When a patient presents to your dental practice with questionable and/or non-restorable teeth requiring full-mouth extractions, the greatest concern is whether or not implants can be placed in the same surgical visit and if so whether the patient will be able to walk out with fixed teeth. Having an implant system within your practice that allows you to load or progressively load, so that these patient’s demands are met, allows you to position your practice at a whole new level.
Of course, certain parameters must be met in order to facilitate this type of treatment. This includes, but is not limited to the quality and quantity of bone, the presence of infection, the patient’s health and the skills of the dental provider. Additionally, the selection of the most appropriate materials for the most ideal situation must be met.
Clinical case
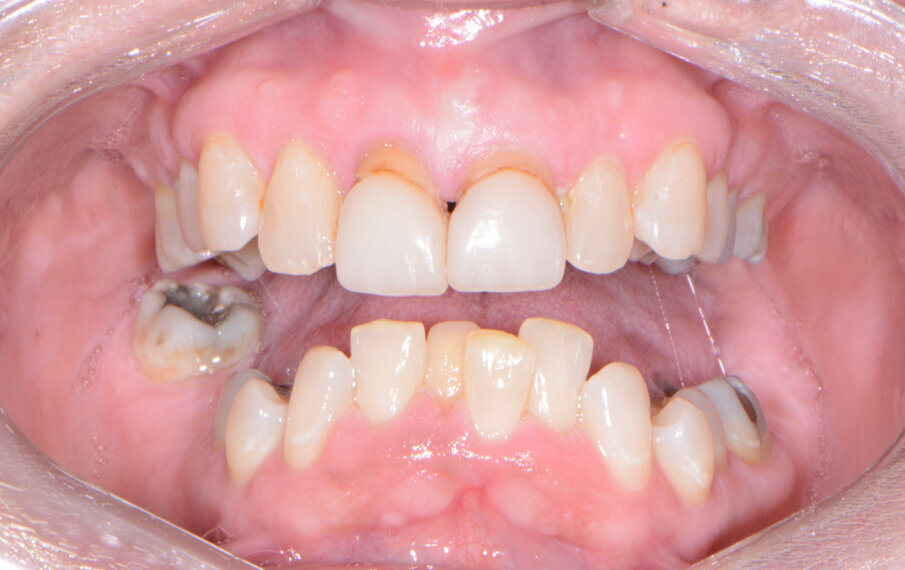
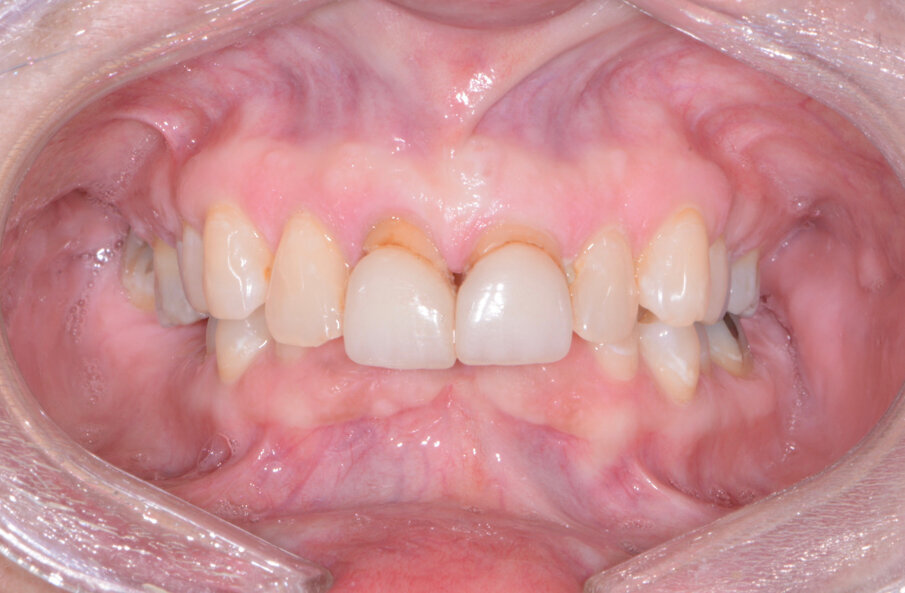
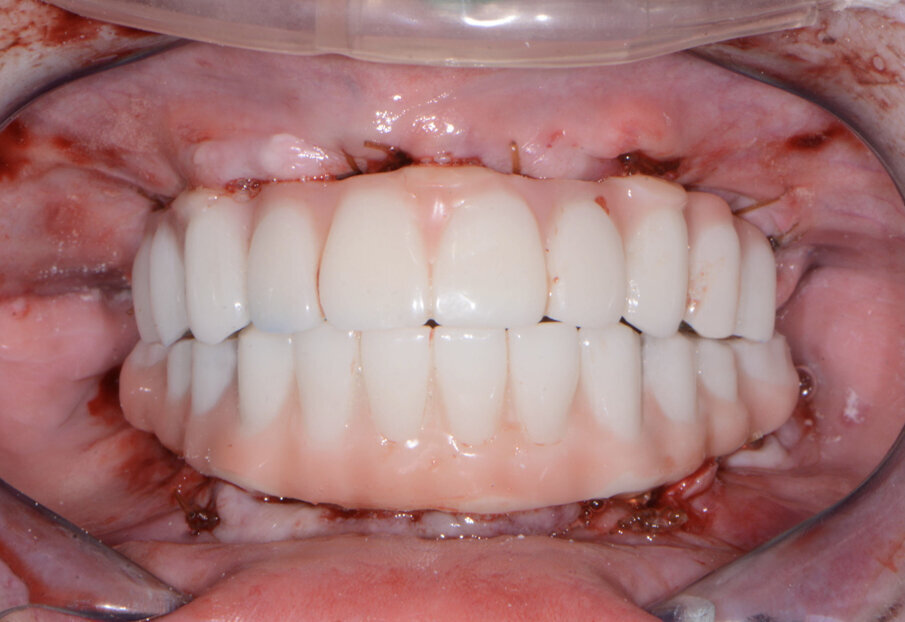
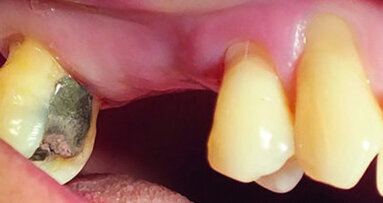
A patient presented to my practice for a consultation wanting to restore her dentition to proper form and function (Fig. 1). She complained of generalised discomfort and mobility in these teeth, apparently due to advanced periodontal disease. There