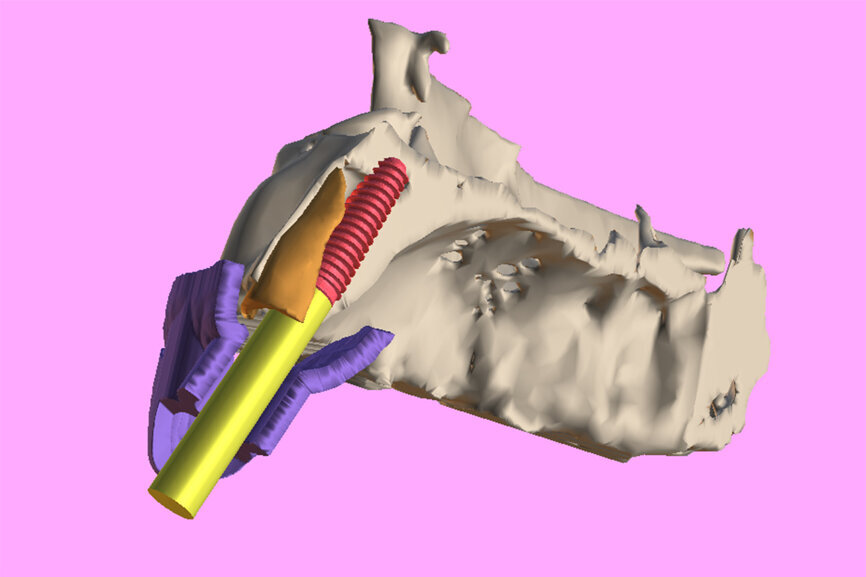
3b: The simulated implant within the Triangle of Bone (red), placed to avoid the root fragment seen in yellow (white arrows).
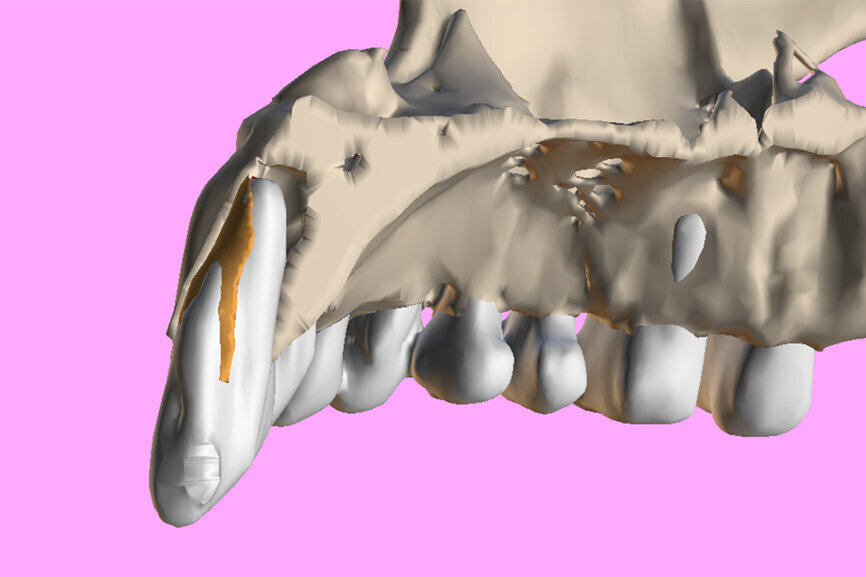
Fig. 4: The segmented root (white) and the root fragment (brown) within the sectioned maxillary surface model.
Fig. 5a: Virtual sectioning of the segmented root using Meshmixer with a simulated custom implant to reach the root apex.
Fig. 5b: The apical portion of the simulated AnyRidge implant can then be positioned so as not to touch the root fragment while engaging in host bone for stability.
Fig. 6a: Two 3D-printed templates designed on the digitised model (green): one for the initial drill to section the tooth at the root apex (a) and the second for using sequential guided drills to drill through the root itself (b).
Fig. 6b: Two 3D-printed templates designed on the digitised model (green): one for the initial drill to section the tooth at the root apex (a) and the second for using sequential guided drills to drill through the root itself (b).
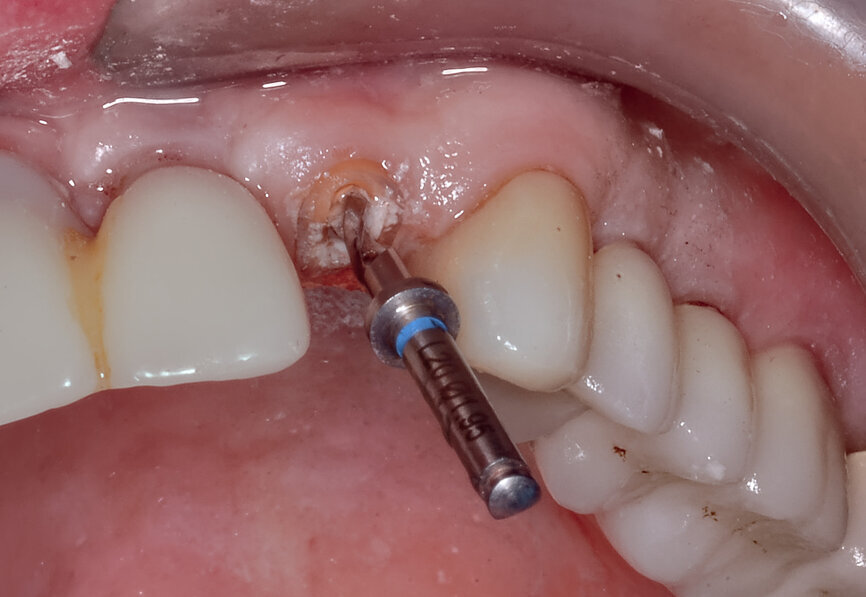
Fig. 7a: A sleeveless guide to accommodate a 2 mm long pilot drill that was used to reach the root apex.
Fig. 7b: Removing the guide allowed for inspection of the drill embedded within the tooth.
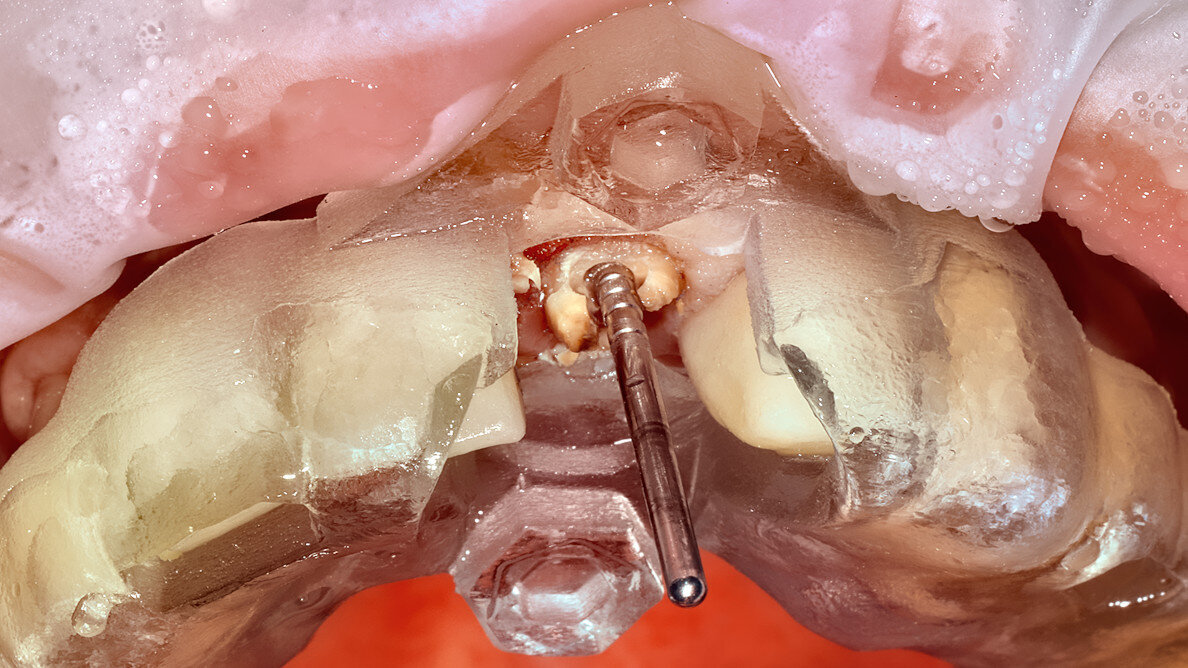
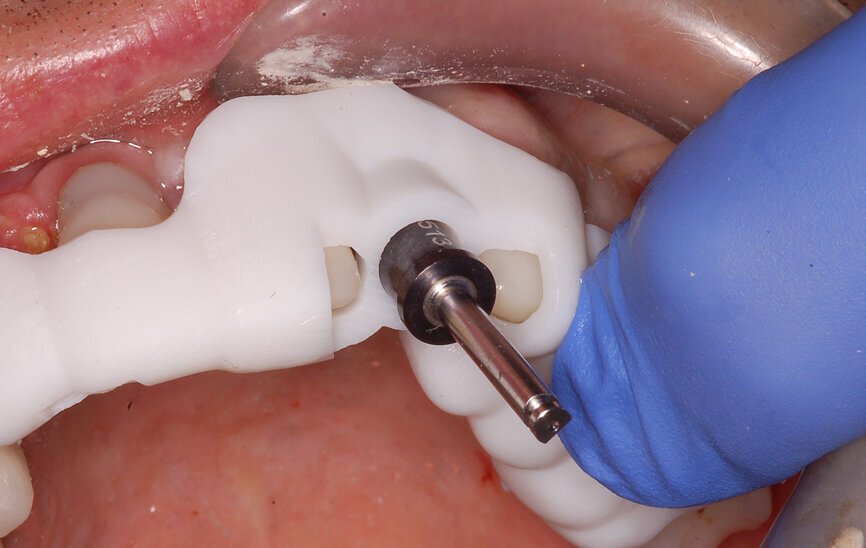
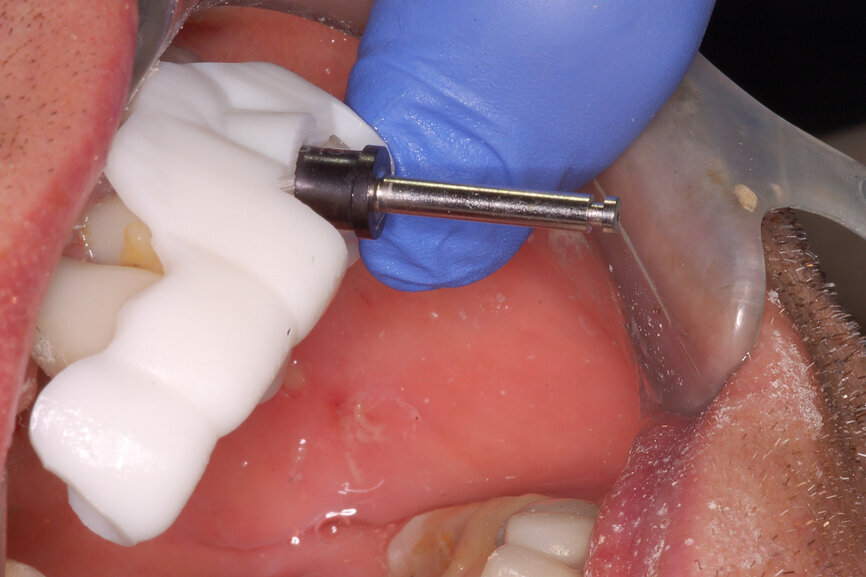
Fig. 8a: Using drill guides with long shanks to engage the sleeveless template allowed for sequential and accurate drilling of the tooth and subsequent bone for implant placement.
Fig. 8b: Using drill guides with long shanks to engage the sleeveless template allowed for sequential and accurate drilling of the tooth and subsequent bone for implant placement.
