Implant-prosthesis systems have continuously evolved regarding osseointegration, implant size reduction and long-term predictability results, guided by the stability and absence of inflammation of the peri-implant tissue. The following case report demonstrates the results that are obtainable today.
Introduction
Recently, we saw an evolution in the macro-geometries of dental implants and prosthetic components that has led to a significant, sometimes radical, increase in the biological yield of dental implants, a modified surgical approach and varied protocols. The use of short implants has become a predictable therapeutic alternative and is sometimes able to avoid complex vertical regeneration procedures. Now, we have evidence of the marginal bone response after years of short implant loading, including with unfavourable levers and crown–root ratios (2:1 or more). In the following case report, I will present a follow-up of nine years after the insertion of GTB implants (Advan) in positions #34 and 36, on which a bridge from implant #34 to 36 was retained.
Case presentation
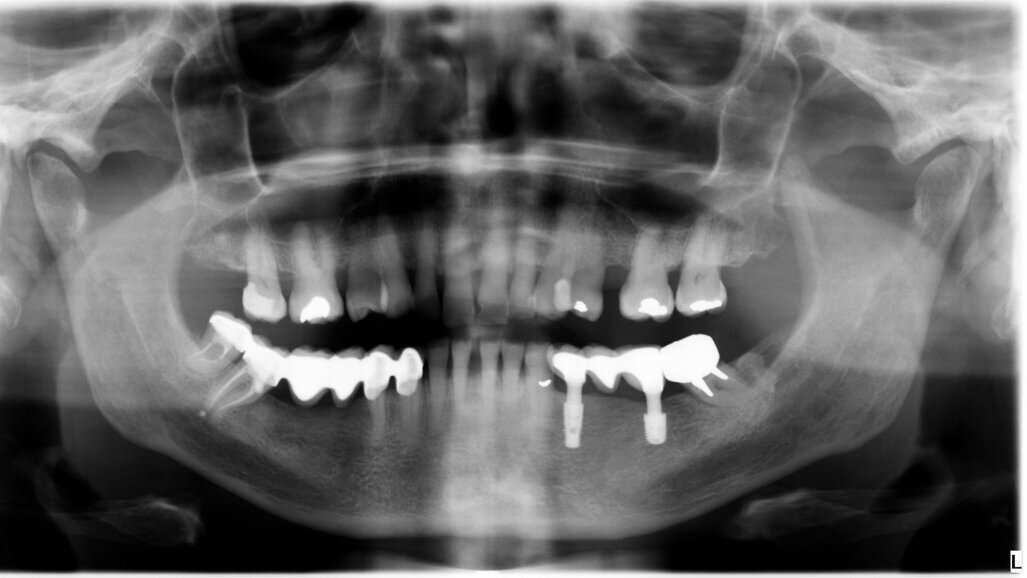
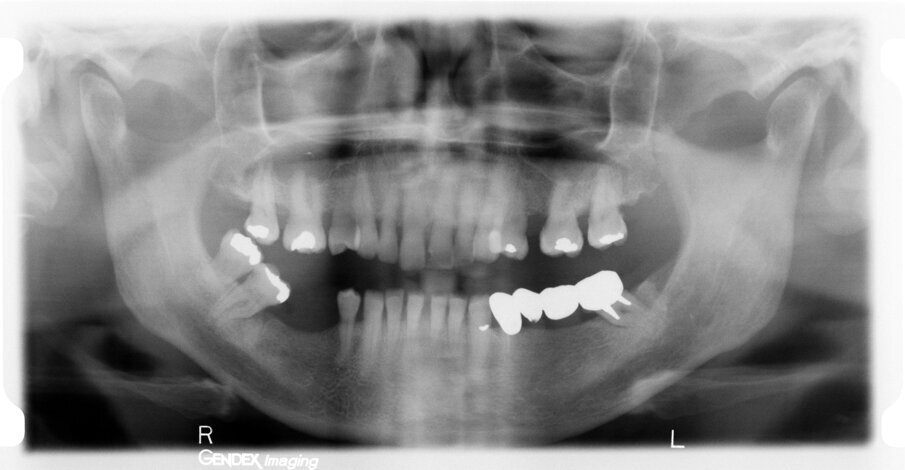
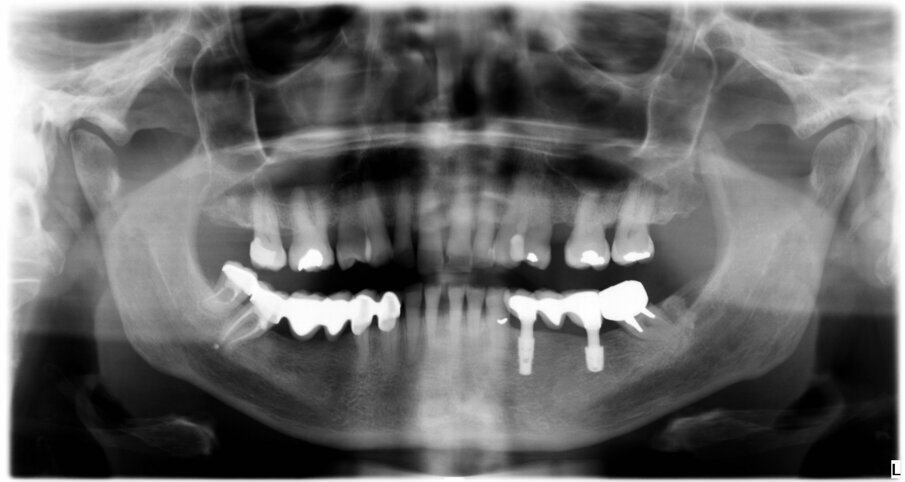
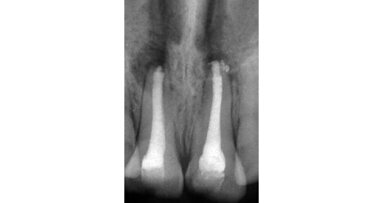
The female patient was 59 years old and had no noteworthy medical history, except for degenerative osteoarthritis of the left hip joint and compensated hypertension. She complained of chewing pain in the third quadrant. On physical examination, she presented with an old-fashioned bridge prosthesis with partial mobility, loaded on natural teeth. After radiographic evaluation with a dental panoramic tomogram of the dental arches, tooth #34 appeared devitalised, and tooth #37 appeared devitalised and a fused post-abutment was mesialised and considerably inclined (Fig. 1).