were several teeth in both arches that had Grade III mobility upon clinical examination. Also, there was hyper-eruption in the anterior mandibular dentition due to her jaw position with a deep impinging bite (Fig. 2).
The clinical evaluation included information regarding lip length and support, the position of the natural teeth, occlusion, restorative space and phonetics. In addition, digital images of frontal, side and occlusal views of the dentition as well as facial shots were captured with a Nikon D7200 (PhotoMed).
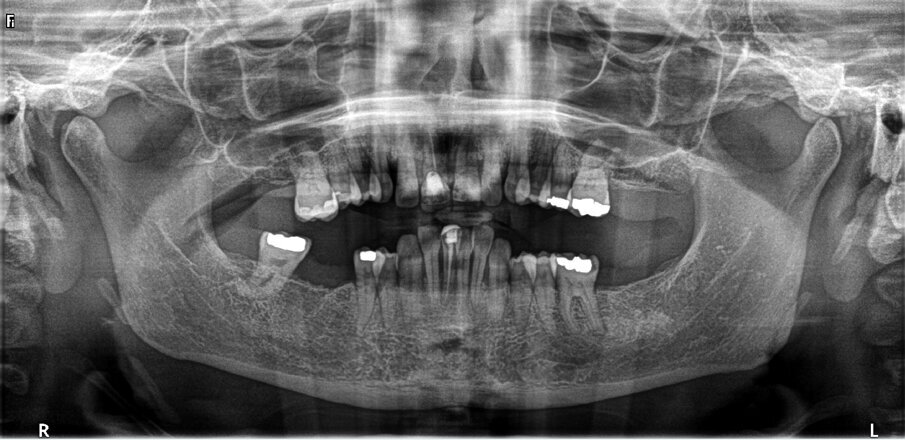
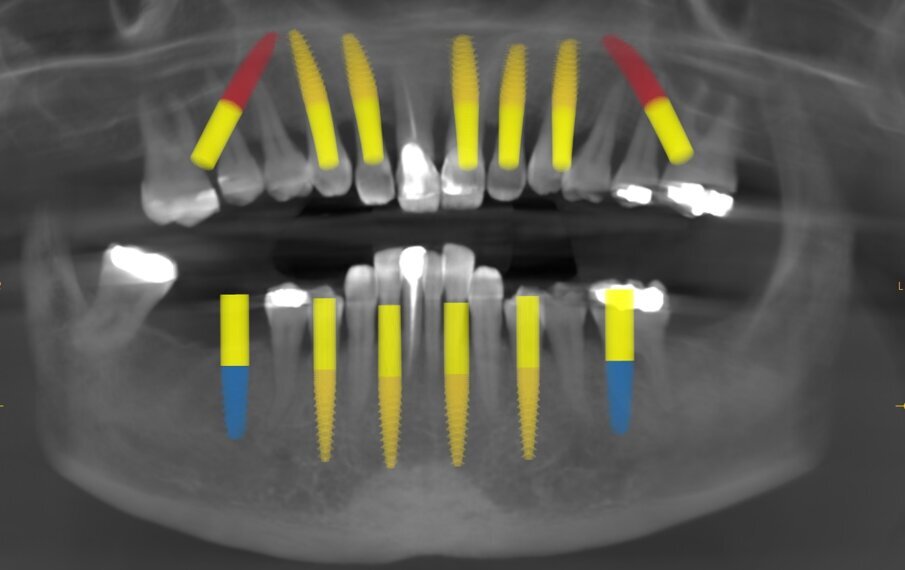
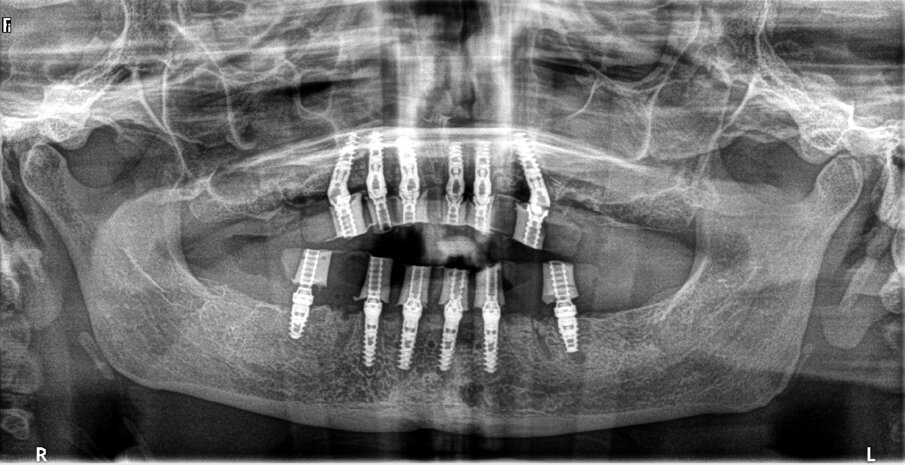
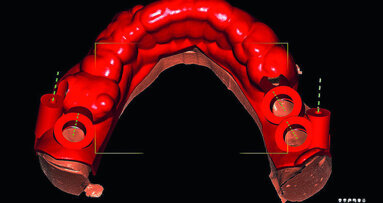
A CBCT scan and panoramic radiograph using the CS 8100 3D device (Carestream Dental; Fig. 3) were taken to accurately capture the information needed to properly plan the treatment for this case that would ensure the most ideal outcome, especially since the patient had discussed how unhappy she was with her existing smile. Using the CS 3D imaging software (Carestream Dental), dental implants were virtually planned in key positions in both arches (Fig. 4).
To further develop the treatment plan, diagnostic model impressions were taken using Silginat polyvinylsiloxane impression material (Kettenbach), poured up and forwarded to the dental laboratory. These models were then mounted on an articulator (Stratos 100, Ivoclar) for further analysis in order to meet the patient’s aesthetic and functional needs.
Fig. 3: Pre-op panoramic radiograph
Fig. 4: Planning with the CS 8100 3D device.
Fig. 5: Surgical guides and provisional restorations.
Financing options using a third-party payment option (LendingClub) were discussed with the patient. This discussion was a very important part of facilitating acceptance of her care, since it made the cost of treatment more feasible.
A 3D virtual treatment plan was further developed from our planning with the CS 3D imaging software, integrating it with the photographs and models. A virtual online integrative meeting with the dental laboratory allowed for a comprehensive review of the assembled digital and clinical information to formulate an optimal treatment plan that would fulfil the necessary requirements for aesthetics, form and function. Within a short amount of time, the dental laboratory had fabricated all the necessary guides for positioning, levelling, drilling and implant placement, in addition to the PMMA provisional restorations and back-up dentures (Fig. 5).