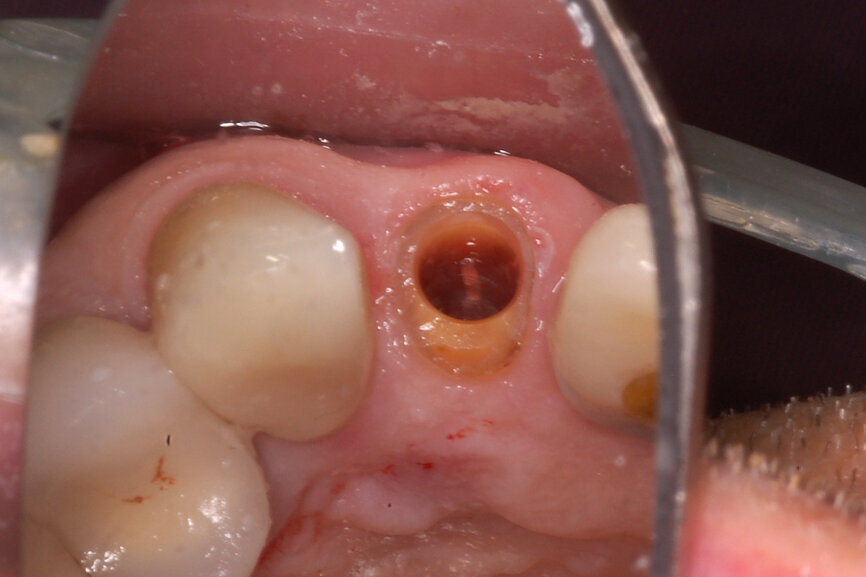
Fig. 9: The cylindrical tooth preparation resulted in the desired crescent shape of the root fragment to provide adequate space for the implant.
Fig. 10: The
implant was placed into the osteotomy through the template using a special manufacturer-specific carrier.
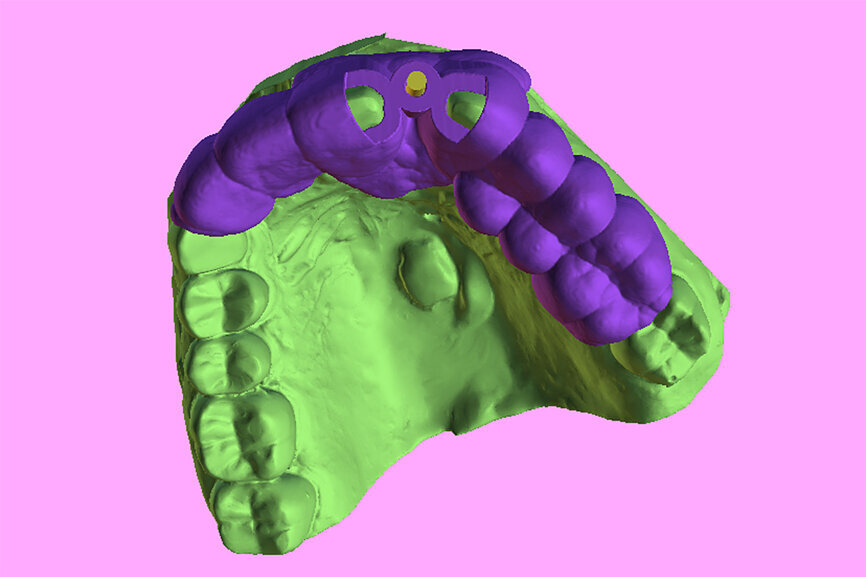
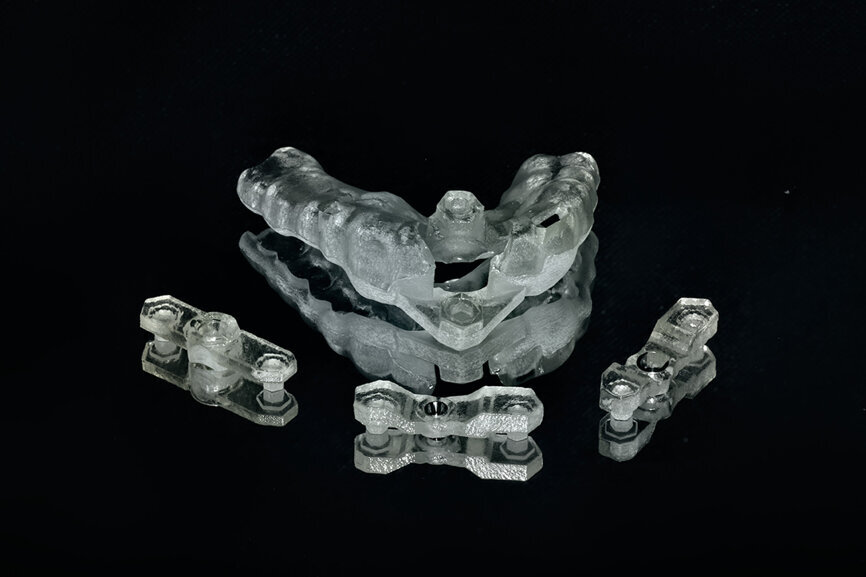
Fig. 11: The stackable tooth-borne guide and the three other separate components.
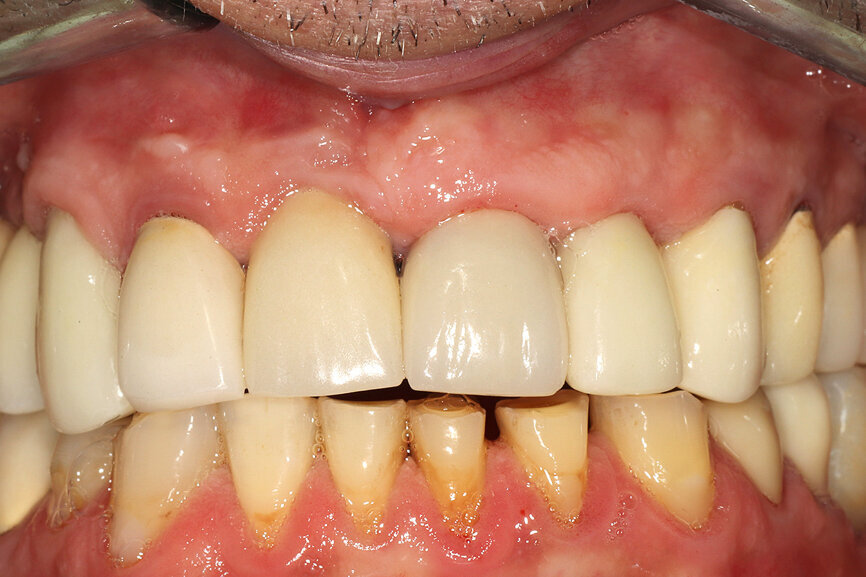
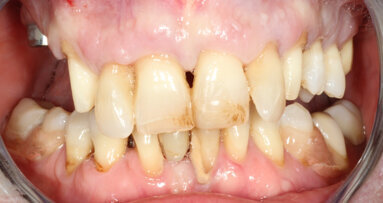
Fig. 12a: A post fracture presenting in the left central incisor, requiring extraction.
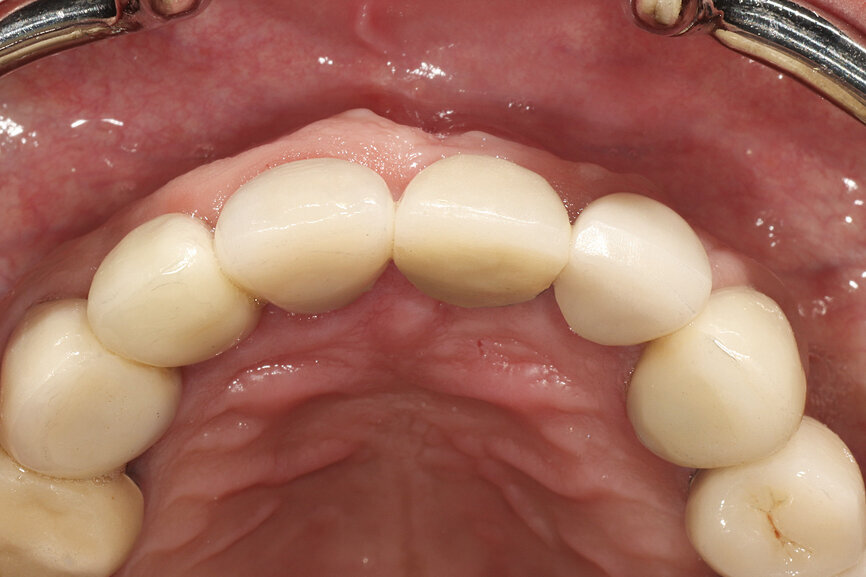
Fig. 12b: The occlusal view illustrated the cervical tissue volume and contours.
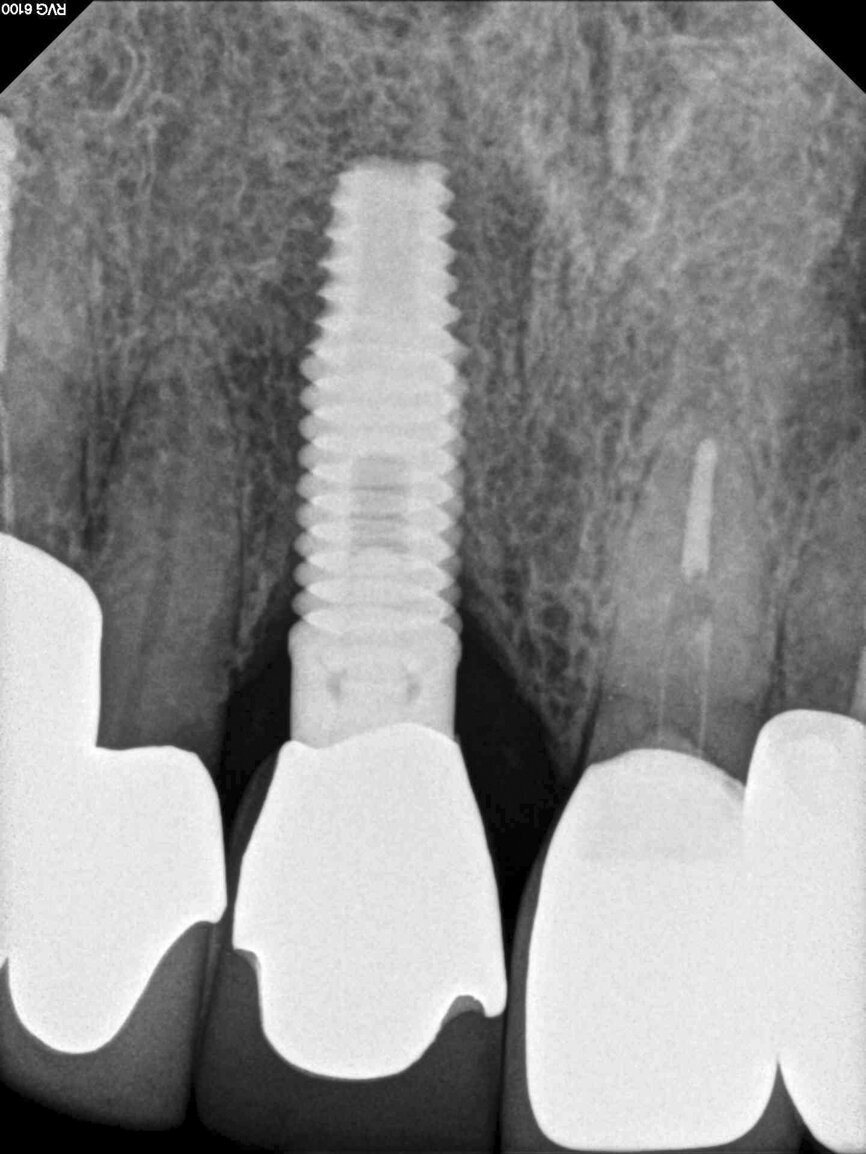
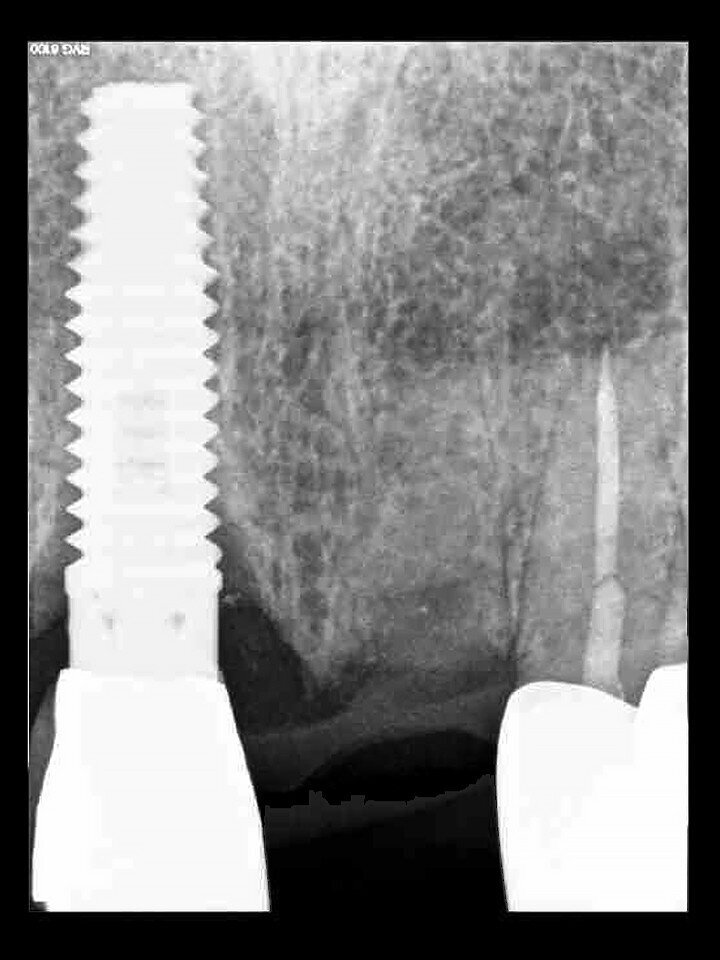
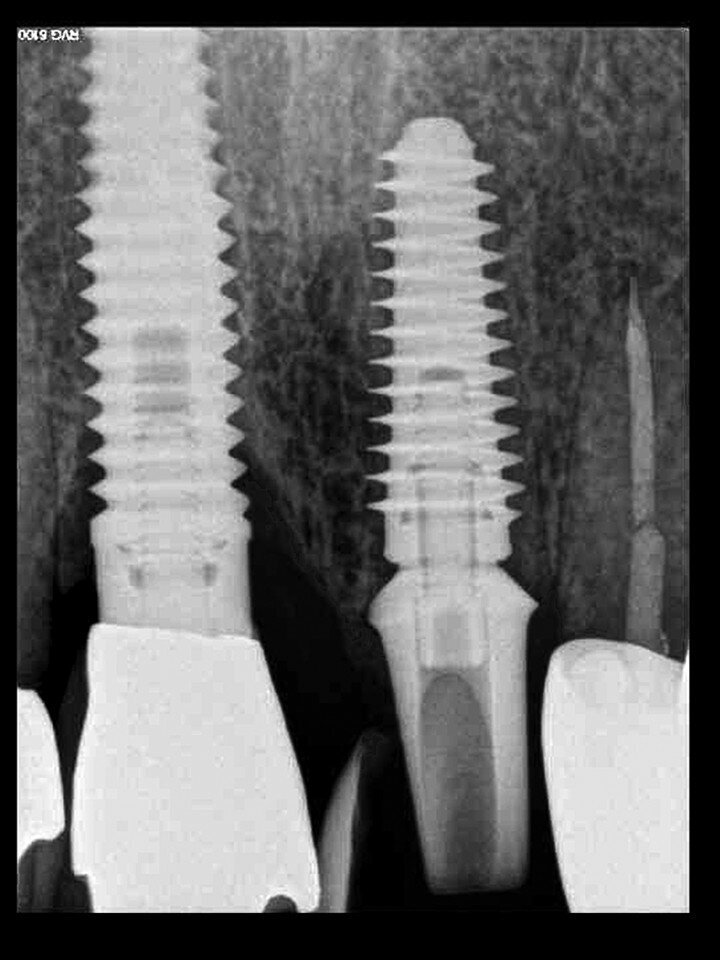
Fig. 13: The pre-op periapical radiograph revealed an existing implant-supported metal–ceramic restoration for the adjacent region #11.