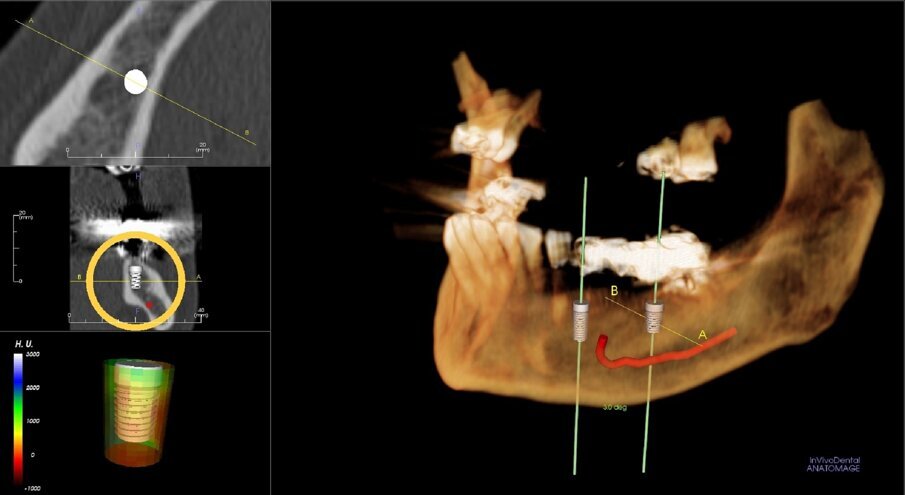
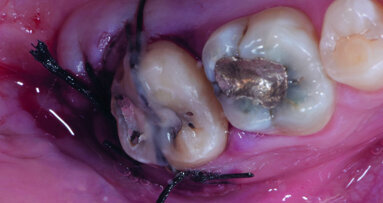
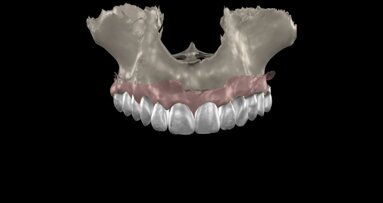
It was evident that tooth #34 had to be extracted. Despite the overload of tooth #37, the patient refused its extraction because it was not painful. We therefore proceeded with the separation of the existing bridge, maintaining the coverage of tooth #37 and the exposure of the edentulous part. Subsequently, the extraction of tooth #34 was performed. A CBCT assessment of the mandibular dental arch was performed, and the insertion of a 3.6 mm diameter and 9.0 mm long GTB implant in position #34 and of a 4.3 mm diameter and only 6.0 mm long GTB implant was planned (Fig. 2). This last choice was necessary not to avoid contact with the inferior alveolar nerve but because of the presence of a very high mylohyoid line and the consequent inclination of the lingual bone wall of the mandible below that line. We favoured the prosthetic axis of the implant rather than a greater length of the implant, which is obtainable by tilting it in a lingual–buccal direction. The surgical planning was performed according to the surgical protocol for GTB implants, which provides for the flattening of the knife blade ridge, the positioning of implants in the prosthetic axis and sinking the implant to the sub-crestal level of 1.5 mm. During surgery, we obtained an insertion torque of 25 Ncm in position #34 and of 20 Ncm in position #36 (Figs. 3a & b).