It is my belief that surgical guides in implant dentistry increase the predictability of treatment outcomes as well as make the clinician extremely efficient. In the past, implant placement routinely took place freehand, but this approach heightened the risk of damage to anatomical structures and lengthened the duration of the surgery. I personally feel that surgical guides give clinicians more confidence in accurately placing implants in every case, whether general practitioners or specialists. Precision surgery reduces stress, decreases liability and leads to a better outcome for the patient.
The implants that would be utilised for this case were Touareg-OS dental implants (Adin Dental Implant Systems; Fig. 6). The Touareg-S and Touareg-OS spiral implants are tapered with a spiral tap that condenses the bone during placement for immediate stability. There are two large variable threads and a tapered design for accurate implant placement, self-drilling, improved aesthetics and better load distribution. In addition, Touareg-OS implants feature the company’s biocompatible and osteoconductive OsseoFix implant surface. This has proved to achieve the desired roughness levels for optimal osseointegration, attain the highest implant surface purity levels and increase the success rate of bone-to-implant contact.
Fig. 6: Touareg-OS dental implants.
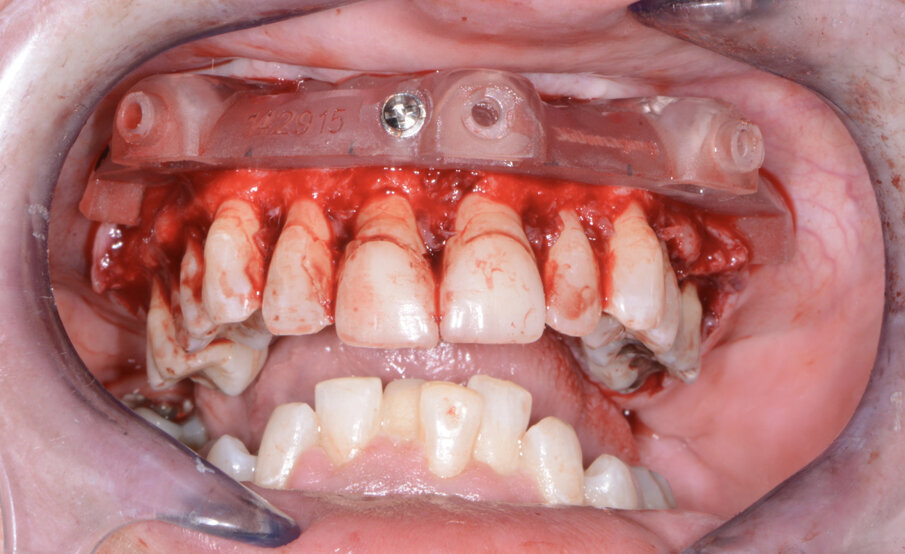
Fig. 7: Maxillary bone levelling foundation guide.
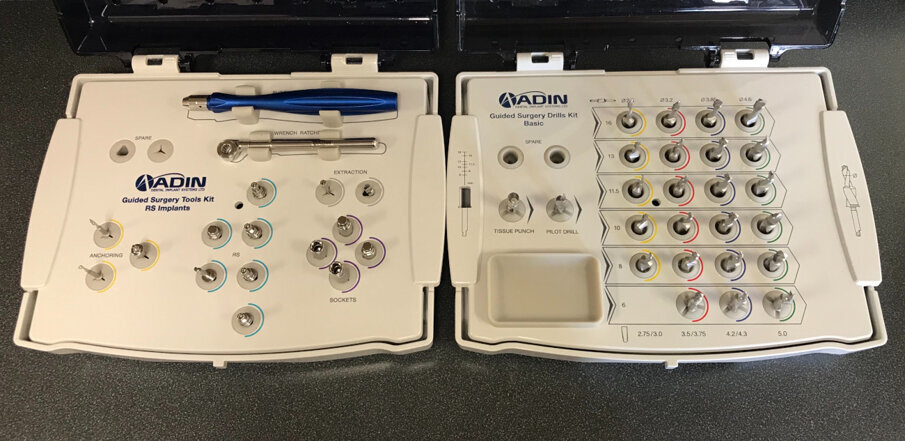
Fig. 8: Guided surgery dental implant kits.