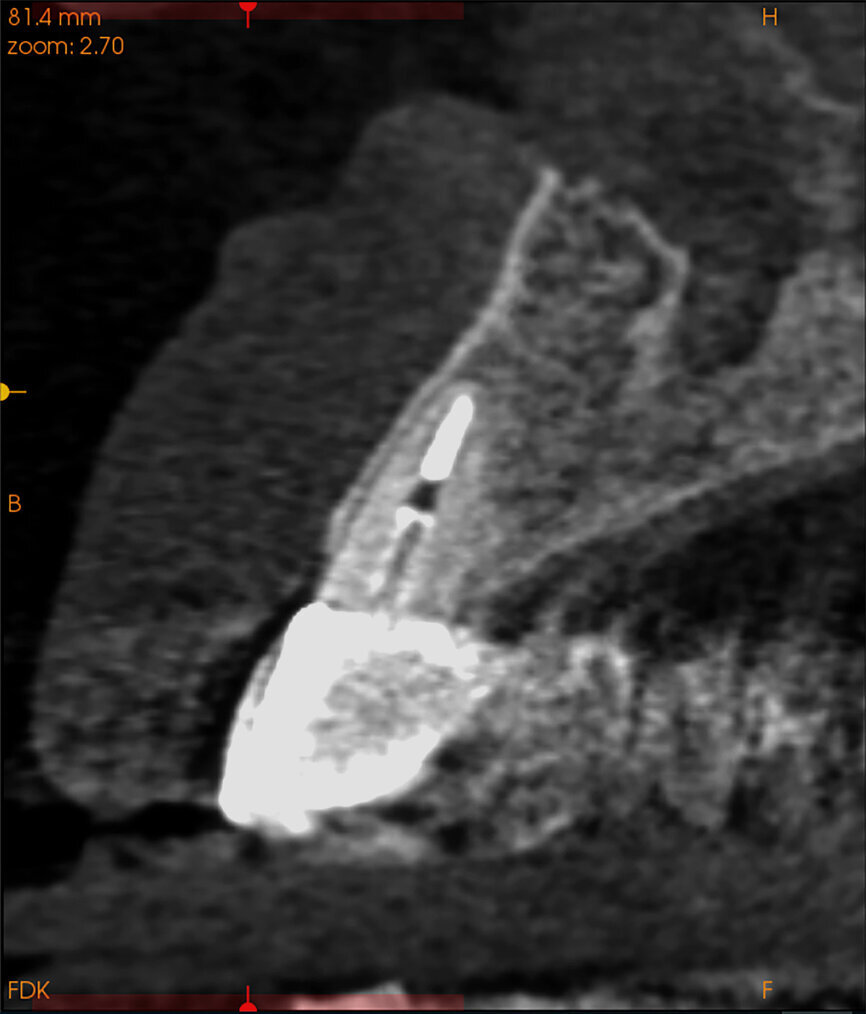
Fig. 14a:
The CBCT cross-sectional image revealed a favourable pre-op condition for a PET procedure.
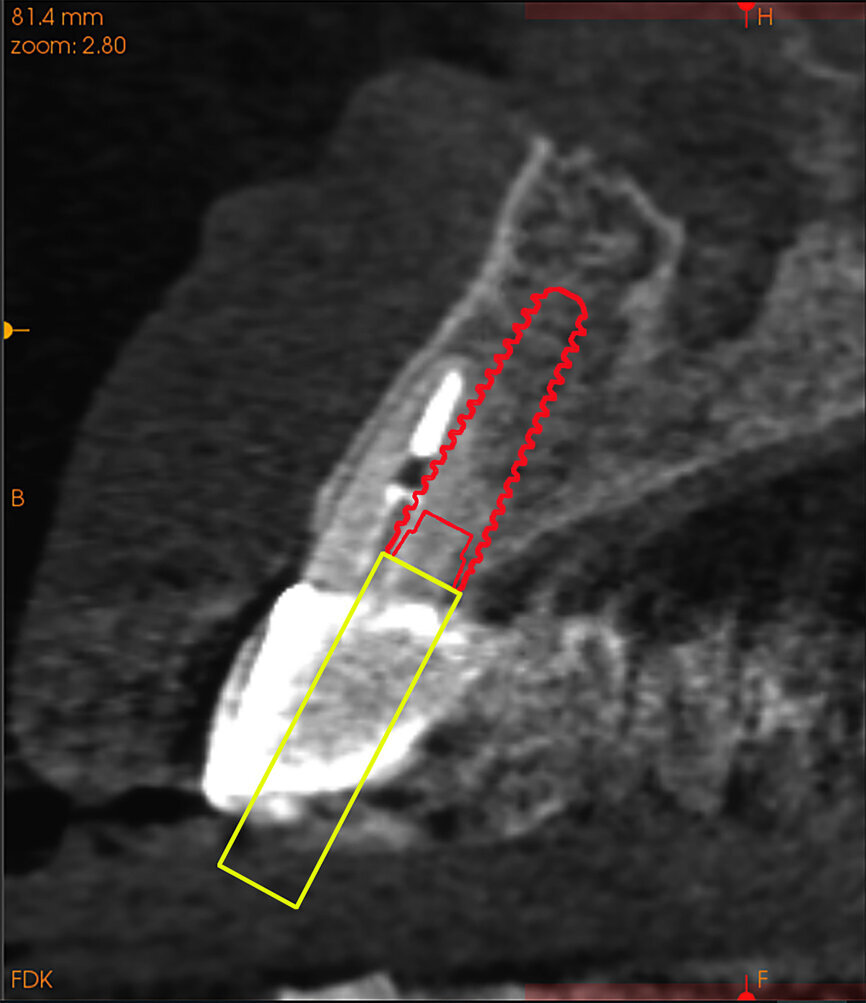
Fig. 14b: Using the native Carestream 3D Imaging Software,
a simulated implant (red outline) and abutment projection (yellow outline) was positioned within the available bone to avoid the root fragment.
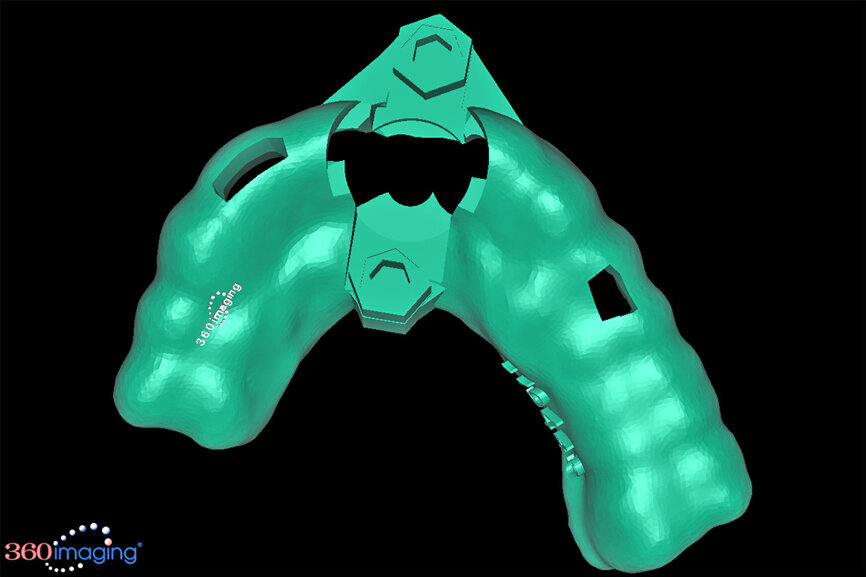
Fig. 15a: The base template was designed to seat firmly on the adjacent teeth, incorporating buccal and lingual hexagonal offsets to engage the different drill
guide inserts.