The soft tissue appeared to have little attached gingiva, which was dissected with the opening of the flap and then sutured with interrupted sutures, and these were removed after ten days. Two healing abutments with a height of 4.5 mm were positioned above the implants immediately after surgery.
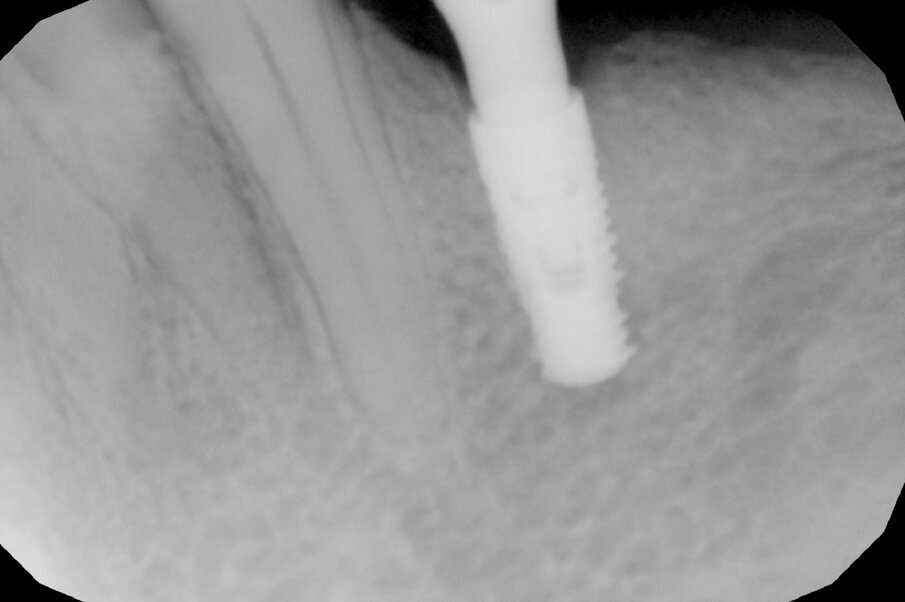
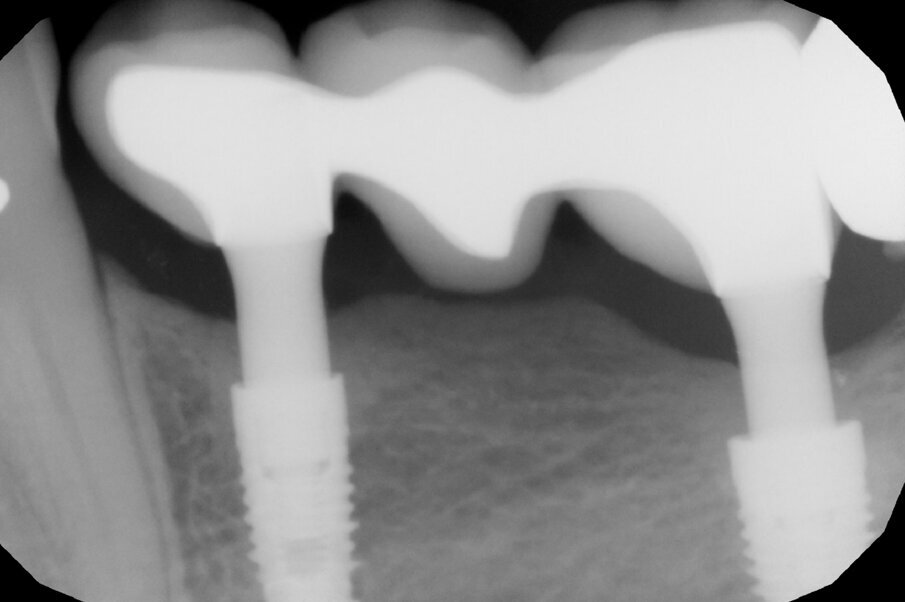
After 70 days, radiographic control was performed and the healing abutments were replaced with two easy abutments directly in order to comply with the one abutment, one time protocol (Fig. 4). The abutments were torqued to 30 Ncm according to the implant’s prosthetic protocol. This is necessary for the activation of the conical coupling between implant and abutment and for a sterile connection that prevents micro-movements and bacterial infiltration between implants and abutments in the sub-crestal area and the resulting bone resorption. Thereafter, we took a polyether impression on snap-on copings directly inserted on the abutments and fabricated a traditional cemented metal–ceramic bridge. In the following months, the patient initially underwent regular check-ups and professional hygiene, but thereafter kept extending the check-up times and neglecting her oral hygiene.