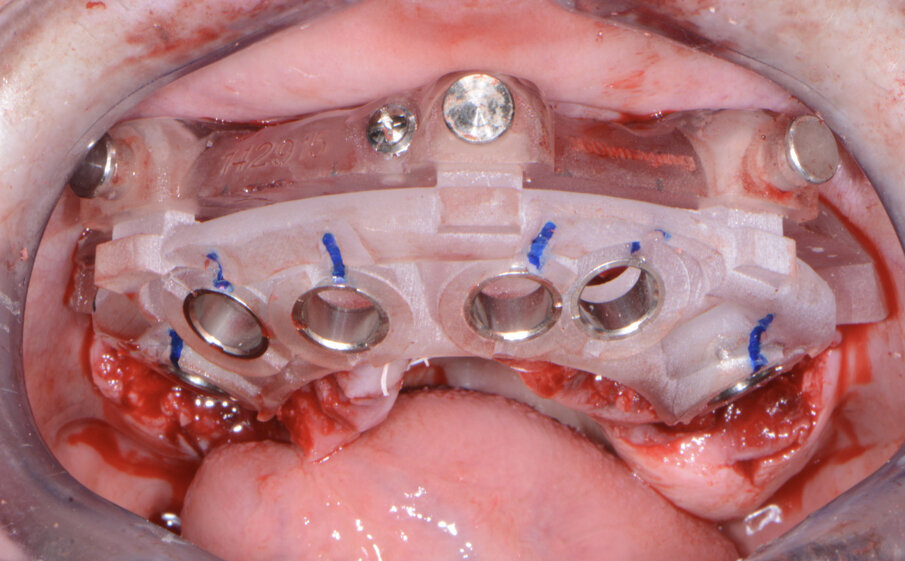
Once the virtual plan had been orchestrated and fully confirmed, the next appointment was for the planned surgery with all the necessary components for the guided surgical approach. The patient was appropriately sedated with intravenous medications, and local anaesthesia was administered in both arches. The tissue was then reflected using the Reflector instrument (GoldenDent) so that the bone levelling surgical guide would be fully seated and fixed with its respective retention screws (Fig. 7). After the positioning of the surgical guide, the maxillary teeth were atraumatically extracted utilising the Physics Forceps (GoldenDent). Once the appropriate bone levelling had been accomplished with the surgical handpiece, the implant surgical guide (Fig. 8) was positioned into the bone levelling guide and the osteotomies for the implants were initiated with a designated pilot drill in the implant system’s guided surgery drill kit (Adin Dental Implant Systems; Fig. 9). Using precise orientation, depth and direction, the guided surgery kit provides fast, effective and predictable preparation and placement of dental implants for dental practitioners. It also features easy-to-follow layouts along containing self-centring drills with built-in stoppers. The unique design of the guide, employing ActiveFlow irrigation technology, directs cooling saline through the guide, ensuring that irrigation reaches the bone and thereby reducing the possibility of bone heating throughout the procedure.
Utilising the Mont Blanc surgical handpiece and AEU 7000 surgical motor (both Aseptico) at a speed of 800 rpm with copious amounts of sterile saline, sequential drill preparation was initiated. Once the osteotomies were complete, the drivers in the guided kit (Adin Dental Implant Systems; Fig. 10) were used to place the dental implants with precise timing so that the flat portion of the internal hex was positioned ideally for receiving the multiunit abutments.
A baseline implant stability quotient (ISQ) reading was taken of these implants utilising the Penguin RFA unit (Aseptico). Since the initial readings were all above 70 ISQ, and the quality of bone after levelling was good, multi-unit abutments (Adin Dental Implant Systems) were tightened into the Touareg-OS dental implants to 30 Ncm, followed by temporary cylinders to 15 Ncm.
Fig. 9: Maxillary implant surgical guide.
Fig. 10: Touareg-OS dental implant.