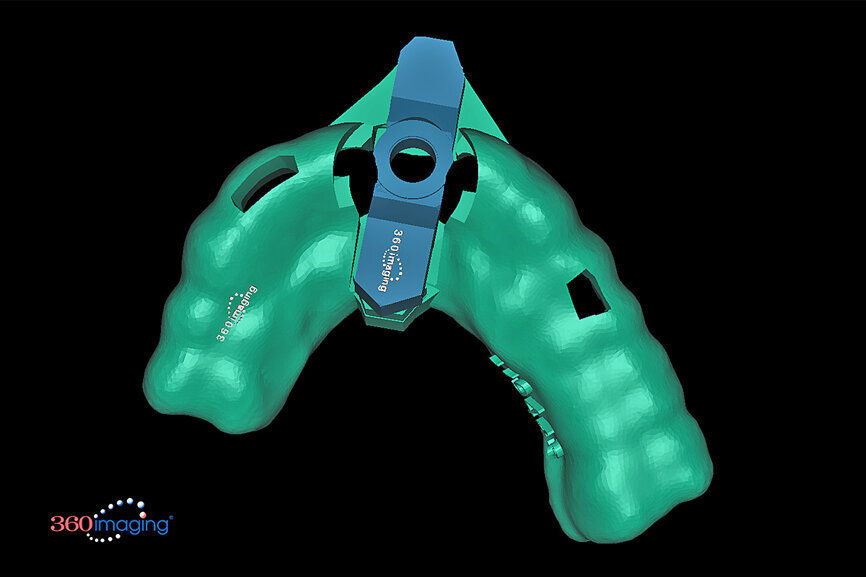
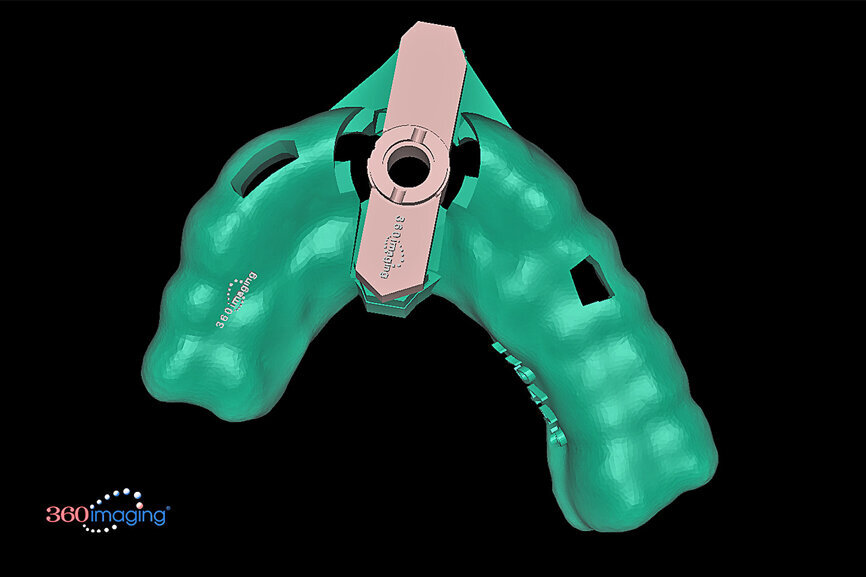
Fig. 15b: Separate inserts were fabricated for the initial drill guide to reach the root apex to accommodate sectioning, followed by a second guide for final osteotomy drilling and implant placement.
Fig. 15c: Separate inserts were fabricated for the initial drill guide to reach the root apex to accommodate sectioning, followed by a second guide for final osteotomy drilling and implant placement.
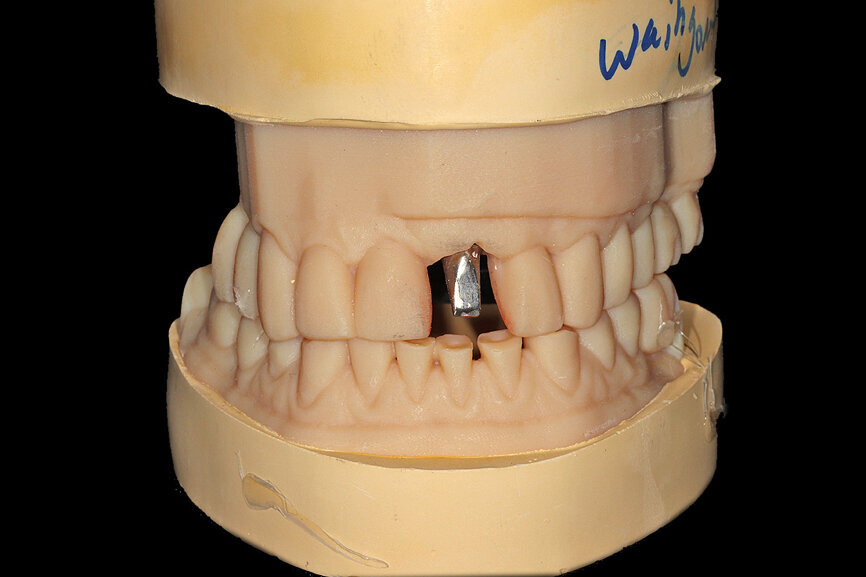
Fig. 16a: The accuracy of the implant and template design allows for true restoratively driven planning combined with CAD/CAM applications for the design
and fabrication of a patient-specific abutment and transitional restoration.
Fig. 16b: The accuracy of the implant and template design allows for true restoratively driven planning combined with CAD/CAM applications for the design
and fabrication of a patient-specific abutment and transitional restoration.
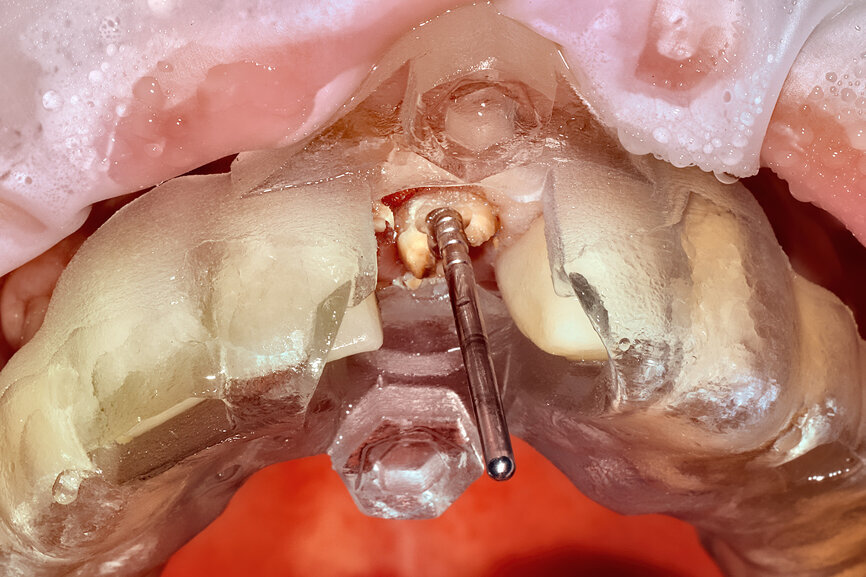
Fig. 17a: Utilising the tooth-borne template and the first insert, initial long shaper drills were used to reach the apex of the root.
Fig. 17b: Utilising the tooth-borne template and the first insert, initial long shaper drills were used to reach the apex of the root.
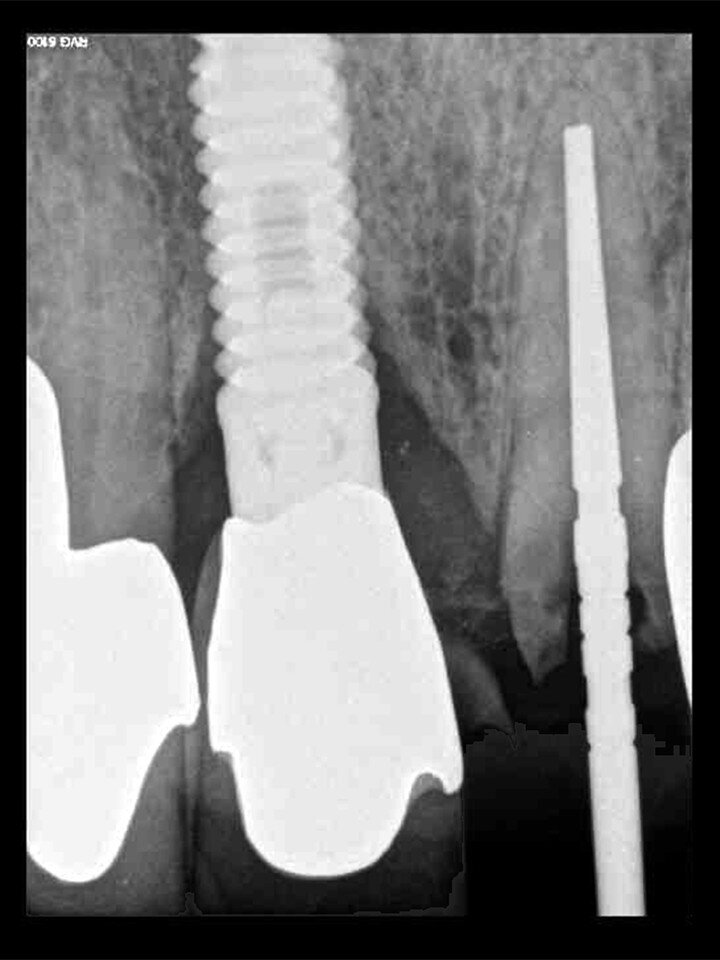
Fig. 18: A periapical radiograph
with a drill in place confirmed that the apex length had been reached and that all the gutta-percha had been removed.
Fig. 19a: The second metal cylinder insert
allowed for the long, round diamond drills to shape the root into the desired crescent shape (a). The insert was removed to access the palatal root (b).
Fig. 19b: The second metal cylinder insert
allowed for the long, round diamond drills to shape the root into the desired crescent shape (a). The insert was removed to access the palatal root (b).
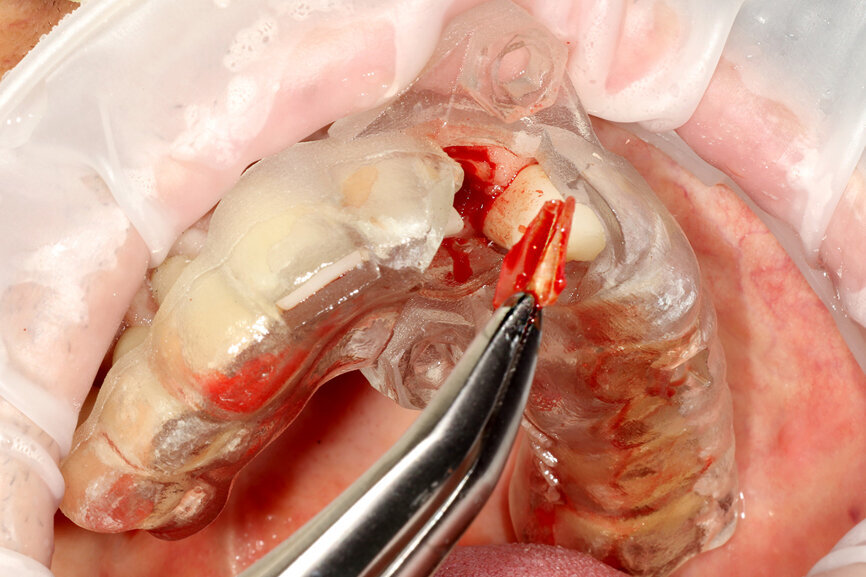
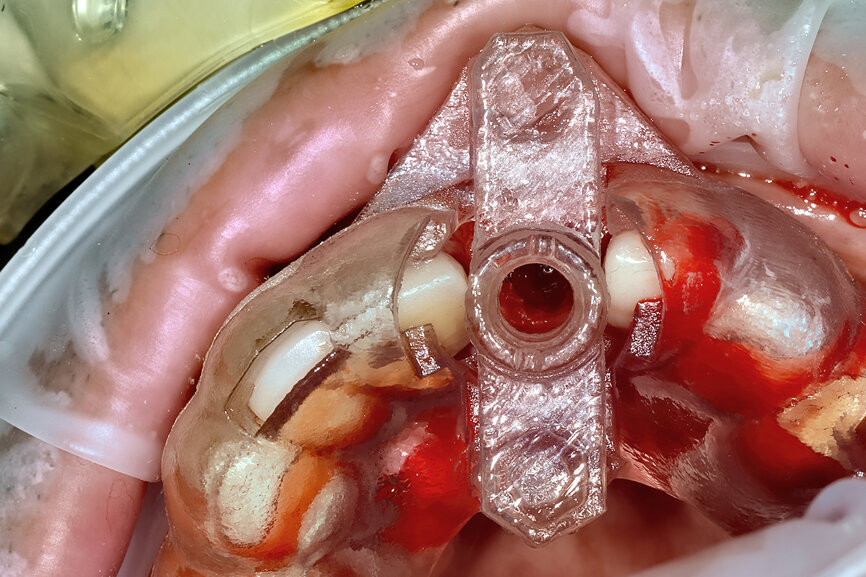
Fig. 20: The sectioned palatal root was carefully removed.
Fig. 21: A periapical radiograph confirmed that the palatal root and all the gutta-percha had been completely removed.