Results
After three years, a panoramic radiograph was performed, highlighting excellent maintenance of the bone trophism and closure of the osteotomies created with the insertion of the implants (Fig. 5). Results of this type testify to the ideal biomechanical situation created above the implants, which are then protected from any bacterial infiltration, not only by the mucosa, which appeared stable and healthy, but also by the bone bridge created to protect the implant necks.
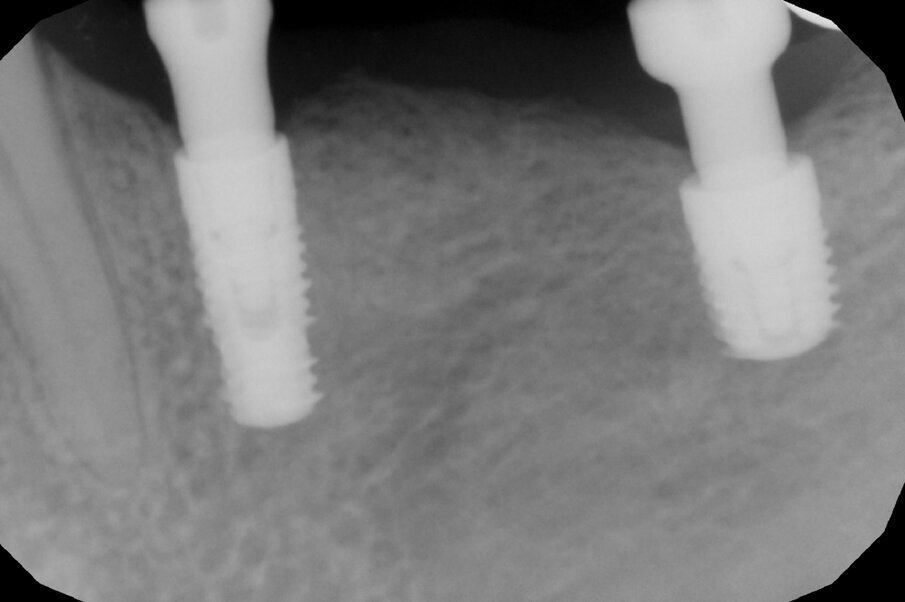
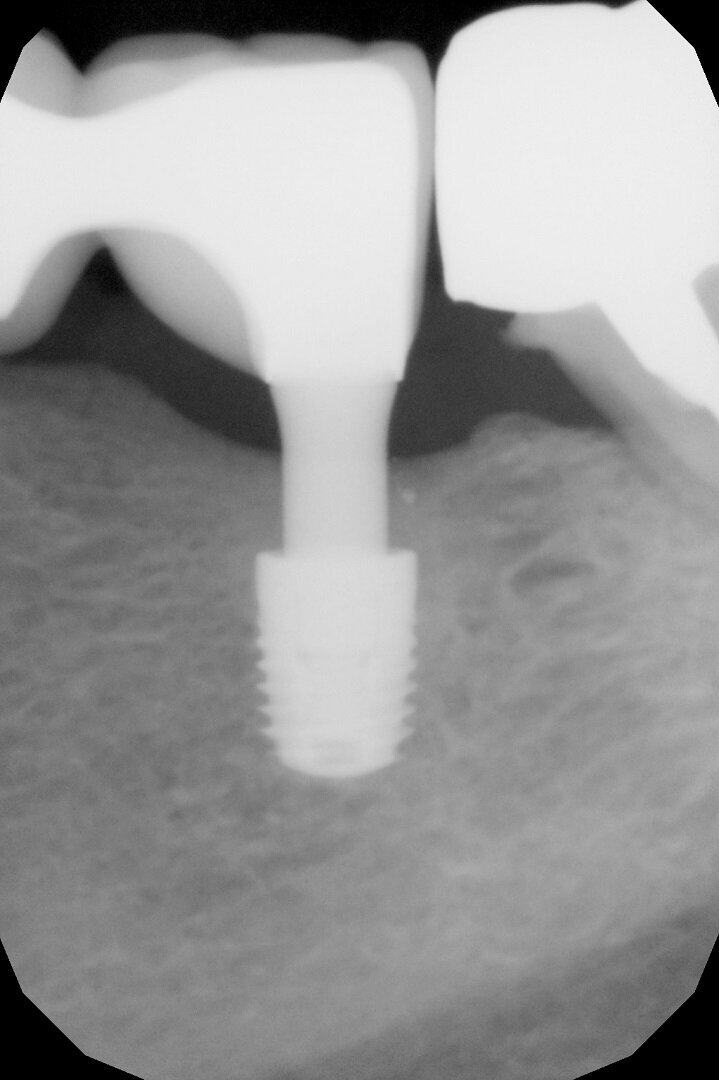
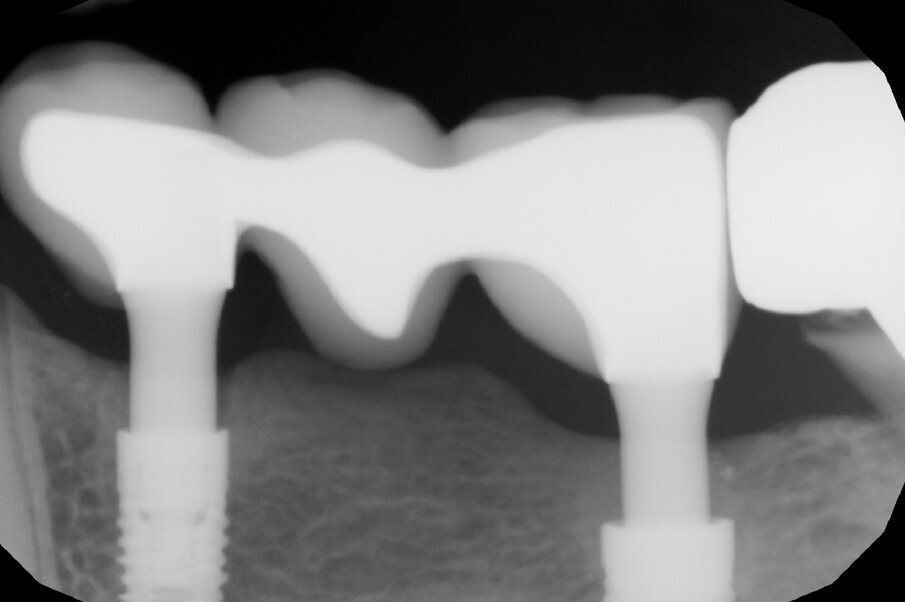
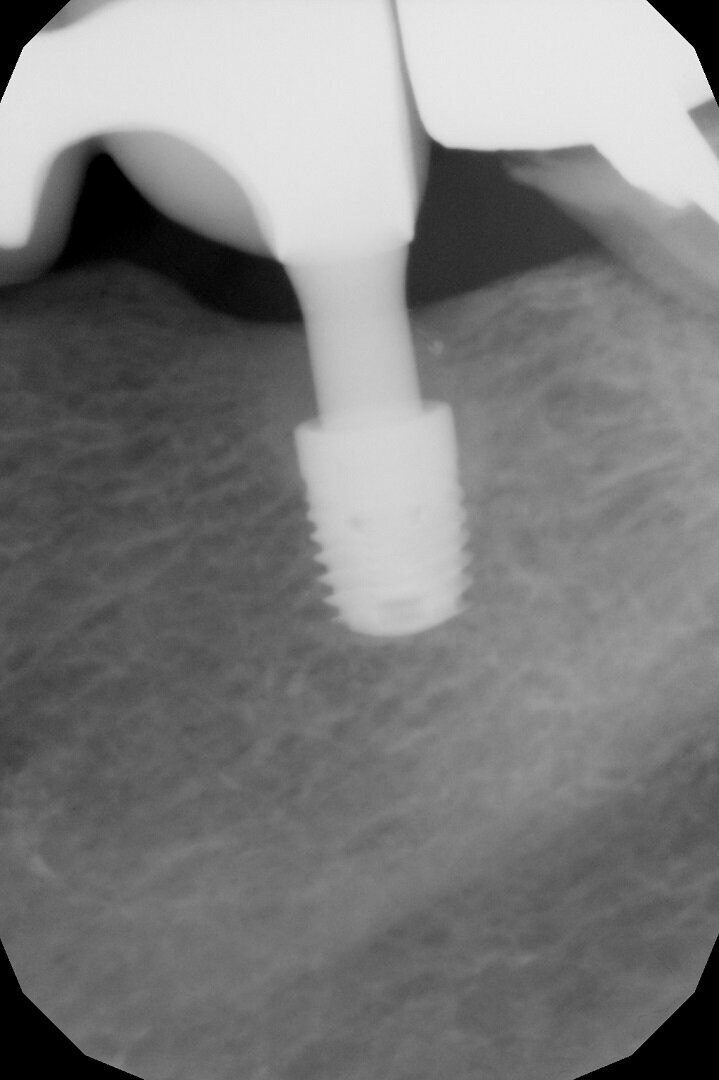
A further radiographic check was carried out seven years after the implants had been placed and showed growth of the bone level and the formation of a curved bone profile to support the interdental papillae, which is typical of natural teeth (Figs. 6a &b). Caries occurred under the crown of tooth #37, but the patient did not wish to have it treated. Upon physical examination, the soft tissue appeared stable and of excellent trophism.
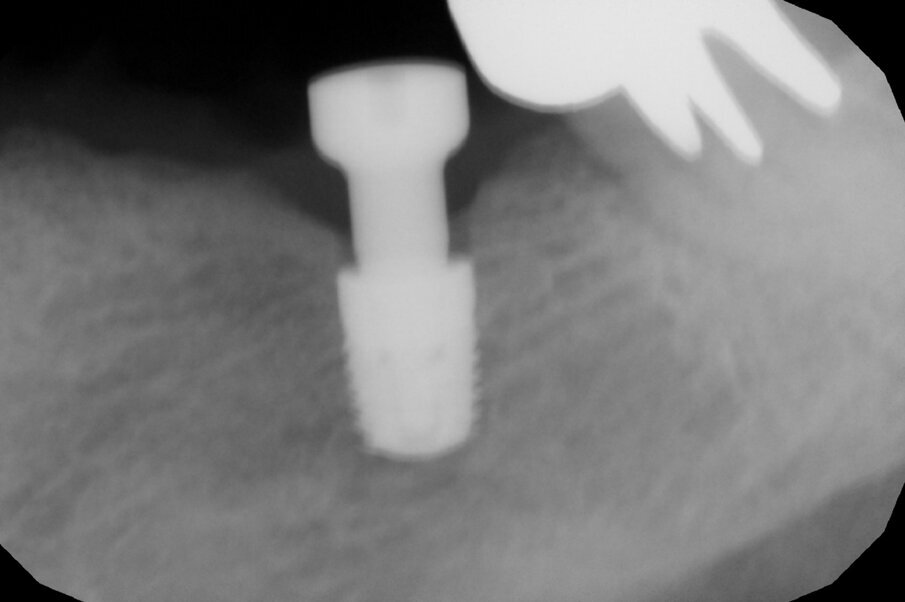
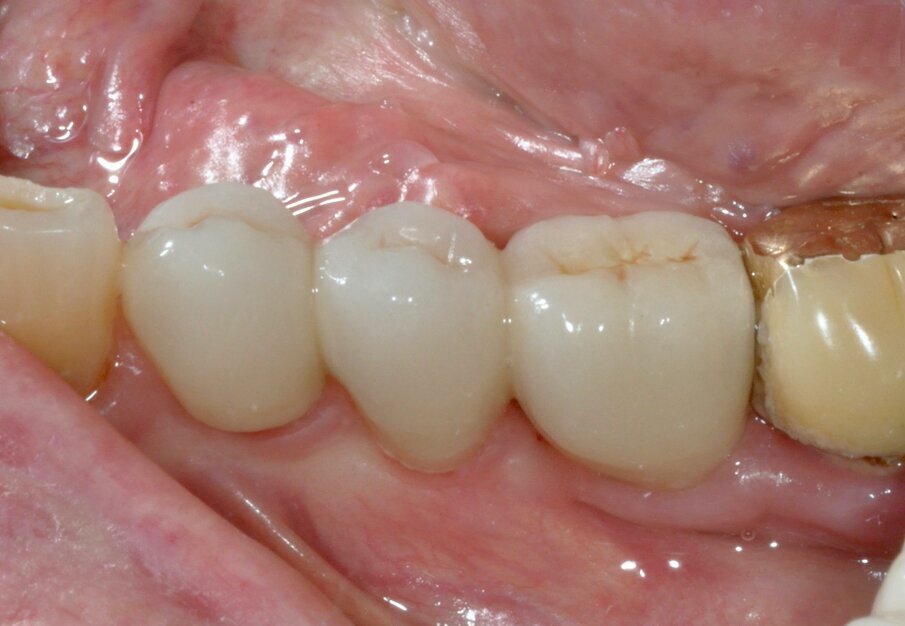
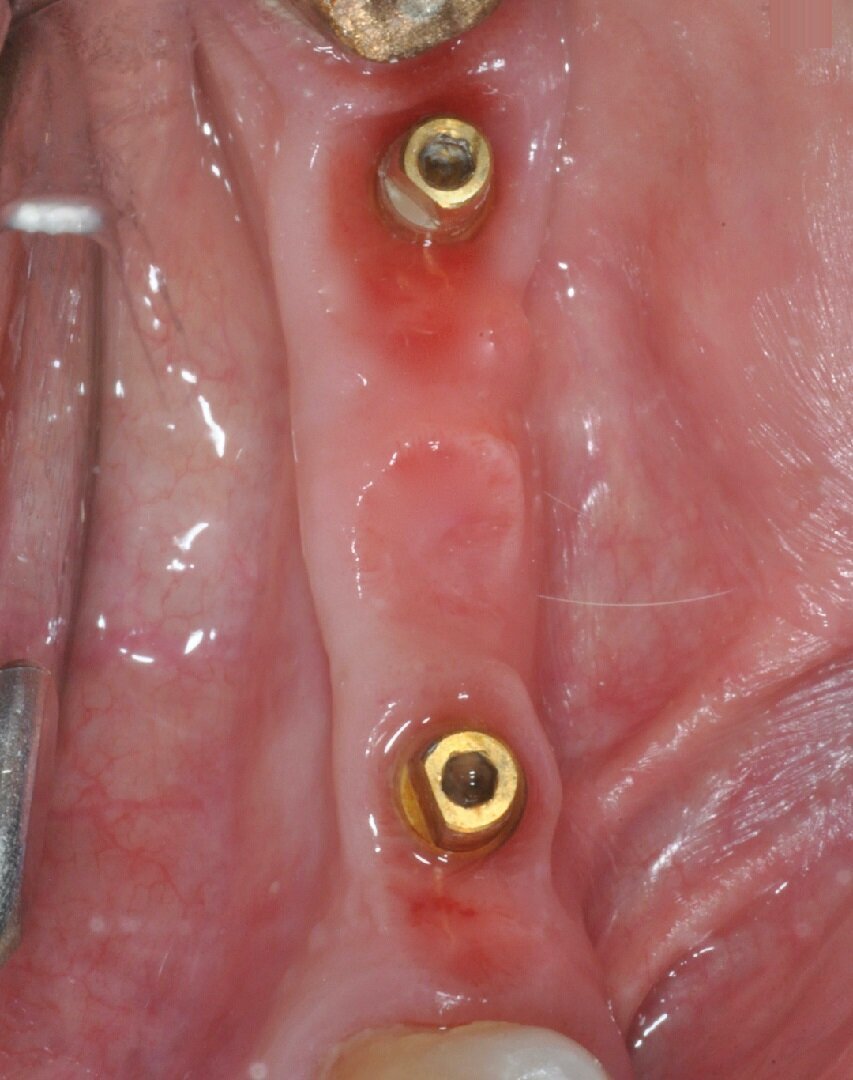
After nine years, a new radiograph was performed which highlighted how the scallop had not only been maintained but even remodelled (Figs. 7a & b). The supra-implant bone appearance around the abutments presented a hyperdense and extreme continuity with the abutment neck, despite the non-punctual hygienic maintenance, highlighted by the state of the soft tissue and by the caries affecting tooth #37, then in the terminal stage (Figs. 8 & 9). After removal of the bridge, we tried probing, but it was absolutely impossible owing to the thickness of the soft tissue.