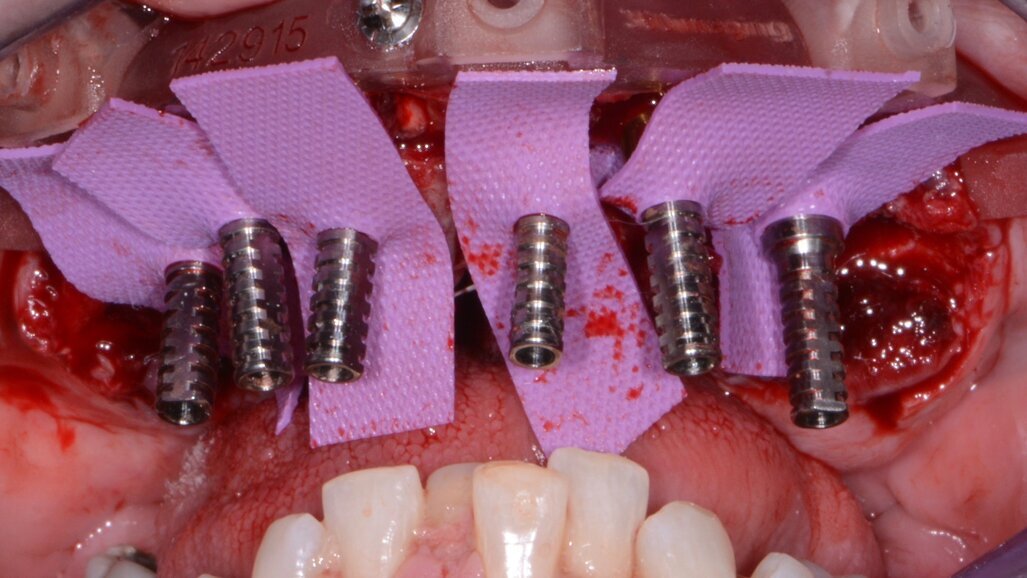
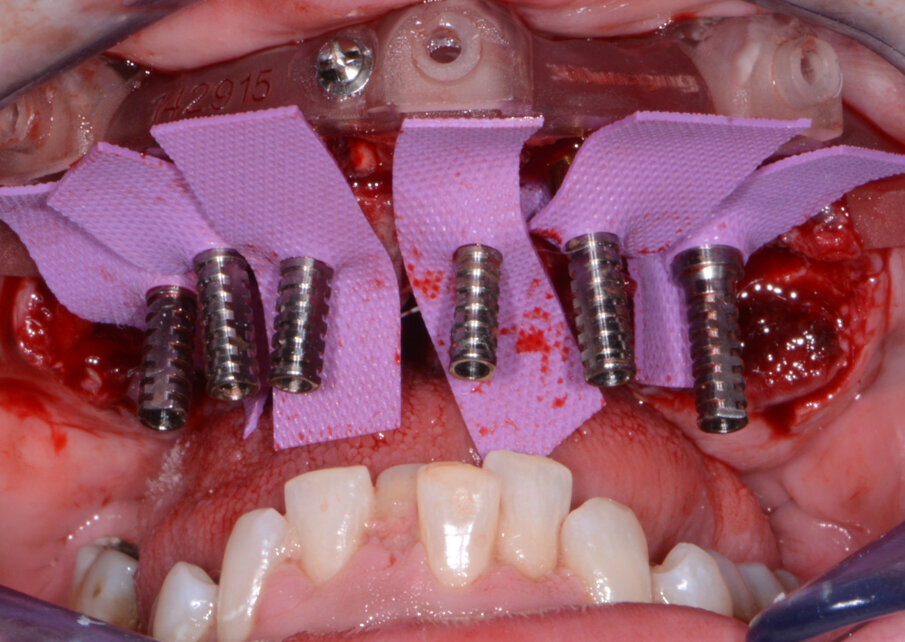
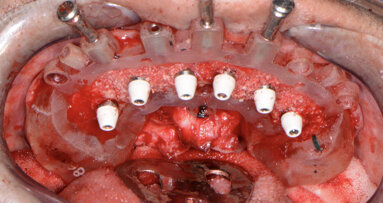
Fig. 11: Maxillary temporary cylinders isolated.
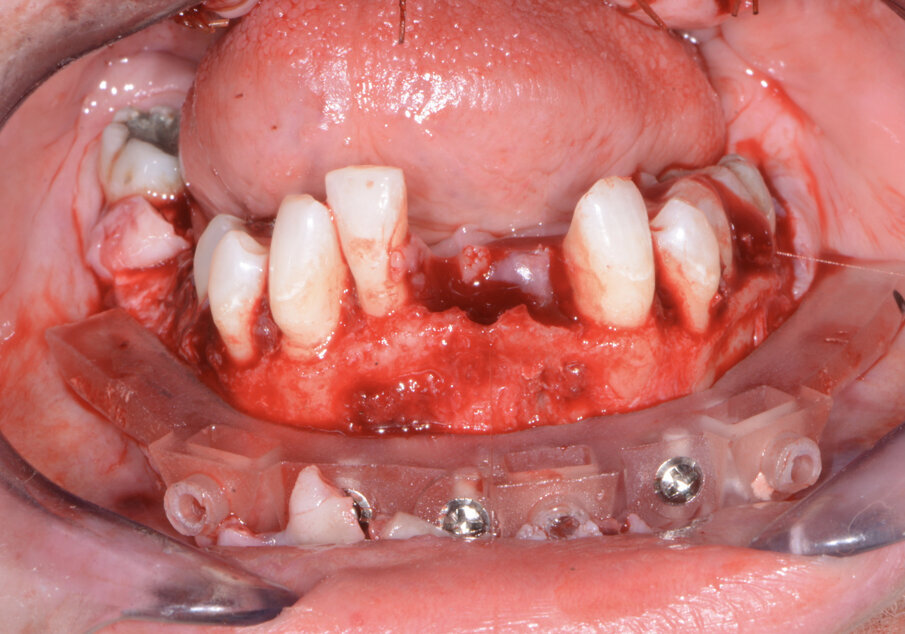
Fig. 12: Mandibular bone levelling foundation guide.