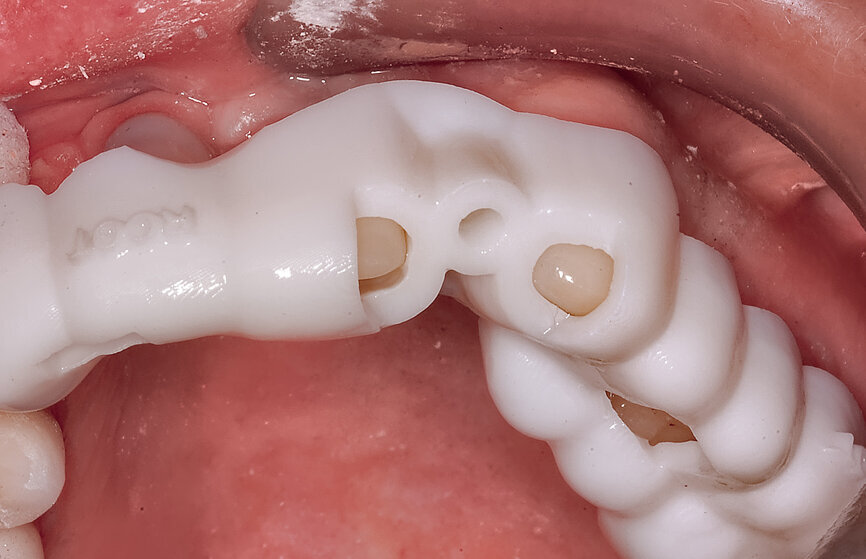
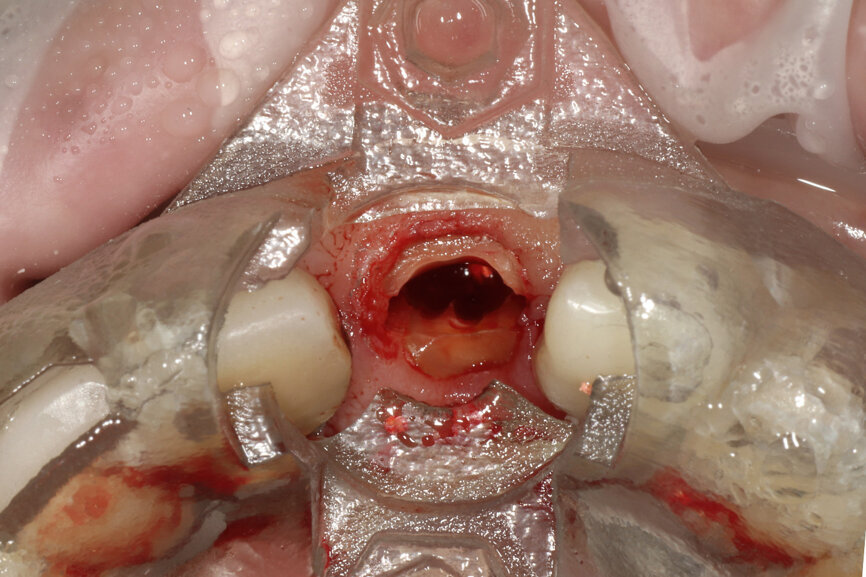
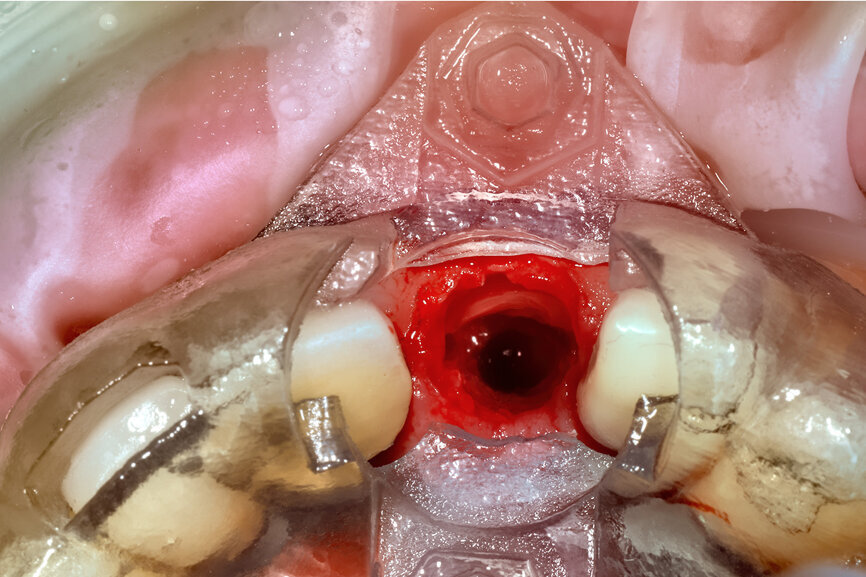
Fig. 22a: The final insert was designed to receive the guided sleeveless drills for accurate osteotomy preparation (a). The osteotomy was prepared to avoid
proximity to the remaining root fragment while leaving sufficient restorative space as previously planned (b).
Fig. 22b: The final insert was designed to receive the guided sleeveless drills for accurate osteotomy preparation (a). The osteotomy was prepared to avoid
proximity to the remaining root fragment while leaving sufficient restorative space as previously planned (b).
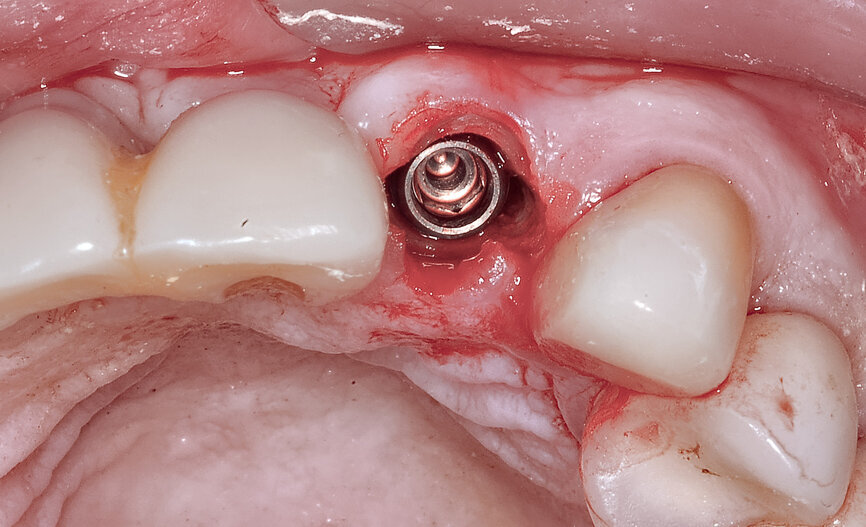
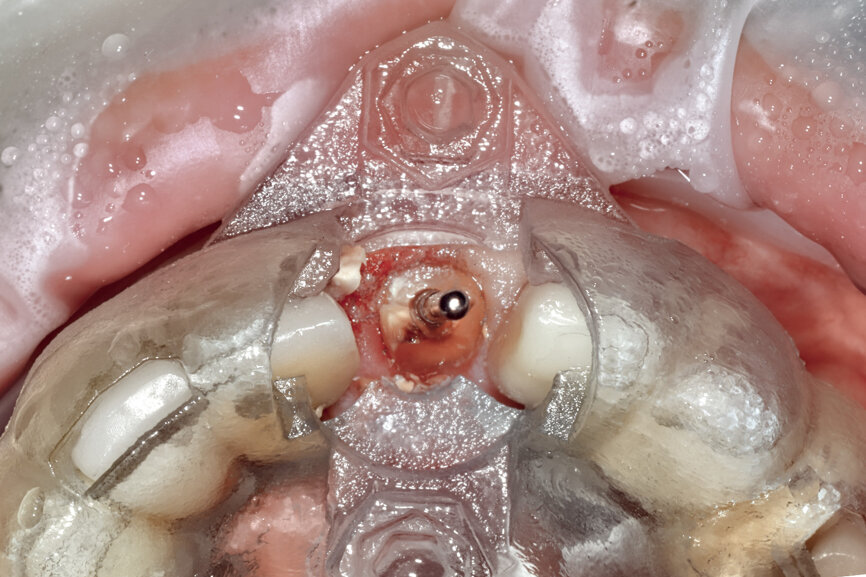
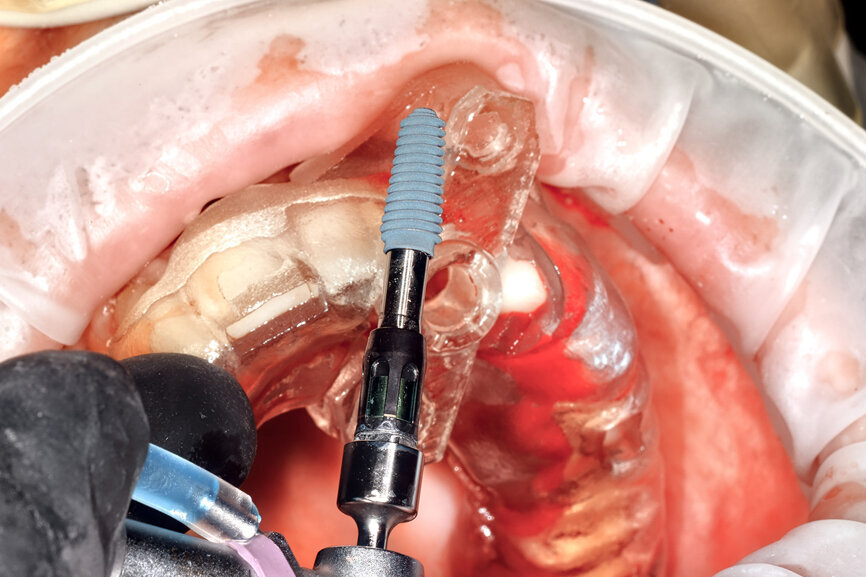
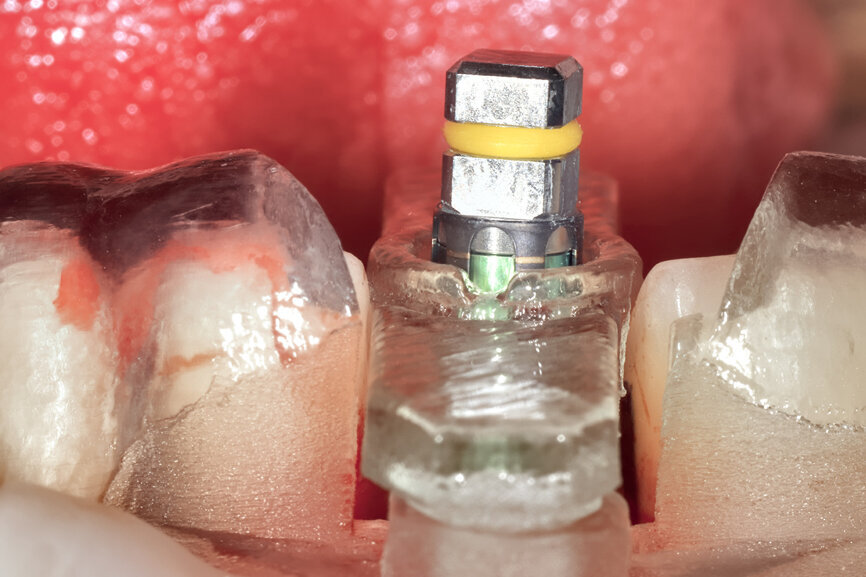
Fig. 23: The implant, seen prior to placement,
using the R2GATE surgical carrier for full-template guidance through the sleeveless guide.
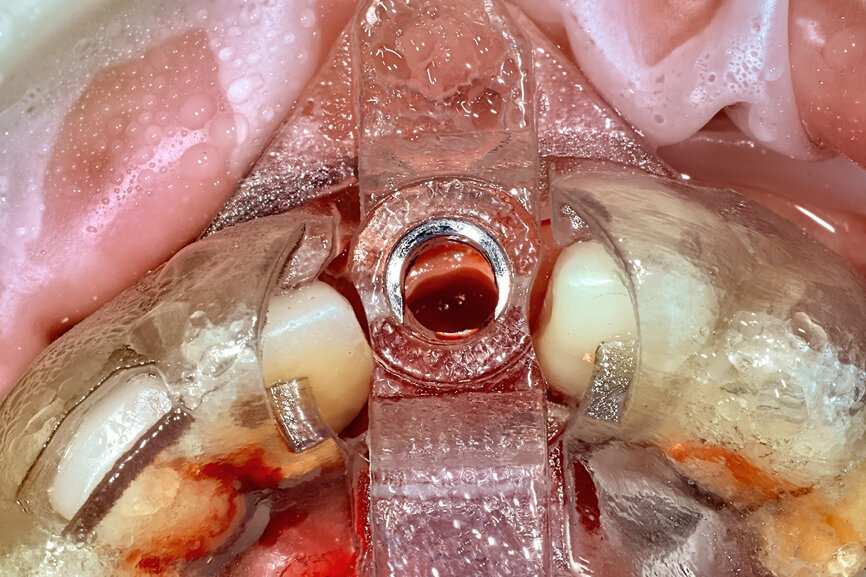
Fig. 24a: Depth control and rotational positioning were accurately
confirmed with the notch indicator on the template corresponding with the insertion tool (a). The occlusal view illustrated that the anti-rotational internal
conical–hexagonal connection was positioned towards the facial aspect (b).