Discussion and conclusion
The GTB implant system, through the adoption of particular macro-geometries and micro-geometries of the implants, is able to obtain great biological yield, enabling the use of short implants in the molar area and their use even as bridge abutments. The accurate execution of the surgical protocol with sub-crestal positioning and non-excessive insertion torque of the implants were indispensable conditions for obtaining the behaviour of the tissue seen in the case described, in order to avoid compressive stress during the integration phase and to achieve an insertion axis as synchronous as possible with the prosthetic axis. The sub-crestal positioning of the implants, as can be seen from the most recent literature, can only be pursued with a system that provides for a sterile implant–abutment connection, free of micromovements (conical connection), otherwise that bone would be lost in a short time after loading. Again, maintenance of tissue trophism over time (and in this case its improvement) can only be achieved with a prosthetic protocol that maximally respects the peri-implant tissue, both in quality and quantity. For this reason, the one abutment, one time protocol and the switching platform are considered essential. Only with scrupulous attention to all the steps described above and with an implant system that allows their implementation is it possible to obtain, in my opinion, long-term results such as those reported in this case. The stability of the tissue above the implants is the best evidence of the excellent health of the biological bone–implant system.
The closure of the bone on the neck of the abutment was complete, evident both from the radiographic point of view and from the inability to probe the tissue. The difference in biological behaviour between the crown–implant system and the natural crown–root system is apparent. In fact, it is clear that, to maximise the performance of implant-prosthesis systems, it is no longer sufficient to imitate nature with canonical crown ratios and soft-tissue emergence profiles that simulate natural teeth. An implant normally has a diameter smaller than that of the root system, and it must respect the bone width while maintaining a quantity of surrounding bone in proportion to the load to be supported, and this should be higher than is normally the case around natural roots.
The soft tissue with its connective fibres around the abutment collar must be respected and maintained as far as possible, in both quantity and quality. This is achievable with a switching platform, a thin implant collar and a minimal emergence profile. Where possible, like in the molar area, aesthetics must therefore be sought at the supragingival level. By systematically adopting these strategic measures, typical of the implant-prosthesis system as opposed to that of the natural tooth, it is probably possible to maintain this type of result long term.
Tags:
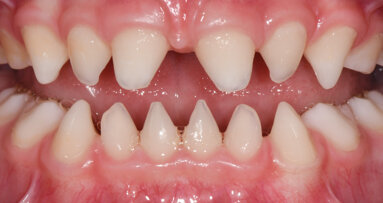
In recent years, dental implants have emerged as a pivotal advancement in dentistry, offering a popular solution for replacing natural teeth lost owing to ...
Complete edentulism is an irreversible condition that is a known marker of disease burden for oral health.1 Edentulism significantly influences both oral ...
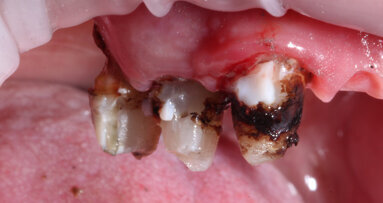
Objective: The objective of this article is to describe the successful management of an apicomarginal defect of a maxillary lateral incisor with a bone ...
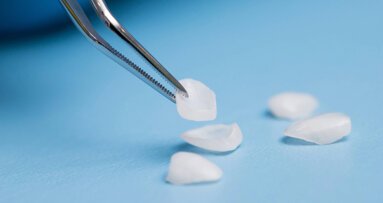
3D printing has emerged as a disruptive innovation in restorative dentistry, offering a high degree of precision, efficiency and customisation.1, 2 Recent ...
HAIPHONG, Vietnam: A new case report has demonstrated what a conservative prosthetic pathway can achieve when a patient with a relatively complex anterior ...
Digital advancements have revolutionised dentistry, providing efficient, precise dental care.1 Intra-oral scanners are replacing traditional means of taking...
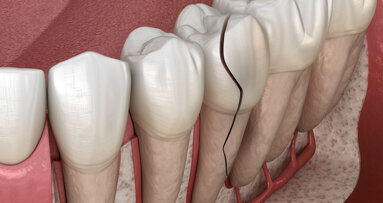
A vertical root fracture (VRF) is a longitudinally oriented fracture of the root that, depending on its cause, can originate from the apex and propagate to ...
Dental autotransplantation entails extracting and repositioning a tooth into a different site in the mouth of the same patient. A successfully transplanted ...
Mineral trioxide aggregate (MTA) was introduced as an alternative to traditional materials for the repair of root perforations and pulp capping and as a ...
As an oral surgeon and prosthodontist specialising in full-mouth rehabilitation, I have consistently sought to integrate advanced technologies into my ...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






























To post a reply please login or register