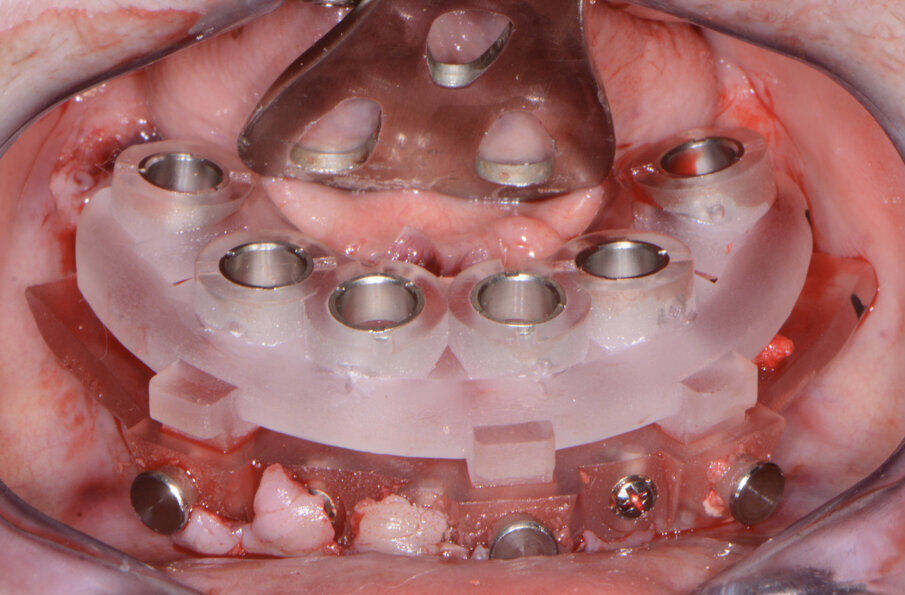
Fig. 13: Mandibular implant surgical guide.
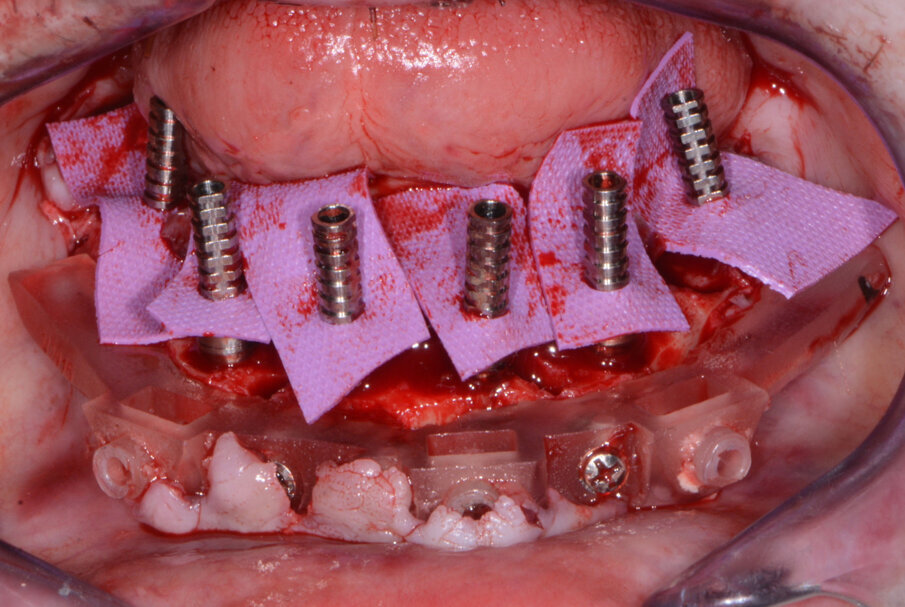
Fig. 14: Mandibular temporary cylinders isolated.