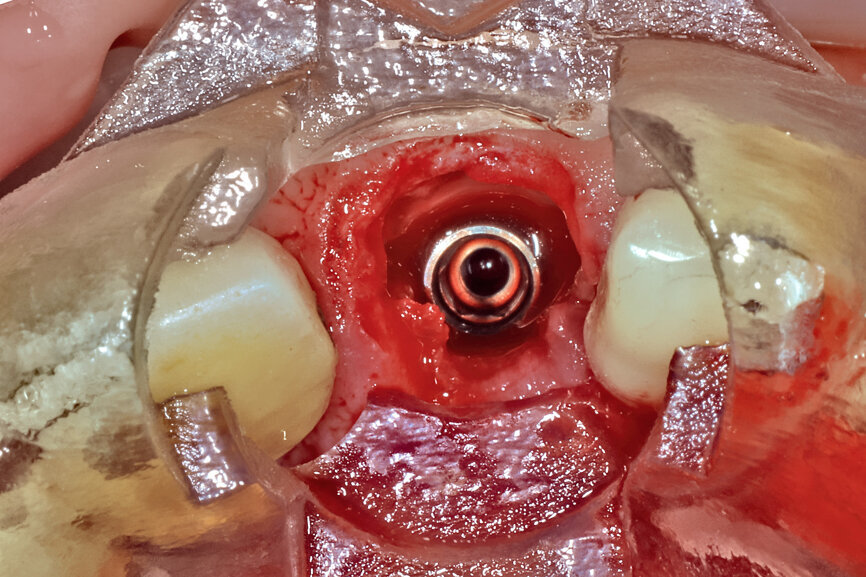
Fig. 24b: Depth control and rotational positioning were accurately
confirmed with the notch indicator on the template corresponding with the insertion tool (a). The occlusal view illustrated that the anti-rotational internal
conical–hexagonal connection was positioned towards the facial aspect (b).
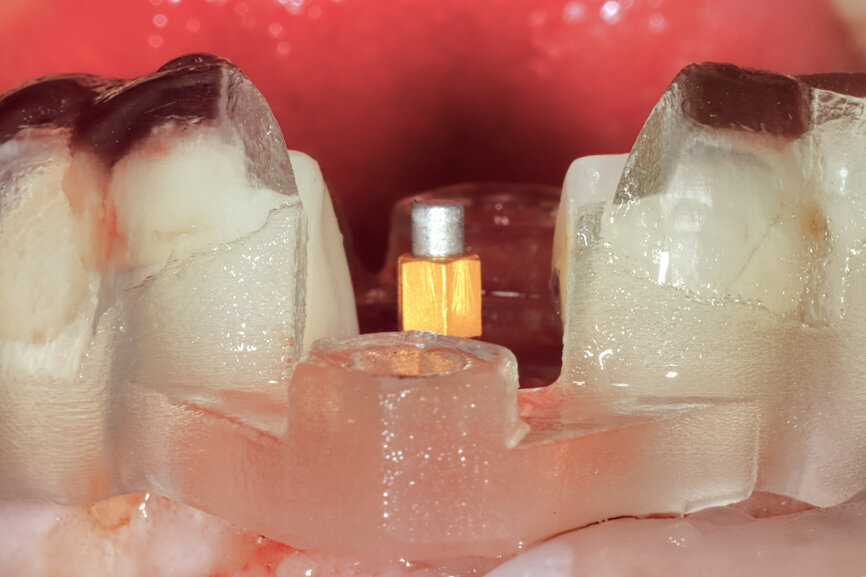
Fig. 25: Using an implant-specific SmartPeg, a baseline ISQ value of 76 confirmed sufficient initial stability to place an immediate restoration.
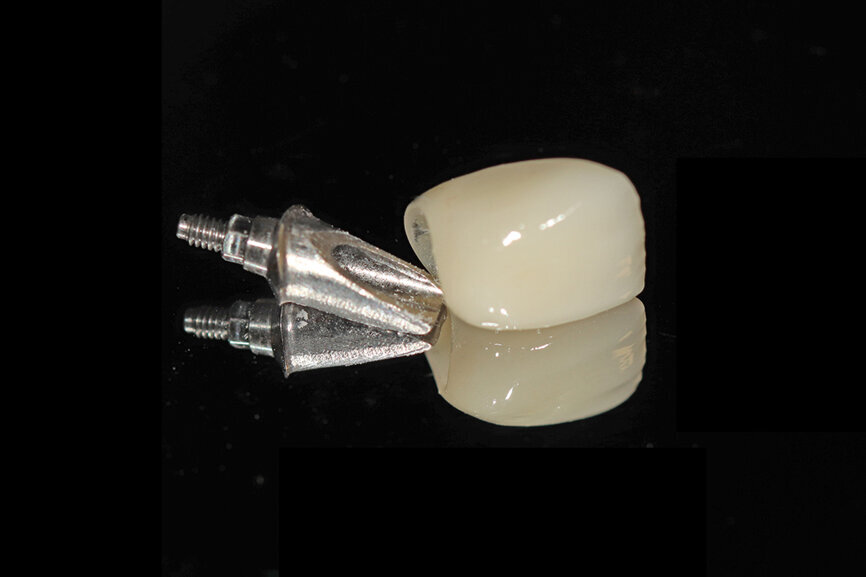
Fig. 26a: The prefabricated CAD/CAM abutment and transitional crown
Fig. 26b: A post-op periapical radiograph confirmed successful sub-crestal placement of
this platform-switched design.
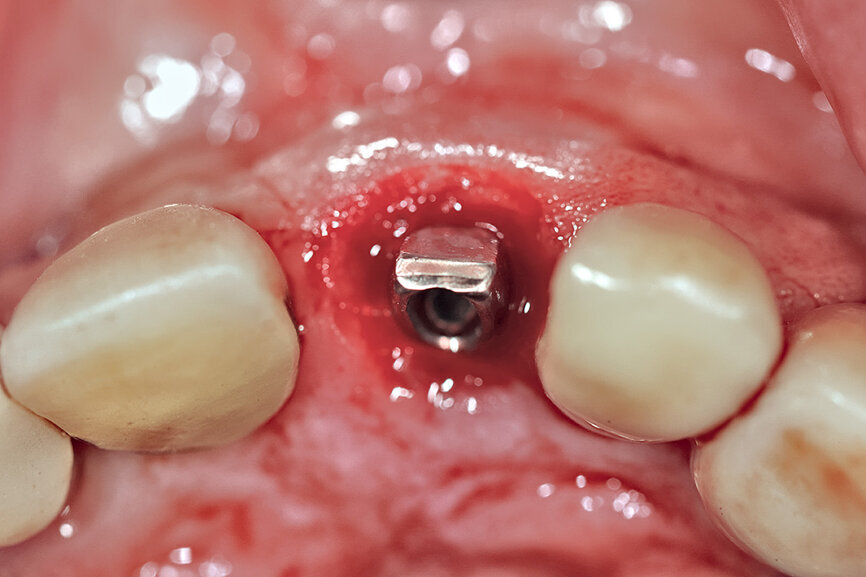
Fig. 26c: The abutment in place.
Fig. 26d: The soft-tissue contours were excellent; no sutures were required for the transitional restoration.
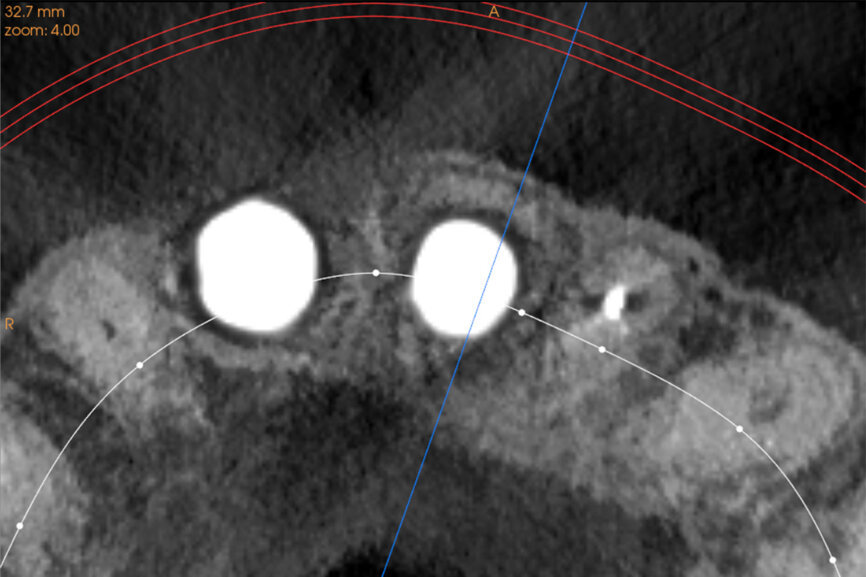
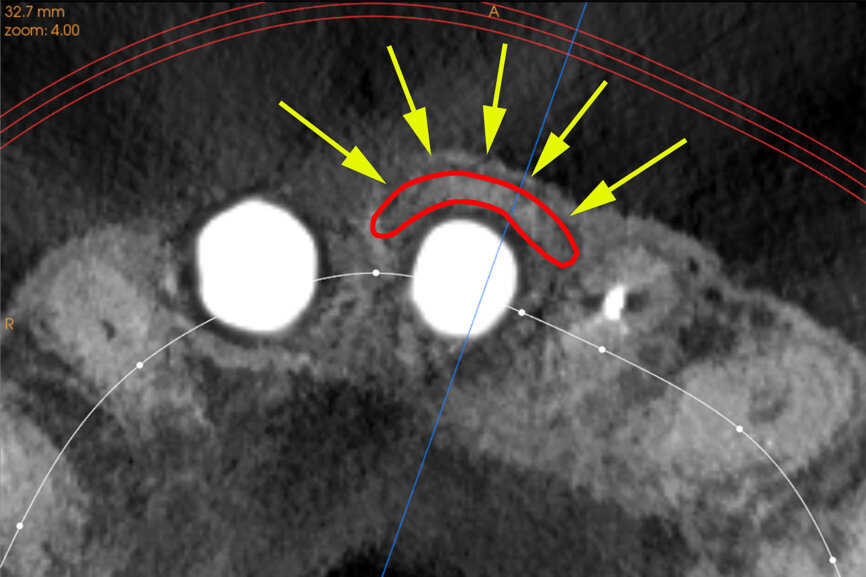
Fig. 27a: The post-op CBCT scan axial view revealed the intact crescent shape of the root membrane (a), as outlined in red in facial to the opaque
implant position (b).
Fig. 27b: The post-op CBCT scan axial view revealed the intact crescent shape of the root membrane (a), as outlined in red in facial to the opaque
implant position (b).
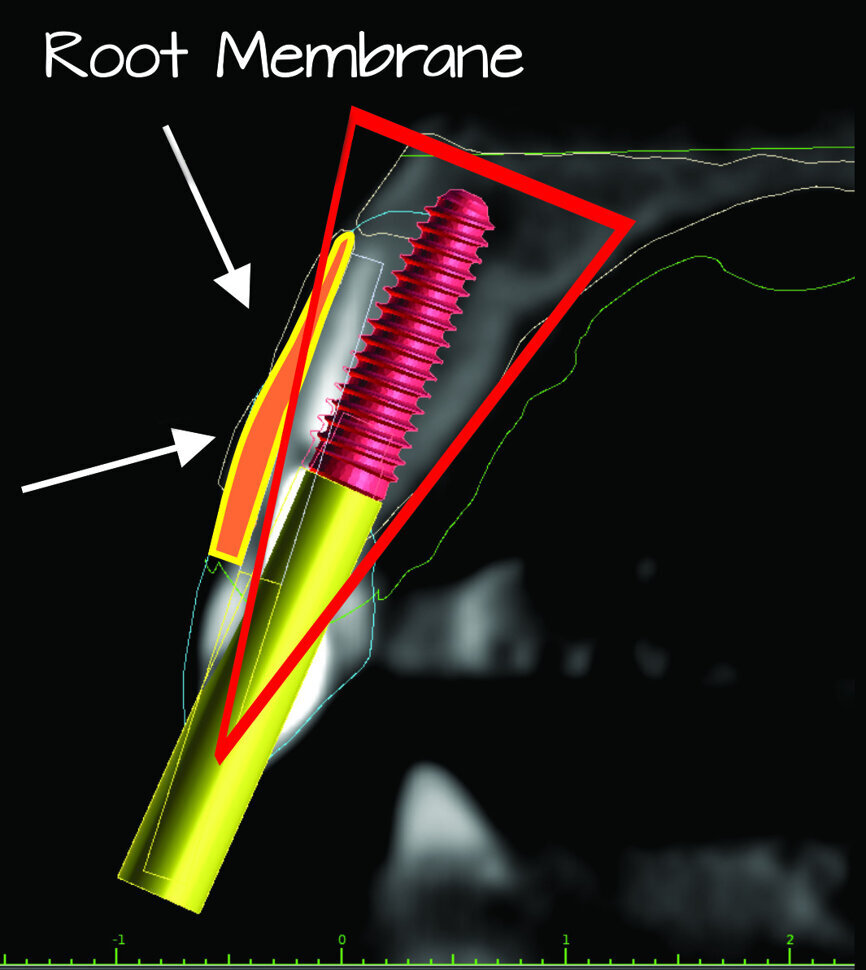
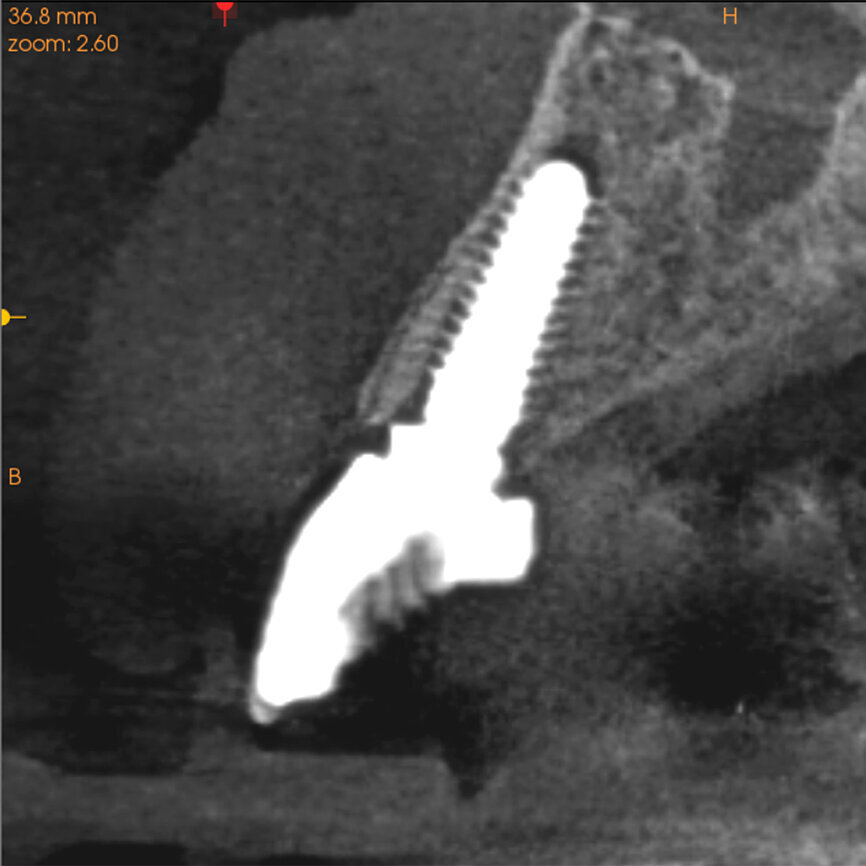
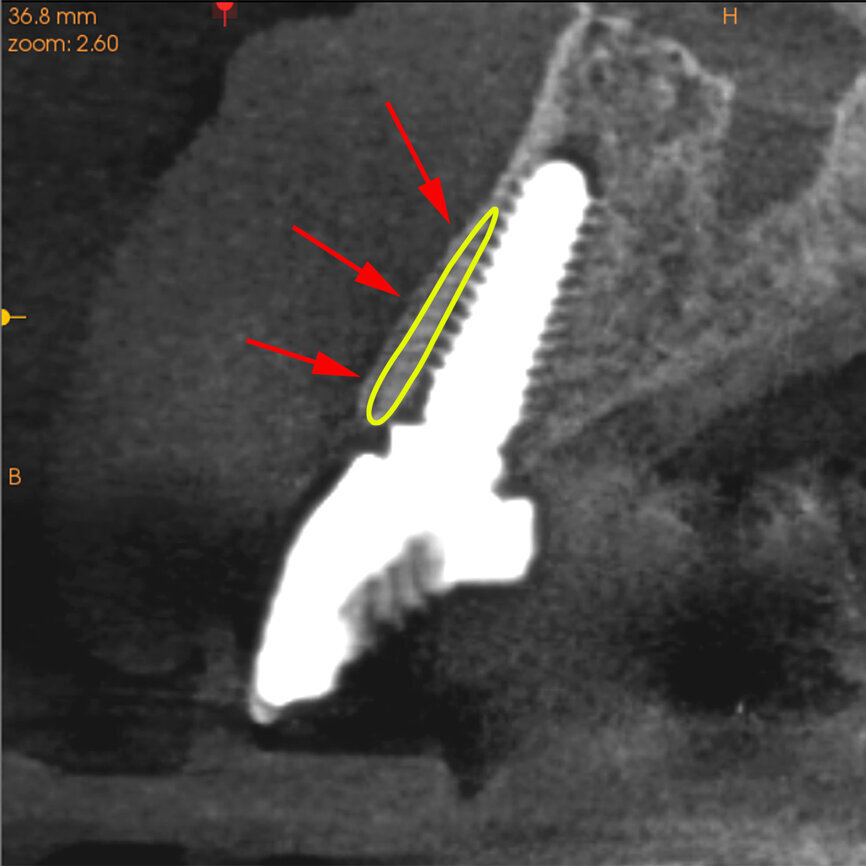
Fig. 28a: The post-op cross-sectional view clearly illustrated the position of the implant (a), the definitive restoration located palatal to the root membrane (b),
as outlined in yellow (red arrows).
Fig. 28b: The post-op cross-sectional view clearly illustrated the position of the implant (a), the definitive restoration located palatal to the root membrane (b),
as outlined in yellow (red arrows).
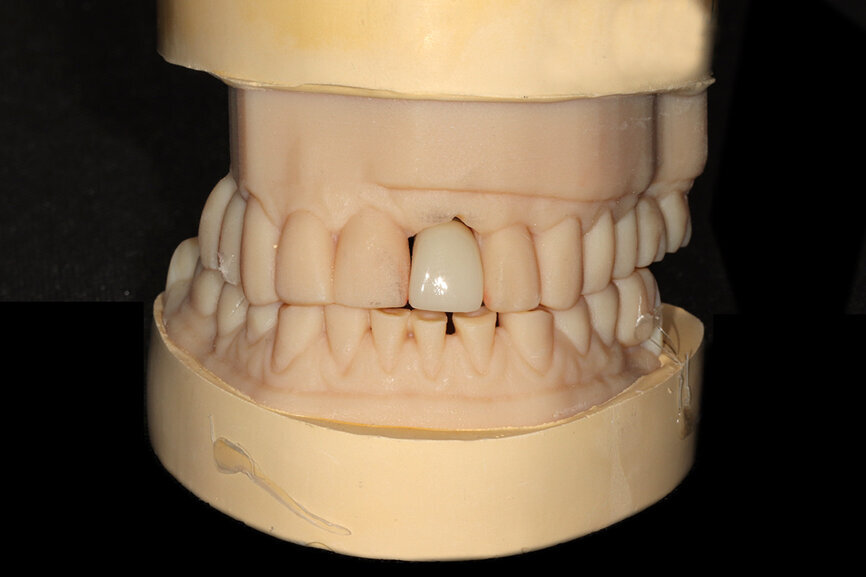
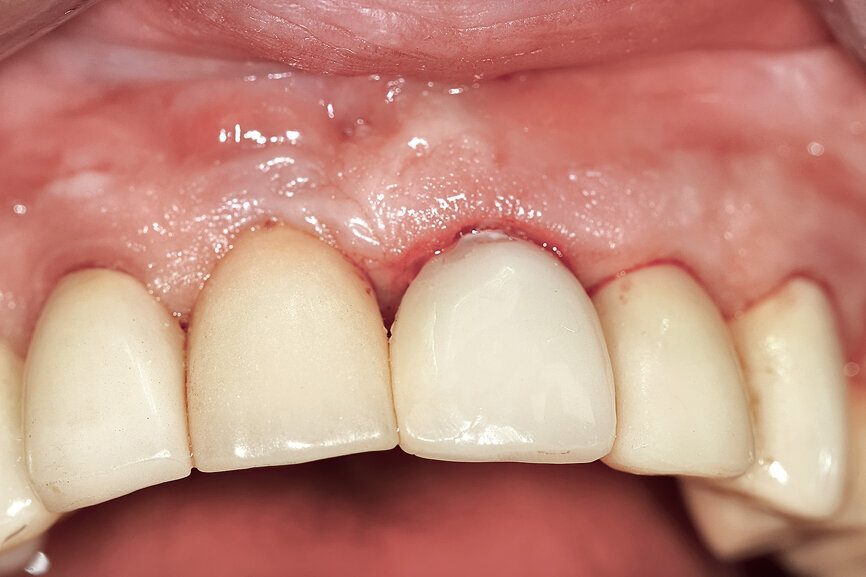
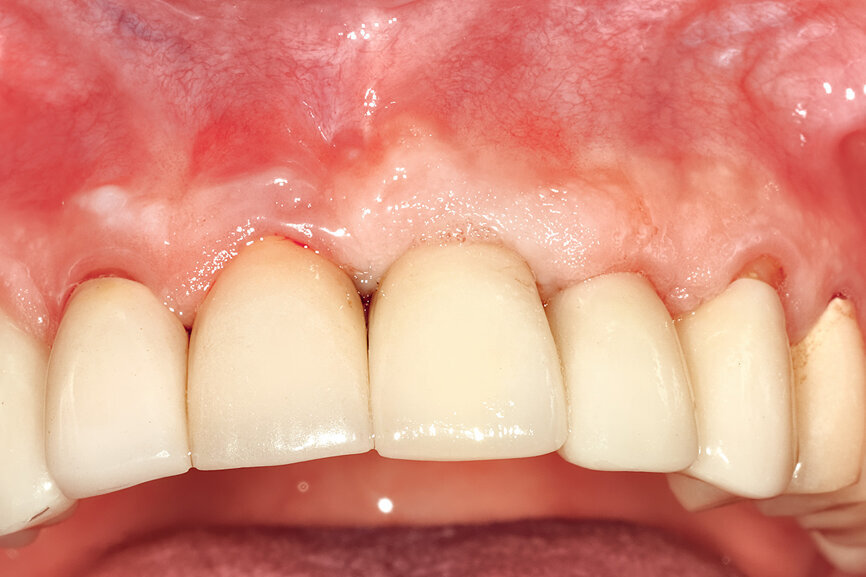
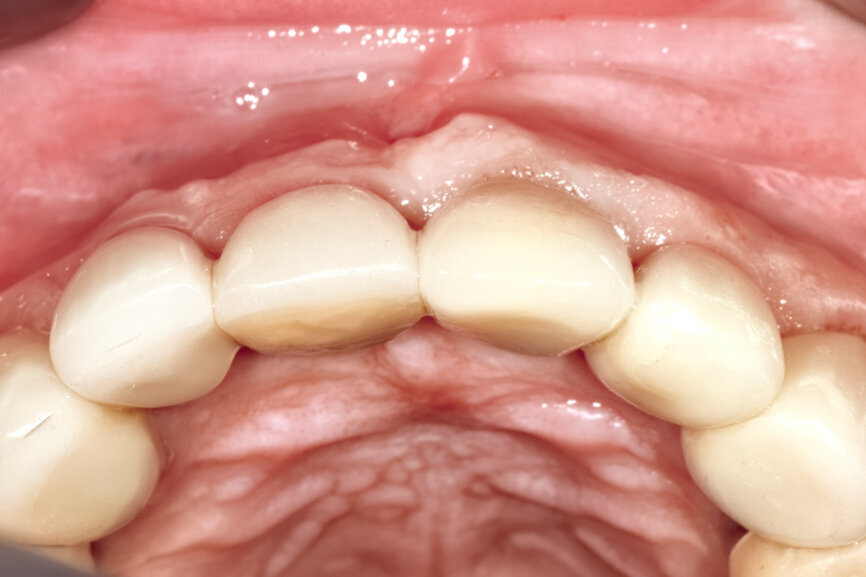
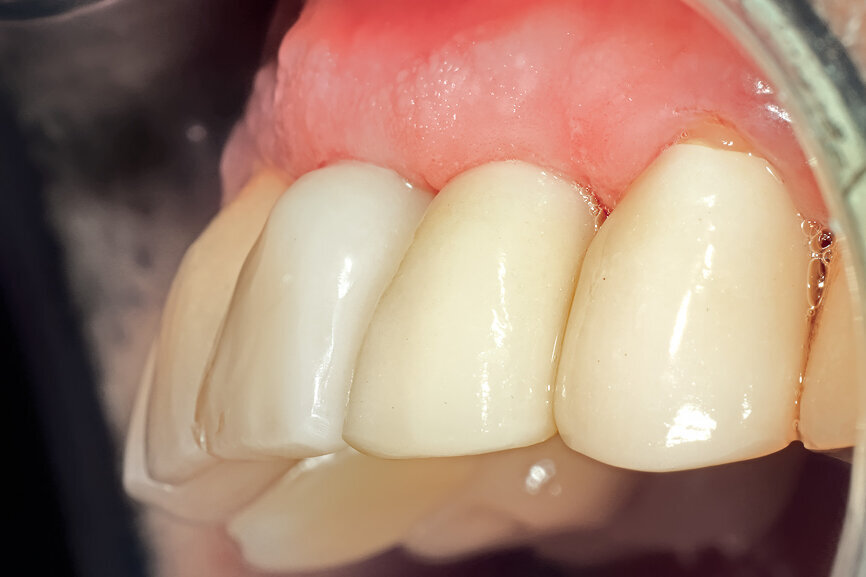
Fig. 29: The definitive restoration exhibited excellent retention of the soft-tissue profile.