Fig. 15: Maxillary and mandibular provisional restorations.
Fig. 16: Post-op panoramic radiograph.
Any residual areas around the implants or in the sockets were grafted with a mineralised and demineralised cortical bone grafting material (GoldenDent) to optimise the area for regeneration.
The prefabricated immediate provisional arch restorations with pre-drilled access openings were inspected before being tried in.
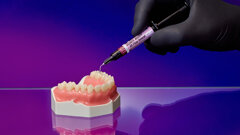
The maxillary provisional restoration was tried in to verify a passive fit over the temporary abutments. Once fit had been confirmed, trimmed dental dam pieces were placed to avoid the restoration (Fig. 11) from locking on during the relining procedure with REBASE III FAST set hard reline material (Tokuyama Dental). After the material had polymerised, the immediate provisional restoration was removed and any access material was removed with the Torque Plus laboratory handpiece (Aseptico) and an acrylic bur (Komet). The same procedures were accomplished in the mandibular arch (Figs. 12–14). Once trimmed and polished, the provisional restorations were seated and tightened with a torque wrench at 15 Ncm (Fig. 15). The access openings were filled in three-quarters of the way with Teflon tape, followed by Cavit filling material (3M ESPE). A postoperative panoramic radiograph was taken immediately after the surgery (Fig. 16).
A few days later, the patient returned for her postoperative appointment with very little discomfort, swelling or bruising. She was very pleased with her new maxillary and mandibular fixed provisional restorations. The occlusion was further checked and adjusted to confirm that there were no interferences in lateral or protrusive movements. The next step in her treatment would consist of full-arch impressions for the definitive restorations approximately four to five months postoperatively.
Conclusion
Having the ability to take a patient from start to finish in a fewer number of appointments within your practice allows you to position yourself as a provider that can fulfil your patient’s surgical and restorative needs. With the proper training and appropriate materials, a dental provider may provide extraction, grafting and implant placement within one appointment at one location. Not only does this allow you to reduce the number of visits for the patient, but this type of service also helps minimise the cost to the patient, since he or she is not seeing multiple dental providers. Most importantly, this enables the dental provider full control of the surgical and prosthetic outcome. Depending on the patient’s desires, the clinical conditions of the oral environment and the skills of the provider, a dentist may choose to extract teeth, level bone and graft with guided dental implant placement within his or her dental practice.
Tags:
When a patient presents to your dental practice with questionable and/or non-restorable teeth requiring full-mouth extractions, the greatest concern is ...
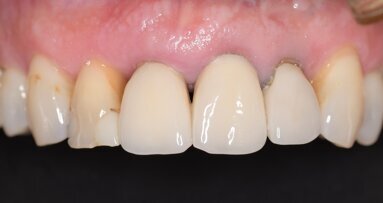
A 62-year-old male patient was referred to my practice for implant planning and treatment in the maxillary anterior region. The teeth in the maxillary ...
Computer-aided implantology (CAI) was introduced more than 25 years ago with the aim of facilitating implant planning and avoiding intra-operative ...
The evolution of digital dentistry has revolutionised the way dental procedures are planned and executed. This case highlights the integration of various ...
As implant dentistry continues to evolve to meet our patient’s demands for aesthetic tooth replacements with minimal downtime or inconvenience, the ...
Immediate placement of implants into fresh extraction sockets has been shown to deliver good outcomes. The literature reports good implant survival rates, ...
Proper 3D implant positioning is a crucial factor for predictable implant and prosthodontic treatment. Guided osteotomy preparation and placing implants ...
The procedure of implantation is becoming an increasingly popular method for replacing teeth. The critical factor in the achievement of a therapeutic and ...
A 52-year-old female patient was concerned about the appearance of her smile. Her upper right first molar and second premolar had been missing for several ...
Straumann Campus provides dental professionals with a myriad of webinars with a focus on implant dentistry and orthodontics. In the coming weeks, the online...
Live webinar
Wed. 3 June 2026
1:00 pm EST (New York)
Live webinar
Thu. 4 June 2026
2:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
12:00 pm EST (New York)
Live webinar
Mon. 8 June 2026
1:00 pm EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 pm EST (New York)
Live webinar
Wed. 10 June 2026
11:00 am EST (New York)
Live webinar
Wed. 10 June 2026
2:00 pm EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



































To post a reply please login or register