Fig. 30a: The occlusal view revealed the volume maintained with
the soft-tissue cervical contours (a), and the lateral retracted view revealed an excellent soft-tissue emergence profile (b).
Fig. 30b: The occlusal view revealed the volume maintained with
the soft-tissue cervical contours (a), and the lateral retracted view revealed an excellent soft-tissue emergence profile (b).
The ability to perform the procedures requires careful diagnosis, treatment planning and excellent control of the drilling process to ensure that the root fragment will be maintained while maximising implant stability. In many cases, it may also be possible to provide immediate transitional restoration when high implant stability is achieved. However, complications can also arise when the root fragment is lost or the implant fails to integrate. It should be noted that PET has mainly been accomplished with a diagnostic freehand method for sectioning roots, osteotomy preparation and implant placement. The current article describes methods of providing PET procedures using full-template guidance based on a thorough appreciation of the existing anatomical structures utilising advanced state-of-the-art treatment planning tools, 3D design software, 3D printing and/or CAD/CAM surgical templates.
One indication for PET is when a patient presents with a horizontally fractured clinical crown (Fig. 1). While a 2D radiograph will reveal the extent of the horizontal fracture, length of the remaining root and approximation of the bone apical to the root, there is not enough information to plan for a PET procedure. A CBCT scan is recommended in order to fully appreciate the root position within the alveolus and the potential difference between the trajectory of the bone and the trajectory of the root as can be visualised with a cross-sectional image (Fig. 2). Utilising interactive treatment planning software makes it possible to plan the initial drill path to accurately section the root to its apex (Fig. 3a). This can be accomplished by creating a custom implant design to match the diameter of the initial drill with an abutment projection in order to fully appreciate the trajectory through the clinical crown (Blue Sky Plan, Blue Sky Bio). It is important to visualise the root fragment that will remain in order to properly simulate the position of the implant in the alveolus (Fig. 3b). The apical portion of the implant can be positioned to gain stability in host bone using the Triangle of Bone. It is important to note that a cross-sectional slice may only be 0.125 mm in thickness based on the CBCT acquisition, and therefore all images in all views must be visualised to confirm the plan. Utilising 3D segmentation (separating objects by density values), it is possible to define each root and further assess the simulated position of the implant with a sagittal cut through the 3D reconstructed volume (Fig. 4).
The ability to export volumes in STL format allows these objects to be edited and utilised in other software applications, such as Meshmixer (Autodesk). The STL file of the root image was imported into Meshmixer, and the root was virtually sectioned using Boolean difference to mimic the crescent shape for PET (Fig. 5a). The apical portion of the simulated implant can then be positioned so as not to touch the root fragment while engaging in host bone for stability (Fig. 5b).
Planning with such precision is predicated on the acquisition of a satisfactory CBCT scan with a proper field of view and the incorporation of occlusal surface data STL files of the arch form, digitised through either an intra-oral scan or a desktop scanner imported into the software. Two 3D-printed templates were then designed on the accurate digitised surface model, one for the initial drill to section the tooth at the root apex and the second to use sequential guided drills to drill through the root itself (Fig. 6).
A 2 mm pilot drill, which was long enough to reach the root apex with the tooth-borne surgical guide in place, was utilised with a sleeveless guided approach (Fig. 7a). Removing the guide allowed for inspection of the drill through the tooth (Fig. 7b). Using guided drills with long shanks in a sleeveless guide allowed for sequential and accurate removal of the tooth and subsequent bone beyond the apex of the natural tooth root (R2GATE, MegaGen; Fig. 8). The cylindrical tooth preparation/osteotomy resulted in the desired crescent shape to provide space for the implant (Fig. 9). The root was then sectioned mesiodistally using specialised drills (Root Membrane Kit, MegaGen) and the palatal sectioned removed. Utilising the template, the implant was placed into the osteotomy using the correct implant carrier to achieve full-template guidance and stability measured using resonance frequency analysis (RFA) to obtain the implant stability quotient (ISQ; Fig. 10).
The concept of drilling through the root is not new and has been reported in the literature.8 Using guided methods for the socket shield technique has also been reported using a CAD/CAM-fabricated template.9 However, the ability to use technology to plan and execute a fully guided procedure for a PET, socket shield technique and root membrane technique illustrates additional methodology to aid clinicians in successful outcomes.
The first concept described the use of two separate templates, one for separating the root at the apex and the second for drilling through the tooth and placing the implant. Continuing the evolution, we present a second option, which does not require the removal of the base template, but has inserts to allow for the different drills and angulation required for the PET technique: the stackable tooth-borne guide. The new technique has four separate components: (1) a base template (stackable tooth-borne guide); (2) a pilot drill guide for the root ape (APEX STACK); (3) a crescent-shaped guide for shaping root fragments (PET Shaper STACK); and (4) a guide for osteotomy drilling and placing the implant through the guide (Surgical Guide STACK; Fig. 11).
Case report
A 62-year-old male patient presented with a hopeless prognosis for a post fracture in the left central incisor requiring extraction (Figs. 12a & b). The preoperative periapical radiograph revealed an existing implant supporting a metal–ceramic restoration for the adjacent region #11 (Fig. 13). The CBCT (CS 9600, Carestream Dental) cross-sectional image revealed a favourable preoperative condition relating to the trajectory of the endodontically treated root to the alveolus for a PET procedure (Fig. 14a). Using the native Carestream 3D Imaging software, a simulated implant and abutment projection was positioned within the available bone to avoid the root fragment (Fig. 14b).
The final positioning of the implant, as determined by the restorative requirements, and design and fabrication of the tooth-borne stackable surgical template, was accomplished using dedicated interactive treatment planning software (360dps, 360Imaging). The base template was designed to seat firmly on the adjacent teeth, incorporating buccal and lingual hexagonal offsets to engage the different drill guide inserts (Fig. 15a). Separate inserts were then fabricated for the initial drill guide to reach the root apex to accommodate sectioning, followed by a second guide for final osteotomy drilling and implant placement (Figs. 15b & c). The accuracy of the implant and template design provides the opportunity for true restoratively driven planning, which can then be combined with CAD/CAM applications to also design and fabricate a patient-specific abutment and transitional restoration in advance of the surgical intervention (Fig. 16).
Prior to the guided drilling, a Gates–Glidden drill was used to remove any gutta-percha within the root. Utilising the tooth-borne template and the first insert, initial long shaper drills (IS1, IS2) were used to reach the apex of the root (Root Membrane Kit; Fig. 17). A periapical radiograph confirmed that the apex length had been reached and that all the gutta-percha had been removed (Fig. 18). The second insert had a metal cylinder that allowed for the long, round diamond drills to shape the root into the desired crescent shape (Fig. 19a). The insert was removed to access the palatal root (Fig. 19b). Using appropriate instrumentation such as periotomes, elvatomes or FRINGS forceps (both TBS Dental), the palatal root was carefully removed (Fig. 20). A periapical radiograph confirmed that the palatal root had been completely removed (Fig. 21). The next insert contained the final diameter to receive the guided sleeveless drills for osteotomy preparation (Fig. 22a). The osteotomy was prepared to avoid proximity to the remaining root fragment while leaving sufficient restorative space, as previously planned in the software simulation (Fig. 22b). Implant placement (AnyRidge, MegaGen) was facilitated by the R2GATE surgical carrier for full-template guidance at the appropriate torque values (Fig. 23). Depth control and rotational positioning were accurately confirmed with the notch indicated on the template to correspond with the insertion tool (Fig. 24).
The initial plan was for immediate extraction, immediate placement and immediate restoration. Therefore, it was essential to measure the implant’s stability with an objective technology, RFA, which provides an ISQ value utilising an implant-specific SmartPeg (Osstell; MEGA ISQ, MegaGen). The baseline ISQ value (76) confirmed sufficient initial stability to place an immediate restoration (Fig. 25). The prefabricated CAD/CAM abutment was then secured to the implant, and a postoperative periapical radiograph confirmed successful sub-crestal placement for this platform-switched design (Fig. 26a). The transitional acrylic restoration was then placed and examined for any occlusal interferences (Fig. 26b). It was important that the restoration be out of occlusion to avoid premature forces that could complicate integration. The soft-tissue contours were excellent, and no sutures were required, since no flap was raised (Figs. 26c & d). After a period of eight weeks, the implant stability was measured to be at 80 ISQ, confirming that the integration process had continued to progress successfully and that the implant was ready for the definitive restoration. An intra-oral scanner and scanning abutment were then utilised to capture the position of the implant and soft-tissue emergence profile. The post- operative CBCT scan revealed the intact crescent shape of the root membrane (Figs. 27 & 28). The definitive restoration was then delivered and exhibited excellent retention of the soft-tissue profile (Figs. 29 & 30).
Conclusion
PET, root membrane and socket shield concepts have gained popularity as the techniques have been refined and their efficacy proved in published long-term studies. The purpose of retaining the root is to maintain the periodontal ligament attachment to the bony walls of the socket in order to prevent subsequent resorption and loss of tissue volume which often occurs after tooth extraction. PET has been proved to preserve bundle bone and tissue volume with and without immediate implant placement, yet this minimally invasive treatment modality is highly technique-sensitive and may result in complications if proper protocols are not followed. Therefore, a complete understanding of the 3D anatomical presentation is essential for preliminary diagnosis, treatment planning and execution of the procedure. The present article has described two alternatives that maximise the diagnostic phase using state-of-the-art CBCT imaging and planning software to provide full-template guidance with a new stackable tooth-borne guide with specific inserts for the root preparation as well as the osteotomy preparation and delivery of the implant. As with most techniques, further clinical trials are recommended to provide additional long-term data to validate these treatment modalities.
Acknowledgement: The authors would like to thank Dr Barry Kaplan of Morristown in New Jersey in the US for his expertise and assistance in the preparation of this article.
Editorial note: A list of references available from the publisher. This article was published in digital―international magazine of digital dentistryVol. 1, Issue 4/2020. It originally appeared in Dentistry Today in September 2020, and an edited version is provided here with permission from Dentistry Today.
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East

































To post a reply please login or register